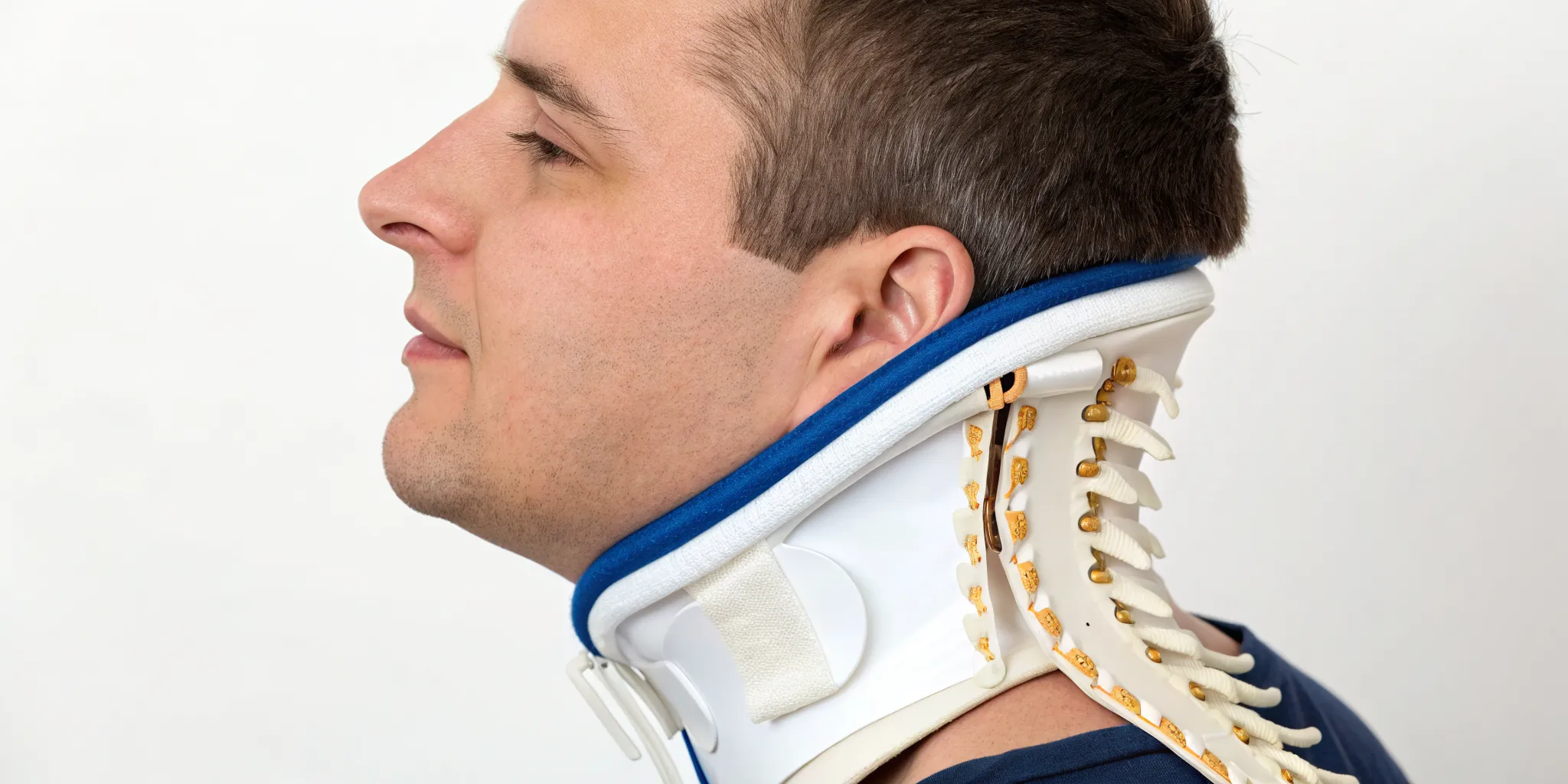
Neck pain is rarely just a neck problem. It’s often a signal from your body that something deeper is out of balance. While conventional treatments might focus on the tight muscles, a functional medicine approach asks why those muscles are so tight in the first place. Conditions like cervical myofascial pain are often linked to underlying issues like chronic inflammation, nutrient deficiencies, or even high stress levels. These factors can make your muscle tissue more vulnerable to developing painful trigger points. Instead of just chasing symptoms, we’ll explore how to identify and address these root causes for a more complete and lasting solution to your pain.
Key Takeaways
- Pinpoint the Real Source of Your Discomfort: Cervical myofascial pain stems from tight knots in your muscles called trigger points, which can send pain to other areas like your head and shoulders, often mimicking tension headaches.
- Connect Your Pain to Your Lifestyle: The problem often goes deeper than a simple muscle strain; factors like poor desk posture, repetitive movements, chronic stress, and even nutritional gaps can create and worsen trigger points.
- Adopt a Multi-Layered Approach to Healing: Lasting relief requires a combination of professional treatments like manual therapy, corrective exercises to restore function, and mindful daily habits to address the root cause and prevent pain from returning.
What Is Cervical Myofascial Pain Syndrome?
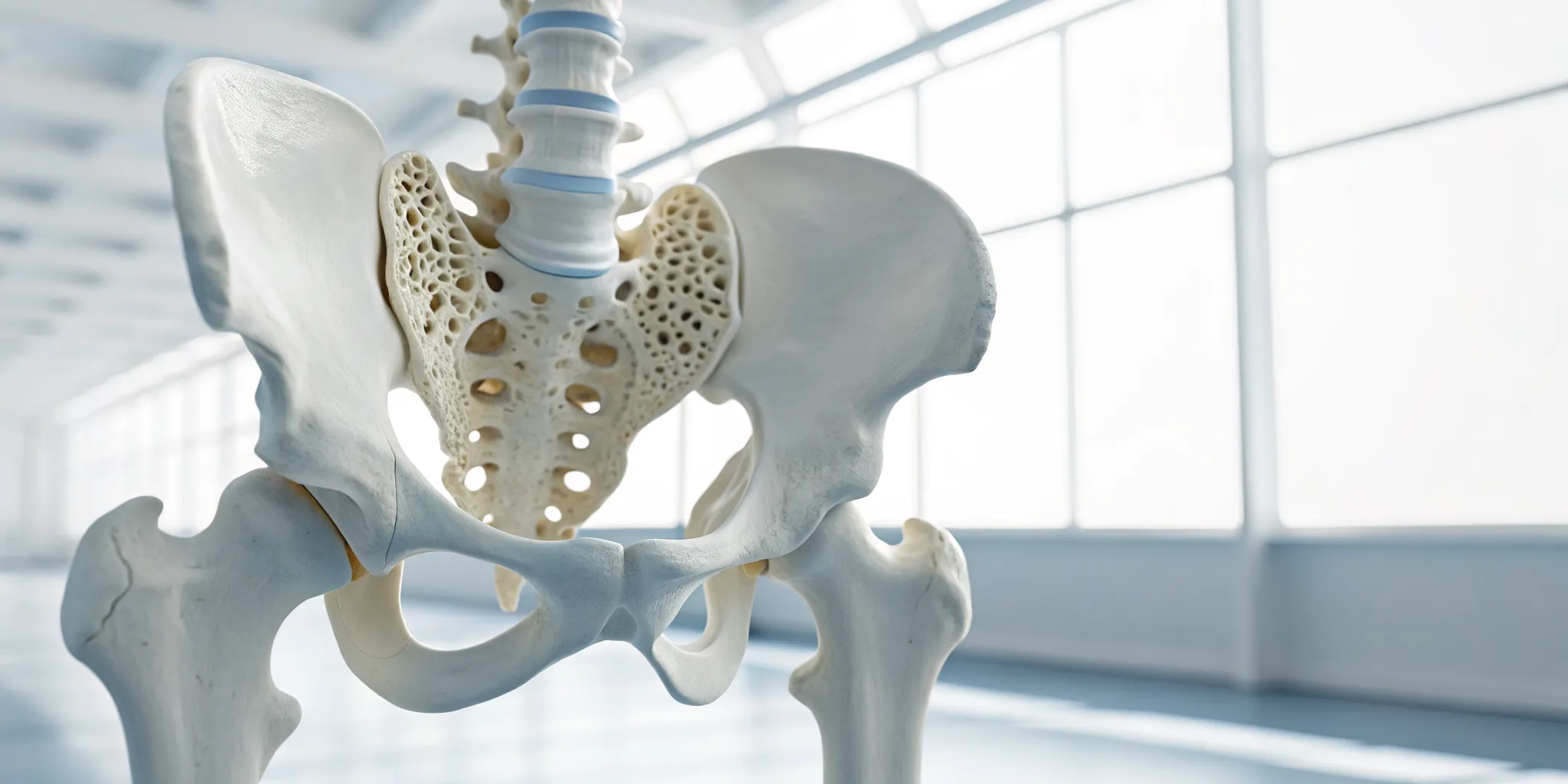
If you’re dealing with persistent, nagging pain in your neck and shoulders, you might be experiencing cervical myofascial pain syndrome. This condition is a common source of chronic discomfort, but it’s often misunderstood. Unlike a simple muscle strain that gets better in a few days, this type of pain centers around specific, hyper-irritable spots in your muscles and the connective tissue, or fascia, that surrounds them. Think of fascia as the thin, web-like casing that holds everything together. When it gets tight and restricted, it can cause a lot of problems. Understanding what makes this type of pain unique is the first step toward finding real, lasting relief and getting back to your life.
Trigger Points and Referred Pain, Explained
So, what’s really going on with this condition? The main culprits are things called trigger points. You can think of them as tiny, contracted knots in your muscle tissue that are tender to the touch and can even cause your muscle to twitch. But the trickiest part of these knots is their ability to cause what’s known as referred pain. This means a trigger point in your neck muscle might not just cause pain right there; it can send pain signals to your shoulder, down your arm, or even trigger tension headaches. It’s a confusing sensation that can make it difficult to pinpoint the true source of your discomfort on your own.
How It Differs From Other Types of Neck Pain
It’s easy to lump all neck pain into one category, but it’s important to know that cervical myofascial pain is different from structural problems like a herniated disc or arthritis. Those conditions involve the bones, joints, and discs of your spine. Myofascial pain, however, is primarily a muscle dysfunction issue. It’s often caused by factors that overload your muscles, such as repetitive strain from work, poor posture while sitting at a computer, a previous injury like whiplash, or even chronic emotional stress. Because the root cause is in the muscle tissue itself, the approach to treatment needs to be different, too.
What Does Cervical Myofascial Pain Feel Like?
Trying to describe neck pain can be tricky. Is it a sharp, stabbing sensation, or a dull, constant ache? Cervical myofascial pain has its own unique signature. It originates in the muscles and the connective tissue (fascia) around them, creating a distinct discomfort that often goes beyond a simple "sore neck." Understanding what this pain feels like is the first step toward finding real relief, because it’s not just about the pain itself, but also about the patterns it follows and the other symptoms that can tag along.
How to Recognize Key Symptoms and Pain Patterns
The hallmark of cervical myofascial pain is the presence of "trigger points." Think of these as hyper-irritable knots or tight bands within your neck and shoulder muscles. When you press on one, it’s not just tender at that spot; it can send pain to another area entirely. This is called referred pain. For example, a trigger point in your shoulder might be the real culprit behind your recurring tension headaches. You might feel a deep, aching pain that’s persistent and makes your muscles feel stiff and weak. Our approach to physical medicine focuses on identifying and releasing these trigger points to address the source of your discomfort.
Beyond the Pain: Secondary Symptoms and Complications
Cervical myofascial pain rarely travels alone. You might notice other symptoms that seem unrelated at first. Many people feel distinct "lumps" in their muscles, have a hard time turning their head fully, or find that the pain disrupts their sleep. Sometimes, the pain can even radiate from your neck down into your arms, causing numbness or a tingling sensation. Dizziness and nausea can also occur. Over time, these persistent trigger points can contribute to other chronic issues, including frequent headaches and migraines or even jaw pain (TMJ syndrome). It’s a chain reaction where one problem can easily lead to another.
When to See a Doctor Immediately
It’s tempting to push through neck pain, hoping it will resolve on its own. While rest and gentle massage can sometimes help, you shouldn't ignore pain that sticks around. If your muscle pain doesn't improve with basic self-care, or if it’s getting worse, it’s time to see a healthcare professional. Persistent pain is your body’s way of telling you that something deeper is going on. Getting an accurate diagnosis is crucial for creating a treatment plan that actually works. Don’t resign yourself to living with the discomfort. A comprehensive evaluation can pinpoint the cause and get you on the path to healing. If you're ready to find answers, we're here to help you get started.
What's Causing Your Neck Pain?
That persistent ache in your neck didn't just appear out of nowhere. Cervical myofascial pain is often a complex issue, stemming from a mix of physical events, daily habits, and even your emotional state. Understanding the source of your pain is the first step toward finding real relief. Let's look at some of the most common culprits behind those stubborn knots and tension.
Physical Trauma and Repetitive Strain
A sudden injury, like whiplash from a car accident, is a well-known cause of neck pain. But trauma doesn't always have to be dramatic. The pain can also build up slowly from repetitive strain, which happens when you overuse your neck and shoulder muscles through repeated motions at work or during a hobby. Think about hours spent painting, typing, or working on an assembly line. These actions can create micro-trauma in the muscle fibers, leading to trigger points. Sometimes, this pain is also a signal of underlying spine issues, like problems with your discs or joints. A thorough evaluation through physical medicine can help pinpoint the exact structural cause.
The Role of Poor Posture and Ergonomics
How are you sitting as you read this? Poor posture is one of the biggest contributors to the neck pain we see today. Constantly looking down at your phone or slouching over a laptop puts immense strain on the muscles in your neck and upper back. Over time, this forward-head posture forces your muscles to work overtime just to hold your head up, leading to fatigue and the formation of painful trigger points. Your workspace setup plays a huge role, too. An office chair without proper support or a computer monitor at the wrong height can force your body into awkward positions, creating the perfect environment for chronic muscle tension and joint pain to develop.
How Stress and Lifestyle Play a Part
Ever notice your shoulders creeping up toward your ears when you're stressed? You're not alone. Emotional and mental stress often shows up as physical tension in the body. When you're anxious or overwhelmed, you might unconsciously clench your jaw or tighten your neck and shoulder muscles. Holding this tension for long periods can create and aggravate trigger points. Beyond stress, other lifestyle factors like poor sleep, a diet lacking in key nutrients, or a lack of regular movement can make your muscles more susceptible to pain and inflammation. Addressing these elements is a key part of a holistic approach to finding lasting relief from neck pain.
Getting a Diagnosis for Cervical Myofascial Pain
Getting a clear diagnosis for cervical myofascial pain is the first step toward real relief. Unlike issues that show up clearly on an X-ray, this condition requires a more hands-on approach. A skilled practitioner will combine a detailed physical exam with a thorough understanding of your health history to connect the dots. It’s a process of both careful investigation and ruling out other potential problems to pinpoint the true source of your discomfort.
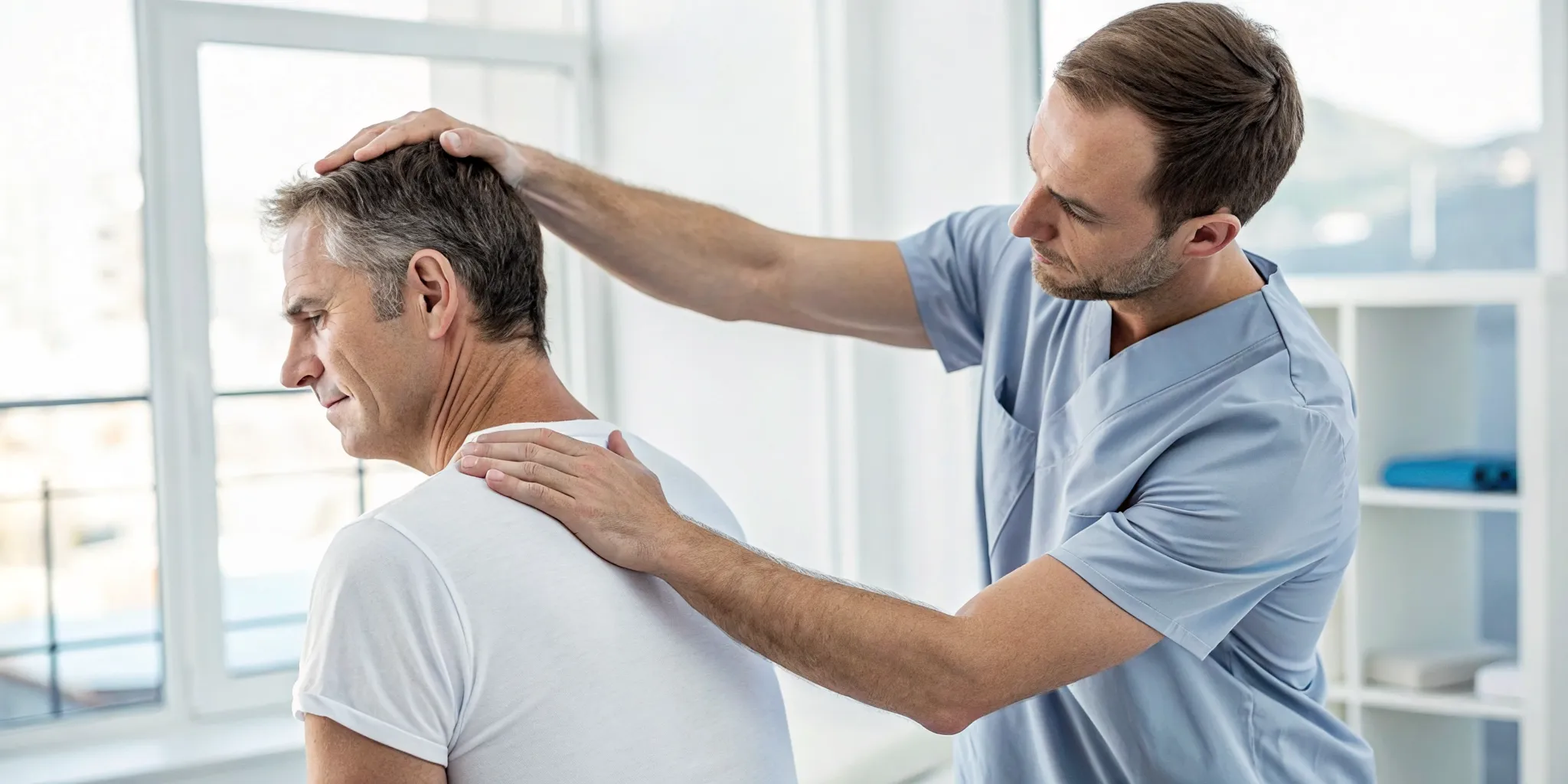
The Physical Exam: Finding Trigger Points
The cornerstone of diagnosing cervical myofascial pain is a detailed physical exam focused on finding trigger points. These are essentially small, tight knots within your muscle fibers that are tender to the touch. When pressed, they don't just hurt at the site of the knot; they can also cause "referred pain," which is pain that shows up in a different, seemingly unrelated area. For example, a trigger point in your shoulder might be the real cause of your tension headache. Our practitioners are trained to locate these specific points in your neck and upper back, helping to map out your unique pain patterns and confirm a diagnosis. This hands-on physical medicine approach is crucial for understanding exactly what's going on.
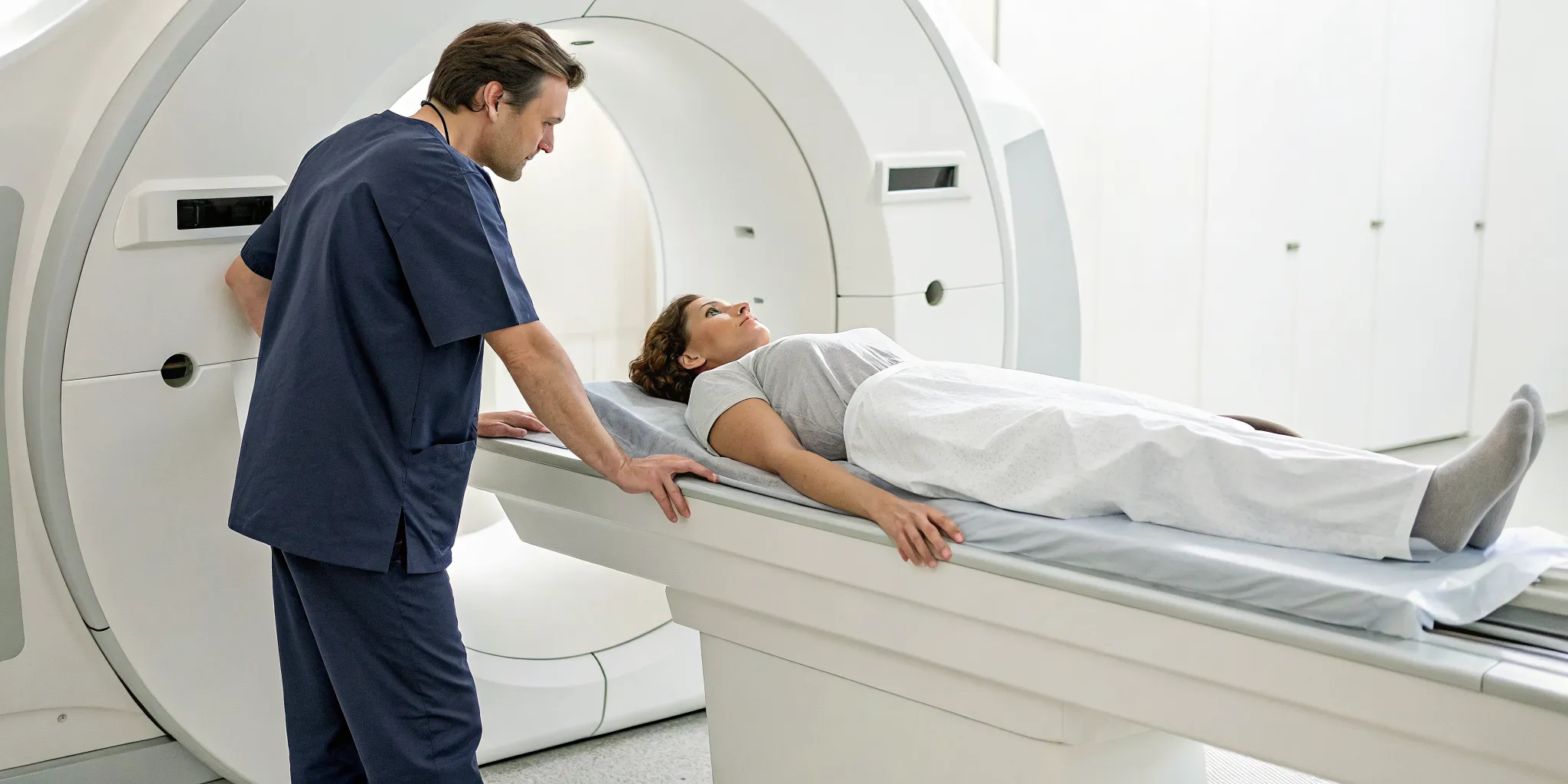
Using Imaging to Rule Out Other Conditions
You might be wondering if an MRI or X-ray can diagnose myofascial pain. The short answer is no. These imaging tests are designed to see bones, discs, and nerves, but they can't visualize the tight bands of muscle that define this condition. So, why would a doctor order one? Imaging is primarily used to rule out other conditions that can cause similar symptoms, like a herniated disc, arthritis, or a pinched nerve. Getting a "clear" MRI can feel frustrating, but it's actually valuable information. It tells us that the source of your pain is likely muscular, allowing us to focus on the right treatment plan for myofascial pain.
Why It's Often Misdiagnosed
Cervical myofascial pain is one of the most commonly overlooked causes of chronic neck pain. Many people suffer for years without a proper diagnosis simply because their imaging results come back normal. When a scan doesn't show an obvious structural problem, it's easy for the root cause to be missed. This is especially true in conventional medicine, where the focus is often on what can be seen on a test. Because it requires a specialized physical exam, myofascial pain syndrome is frequently underdiagnosed, leaving patients feeling like their pain isn't being taken seriously. A practitioner experienced in musculoskeletal health can recognize the signs and provide the validation and treatment you need.
How to Treat Cervical Myofascial Pain
Finding relief from cervical myofascial pain often involves a combination of strategies tailored to your specific needs. The goal isn't just to soothe the immediate discomfort but to address the underlying causes of your trigger points. From hands-on therapies that release tight knots to exercises that restore proper function, a comprehensive treatment plan can help you get back to feeling your best.
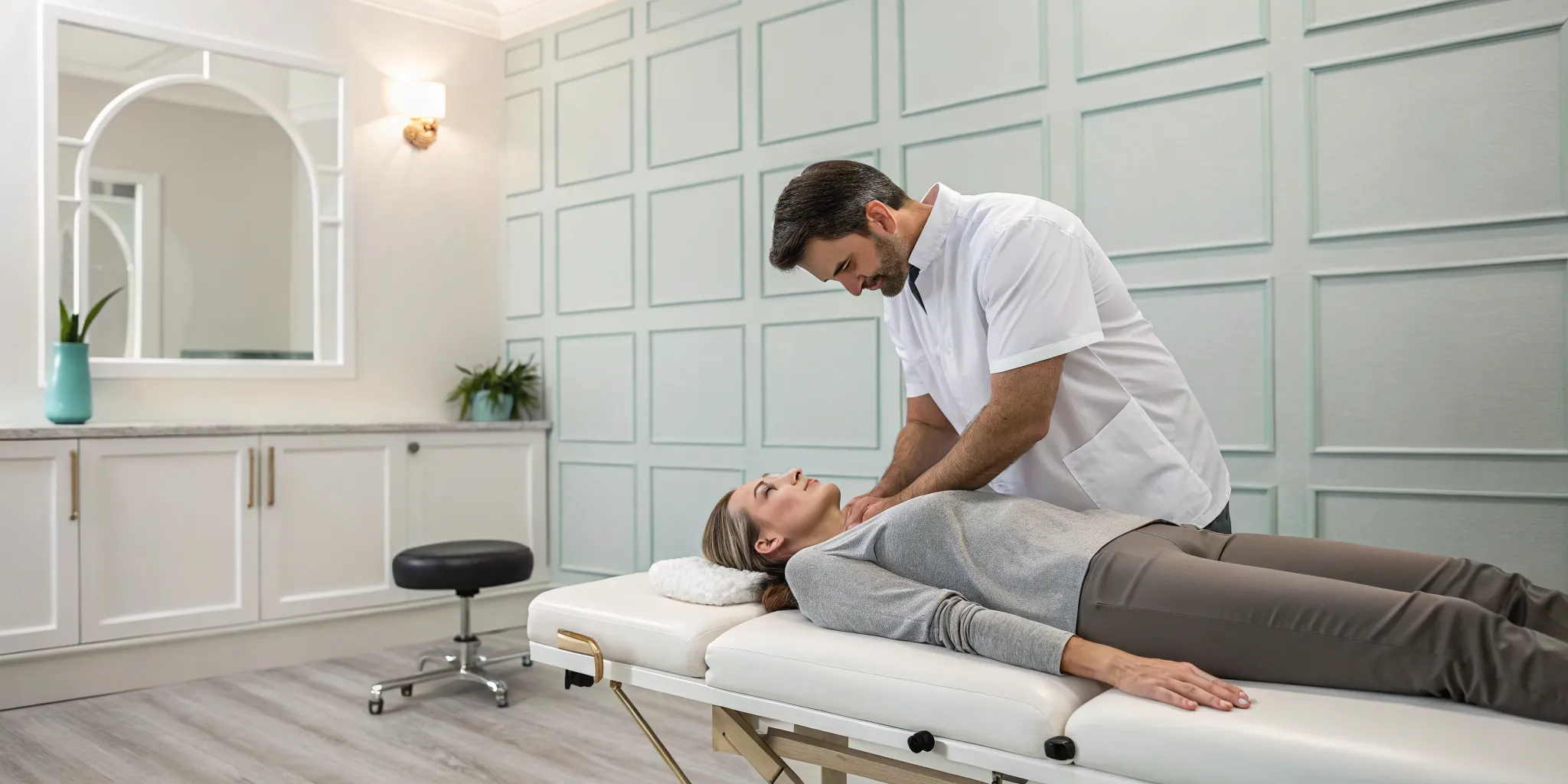
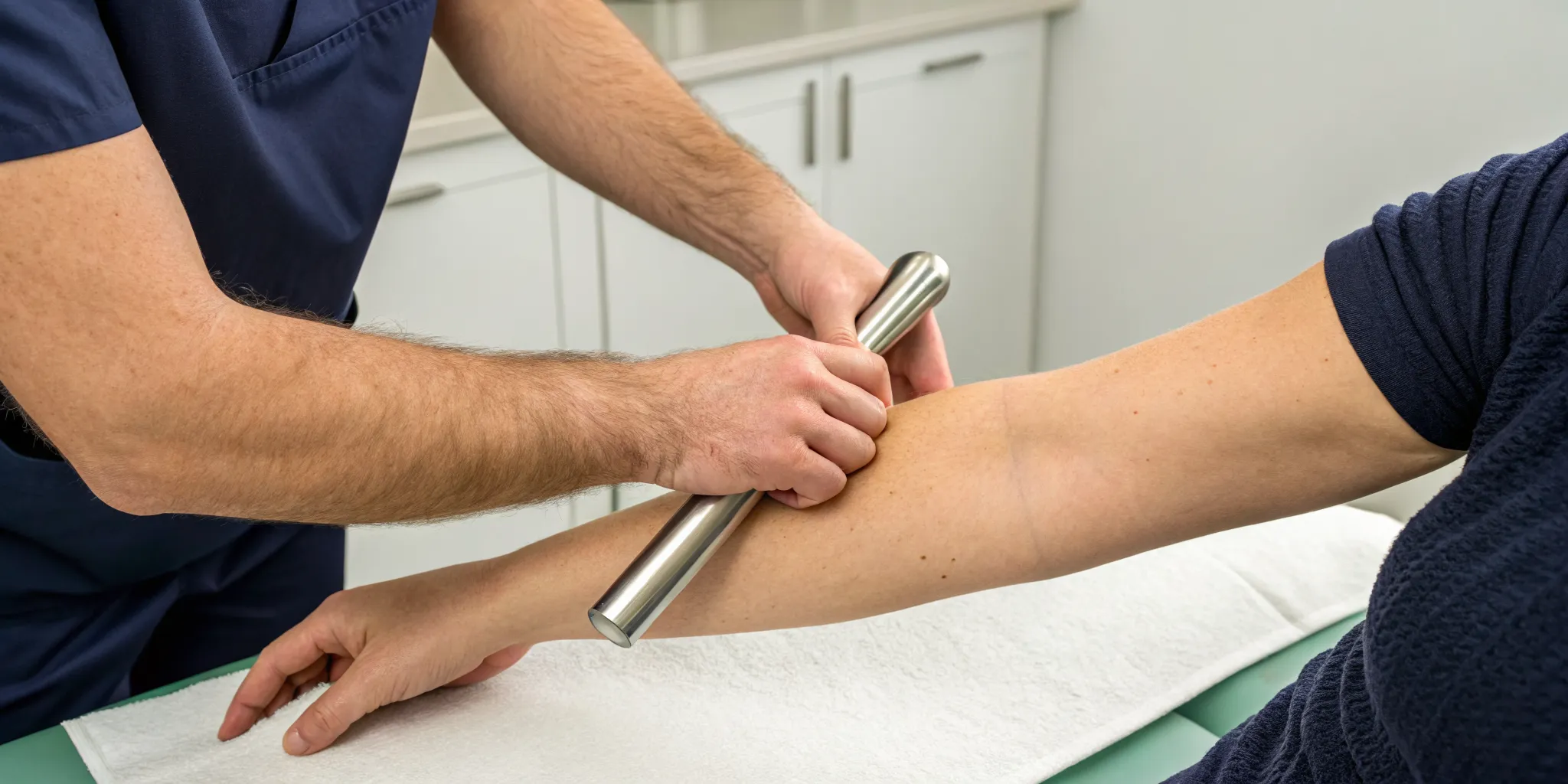
Hands-On Relief: Manual and Myofascial Therapies
Manual therapies are often the first line of defense because they directly target the tight bands of muscle and fascia. A skilled practitioner can identify your unique tension patterns and use specific techniques to release them. Chiropractic adjustments, for example, can correct spinal misalignments that contribute to muscle strain. Myofascial release involves applying gentle, sustained pressure to the connective tissue, helping to ease pain. These non-invasive treatments are part of a holistic physical medicine approach that focuses on restoring your body’s natural alignment and function, providing lasting relief without medication.
Physical Therapy and Rehabilitation Exercises
Physical therapy plays a crucial role in treating current pain and preventing its return. A therapist can guide you through a program of massage, targeted release techniques, and specific stretches to lengthen tight neck muscles. You’ll also learn strengthening exercises to better support your head and neck, which is essential for long-term stability. A major focus of rehabilitation is improving your posture. By becoming more aware of how you sit, stand, and move, you can reduce the daily strain on your neck muscles. This active approach empowers you to take control of your recovery and build resilience against future flare-ups.
Medications and Injection Options
In some cases, medication can help manage symptoms while you pursue other therapies. Your doctor might suggest over-the-counter pain relievers like ibuprofen to reduce inflammation. For more persistent pain, muscle relaxers or certain antidepressants may be prescribed to calm overactive muscles and nerves. For stubborn trigger points, injections can offer direct relief. A practitioner might inject a local anesthetic to break the pain cycle. Another effective technique is dry needling, where a thin needle is inserted into the trigger point to release tension. These options are typically used as part of a broader treatment plan.
A Functional Medicine Approach to Neck Pain
Traditional treatments for neck pain often focus on the site of the pain itself, using things like massage or medication to relieve tight muscles. While these can provide temporary relief, they don’t always address the reason the muscles became tight in the first place. This is where functional medicine comes in. Instead of just treating the symptom (the pain), we look at the whole picture of your health to find and address the root cause.
A functional medicine approach recognizes that your neck pain isn't happening in isolation. It could be connected to your diet, stress levels, gut health, or even hormonal imbalances. By understanding these connections, we can create a personalized plan that not only eases your current pain but also helps prevent it from coming back. It’s about restoring balance to your entire system so your body can heal itself.
Finding the Root Cause Beyond Muscle Tension
It’s easy to assume your neck hurts simply because you strained a muscle. While overuse or injury are common culprits, they often aren't the full story. Sometimes, cervical myofascial pain is a reaction to deeper issues within the spine, like problems with your facet joints or discs. A functional medicine practitioner digs deeper to ask why your muscles are so vulnerable to strain. We investigate underlying factors like chronic inflammation, nutrient deficiencies, or poor gut health, all of which can make your muscle tissue less resilient and more prone to developing painful trigger points. By identifying these root causes, we can build a more effective and lasting treatment plan.
Using Nutrition to Support Healing
What you eat has a direct impact on pain and inflammation throughout your body. Certain foods, like processed sugars and unhealthy fats, can fuel inflammation and make your neck pain feel worse. On the other hand, a diet rich in anti-inflammatory foods like leafy greens, berries, and fatty fish can help calm your system and support muscle recovery. Specific nutrient deficiencies, such as a lack of magnesium or vitamin D, can also contribute to muscle tightness and pain. We can use targeted nutritional strategies and supplements to give your body the building blocks it needs to repair tissue, reduce inflammation, and keep your muscles functioning smoothly.
How to Address Inflammation and Hormonal Imbalances
If you’re constantly stressed or anxious, you might find yourself unconsciously clenching your jaw or tensing your shoulders, which can lead to trigger points in your neck. This isn't just a bad habit; it's a physiological response. Chronic stress can disrupt your hormones, particularly cortisol, which in turn drives up inflammation and makes you more sensitive to pain. This creates a frustrating cycle where stress causes pain, and pain causes more stress. We work to break this cycle by addressing the conditions we treat at their source, using lifestyle changes, stress-management techniques, and targeted support to restore hormonal balance and reduce inflammation. The goal is to help your muscles relax and function properly again.
Lifestyle Changes to Manage Your Pain
While professional treatments are essential for relief, the small choices you make every day have a huge impact on managing cervical myofascial pain. Your daily habits can either contribute to the cycle of pain or help break it. By making a few strategic adjustments to your workspace, sleep habits, and stress levels, you can create an environment that supports your body’s healing process and prevents future flare-ups. Think of these changes as powerful tools you can use to take back control and find lasting comfort.
Fix Your Workspace and Posture
If you spend hours at a desk, your posture can become a major source of neck strain. Poor posture can lead to the formation of trigger points, which are those tight, painful knots in your muscle fibers. An ergonomic workspace isn't a luxury; it's a necessity for preventing pain. Start by adjusting your monitor so the top of the screen is at or slightly below eye level. Your chair should support the natural curve of your lower back, and your feet should rest flat on the floor. Remember to take short breaks every hour to stand, stretch, and move around. Our physical medicine team can offer personalized guidance on correcting posture and strengthening key muscles.
Choose the Right Pillow and Sleep Position
A painful neck can make getting a good night's sleep feel impossible. You might toss and turn, struggling to find a comfortable position, only to wake up feeling stiff and sore. The right pillow and sleep position are critical for letting your neck muscles rest and recover overnight. Sleeping on your stomach is the worst position for neck pain, as it forces your head to be twisted for hours. Instead, try sleeping on your back or side. Choose a pillow that keeps your head and neck aligned with your spine. A cervical pillow with a contour for your neck or a memory foam pillow that molds to your shape can provide the support you need.
Manage Stress with Relaxation Techniques
Stress and anxiety often cause us to unconsciously tense our muscles, especially in the neck and shoulders. This constant muscle tension can create and aggravate trigger points. Learning how to manage stress is a key part of managing myofascial pain. You don’t need a complicated routine; simple relaxation techniques can make a big difference. Try incorporating a few minutes of deep breathing exercises into your day, practice mindfulness meditation, or go for a gentle walk to clear your head. Addressing the root causes of stress is a core part of functional medicine, helping your body become more resilient to both physical and emotional pressures.
How to Keep Neck Pain From Coming Back
Getting out of pain is a huge relief, but the real goal is to stay that way. Preventing cervical myofascial pain from returning involves being proactive and turning healthy habits into a natural part of your routine. It’s about making small, consistent efforts that add up to long-term wellness. By focusing on movement, your daily environment, and a solid maintenance strategy, you can take control of your neck health and keep discomfort from creeping back into your life.
Incorporate Daily Stretches and Exercises
Gentle, consistent movement is one of your best defenses against recurring neck pain. Think of it as daily maintenance for your muscles. Simple stretches, like slowly tilting your head from side to side or gently tucking your chin to your chest, can release tension and improve flexibility. Strengthening the muscles in your neck and upper back provides better support for your head, reducing strain on the cervical spine. Our approach to physical medicine often includes a personalized plan of stretches and exercises designed to restore balance and function. The key is consistency; just a few minutes each day can make a significant difference in keeping your neck muscles relaxed and resilient.
Build Better Habits at Work
Your work environment can either help or hurt your neck. If you spend hours at a desk, small adjustments can have a big impact. Position your computer monitor at eye level so you aren't constantly looking down. Make sure your chair provides good lumbar support, and keep your feet flat on the floor. It’s also important to take frequent breaks. Set a timer to remind yourself to get up, walk around, and stretch every 30 to 60 minutes. These simple ergonomic adjustments help you maintain a neutral posture and prevent the repetitive strain that often leads to trigger points and pain flare-ups.
Create a Long-Term Maintenance Plan
True prevention goes beyond daily habits. A long-term maintenance plan helps you stay ahead of pain and address underlying issues before they become major problems. This might include regular check-ins with a professional who understands your body and your history. Treatments like chiropractic care can be incredibly effective for managing muscle tension and ensuring your spine is properly aligned, which helps prevent future flare-ups. Working with a practitioner to create a personalized strategy is the best way to manage the conditions we treat at their source. This proactive approach ensures you’re not just reacting to pain but actively building a foundation for lasting health.
When Is It Time to See a Professional?
Trying to manage neck pain on your own can be frustrating. You might wonder if the ache will go away with a little more time, a new pillow, or a few stretches. While self-care is a great first step, there comes a point when it’s not enough. If your pain lingers for more than a couple of weeks, gets worse, or starts interfering with your daily activities like working, sleeping, or enjoying your hobbies, it’s a clear signal that your body needs more support.
Ignoring persistent pain won’t make it disappear. In fact, it can often lead to more complex issues down the road. A professional evaluation is the best way to get an accurate diagnosis and understand what’s truly causing your discomfort. At Ascend Functional Health, we look beyond the symptoms to create a personalized plan that addresses the root of the problem. Getting expert guidance helps you move from simply managing pain to actively healing, so you can get back to feeling your best. If you're unsure whether your symptoms warrant a visit, it's always better to get it checked out.
Red Flags: Symptoms That Need Immediate Attention
Most neck pain is related to muscle strain, but it’s important to recognize when your symptoms might point to something more serious. While rare, severe neck pain can be a sign of an underlying condition that needs prompt medical care. Think of these as "red flags" that tell you to stop guessing and see a doctor right away.
You should seek immediate medical attention if your neck pain is accompanied by:
- Fever, chills, or a severe headache
- Numbness, weakness, or tingling that radiates down your arms or legs
- Unexplained weight loss
- Loss of bladder or bowel control
- Pain that is severe, constant, and gets worse at night
If your muscle pain simply isn't getting better with rest, massage, or other home remedies, it's time to schedule a consultation.
Why Early and Comprehensive Treatment Matters
When you’re dealing with persistent pain, it’s tempting to put off seeing a professional. But waiting can make things worse. Getting treatment early helps stop the pain from spreading and becoming a long-term, chronic problem. The longer you live with pain, the more it can impact your daily life, affecting everything from your mood to your ability to work and sleep.
The good news is that the outlook for cervical myofascial pain is generally positive with the right treatment plan. An early and thorough evaluation allows us to pinpoint the root cause of your pain, whether it’s a postural issue, an old injury, or an underlying imbalance. By addressing the source, our Physical Medicine approach provides more than just temporary relief. It sets you on a path toward lasting healing and helps prevent the pain from coming back.
Related Articles
- How a Chiropractor Helps Neck Pain and Headaches
- How to Choose the Right Neck Strain Doctor
- Spinal Narrowing Neck: Symptoms & Treatments
Frequently Asked Questions
How can I tell if my neck pain is myofascial pain or just a simple muscle strain? A typical muscle strain from sleeping wrong or a tough workout usually feels better within a few days. Cervical myofascial pain is different; it's a chronic condition that sticks around. The key distinction is the presence of trigger points, which are specific, tender knots in your muscles. These knots don't just hurt where they are located; they can send pain to other areas, like your head or down your arm, a sensation known as referred pain.
Why didn't my MRI or X-ray show the cause of my pain? This is a very common and frustrating experience. Imaging tests like MRIs and X-rays are excellent for looking at bones, discs, and nerves, but they can't see the soft tissue details of a muscle knot or tight fascia. A "normal" scan is actually helpful information, as it allows us to rule out structural problems like a herniated disc and confirms that the source of your pain is likely muscular in nature.
Can I treat this pain on my own with stretching and better posture? Improving your posture and incorporating gentle stretches are crucial for long-term management and prevention. However, they often aren't enough to resolve the problem on their own. Deep-seated trigger points usually require hands-on, professional treatment to release them effectively. Think of lifestyle changes as essential maintenance that supports the foundational work done through targeted therapies.
How is a functional medicine approach different from just getting a massage for my tight muscles? A massage can provide wonderful, immediate relief by relaxing tense muscles, but it primarily addresses the symptom. A functional medicine approach asks why your muscles are so tight in the first place. We investigate underlying factors like chronic inflammation, nutrient deficiencies, or hormonal imbalances that could be making your muscles more prone to developing trigger points. The goal is to correct the root cause for more lasting relief.
What's the most important first step if I suspect I have this condition? The best first step is to get a comprehensive evaluation from a healthcare professional who is experienced in diagnosing musculoskeletal conditions. Self-diagnosing can lead to frustration and ineffective treatments. A proper diagnosis will confirm the source of your pain and allow for a personalized treatment plan that addresses your specific needs, helping you find the most direct path to feeling better.