If walking through the grocery store is only comfortable when you’re leaning on the cart, you’re not alone. That specific relief is a classic sign of a condition that causes persistent lumbar spinal stenosis leg pain. This happens when the spinal canal in your lower back narrows, putting pressure on the nerves traveling down to your legs. Even in cases of severe spinal stenosis lumbar, finding relief is possible. This guide focuses on the most effective lumbar canal stenosis treatment options that are non-surgical, helping you get back on your feet without invasive procedures.
Key Takeaways
- Recognize the key signs of stenosis: Pay attention to lower back and leg pain, numbness, or weakness that gets worse when you stand or walk but feels better when you sit down or lean forward.
- Explore non-surgical options first: Effective management often involves a personalized plan combining physical therapy, chiropractic adjustments, and anti-inflammatory nutrition to address the root cause of your pain without invasive procedures.
- Make supportive lifestyle changes: You can significantly influence your comfort and mobility by incorporating low-impact exercise, maintaining a healthy weight, and practicing good posture to reduce daily strain on your spine.
Understanding Lumbar Spinal Stenosis
If you're dealing with persistent low back pain, you might have heard the term "spinal stenosis." In simple terms, lumbar spinal stenosis is a narrowing of the spinal canal in your lower back. Think of your spine as a protective tunnel that houses your spinal cord and the nerves branching out from it. When this tunnel becomes too narrow, it can put pressure on those nerves, leading to pain, weakness, or numbness, primarily in your legs and lower back.
This condition is quite common, especially as we get older. The narrowing doesn't happen overnight; it's usually a gradual process. Understanding what's happening inside your body is the first step toward finding effective relief and getting back to the activities you love. At Ascend Functional Health, we focus on identifying the root cause of your pain to create a personalized plan that supports your body's natural healing process.
How Common Is Spinal Stenosis?
If you've recently been told you have spinal stenosis, you're in very good company. This condition is an incredibly common part of the aging process, with some degree of age-related spinal change affecting up to 95% of people by the time they turn 50. While it's most often diagnosed in adults over 50, it's not just a number on a chart; it affects hundreds of thousands of people in the U.S. alone. The good news is that a diagnosis doesn't automatically point toward invasive procedures. In fact, many people with mild to moderate symptoms find significant relief through a personalized care plan. Understanding that this is a widespread and manageable condition is the first step toward seeking the right kind of support to improve your quality of life.
Why Does the Spinal Canal Narrow?
So, what causes this narrowing? Most often, it’s the result of normal wear and tear on the spine that comes with age. Over time, changes in your body can start to crowd the spinal canal. Conditions like herniated discs, degenerative disc disease, or osteoarthritis can cause bone spurs or thickened ligaments that intrude on the space meant for your nerves.
When these spaces get too tight, they can squeeze or "pinch" your spinal cord and the nerves that travel from your spine down to your legs. This pressure is what triggers the symptoms you feel, whether it's a dull ache in your back, a sharp pain down your leg, or a tingling sensation in your feet. Our approach to physical medicine aims to address these underlying structural issues without invasive procedures.
Lumbar vs. Cervical Stenosis: What's the Difference?
Spinal stenosis can happen anywhere along the spine, but it most commonly affects the lower back (lumbar spine) and the neck (cervical spine). The location of the narrowing determines the symptoms you'll experience.
Lumbar spinal stenosis, the focus here, typically causes pain in the lower back that can radiate down through your buttocks and into one or both legs. You might also feel cramping or weakness in your legs, especially when walking.
Cervical stenosis, on the other hand, affects the neck. Its symptoms often involve numbness, tingling, or weakness in an arm, hand, leg, or foot. It can also lead to problems with balance and walking. Distinguishing between the two is key to getting the right diagnosis and treatment for the conditions we treat.
Classifying Stenosis by Location
To get a clearer picture of what’s happening, it helps to know that stenosis is classified based on where the narrowing occurs within your spine. The two main locations are the foramina and the central canal. While both can cause similar symptoms, understanding the specific site of the nerve compression is essential for developing an effective plan to manage your discomfort and improve your mobility. This detailed classification allows for a more targeted approach, ensuring that the strategies used address the precise area where the pressure is being applied to your nerves.
Foraminal vs. Central Canal Stenosis
Foraminal stenosis happens when the openings on the sides of your vertebrae, called the foramina, become smaller. Think of these as the doorways through which your spinal nerves exit to travel to the rest of your body. When these doorways shrink, often due to a bone spur or a bulging disc, the nerve can get pinched on its way out. This compression can lead to pain, numbness, or weakness in the areas that nerve serves, like your legs. Interestingly, the severity of the narrowing doesn't always match the intensity of the symptoms; some people with significant foraminal stenosis experience very little discomfort.
Central canal stenosis, on the other hand, involves the narrowing of the main channel that runs down the center of your spine, housing the spinal cord itself. This is the primary "highway" for your nerves. Age-related changes, such as the thickening of ligaments or degenerative disc issues, can cause this canal to become constricted. This puts pressure on the spinal cord and nerve roots within it, often resulting in back pain, stiffness, and neurological symptoms like tingling or weakness in both legs. Pinpointing whether the issue is in the central canal or the foramina is a critical step in understanding the unique nature of the conditions we treat and tailoring a precise approach to your care.
What Causes Lumbar Spinal Stenosis?
Spinal stenosis doesn't just appear overnight. It develops gradually as the spaces within your spine begin to narrow, putting pressure on the nerves that travel through your lower back. While it might sound complex, the reasons behind this narrowing are often straightforward. Understanding what causes this condition is the first step toward finding a path to relief. Most cases are linked to the natural aging process, but injuries and even genetics can play a role in why you might be experiencing symptoms.
How Aging and Wear-and-Tear Contribute
For most people, lumbar spinal stenosis is a result of the natural wear-and-tear that happens to the spine over decades. Think of it like the tread on a tire wearing down with use. As we age, the structures in our spine can change. This includes conditions like osteoarthritis, which can cause bone spurs to grow into the spinal canal. The soft, cushion-like discs between your vertebrae can also lose water content and flatten, or even bulge out in a herniated disc. These age-related changes slowly reduce the amount of space available for your spinal nerves, leading to the pressure that causes pain and other symptoms.
Can You Be Born With Spinal Stenosis?
While aging is the most common culprit, some people are simply born with a smaller spinal canal. This is known as congenital stenosis. If you have this condition, you might not experience any issues for years. However, because your spinal canal is already narrower than average, even minor age-related changes that wouldn't bother someone else can be enough to trigger symptoms. People with congenital stenosis often start noticing pain, numbness, or weakness much earlier in life, sometimes in their 30s or 40s, because there's less room to accommodate any changes like a bulging disc or a bone spur.
Do Past Injuries and Surgeries Play a Part?
A significant injury to your lower back can also set the stage for spinal stenosis. Trauma from a car accident, a fall, or a sports injury can cause fractures or dislocations of the vertebrae. The resulting inflammation and swelling can immediately narrow the spinal canal and put pressure on your nerves. Over time, the healing process itself can contribute to the problem. Scar tissue from a past injury or even a previous spinal surgery can build up and take up valuable space within the canal. Our approach to physical medicine focuses on proper healing to help manage these long-term effects.
Other Conditions That Can Cause Stenosis
Beyond the typical age-related changes, a few other health conditions can contribute to the narrowing of your spinal canal. For instance, the ligaments that help hold your spine together can thicken and harden over time, causing them to bulge into the spinal space. Similarly, osteoarthritis can lead to the formation of bone spurs that grow into the canal, further reducing the room available for your nerves. These issues often develop slowly, and you might not notice them until the pressure on your nerves becomes significant enough to cause symptoms. Understanding these contributing factors is a key part of developing a comprehensive care plan.
Less commonly, other conditions can play a role. For example, certain bone diseases like Paget's disease can cause abnormal bone growth that affects the spine. In rare cases, abnormal growths or cysts can also take up space within the spinal canal. It's also important to consider the role of systemic inflammation, which can worsen conditions like arthritis. Our approach to functional medicine often involves looking at the bigger picture to see how we can support your body's overall health and reduce the factors that contribute to your pain.
Lifestyle Habits That Increase Your Risk
While you can't stop the aging process, certain factors can influence how quickly your spine changes. Spinal stenosis is most common in people over 50, affecting a large percentage of the population as they get older. A sedentary lifestyle can lead to weak core and back muscles, which provide less support for your spine and may accelerate degenerative changes. Similarly, jobs that involve heavy lifting can speed up wear-and-tear. Addressing these factors is a key part of a functional medicine approach, which looks at how your daily habits, including maintaining a healthy weight, impact your overall spinal health and put extra stress on your discs.
How to Know If You Have Lumbar Spinal Stenosis
Lumbar spinal stenosis can be tricky because its symptoms often develop slowly and can come and go. You might dismiss them as normal signs of aging at first, but paying attention to specific patterns can help you understand what’s happening in your body. The most telling signs involve pain and other sensations in your lower back and legs, especially when you’re standing or walking. If you notice that your symptoms change depending on your posture, that’s a key indicator that stenosis could be the cause. At Ascend Functional Health, we help you connect these dots to get to the root of your discomfort.
What Are the Most Common Symptoms?
The signs of spinal stenosis can show up in your back, legs, and even your feet. Symptoms can vary from person to person, but there are common threads. You might feel a dull ache or sharp pain in your lower back. This discomfort often travels, starting in your buttocks and moving down your leg. Many people also report numbness, a "pins and needles" tingling, or a heavy feeling in their legs. A classic sign is that the pain gets worse when you stand or walk for a long time but feels better when you sit down or lean forward.
Why Does Walking Cause Leg Pain?
If you experience leg pain or cramping that flares up when you walk but disappears when you take a seat, it’s a hallmark symptom of lumbar spinal stenosis. This is called neurogenic claudication. When you stand or walk, the space in your spinal canal can narrow slightly, putting more pressure on the nerves. Bending forward or sitting opens up that space, which relieves the pressure and eases the pain. This is why many people with stenosis find they can walk much farther if they lean on a shopping cart or a walker.
What Stenosis-Related Back Pain Feels Like
The back pain from lumbar spinal stenosis isn't always constant. It can fluctuate, meaning you might have good days and bad days. The pain is often described as a deep, aching feeling in the lower back. For many, this discomfort is directly linked to activity. Standing in line at the grocery store might become difficult, but sitting in the car on the way home provides relief. This positional nature of the pain is a significant clue. It’s not just about whether you’re moving, but how your body is positioned while you do it.
Spotting Numbness and Weakness in Your Legs
Feeling like your legs might give out or noticing a persistent numbness can be unsettling. With spinal stenosis, these sensations happen because the compressed nerves in your lower back are having trouble sending clear messages to your leg muscles. When your legs feel weak, it’s because they are not getting the proper signal from your nerves to function correctly. This can affect your balance and make walking feel unsteady. You might also notice tingling or a loss of sensation in parts of your leg or foot, which is another sign of nerve interference.
When to Seek Immediate Care: Recognizing Red Flags
While most symptoms of lumbar spinal stenosis can be managed effectively over time, it's important to know which signs indicate a more serious problem that requires immediate attention. Listening to your body is always key, but certain symptoms are clear signals that you shouldn't wait. These "red flags" point to significant nerve compression that needs to be addressed right away to prevent lasting issues. Understanding what to look for empowers you to take the right action at the right time, ensuring you protect your long-term health and mobility.
Understanding Cauda Equina Syndrome
Cauda equina syndrome is a rare but serious condition that can arise from severe spinal stenosis. It happens when the bundle of nerve roots at the very bottom of your spinal cord—called the cauda equina, or "horse's tail"—becomes severely compressed. This compression can cut off sensation and movement to your lower body. Unlike the gradual onset of typical stenosis symptoms, the signs of cauda equina syndrome can appear suddenly and require urgent evaluation. Recognizing these specific symptoms is crucial for preventing permanent nerve damage.
If you experience any of the following, it is critical to seek immediate medical care. Pay close attention to a sudden loss of bowel or bladder control, numbness in the groin or inner thigh area (often called the "saddle region"), or a sudden, severe weakness in both legs. These severe symptoms are not typical of standard lumbar stenosis and signal a need for prompt assessment. Acting quickly is the most important step you can take to address the nerve compression and support a better outcome.
How Is Lumbar Spinal Stenosis Diagnosed?
Figuring out if you have lumbar spinal stenosis involves a few key steps. It’s not something you can self-diagnose, so getting a professional evaluation is essential for getting the right treatment. The process usually starts with a thorough physical exam and a discussion of your symptoms, followed by imaging tests to get a clear look at what’s happening inside your spine. This combination of hands-on assessment and advanced technology helps us pinpoint the exact cause of your pain and create a plan that’s tailored to you.
What to Expect During a Physical Exam
Your diagnostic journey starts with a detailed conversation about your health. We’ll discuss your symptoms, when they started, and what makes them better or worse. After that, we’ll perform a physical exam to check your muscle strength, balance, reflexes, and range of motion. We might ask you to walk, bend forward, or lift your legs to see what movements trigger pain. These simple tests help us see how your body responds and can point toward nerve compression caused by stenosis. This initial evaluation is key to understanding your unique situation before moving on to imaging. Ready to start the conversation? You can schedule a consultation with our team.
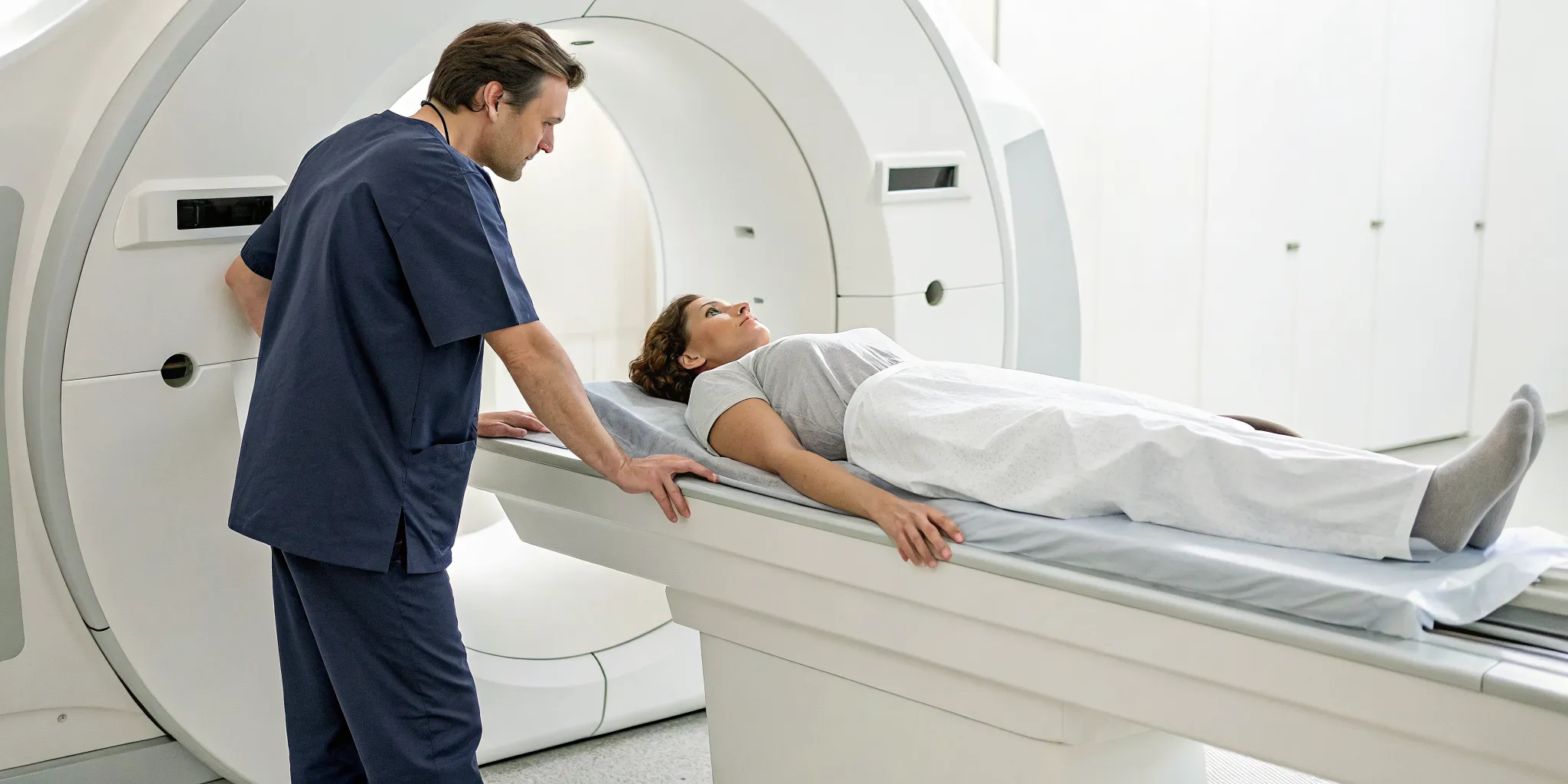
Why You Might Need an MRI or CT Scan
While a physical exam gives us important clues, we often need to see inside your spine to confirm a diagnosis. A Magnetic Resonance Imaging (MRI) scan is the gold standard for this. It uses a powerful magnet and radio waves to create detailed pictures of your spinal cord, nerves, and discs without using radiation. An MRI can show us exactly where the spinal canal is narrowing. If an MRI isn't an option for you, a Computed Tomography (CT) scan can be used. A CT scan creates cross-sectional images of your spine, giving us another valuable view of its structure.
When Are Advanced Diagnostic Tests Needed?
Sometimes, we need a little more information to complete the puzzle. A simple X-ray is often a helpful first step in imaging. While X-rays don’t show soft tissues like nerves, they are excellent for revealing changes in the bones, such as bone spurs or a loss of disc height, which are common contributors to stenosis. In some cases, a CT myelogram may be recommended. This is a CT scan where a special dye is injected to make the spinal cord and nerves show up more clearly. Combining these tests helps us build a complete picture of your spinal health, which is fundamental to our functional medicine approach.
Exploring Non-Surgical Lumbar Stenosis Treatments
If you’ve been diagnosed with lumbar spinal stenosis, your first thought might be about surgery. But for many people, surgery isn’t the first step. There are several effective non-surgical treatments that can significantly reduce pain and improve your ability to get back to your daily activities. The goal of these therapies is to manage your symptoms, strengthen the muscles that support your spine, and reduce inflammation around the compressed nerves.
Finding the right approach often involves combining a few different strategies. What works best for you will depend on the specifics of your condition and your overall health. At Ascend, we focus on creating a personalized treatment plan that addresses the root cause of your pain, not just the symptoms. By exploring these options, you can find lasting relief and improve your quality of life without going under the knife.
How Physical Therapy Strengthens Your Back
One of the most important non-surgical treatments for spinal stenosis is physical therapy. When your back hurts, your first instinct might be to rest, but staying active is essential for managing your symptoms. A physical therapist can guide you through specific exercises and stretches designed to improve your strength, flexibility, and posture. This helps take pressure off your spinal nerves and provides better support for your lower back.
A tailored physical medicine program will focus on strengthening your core and back muscles, which act as a natural brace for your spine. By building up this support system, you can reduce pain and make daily movements easier. Your therapist will teach you how to move safely to avoid further irritation.
Managing Pain with Anti-Inflammatory Medication
Medication can be a useful tool for managing the pain and inflammation associated with spinal stenosis. The discomfort you feel is often caused by swelling around the compressed spinal nerve. Anti-inflammatory medications, like NSAIDs (nonsteroidal anti-inflammatory drugs), can help reduce this swelling, which in turn may relieve the pressure on the nerve and ease your pain.
These medications can provide enough relief to help you participate more comfortably in other treatments, like physical therapy. While they don't fix the underlying narrowing of the spinal canal, they can be an effective part of a comprehensive plan to manage your symptoms. It's always best to talk with your doctor to determine which medication is right for you and how to use it safely.
Other Medications for Nerve-Related Pain
When nerve pain is the primary issue, standard anti-inflammatories may not be enough. In these cases, a doctor might discuss other types of prescription options that target nerve pathways directly. For example, some antidepressants can be effective for easing chronic nerve pain, not because of their mood-related effects, but because of how they influence pain signals. Similarly, certain anti-seizure drugs are sometimes used to help calm damaged nerves and reduce the discomfort they cause. These approaches aim to address the specific nature of nerve-related symptoms.
For severe pain, stronger prescription drugs like opioids may be considered for very short-term relief. However, these are used cautiously due to the high potential for dependency. The focus is always on finding a sustainable path to feeling better, and that involves a careful conversation with your provider about the benefits and risks of any treatment. This ensures the choice you make supports your overall well-being and long-term health goals, rather than just masking symptoms temporarily.
Should You Consider Epidural Steroid Injections?
For more targeted relief, an epidural steroid injection may be an option. This procedure involves injecting a strong anti-inflammatory medicine directly into the space around your spinal nerves. The goal is to deliver medication right to the source of the inflammation, which can provide powerful, though often temporary, pain relief.
These injections can be particularly helpful if your pain is severe and limits your ability to function. By calming the inflammation, an injection can create a window of opportunity for you to make progress with physical therapy and other rehabilitative exercises. It’s a way to break the cycle of pain and get you moving again, but it’s typically used alongside other long-term strategies for managing your condition.
Understanding the Limitations and Risks
It's important to have a clear picture of what non-surgical treatments can and can't do. While options like medication and injections are excellent for managing pain, they don’t change the physical structure of your spine. They won't reverse the narrowing that has already happened, whether it's from years of wear-and-tear or a past injury. Instead, the goal is to reduce inflammation and control your symptoms. This creates a crucial window for you to participate in other therapies, like physical therapy, that build long-term strength and stability. The relief you feel might last for months, or it could be shorter. This is normal, and it’s why we emphasize a comprehensive approach that supports your body's healing process for the long haul.
How Chiropractic Care Can Provide Relief
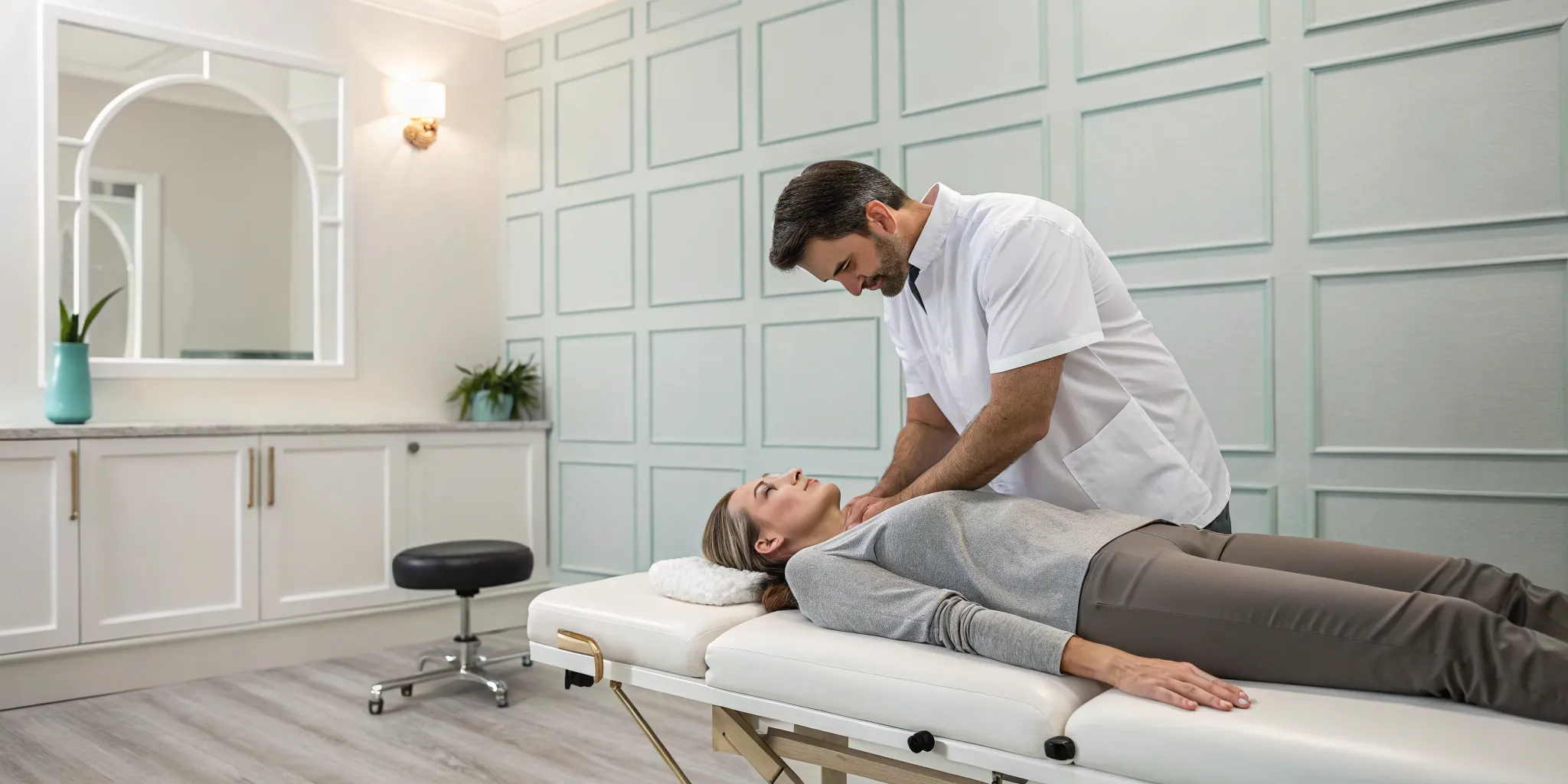
Chiropractic care is another excellent non-surgical option for managing spinal stenosis symptoms. A chiropractor focuses on improving spinal mobility and function through gentle, targeted adjustments. For stenosis, the goal isn’t to change the narrowing of the canal itself but to restore movement in the surrounding spinal joints and reduce pressure on the nerves.
By using specific techniques, a chiropractor can help improve your flexibility and decrease pain. This hands-on approach is a core part of our physical medicine services at Ascend. We work to improve your spine’s overall mechanics, which can provide significant relief and help you maintain an active lifestyle. Regular chiropractic care can be a key part of your long-term strategy for living well with spinal stenosis.
Other Minimally Invasive Procedures
When foundational treatments like physical therapy and chiropractic adjustments aren't providing enough relief, there are other options to explore before considering more invasive routes. Minimally invasive procedures are designed to target the source of your pain with less impact on your body than traditional surgery. These techniques can be an effective next step for managing symptoms and improving your mobility. They focus on directly addressing the pressure on your spinal nerves, offering a more targeted approach to pain relief when you need it.
Minimally Invasive Lumbar Decompression (MILD)
Minimally Invasive Lumbar Decompression, often called the MILD procedure, is a technique specifically designed to address stenosis caused by a thickened ligament in the spine. In this procedure, a doctor removes small pieces of the ligament tissue to create more space in the spinal canal, which relieves the compression on your nerves. It’s a targeted approach that can lead to significant improvements in pain and functional outcomes for the right candidates. Because it addresses a very specific cause of narrowing, it’s a specialized option that can help you stand longer and walk farther with less pain.
Nerve Blocks and Radiofrequency Ablation (RFA)
Nerve blocks and Radiofrequency Ablation (RFA) are two procedures focused on interrupting pain signals. A nerve block involves injecting an anesthetic near the affected nerve to provide temporary pain relief. It can also be used as a diagnostic tool to confirm which nerve is causing the problem. RFA is a longer-lasting solution where heat is used to create a lesion on the nerve, which stops it from sending pain signals. Studies show these procedures can yield good results, providing meaningful relief that helps people get back to their daily activities with greater comfort.
Holistic Approaches to Managing Spinal Stenosis
While conventional treatments are essential, a holistic approach can make a significant difference in your daily comfort and long-term spinal health. These strategies work alongside medical care to address your body as a whole system. Instead of just masking pain, the goal is to reduce inflammation, improve mobility, and give your body the support it needs to feel its best. By incorporating these methods, you can build a more comprehensive and personalized plan for managing spinal stenosis and reclaiming your quality of life.
Taking a Functional Medicine Approach to Your Spine
When you’re dealing with chronic pain from spinal stenosis, it’s easy to focus only on the symptoms. But what if we looked deeper? A functional medicine approach does exactly that. It’s a partnership where we work together to identify and address the root causes of your pain, rather than just treating the discomfort itself. We consider factors like inflammation, nutritional deficiencies, and lifestyle habits that might be contributing to your condition. This allows us to create a personalized plan that supports your body’s natural healing abilities for more sustainable relief.
How Acupuncture and Massage Can Help
Acupuncture and massage are powerful tools for managing the discomfort of spinal stenosis. Acupuncture involves stimulating specific points on the body, which can help relieve pain and reduce pressure on compressed nerves. Think of it as helping your body’s own pain-relief system work more effectively. Massage therapy complements this by focusing on the muscles surrounding your spine. It can ease muscle tension, improve circulation to the affected area, and provide a welcome sense of relief. Both therapies are excellent, non-invasive ways to support your physical medicine treatment plan.
Eating to Reduce Inflammation and Pain
What you eat has a direct impact on inflammation levels throughout your body, including around your spine. Adopting an anti-inflammatory diet can be a game-changer for managing spinal stenosis. This means focusing on whole foods that fight inflammation and avoiding those that trigger it. Fill your plate with foods rich in omega-3 fatty acids like salmon and walnuts, and plenty of colorful fruits and vegetables packed with antioxidants. Simple swaps, like choosing olive oil over vegetable oil, can also help reduce inflammation and support your overall spinal health.
Mind-Body Techniques for Pain Control
Managing spinal stenosis isn't just about your physical body; your mind plays a huge role, too. Mind-body techniques like gentle yoga, meditation, and tai chi can help you manage pain while also improving strength and flexibility. These practices teach you to connect with your body, improve your posture, and build core strength to better support your spine. Meditation and deep-breathing exercises can also help calm the nervous system, which can change your perception of pain and reduce the stress that often comes with a chronic condition.
When Is Surgery the Right Choice?
Deciding to have surgery is a major step, and for lumbar spinal stenosis, it’s rarely the first line of defense. At Ascend Functional Health, our philosophy is to start with the most effective, least invasive treatments possible. We focus on helping your body heal itself through physical medicine, targeted nutrition, and other holistic strategies. Surgery is typically considered only after these conservative methods have been thoroughly explored without providing the relief you need.
It’s a conversation, not a command. If your pain and symptoms are severely impacting your quality of life, it’s important to understand all your options, including surgical ones. The goal is always to get you back to living comfortably and doing the things you love. Below, we’ll walk through the signs that might point toward surgery, the common procedures available, and what you can expect during the recovery period. This information can help you have a more informed discussion with your healthcare team to decide on the best path forward for you.
Signs It's Time to Consider Surgery
So, when does the conversation shift toward surgery? This usually happens when non-surgical treatments, like physical therapy and medication, haven't been enough to manage your symptoms. If your daily life is significantly impaired, it might be time to explore other options. Key signs include severe or unrelenting pain that doesn't respond to other care, persistent numbness or weakness in your legs that makes walking difficult, or a loss of mobility that restricts basic activities. The decision is deeply personal and should be made in partnership with a medical team that understands your health history and goals. If you're experiencing these symptoms, it's a good idea to schedule a consultation to discuss your situation.
What Are the Different Types of Surgery?
If surgery is deemed necessary, the primary goal is to create more space in the spinal canal to relieve pressure on the nerves. The most common procedure for this is a lumbar laminectomy. During this surgery, a surgeon removes a portion of the bone called the lamina, which acts as the "roof" of your spinal canal. This simple removal can provide immediate relief. Other surgical options include a laminotomy, which involves removing a smaller piece of the lamina, or a foraminotomy, which widens the area where nerve roots exit the spine. In some cases, a spinal fusion may be performed to stabilize the spine. The right procedure depends entirely on the specifics of your condition.
Modern Surgical Options
When surgery becomes the best option, the main objective is straightforward: to create more room for your nerves. This is often achieved through a procedure called a lumbar laminectomy, where a surgeon removes the lamina—the bony arch of your vertebra—to relieve pressure. Think of it as taking the roof off a crowded tunnel to give everything inside more space. For less severe cases, a surgeon might perform a laminotomy, which involves removing only a small part of the lamina, or a foraminotomy, which focuses on widening the specific openings where nerves exit the spine. These modern techniques are designed to be as precise as possible, targeting only the areas causing the compression.
Understanding Success Rates and Risks
Deciding on surgery is a significant choice, and it's important to have a clear picture of what to expect. While many people experience significant relief from their symptoms after surgery, success isn't guaranteed for everyone. Like any procedure, there are potential risks, such as infection or blood clots. The outcome often depends on your overall health and the specific cause of your stenosis. This is why a thorough discussion with your healthcare provider is so crucial. It’s a time to weigh the potential benefits against the risks and ensure the chosen path aligns with your personal health goals. We believe in empowering you to make informed decisions about your care every step of the way.
What Does Recovery from Surgery Involve?
It’s important to remember that most people with spinal stenosis live full, active lives without ever needing surgery. For those who do, recovery is a process that requires patience and commitment. Post-surgery, you will likely begin working with a physical therapist to regain strength and mobility safely. You’ll also need to be mindful of your movements, avoiding activities like bending, twisting, and lifting for several weeks to months to allow your spine to heal properly. Our physical medicine team can help create a plan that supports your body both before and after a procedure, ensuring you have the guidance you need for a strong recovery.
Lifestyle Changes for Lasting Relief
While medical treatments are essential, the small choices you make every day can have a huge impact on managing lumbar spinal stenosis. Integrating healthier habits into your routine can help reduce pain, improve mobility, and give you more control over your well-being. Think of these changes not as a complete overhaul, but as simple, powerful adjustments that support your spine and your overall health.
From gentle movement to mindful posture, these strategies work alongside your treatment plan to provide lasting relief. Let’s explore some practical lifestyle changes you can start making today.
Safe Exercises to Support Your Spine
When you’re in pain, exercise might be the last thing on your mind. But the right kind of movement is one of the best things you can do for your back. The goal is to strengthen the muscles that support your spine without adding extra strain. Low-impact exercises are perfect for this. Activities like walking, swimming, or cycling get your blood flowing and build strength gently.
A structured physical therapy program is also a cornerstone of non-surgical treatment. A professional can guide you through specific stretches and exercises designed to improve your flexibility, correct your posture, and ease your symptoms. At Ascend, our Physical Medicine services focus on creating a personalized plan that helps you move with more confidence and less pain.
How Managing Your Weight Supports Your Back
Carrying extra weight places a significant load on your entire body, especially your spine. For someone with lumbar spinal stenosis, this added pressure can compress the spinal canal even more, making symptoms worse. By maintaining a healthy weight, you can directly reduce the strain on your spine and find noticeable relief from pain and discomfort.
This isn’t about a crash diet; it’s about making sustainable choices. Our Functional Medicine approach can help you identify the right nutritional strategies for your body. Focusing on anti-inflammatory foods and balanced meals not only helps with weight management but also supports your body’s natural healing processes, creating a positive cycle for your spinal health.
Easy Adjustments for Better Posture
You might be surprised by how much your daily posture affects your back pain. Many everyday activities, from sitting at a desk to lifting groceries, can make stenosis symptoms worse if done incorrectly. Adopting healthy habits, including good posture and ergonomic adjustments, can make a world of difference. Start by being mindful of how you sit and stand. Try to keep your spine in a neutral position, with your shoulders back and your head held high.
If you work at a desk, create an ergonomic setup. Adjust your chair so your feet are flat on the floor, and position your screen at eye level to avoid slouching. These simple self-care adjustments can prevent the daily wear-and-tear that aggravates your condition.
Adapting Daily Activities to Reduce Pain
Living with lumbar spinal stenosis often means learning to listen to your body. Your pain can fluctuate, with some days being better than others. Instead of pushing through the pain, it’s helpful to adjust your activities to match how you’re feeling. On a good day, you might go for a longer walk. On a tougher day, you might opt for gentle stretching or simply take more breaks.
Simple modifications can provide significant relief. For example, many people find that leaning forward slightly, like when pushing a shopping cart, can ease leg pain. When it comes to sleep, some find that using a recliner or an adjustable bed helps maintain spinal alignment and reduces nerve compression overnight. It’s all about finding what works for you and adapting your routine to support your back.
Using Walking Aids and Ergonomic Supports
If you’ve ever noticed that a trip to the grocery store feels much more manageable when you’re leaning on the cart, you’ve discovered a key strategy for managing stenosis. This isn't a coincidence; leaning forward slightly opens up the space in your spinal canal, which takes pressure off the compressed nerves in your lower back. Walking aids like a walker or even a cane can replicate this effect, providing the support you need to stay mobile with less pain. They encourage a posture that gives your nerves a little more breathing room, allowing you to walk farther and more comfortably.
This principle of supportive posture extends to all parts of your day, especially if you spend time sitting. Creating an ergonomic environment is about making small, intentional adjustments to reduce the daily strain on your spine. If you work at a desk, for instance, make sure your chair is adjusted so your feet can rest flat on the floor. Position your computer screen at eye level to prevent slouching, which can aggravate your symptoms. These simple changes help maintain a healthier spinal alignment throughout the day, preventing the cumulative stress that can lead to increased pain.
Can You Stop Lumbar Spinal Stenosis from Worsening?
Receiving a lumbar spinal stenosis diagnosis can feel overwhelming, but it’s important to know that you have a significant amount of control over how the condition progresses. While you can’t reverse the anatomical changes that have already occurred, you can absolutely take steps to manage your symptoms, slow the progression, and maintain a high quality of life. The key is to be proactive. By focusing on your overall health, maintaining mobility, and understanding the facts about stenosis, you can build a strong foundation for lasting spinal health.
Why Taking Action Early Matters
When it comes to managing spinal stenosis, the sooner you act, the better your outcome will be. Research shows that one of the most important factors in reducing the impact of stenosis is improving your overall physical health. Think of it this way: your spine is part of a larger system. By strengthening the muscles that support it, reducing inflammation throughout your body, and maintaining a healthy weight, you take a significant amount of pressure off your lower back. Our approach to functional medicine focuses on identifying these interconnected factors to create a personalized plan that supports your body’s natural ability to heal and function properly.
How to Maintain Your Spinal Mobility
Staying active is one of the best things you can do for lumbar spinal stenosis. Gentle, consistent movement helps nourish your spinal discs, improve flexibility, and strengthen your core and back muscles. A tailored physical therapy program can teach you specific exercises to improve your strength and posture, which can dramatically ease your symptoms. Simple changes, like being mindful of your posture when sitting and standing, can also make a big difference. Combining these efforts with regular chiropractic care can help maintain proper spinal alignment and relieve nerve pressure, forming a core part of our physical medicine services.
Stenosis Progression: Myths vs. Facts
There’s a lot of misinformation out there about spinal stenosis that can cause unnecessary worry. Let’s clear up a couple of common myths. One major misconception is that the condition always gets worse over time. The truth is, that’s not a guarantee. With the right care and lifestyle adjustments, many people are able to manage their symptoms effectively for years, and some even see a decrease in the narrowing of their spinal canal. Another myth is that leg weakness is an irreversible nerve issue. Often, this weakness is due to pressure, and simple aids like a cane can help by unloading the spine and reducing that pressure.
What Research Says About Prognosis
The long-term outlook for lumbar spinal stenosis is often much more positive than people expect. While the condition is chronic, it doesn't mean your symptoms are destined to get worse. In fact, research on the natural progression of stenosis shows that many people experience periods where their symptoms remain stable or even improve with conservative care. The key takeaway is that proactive management makes a significant difference. By focusing on strengthening the muscles that support your spine, improving your mobility, and reducing inflammation through lifestyle choices, you can have a major influence on your long-term comfort. This is why our integrated approach at Ascend, which combines physical medicine with functional medicine strategies, is so effective for creating lasting relief.
How to Live Well with Lumbar Spinal Stenosis
Receiving a diagnosis of lumbar spinal stenosis can feel overwhelming, but it doesn’t mean you have to give up the activities you love. With the right strategy, you can manage your symptoms, stay active, and maintain your quality of life. The key is to take a proactive approach that combines professional guidance with smart, consistent self-care. Think of it not as a set of limitations, but as a new path toward understanding your body and supporting it in the best way possible. By focusing on a personalized plan, long-term pain management, and practical ways to maintain mobility, you can continue to live a full and independent life.
Building Your Personalized Treatment Plan
Because spinal stenosis affects everyone differently, a one-size-fits-all treatment plan simply won’t work. The primary goal is always to relieve pressure on your spinal cord and nerves, which in turn reduces pain and helps you move more freely. At Ascend Functional Health, we start by creating a personalized plan that addresses the root cause of your symptoms. This involves a comprehensive evaluation of your spine, lifestyle, and overall health. Your unique roadmap might include a combination of Physical Medicine to restore function and targeted Functional Medicine protocols to support your body’s natural healing processes.
Long-Term Strategies for Managing Pain
Managing spinal stenosis pain is an ongoing practice, not a one-time fix. Lasting relief comes from building healthy habits that support your spine day in and day out. Physical therapy is a cornerstone of non-surgical treatment, as it helps improve your strength, flexibility, and posture to ease symptoms. Beyond formal therapy, simple changes like being mindful of your posture and incorporating regular, gentle movement can make a huge difference. We also work with you to identify lifestyle factors, like nutrition and stress, that may contribute to inflammation and pain, helping you build a sustainable, long-term strategy for feeling your best.
How to Maintain Your Independence and Mobility
Staying active is one of the most important things you can do for your spinal health and overall independence. While it might seem counterintuitive when you’re in pain, the right kind of movement is essential. Low-impact exercises like walking, swimming, or cycling can strengthen the muscles that support your spine without adding extra strain. You might also find simple tricks that help, like leaning on a shopping cart while at the store to relieve pressure. By learning to modify certain activities and listening to your body, you can continue to engage in daily life with confidence and control.
Related Articles
- Spinal Narrowing Neck: Symptoms & Treatments
- Bulging Disc Therapy Treatment: A Complete Guide
- Revitalize Your Spine with Spinal Decompression Therapy in Tampa, FL
Frequently Asked Questions
Can exercise make my spinal stenosis worse? This is a common and completely valid concern. While certain high-impact movements or improper form can definitely aggravate your symptoms, the right kind of exercise is one of the most effective tools for managing stenosis. The goal is to strengthen the core and back muscles that support your spine, which actually takes pressure off the compressed nerves. Low-impact activities like swimming, walking, and guided physical therapy are excellent for improving mobility and reducing pain without causing extra strain.
Is lumbar spinal stenosis something I just have to live with? Not at all. While the physical narrowing in your spine may not be reversible without surgery, the symptoms are highly manageable. Think of it less as a permanent sentence and more as a condition that you can actively control. Through a combination of physical medicine, lifestyle adjustments, and holistic strategies, many people find significant, long-term relief and continue to live full, active lives. The key is to find a personalized plan that addresses the root causes of your discomfort.
How is a functional medicine approach different from just seeing a regular doctor for this? A conventional approach often focuses on managing the direct symptoms of stenosis, for example, using medication to reduce pain or injections to decrease inflammation. A functional medicine approach looks at your body as an interconnected system. We investigate underlying factors that could be contributing to your pain, such as chronic inflammation from your diet, nutritional deficiencies, or other lifestyle habits. By addressing these root causes, we aim to create more sustainable relief and improve your overall health, not just mask the pain.
Do I need to lose weight to feel better? Maintaining a healthy weight can be a powerful part of your management plan, but it's just one piece of the puzzle. Extra body weight adds mechanical stress to your spine, which can increase the pressure on your nerves and make symptoms worse. For some people, even a modest weight loss can lead to a noticeable reduction in pain. We approach this as part of a holistic strategy that includes anti-inflammatory nutrition and healthy movement, focusing on overall well-being rather than just the number on the scale.
What's the very first step I should take if these symptoms sound familiar? If you're experiencing pain, numbness, or weakness in your lower back and legs, the most important first step is to get a clear and accurate diagnosis from a healthcare professional. Trying to guess what's going on or pushing through the pain can often make things worse. Seeking a professional evaluation will help you understand the specific cause of your symptoms and allow you to create a safe, effective treatment plan tailored to your body.