When you receive a test result that indicates low bone density, the conventional approach often jumps straight to medication. But that can feel like putting a bandage on a problem without understanding what caused it in the first place. At Ascend, we see a low bone density test result not as a diagnosis, but as a critical clue. It’s the "what," but our focus is on discovering the "why." Is it a nutritional deficiency? A hormonal imbalance? An issue with gut health affecting nutrient absorption? We use your results as the starting point for a deeper investigation to address the root cause and help your body rebuild strength from within.
Key Takeaways
- Get a Baseline for Your Bone Health: A bone density test is a quick, non-invasive way to measure your bone strength and catch potential issues like osteoporosis before a fracture occurs. While general age guidelines exist, personal risk factors like family history or certain health conditions may mean you should consider testing earlier.
- Use Your Results as a Starting Point: Your test results provide a clear picture of where your bone health stands, from normal to low bone mass (osteopenia) or osteoporosis. This information empowers you to work with your doctor on a proactive plan that includes diet, weight-bearing exercise, and other lifestyle changes.
- Look Beyond the Scan to Find the "Why": Low bone density is a symptom, not the root problem. A functional medicine approach uses your test results to dig deeper, investigating underlying causes like hormonal imbalances or nutrient deficiencies to create a truly personalized plan for building stronger bones.
What Is a Bone Density Test?
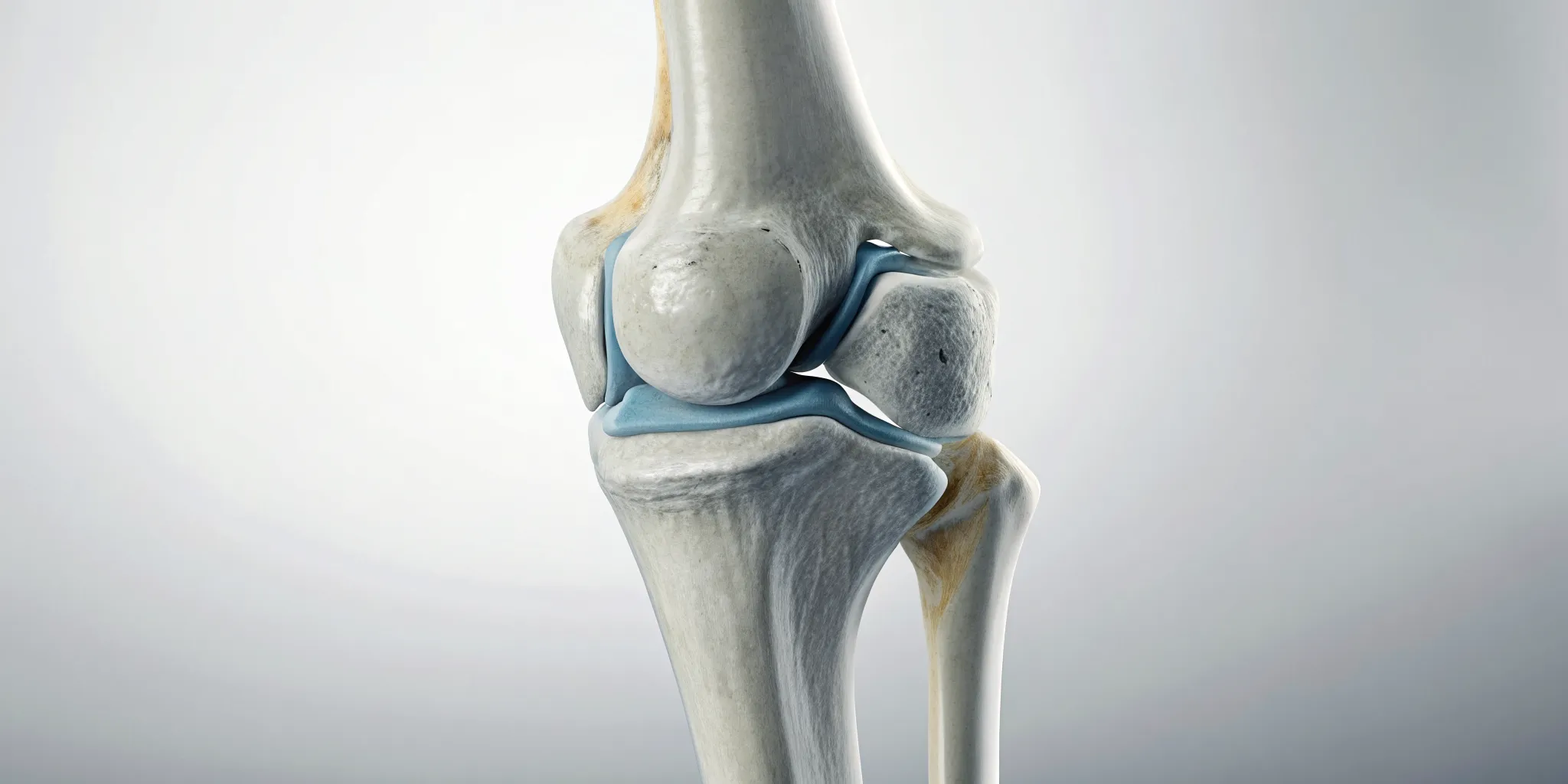
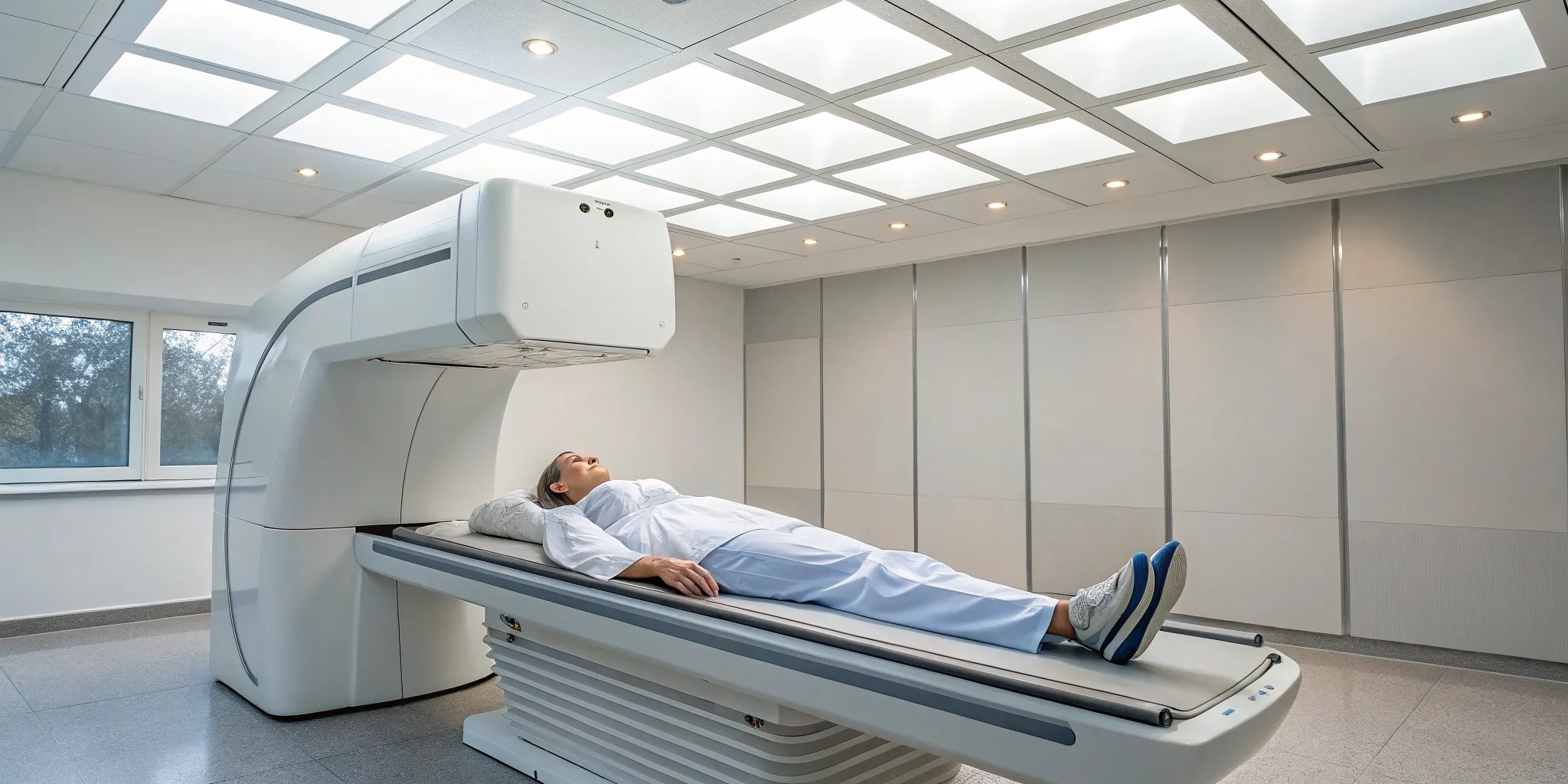
Ever wondered about the true strength of your bones? That’s exactly what a bone density test can tell you. Think of it as a quick, painless snapshot of your bone health. This simple imaging procedure, most commonly known as a DEXA scan, uses low-level X-rays to measure the amount of calcium and other minerals packed into your bones. The test usually focuses on areas most prone to fractures, like your hip and spine.
The main goal is to catch bone loss early. It’s the gold standard for diagnosing conditions like osteoporosis, a disease that weakens bones and increases your risk of unexpected fractures. Identifying low bone density before a break happens allows you to take proactive steps to protect your skeletal structure. At Ascend, our approach to Physical Medicine is all about understanding the complete picture of your health. Knowing your bone density is a critical piece of that puzzle, helping us create a personalized plan to keep you strong, mobile, and active for years to come.
How DEXA Scans Measure Bone Health
So, how does this technology actually work? DEXA stands for dual-energy X-ray absorptiometry, and it’s considered the most accurate method for measuring bone mineral density (BMD). During the scan, two different X-ray beams, one high-energy and one low-energy, are passed through your body. By measuring the absorption of each beam, the machine can calculate the precise density of your bones with incredible accuracy.
This detailed measurement gives your healthcare provider a clear picture of your bone strength. The results from a DEXA scan are essential for evaluating your overall bone health and determining your personal risk of fractures, allowing for early and effective intervention.
The Testing Process, Step by Step
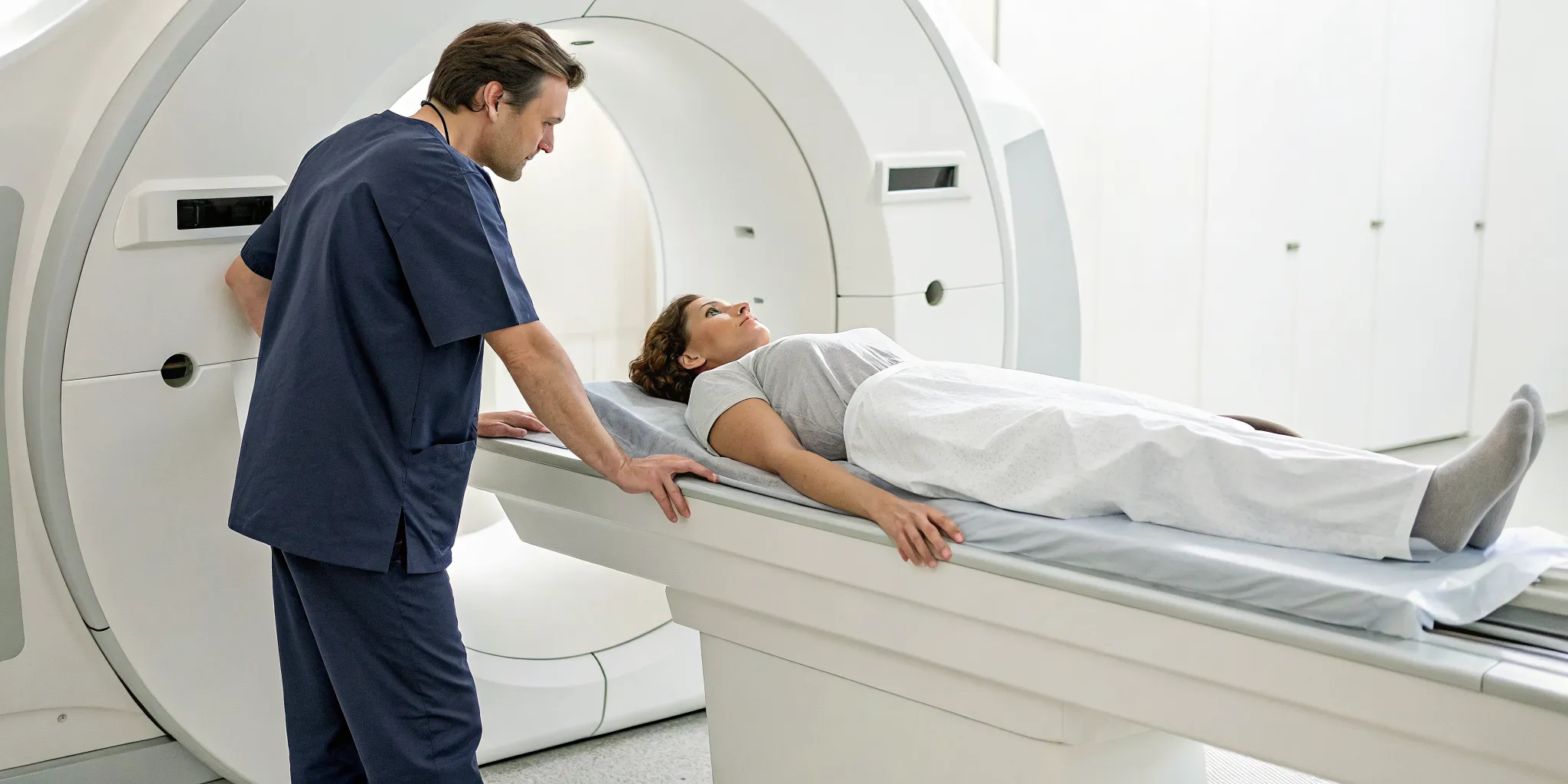
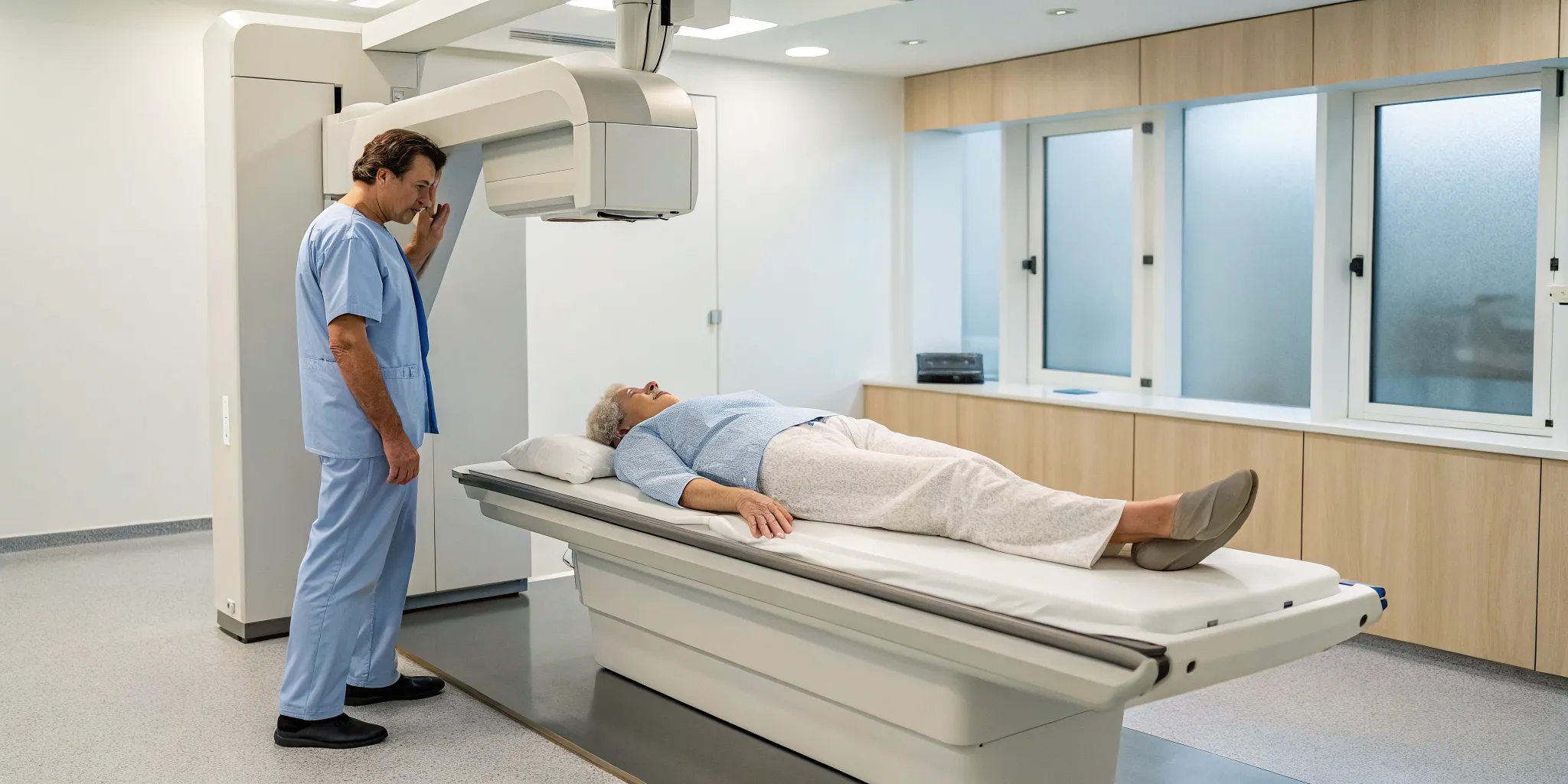
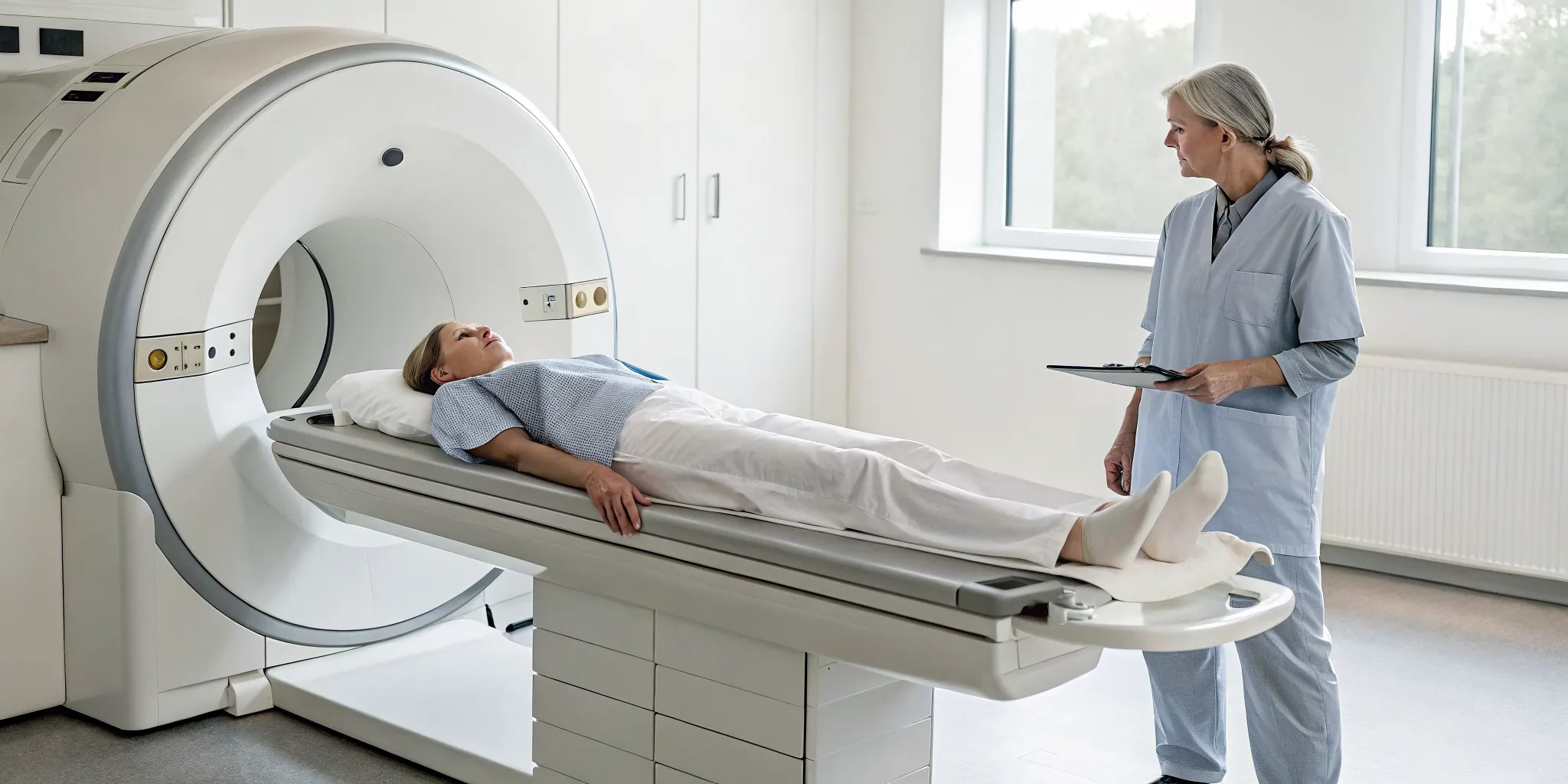
If you’re scheduled for a bone density test, you can rest easy knowing the process is incredibly straightforward. The entire scan typically takes only 10 to 30 minutes. You’ll be asked to lie comfortably on a padded table while a mechanical arm passes slowly over your body, scanning the targeted areas.
It’s completely painless, and the only real requirement is that you stay still during the scan. Your technician might ask you to hold your breath for a few seconds to ensure the images are clear. A bone density test requires very little preparation, making it a simple but powerful tool for assessing your health. If you have any questions about the process, we’re always here to help.
Should You Get a Bone Density Test?
Deciding whether to get a bone density test can feel like just another item on a long health to-do list. But it’s a key step in understanding your long-term health, especially as you get older. Think of it as a proactive check-in on your body’s foundation. While there are general guidelines, your personal health history plays a huge role. Certain risk factors, lifestyle habits, and medical conditions can make an earlier screening a smart move. Let’s walk through who should consider a test and why, so you can feel confident talking to your doctor about your bone health.
Age Guidelines for Women and Men
As a general rule, most women should get a bone density scan starting at age 65, and men should consider one at age 70. This is because bone loss naturally accelerates as we age, and these milestones are when the risk for osteoporosis becomes more significant. However, age isn't the only factor. If you're over 50 and have broken a bone, it’s a good idea to get a baseline scan. These guidelines are a great starting point, but a functional medicine approach can help you understand your personal risk profile and decide on the right timing for you.
Risk Factors That Call for Earlier Testing
You don’t have to wait until your late 60s to think about bone health. Certain factors can increase your risk of bone loss much earlier in life. If you have a very low body weight or have lost more than half an inch in height within a year, it might be time for a test. A family history of osteoporosis is another important clue. Your daily habits matter, too. A lifestyle with little physical activity, long-term tobacco use, or heavy alcohol consumption can weaken your bones over time. Being aware of these risks allows you to take control and get screened sooner rather than later.
Health Conditions That Can Weaken Bones
Sometimes, bone loss is a side effect of another health issue or medication. Certain autoimmune diseases, for example, can interfere with your body’s ability to build and maintain strong bones. The same goes for having low Vitamin D levels, which is essential for calcium absorption. Some common medications, including long-term use of corticosteroids (like prednisone) or certain acid reflux drugs, can also contribute to weaker bones. Understanding these connections is central to our work at Ascend. By looking at your complete health picture, we can identify the root causes of your symptoms and create a plan that supports your entire body, bones included.
How to Prepare for Your Bone Density Test
Getting ready for a bone density test is simple and doesn't require much effort. Knowing what to do beforehand can make the entire process feel smooth and stress-free. A few small adjustments the day before and the day of your appointment are all it takes to ensure your results are as accurate as possible. From what you wear to the supplements you take, here’s a quick guide to help you prepare for your test with confidence.
Your Pre-Test Checklist
To get the most accurate reading, there are a few things to keep in mind before your appointment. First, let your doctor know if you’ve recently had a test that involved a barium exam or a contrast dye injection, as these can interfere with the results. It’s also important to avoid taking calcium supplements for at least 24 hours before your scan. On the day of the test, opt for loose, comfortable clothes without any metal. Think sweatpants or leggings instead of jeans with zippers, belts, or buttons. It’s best to leave jewelry at home, too.
What to Expect on Test Day
The bone density test itself is quick and painless. You’ll be asked to lie down on a padded table, and a mechanical arm will slowly pass over your body to scan specific areas. The most common and accurate method is the central DEXA (dual-energy X-ray absorptiometry) scan, which typically examines the bones in your lower spine and hip. The entire process is non-invasive and usually takes only about 10 to 30 minutes to complete. You can just relax while the machine does its work.
Costs and Insurance Coverage
The cost of a bone density test can vary, so it’s a good idea to check with your insurance provider beforehand to understand your coverage. Many plans cover bone density screening, especially if you meet certain risk factors. For example, Medicare Part B covers the full cost of the test every 24 months for eligible individuals. If you have questions about your insurance or the testing process, our team at Ascend Functional Health is here to help. Feel free to contact our Tampa office for more information.
What Do Your Bone Density Results Mean?
Getting your test results can feel a little intimidating, but they’re actually pretty straightforward once you know what to look for. Your report gives you a clear picture of your bone health, and we’re here to help you make sense of it all. The main things to focus on are your T-score and Z-score. These numbers tell you how your bone density compares to a standard benchmark. Think of it as a snapshot that helps us understand your risk for fractures and guides our next steps together. It’s not just about the numbers; it’s about what we do with that information to support your long-term health and keep you feeling strong and active.
Decoding Your T-Score and Z-Score
Your report will feature two key numbers: a T-score and a Z-score. The T-score is the most common one we look at, especially for postmenopausal women and men over 50. It compares your bone density to that of a healthy 30-year-old, which is when bone mass is typically at its peak. The Z-score, on the other hand, is used for premenopausal women, men under 50, and children. This score compares your bone density to the average for someone of your own age, sex, and ethnicity. In both cases, a higher number is better, indicating stronger, denser bones that are less likely to fracture.
From Normal to Osteoporosis: Understanding the Ranges
When looking at your T-score, the numbers fall into specific ranges that tell us about your bone health. A score of -1.0 or above is considered normal and healthy. If your score is between -1.0 and -2.5, it indicates low bone density, a condition called osteopenia. This isn't osteoporosis yet, but it’s a sign that you have a greater risk of developing it down the road. A T-score of -2.5 or lower suggests that you likely have osteoporosis, meaning your bones have become more fragile and susceptible to fractures. Understanding where you fall on this spectrum is the first step toward creating a personalized plan to protect your bones.
Common Myths About Your Results
It’s important to know that while a bone density test can tell you if you have bone loss, it can’t tell you why. This is a crucial distinction. Low bone density is a symptom, not the root problem. Uncovering the underlying cause, whether it’s a nutritional deficiency, a hormonal imbalance, or a gut health issue, is where our approach can truly make a difference. This is why we often use Functional Medicine to dig deeper with more in-depth testing. Another practical point to remember is that insurance coverage for these tests can vary, so it’s always a good idea to check with your provider beforehand to understand your benefits.
What to Do If Your Bone Density Is Low
Receiving a low bone density result can feel unsettling, but it’s important to see it for what it is: a powerful piece of information. This result isn’t a final diagnosis but a starting point. It gives you a clear opportunity to take proactive steps to protect your bones and reduce your risk of fractures down the road. Think of it as an early warning system that allows you to make meaningful changes.
The great news is that there is so much you can do to support your bone health. From simple lifestyle adjustments in your diet and exercise routine to more targeted treatments, you have options. A functional medicine approach, like the one we use at Ascend, focuses on understanding the root cause of your bone loss. We look beyond the symptoms to see what’s really going on with your body, whether it’s a nutritional deficiency, a hormonal imbalance, or gut health issues that affect nutrient absorption. This allows us to create a plan that’s tailored specifically to you.
Your First Steps After Getting Your Results
When you get your results, take a deep breath. The first and most important step is to schedule a follow-up appointment to discuss what your T-score and Z-score actually mean for you. Knowing your numbers is the key to staying ahead of osteoporosis and protecting your long-term health. During this conversation, you can get a clear picture of your personal fracture risk and begin to map out a plan.
This is your chance to ask questions and work with a professional to create a personalized plan that addresses your unique health profile. Instead of just treating the number, we can investigate why your bone density is low in the first place and build a strategy that supports your entire body.
Lifestyle Changes for Stronger Bones
Your daily habits have a huge impact on your bone health. Two of the most effective areas to focus on are diet and exercise. Your doctor will likely recommend incorporating more weight-bearing exercises into your routine. This doesn't have to mean heavy lifting; activities like walking, dancing, jogging, and climbing stairs all count. These movements put gentle stress on your bones, which signals your body to build them up stronger.
On the nutrition side, getting enough calcium and vitamin D is essential. You can find calcium in dairy products like milk and yogurt, leafy greens like spinach and collards, and fortified foods. Vitamin D, which helps your body absorb calcium, is best sourced from sunlight, but you can also find it in fatty fish and fortified milk. A holistic health plan can help you identify and fill any nutritional gaps.
Exploring Treatment and Follow-Up Testing
If lifestyle changes aren't enough, your doctor may discuss other options, including medication or targeted supplements. Consider your results a prompt to discuss preventive measures, like adding strength training and specific nutrients like vitamin K to your routine. A functional medicine approach uses in-depth testing to identify deficiencies and create a supplement protocol designed for your body’s specific needs.
You’ll also want to talk about a schedule for follow-up scans. How often you’ll need another test depends on your results and risk factors. Generally, someone at high risk may be re-tested every two years, while those with lower risk might wait much longer. Regular monitoring helps you and your doctor see how well your plan is working and make adjustments as needed.
How Functional Medicine Can Improve Your Bone Health
Getting your bone density test results is an important first step, but what comes next is even more critical. A conventional approach might focus on medication alone, but this often overlooks the underlying reasons why your bones are losing density in the first place. This is where functional medicine shines. Instead of just managing symptoms, we focus on identifying and addressing the root causes of your health concerns.
The functional medicine approach to bone health is a comprehensive strategy that looks at your body as an interconnected system. We know that bone loss isn't just an isolated issue; it can be linked to gut health, nutrient deficiencies, inflammation, and hormonal imbalances. By digging deeper, we can create a personalized plan that supports your body’s natural ability to build and maintain strong, healthy bones for the long haul. This involves a detailed look at your unique physiology to create a strategy that works for you.
Finding the Root Cause of Bone Loss
A bone density test gives us a valuable snapshot of your current bone mass, but it doesn’t tell the whole story. Think of it as the "what," while functional medicine helps us uncover the "why." We use your test results as a starting point to investigate the underlying factors contributing to bone loss. This could be anything from poor nutrient absorption in your gut to chronic inflammation or an undiagnosed autoimmune condition.
To get a complete picture, we often use advanced diagnostic tools beyond a standard DEXA scan. Comprehensive blood panels, stool tests, and assessments for inflammatory markers can reveal the hidden stressors that are impacting your bone health. By identifying these root causes, we can move beyond a one-size-fits-all approach and develop a targeted, effective treatment plan tailored specifically to your body’s needs.
Personalized Nutrition and Supplement Plans
Once we understand the root cause of your bone loss, we can build a personalized nutrition and supplement plan to give your body the tools it needs to rebuild. While getting enough calcium and vitamin D is essential, true bone health is more complex. It also requires other key nutrients like magnesium, vitamin K2, zinc, and collagen, all working together in balance.
We’ll help you create a diet rich in whole, nutrient-dense foods that support bone formation and reduce inflammation. For many people, diet alone isn’t enough to correct deficiencies, which is where targeted supplementation comes in. Based on your lab results, we can recommend specific, high-quality supplements in the right forms and dosages to ensure your body can actually absorb and use them effectively. This personalized strategy helps you build stronger bones from the inside out.
Hormone Balancing and In-Depth Testing
Hormones are powerful chemical messengers that play a critical role in regulating bone turnover, the natural process of breaking down old bone and replacing it with new tissue. As we age, hormonal shifts, especially the decline in estrogen during menopause, can significantly accelerate bone loss. However, other hormones like testosterone, DHEA, and thyroid hormones are also vital for maintaining a strong skeleton.
Our longevity medicine services include in-depth hormone testing to assess your levels and identify any imbalances that could be compromising your bones. Based on these results, we can create a customized plan to restore hormonal harmony. This may involve lifestyle adjustments, targeted nutritional support, or bioidentical hormone replacement therapy (BHRT) to help protect your bones and support your overall vitality.
Related Articles
- Functional Movement Screening: A Complete Guide
- At Home Lab Tests | Alessi Functional Health
- Functional Medicine Page | Alessi Functional Health
- The 5 Best At-Home Estrogen Tests Reviewed
- Comprehensive Blood Work | Alessi Functional Health
Frequently Asked Questions
Is the bone density test painful or unsafe? Not at all. The test is completely painless and non-invasive. You just lie comfortably on a table for a few minutes while a scanner passes over you. While it does use X-rays, the radiation exposure is extremely low, even less than what you’d get on a cross-country flight. It’s considered a very safe and routine procedure for assessing bone health.
What's the real difference between osteopenia and osteoporosis? Think of osteopenia as a warning sign. It means your bone density is lower than the ideal peak for your age, but not low enough to be classified as osteoporosis. It’s a middle ground that signals you have an increased risk for developing osteoporosis later. Osteoporosis is more serious; it means your bone density has dropped to a point where your bones are significantly more fragile and much more likely to fracture.
If my results show low bone density, can I actually reverse it? Yes, you can absolutely improve your bone density. While the term "reversal" can be tricky, you can definitely make your bones stronger and halt further loss. This involves a consistent plan that often includes weight-bearing exercise, a diet rich in bone-building nutrients like calcium and vitamin K2, and targeted supplements. A functional medicine approach helps identify why you're losing bone in the first place, creating a more effective and personalized strategy for rebuilding.
How often will I need to get re-tested? The frequency of follow-up tests really depends on your initial results and personal risk factors. If your bone density is normal or only slightly low, your doctor might suggest waiting several years before your next scan. However, if you have osteoporosis or several risk factors, you’ll likely be re-tested every two years to monitor your progress and see how well your treatment plan is working.
Why look for a "root cause" if I can just take medication for bone loss? Medication can be a helpful tool, but it often just manages the symptom (bone loss) without addressing the reason it's happening. A functional medicine approach digs deeper to find out why your bones are weakening. The cause could be a gut issue preventing you from absorbing nutrients, a hormonal imbalance, or chronic inflammation. By identifying and addressing the root problem, we can create a more sustainable, long-term solution for stronger bones and better overall health.