For years, the advice was simple: once your knee cartilage is gone, it's gone. This left you with two tough choices: live with the pain or face a major surgery. But that's no longer the full story. The game has changed. Advanced cartilage regeneration medicine offers a new path forward, using your body's own powerful healing abilities to restore joint health. These therapies don't just mask the problem; they create the right environment for your body to actually rebuild damaged tissue. It’s a fundamental shift from temporary fixes to lasting solutions.
Key Takeaways
- Healing from within is a real option: Modern regenerative treatments work by concentrating your body's own powerful healing agents—like platelets and growth factors—to repair cartilage damage at its source, offering a way to rebuild tissue rather than just mask pain.
- Your treatment's success depends on your daily habits: The choices you make after a procedure are just as important as the procedure itself. A dedicated physical therapy plan, an anti-inflammatory diet, and managing your weight are crucial for protecting your joint and achieving a lasting recovery.
- A personalized plan is non-negotiable: Every knee injury is different, and the right solution depends on the specific type and extent of your cartilage damage. A thorough evaluation with a specialist is the essential first step to creating a targeted treatment strategy that will work for you.
Why Your Knee Cartilage is Key to Movement
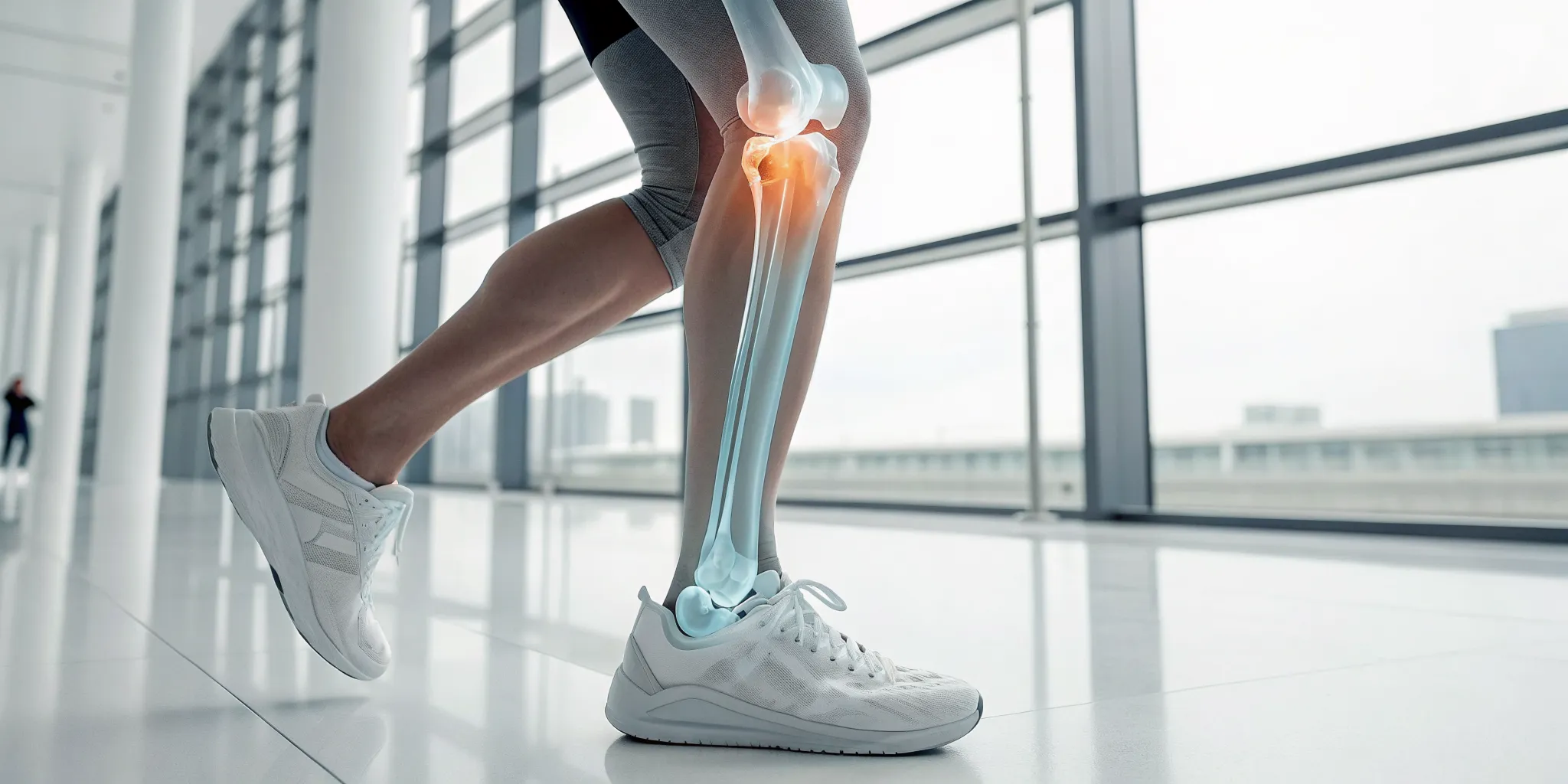
If you’ve ever experienced knee pain, you’ve probably heard the word “cartilage” thrown around. But what is it, really? Think of knee cartilage as your body’s built-in shock absorber and gliding surface, all in one. It’s a firm, flexible tissue that plays a huge role in keeping your knees healthy and moving without pain. Understanding how it works is the first step toward protecting it for the long haul. When this crucial tissue gets damaged, whether from an injury or just daily wear and tear, it can seriously impact your ability to walk, run, and live comfortably. That’s why focusing on cartilage health is so important for your overall mobility and quality of life.
Your Knee's Natural Shock Absorber
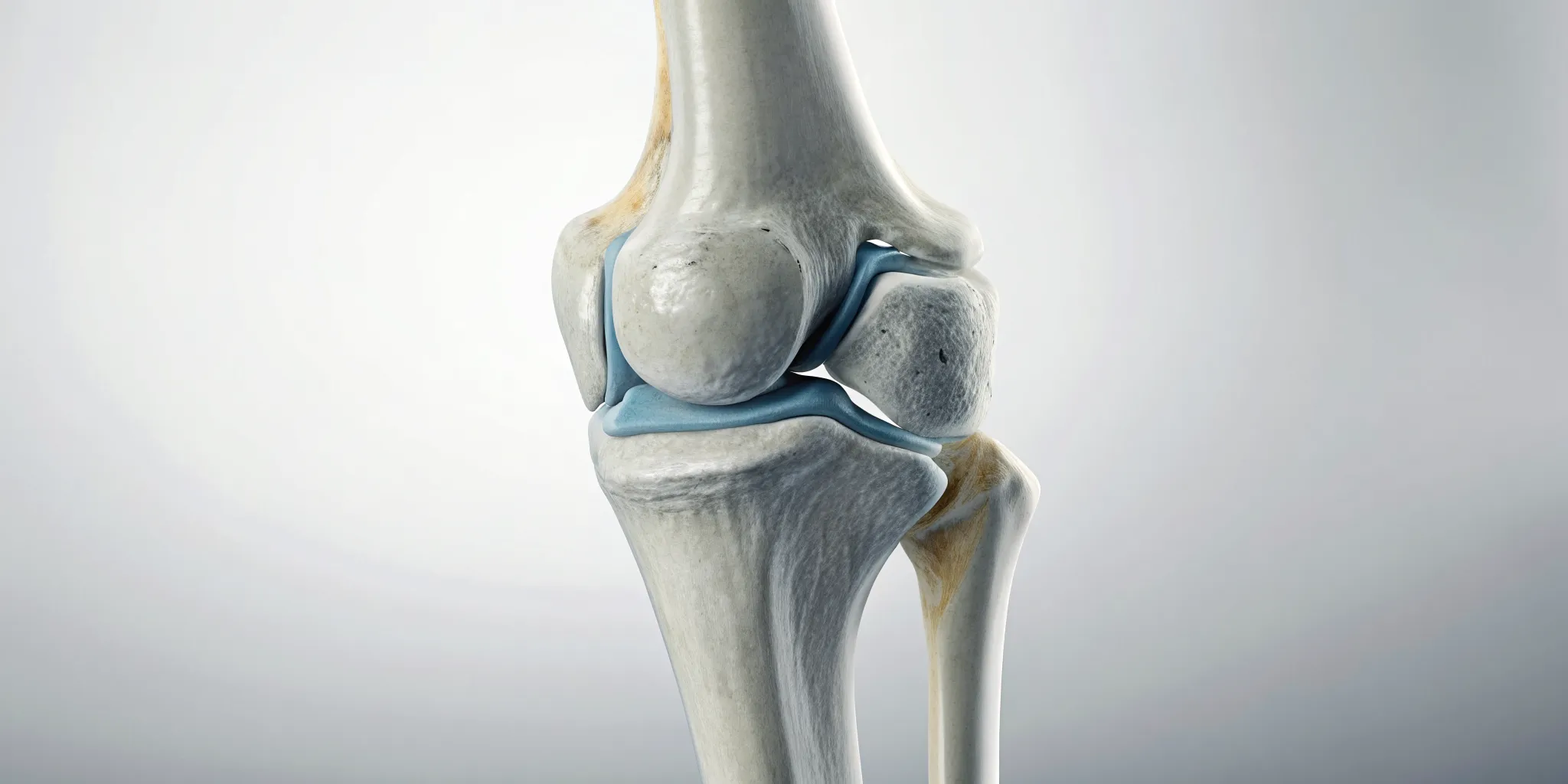
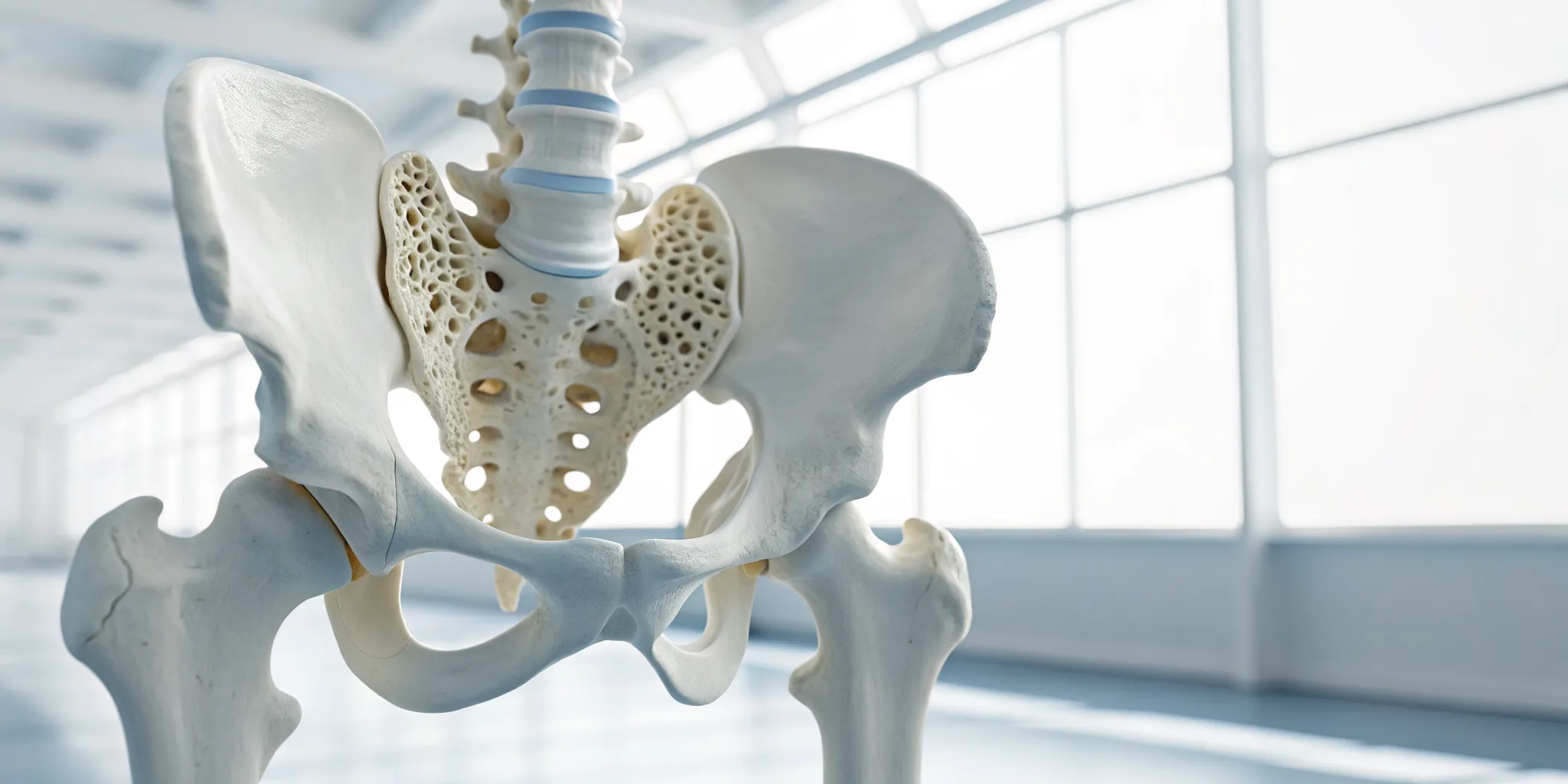
Your knee joint is where your thigh bone (femur) meets your shin bone (tibia). The ends of these bones are covered by a smooth, tough, white tissue called articular cartilage. This covering is incredibly slick, allowing your bones to glide over each other with almost no friction. It also acts as a cushion, absorbing the impact from every step you take, whether you’re walking to the mailbox or running a marathon. Without this protective layer, the simple act of bending your knee would be a painful, grinding motion. This amazing tissue is what makes fluid, seamless physical movement possible.
A Quick Guide to Cartilage Types
Your knee actually has two types of cartilage, and each has a specific job. First, there’s the articular cartilage we just talked about, which coats the ends of your bones for smooth gliding. The second type is the meniscus. You have two of these C-shaped pieces of cartilage in each knee, sitting between the thigh and shin bones. The meniscus acts more like a shock-absorbing pad and stabilizer. It helps distribute your body weight evenly across the joint, preventing too much pressure on any one spot. Together, these two types of cartilage work as a team to keep your knee stable, cushioned, and moving freely.
What Happens When Your Cartilage Wears Down?
When cartilage gets damaged, it can’t protect your bones as effectively. This can happen suddenly from a sports injury or slowly over time from overuse. As the cartilage thins out or tears, you might start to notice symptoms like pain, swelling, and a clicking or catching sensation when you move. Because cartilage doesn’t have its own blood supply, it can’t heal itself very well. If left unaddressed, this damage can expose the underlying bone, leading to chronic pain and inflammation. This progressive wear-and-tear is what defines osteoarthritis, one of the most common conditions we treat that can significantly limit your mobility.
The Widespread Impact of Osteoarthritis
Osteoarthritis isn't just a minor ache that comes with getting older; it's a significant health challenge that touches millions of lives. This condition affects a staggering 20% of the U.S. population, making it one of the most common causes of joint pain. The impact goes beyond personal discomfort, contributing to about $65 billion in direct healthcare expenses each year. It's particularly relevant for anyone who's had a significant joint injury in the past—about half of the people who tear their ACL will develop osteoarthritis in that knee within 15 years. This happens because cartilage, the joint's natural cushion, struggles to heal on its own. The result is often a cycle of chronic pain and inflammation that can make everyday activities difficult, underscoring why proactive joint care is so essential.
Spotting the Signs of Damaged Knee Cartilage
That nagging knee pain can be tough to ignore, especially when it starts interfering with your daily life. But how do you know if it’s just a minor strain or something more serious, like cartilage damage? Understanding the potential causes and recognizing the key warning signs are the first steps toward getting the right kind of help. Your body often sends clear signals when something is wrong; learning to interpret them can make all the difference.
What Causes Cartilage to Break Down?
Knee cartilage damage isn't just for professional athletes. It can happen to anyone from a sudden, acute injury—like a quick pivot during a weekend tennis match—or it can develop slowly from overuse and repetitive stress over time. Think of activities like running on hard surfaces or jobs that require constant squatting. These actions can gradually wear down the smooth, protective cartilage in your knee joint. This can lead to significant discomfort and make it harder to move freely, impacting everything from your workout routine to simply walking up the stairs.
The Link Between Joint Injuries and Arthritis
It’s a common story: a knee injury in your twenties comes back as persistent joint pain in your forties. This isn't a coincidence; there's a direct line connecting past trauma to future arthritis. When an injury damages your cartilage, it disrupts the smooth, protective surface that allows your joint to move freely. The real challenge is that cartilage has a very limited ability to heal itself because it lacks a direct blood supply. That initial damage doesn't just repair and go away. Instead, it can set off a chain reaction of gradual wear and tear, leading to the inflammation and discomfort of osteoarthritis. Understanding this connection is crucial because it highlights why addressing joint health with a comprehensive physical medicine approach is so important for your long-term mobility.
Don't Ignore These Knee Symptoms
If your knee cartilage is damaged, it will likely let you know. The most common complaint is a persistent, dull ache that gets worse with activity, often accompanied by swelling. You might also notice other distinct sensations. Many people report a feeling of their knee "locking up," "catching," or even "giving way" unexpectedly. A clicking or grinding noise when you bend your knee is another tell-tale sign. These symptoms can seriously affect your mobility and quality of life, so it's important not to dismiss them as normal aches and pains.
Is It Age or an Injury?
It’s easy to chalk up knee pain to getting older, but that’s not always the full story. While age-related wear and tear is a factor, a specific injury can accelerate cartilage damage, especially if it isn't allowed to heal properly. An untreated injury can lead to further problems in the surrounding bone and tissue, making recovery more complex. Symptoms like sharp pain, tenderness, stiffness, and swelling could point to a specific tear, such as a meniscus tear. Getting a clear diagnosis is key to understanding the root cause of your pain and exploring effective regenerative medicine options.
Rebuilding Cartilage: Your Non-Surgical Options
If you're dealing with knee pain from cartilage damage, the thought of surgery can be daunting. The good news is that you might not have to go under the knife. The field of regenerative medicine is making incredible strides, offering non-surgical treatments that work with your body’s natural healing abilities to repair tissue, reduce pain, and improve how you move. These approaches focus on addressing the root cause of the problem rather than just managing symptoms, which is a core part of our philosophy at Ascend Functional Health.
Instead of invasive procedures with long recovery times, these treatments often involve simple injections that introduce powerful, natural healing agents directly to the site of your injury. From using your own blood platelets to harnessing the potential of stem cells, these methods are designed to create an environment where your cartilage can actually regenerate. It’s a fundamental shift from simply patching up a problem to truly helping your body rebuild itself from the inside out. Let's look at some of the most effective non-surgical options available that could help you get back on your feet, pain-free.
How PRP Injections Can Help Heal Cartilage
Platelet-Rich Plasma (PRP) therapy is a straightforward and effective treatment that uses your body's own healing power. The process starts by drawing a small sample of your blood, which is then placed in a centrifuge to separate and concentrate the platelets. This platelet-rich plasma is then injected directly into your damaged knee joint. These platelets are packed with growth factors that act as signals, telling your body to start the repair process. They can help reduce inflammation, alleviate pain, and encourage new tissue growth. Since PRP uses your own blood, it's a very safe option with minimal risk of side effects.
Exploring Stem Cell and Other Cellular Therapies
Stem cell therapy is one of the most exciting areas of regenerative medicine. Stem cells are unique because they can develop into many different types of cells, including cartilage cells. When injected into a damaged knee, they have the potential to repair or replace worn-out tissue. Researchers are actively exploring how to best use stem cells to treat osteoarthritis and other joint conditions. The goal is to tap into the body's fundamental healing processes to achieve lasting relief and restore function. Our regenerative medicine services explore these cutting-edge options to help you find the right path to healing.
Understanding Different Types of Stem Cells
When we talk about stem cells, we're referring to your body's own master cells. Think of them as blank slates with the incredible ability to turn into other types of cells, like the cartilage cells your knee needs to heal. Beyond just rebuilding tissue, they also play a crucial role in calming inflammation and creating a healthier environment within the joint, which encourages natural repair. For cartilage regeneration, the most studied and utilized types are Mesenchymal Stem Cells (MSCs). These powerful cells can be sourced from different areas of your own body, including bone marrow, fat tissue, and the lining of your joints, offering a personalized approach to healing.
Using Bone Marrow Aspirate Concentrate (BMAC)
One of the most effective ways to use your body's own healing potential is with Bone Marrow Aspirate Concentrate, or BMAC. This procedure involves taking a small sample of your bone marrow, which is a rich source of Mesenchymal Stem Cells and other important healing factors. This concentrate is then precisely injected into your damaged knee. It’s a comprehensive approach because it delivers a whole team of restorative cells directly to where they're needed most. Research has shown this technique can be highly effective, with one study on athletes demonstrating that BMAC successfully repaired large cartilage injuries in a single procedure, making it a promising option for more significant damage.
Lubricating Your Joint with Hyaluronic Acid
Think of hyaluronic acid as your body's natural joint lubricant. It's a key component of the synovial fluid that cushions your joints and allows them to move smoothly. In knees affected by osteoarthritis, this fluid can thin out, leading to pain and stiffness. Hyaluronic acid injections supplement your body's natural supply, helping to restore the joint's cushioning and lubrication. This can significantly reduce pain and improve your mobility, making daily activities much more comfortable. It’s a way to give your knee the support it needs to function properly again.
Understanding the Temporary Effects
It's helpful to think of these regenerative treatments as a powerful reset for your knee, rather than a one-and-done cure. While they offer significant relief and promote your body's healing process, the results aren't always permanent. For example, PRP therapy is fantastic for reducing inflammation and encouraging new tissue growth, but its benefits typically last about six to twelve months. Similarly, hyaluronic acid injections can greatly improve joint lubrication and make movement easier, but you might need follow-up treatments every few months to sustain those effects. The goal is to give your body a major advantage in the healing process and significantly improve your quality of life. This often means creating a long-term care plan to help you maintain your progress and keep you moving comfortably for years to come.
A Personalized Approach to Cartilage Repair
At Ascend Functional Health, we see regenerative medicine as a partnership with your body. Our philosophy is built on the idea that the body has an incredible, innate ability to heal itself when given the right support. We focus on innovative techniques that enhance these natural regenerative capabilities. Instead of a one-size-fits-all solution, we create personalized protocols that address the root cause of your knee pain. By understanding your unique situation, we can use groundbreaking approaches to help you not only find relief but also achieve long-term joint health and get back to doing what you love.
Pulsed Electromagnetic Fields (PEMFs)
Pulsed Electromagnetic Field (PEMF) therapy is an innovative approach that uses targeted energy fields to support your body's healing process from the outside in. Think of it as a way to gently energize your cells, encouraging them to repair themselves more effectively. This non-invasive method has shown promising results for joint health. Research suggests that PEMF therapy can stimulate cartilage cell growth, improve the strength of existing cartilage, and help reduce painful joint swelling. It’s a gentle yet powerful tool that works at a cellular level to create a better environment for tissue regeneration, helping to protect your knee and speed up recovery without any injections or downtime.
Considering Prolotherapy
Prolotherapy is another type of injection-based treatment designed to work with your body’s natural repair system. It involves injecting a solution, typically containing a substance like dextrose, into the specific area of injury, such as the ligaments or tendons around the knee. This solution creates a mild, localized inflammation, which acts as a signal to your body, calling its healing resources to the site. The goal is to trigger the growth of new, healthy tissue and strengthen the joint. While some studies indicate that prolotherapy can be a beneficial regenerative treatment for knee issues, it's important to know that more extensive research is still needed to fully understand its effectiveness.
When is Surgery the Right Choice for Cartilage Repair?
When non-invasive treatments aren't enough to address significant cartilage damage, surgery might be the next step. While our goal at Ascend is always to support the body’s healing with the least invasive methods possible, it’s helpful to understand the surgical landscape. These procedures are designed to repair or replace damaged cartilage, aiming to restore function and reduce pain for the long term. Each technique has a different approach, from transplanting your own tissue to using lab-grown cells to encourage new growth. Let's walk through some of the most common and innovative surgical options available today.
MACI: Growing Your Own Cartilage Cells for Repair
MACI, which stands for Membrane-induced Autologous Chondrocyte Implantation, is a fascinating two-step procedure. First, a surgeon takes a small sample of your healthy cartilage cells. These cells are then sent to a lab to multiply over several weeks. In a second surgery, this new tissue is implanted back into your knee to repair the damaged area. Johns Hopkins Medicine notes that this innovative approach uses your own cartilage cells to regenerate the tissue, which can lead to better outcomes. It’s a highly personalized treatment that harnesses your body's own building blocks to heal itself from the inside out.
OATS: Relocating Healthy Cartilage to Damaged Areas
Think of the OATS procedure as a specialized type of tissue transplant. OATS stands for Osteoarticular Transfer System, and it involves moving healthy cartilage from a non-weight-bearing part of your joint to a damaged area. It’s like patching a pothole with a perfect piece of pavement from a less-traveled road. This technique is especially effective for smaller spots of cartilage damage. Because the OATS Procedure uses your own tissue, the risk of rejection is minimal. It’s a straightforward and effective way to fill in gaps in your cartilage and restore a smooth surface to the joint.
The Risk of Donor Site Morbidity
While moving healthy tissue to a damaged area sounds like a perfect fix, it's important to consider where that "patch" comes from. This brings up a key consideration called donor site morbidity, which refers to any complications that can arise at the spot where the healthy tissue was taken. Even though the cartilage is harvested from a less critical, non-weight-bearing area, you're still creating a new site of injury. This can lead to lasting pain, stiffness, or functional limitations in the donor area, which can complicate your overall recovery and rehabilitation. It’s a crucial trade-off to discuss with your specialist when evaluating if this type of surgical repair is the best path forward for your specific situation.
The RECLAIM System for Larger Cartilage Defects
One of the newer techniques in cartilage repair is the RECLAIM procedure. Developed at the Mayo Clinic, this method combines your own tissue with donor stem cells to kickstart the healing process. A surgeon takes a tiny amount of cartilage from your joint and mixes it with specialized donor stem cells. This mixture is then injected into the damaged spot to promote new growth. The new procedure called RECLAIM is a powerful example of regenerative medicine in action, blending your body's potential with the latest in stem cell science to address damage in both knee and hip joints.
Who is Eligible for RECLAIM?
The RECLAIM procedure isn't for every type of knee pain; it's a targeted solution for a specific kind of injury. The ideal candidate is typically between 18 and 55 years old, active, and dealing with a recent, painful cartilage injury from sports or physical activity. It’s important to understand that this isn't a treatment for widespread, chronic arthritis. Instead, its purpose is to repair distinct areas of damage before the joint deteriorates further. The focus is on creating a lasting repair that restores the joint's smooth surface, with the goal of keeping you moving comfortably for many years down the road.
Microfracture: Prompting Your Body's Healing Response
Microfracture surgery is a well-established technique that prompts your body to create new cartilage. During this procedure, a surgeon creates tiny holes in the bone just beneath the damaged cartilage. This controlled injury stimulates a healing response, bringing new blood and stem cells to the surface to form a new, cartilage-like tissue called fibrocartilage. While not as durable as your original cartilage, it can effectively cover the damaged bone and relieve pain. Microfracture surgery is often recommended for smaller cartilage defects and can be a great option for restoring joint function and getting you back on your feet.
The Limitations of Fibrocartilage
While microfracture is a clever way to trigger a healing response, it’s important to understand the type of tissue it creates. The new, scar-like tissue that forms is called fibrocartilage, and it’s not quite the same as the original, smooth articular cartilage that once covered your joint. Think of it as a patch rather than a perfect replacement. This fibrocartilage is less durable and not as resilient as your native tissue. While it can certainly provide a new surface to cover the exposed bone and reduce pain, its limitations mean it may not offer the same long-term performance, which is a key consideration when weighing your options.
Minced Cartilage Techniques
Another approach gaining traction involves using tiny, minced pieces of cartilage to fill in defects. These methods often use the small cartilage fragments to create a paste or place them on a scaffold to encourage new growth directly in the damaged area. Some techniques use the patient's own cartilage, while others, like DeNovo NT, use minced cartilage from young human donors mixed with a special biological glue. The goal is to repair the damage in a single surgery, and while many of these techniques are still evolving, early human studies look promising for this innovative strategy.
Allograft Cartilage Implantation
Allograft cartilage implantation is a procedure that uses tissue from a donor to repair a damaged knee joint. The primary advantage of this method is that it doesn't require a second surgical site on your body to harvest your own cartilage, which can simplify the procedure and recovery. However, this approach comes with its own set of considerations. There is a small risk that your body could reject the donor tissue or that an infection could develop. The long-term durability of the transplanted tissue can also be a concern, making it crucial to discuss the pros and cons with a specialist to determine if it's the right fit for your specific situation.
The Evolution of Cartilage Repair: New vs. Traditional Methods
When you’re dealing with knee pain, you want a solution that lasts. Traditional treatments often focus on managing symptoms, but the field of regenerative medicine is changing the game by focusing on healing the source of the problem. These newer approaches are designed to work with your body’s natural healing abilities, offering more personalized and potentially longer-lasting results than older methods. Let's look at how these innovative treatments stack up.
What's New in Cartilage Regeneration Medicine?
Scientists are constantly discovering more about how our bodies work, leading to exciting new possibilities for cartilage repair. For example, researchers at Stanford Medicine found that by blocking a specific protein, they could encourage joint cartilage to regrow in mice. This kind of discovery opens the door for treatments that could one day help the body rebuild its own cartilage, offering a way to truly repair damage rather than just patching it up. It’s a significant shift from simply managing pain to actively promoting healing from within.
Targeting Aging with Gerozyme Inhibitors
One of the most exciting frontiers in cartilage repair involves looking at the aging process itself. Stanford Medicine scientists have identified a protein that increases as we age and can prevent tissues from functioning properly. By blocking this protein, they found a way to regrow joint cartilage in mice. This research suggests that future treatments could target the underlying mechanisms of aging to help the body rebuild its own cartilage. It’s a groundbreaking concept that moves beyond managing symptoms and toward actively promoting healing from within by addressing one of the root causes of tissue breakdown.
Experimental Drug Therapies
Alongside cellular treatments, researchers are also exploring how certain medications might support cartilage regeneration. While still in the early stages, some studies suggest that specific drugs could play a role in the healing process. For example, medications like teriparatide are being investigated for their potential to help repair cartilage. This area of research is part of a wider effort to find pharmacological interventions that can create a better environment for tissue repair, offering another potential tool in the toolkit for joint health.
Advanced Cellular and Genetic Therapies
We’ve already touched on stem cells, but the research in this area continues to advance rapidly. Stem cells are remarkable because they can develop into many different types of cells, including the chondrocytes that make up cartilage. When introduced to a damaged knee, they hold the potential to replace worn-out tissue and restore function. Scientists are actively studying how to optimize these therapies to treat joint conditions, aiming to harness the body’s most fundamental healing processes for lasting relief and improved mobility.
The Role of Exosomes in Healing
Another cutting-edge area of study involves exosomes. Think of exosomes as tiny messengers released by your cells, carrying important instructions and materials from one cell to another. In the context of joint health, these messengers are incredibly powerful. They can help repair damaged cartilage, encourage the growth of stem cells, and reduce inflammation. Because they play such a key role in cellular communication, exosomes are a promising avenue for enhancing the body’s natural healing response and creating the ideal conditions for tissue regeneration.
The Importance of Continued Research
While all of these advancements are incredibly promising, it's important to remember that many are still in the research phase. A lot of these new treatments lack long-term studies to fully confirm their effectiveness and safety. One of the biggest challenges, especially for cell-based therapies, is making sure the new cells survive and integrate properly into the existing tissue. This highlights the need for continued, careful research to refine these techniques and bring safe, effective, and lasting solutions to those dealing with cartilage damage.
Building New Cartilage with Tissue Engineering
Another exciting area is tissue engineering, which uses your body's own cells to create new tissue. Procedures like the RECLAIM technique are at the forefront of this approach. This method involves taking a small sample of your own healthy cartilage and using it with donor stem cells to repair damaged areas in the knee. Think of it as a highly personalized patch for your joint. This is a world away from traditional methods that might use synthetic materials. It’s all about creating a living, functional repair that integrates seamlessly with your body.
The Future of 3D Bioprinting
Looking even further ahead, 3D bioprinting is poised to take tissue engineering to a whole new level. Imagine a technology that can print a new piece of cartilage that is a perfect, custom fit for your knee. That’s the promise of 3D bioprinting. This process uses a specialized “bio-ink” made of living cells—often stem cells—to construct new cartilage, layer by layer. The goal is to create a living implant that not only matches the exact shape of the damaged area but also mimics the complex structure of natural tissue. This could lead to breakthroughs in how we approach cartilage regeneration, allowing for the development of living tissues that can integrate seamlessly with the body. While still in advanced stages of research, this technology represents the ultimate in personalized joint repair.
Which Treatments Have the Best Long-Term Outcomes?
So, do these new treatments actually work better? The evidence is very promising. The RECLAIM procedure, for instance, has shown that new cartilage can fill in damaged spots within a year, and the joint could stay healthy for 13 to 20 years. This offers a much more durable solution than many older treatments. Plus, advanced options like OATS and MACI are becoming more accessible as insurance companies are beginning to provide coverage. This growing acceptance makes cartilage regeneration a more realistic option for more people seeking long-term relief from knee pain.
Simple Lifestyle Habits for Healthier Knees
Regenerative medicine offers incredible tools for healing, but the journey doesn't end with a procedure. The daily choices you make play a huge role in supporting your body's ability to repair itself and maintain long-term joint health. Think of it as creating the best possible environment for healing to happen. By focusing on movement, nutrition, and other key lifestyle factors, you can protect your investment in your health, reduce inflammation, and keep your knees feeling their best for years to come. At Ascend Functional Health, our approach combines advanced treatments with personalized lifestyle guidance because we know that true, lasting wellness comes from addressing the whole picture. These changes aren't about restriction; they're about empowering you to take an active role in your own healing.
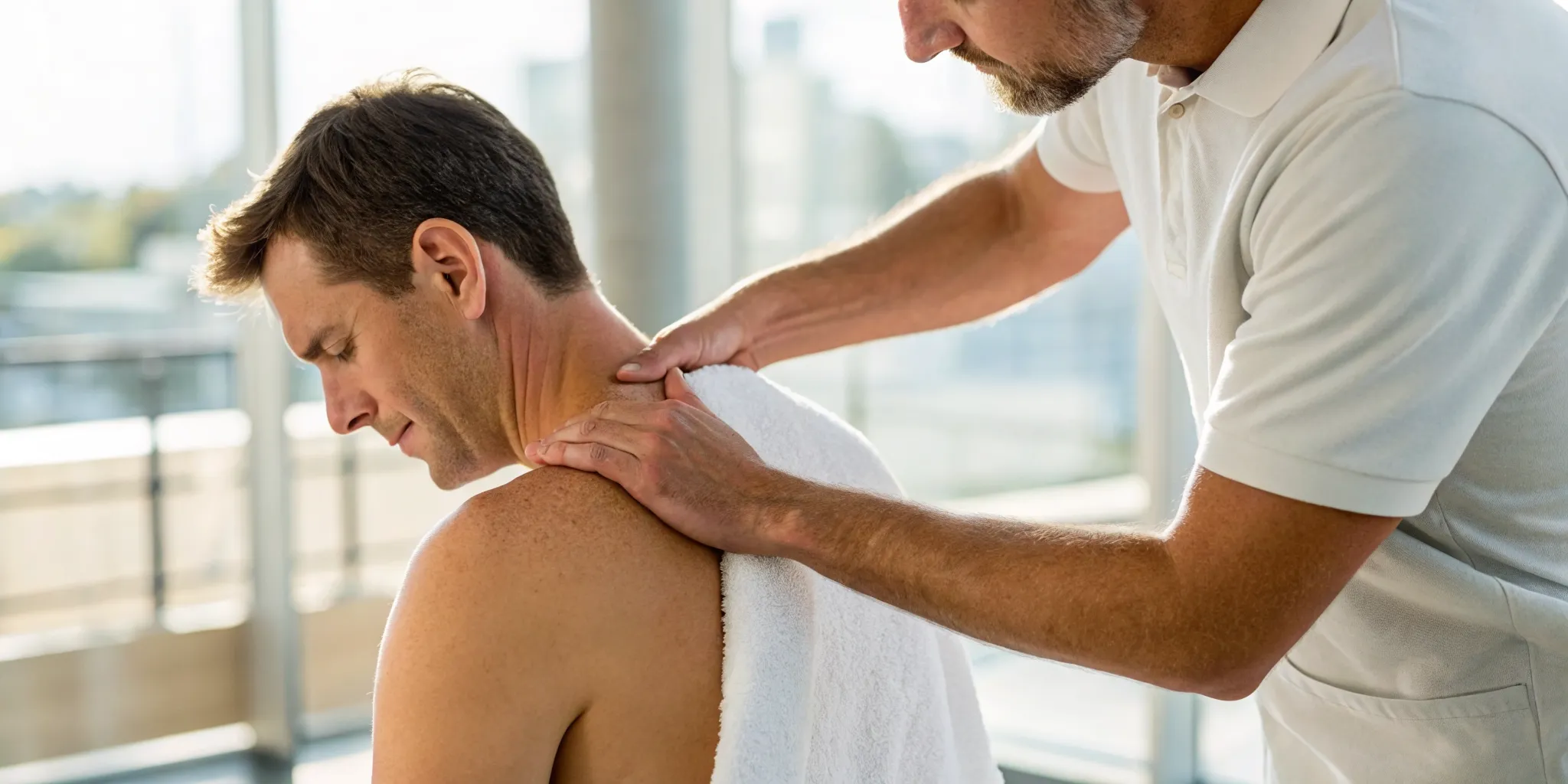
Why Movement is Medicine for Your Knees
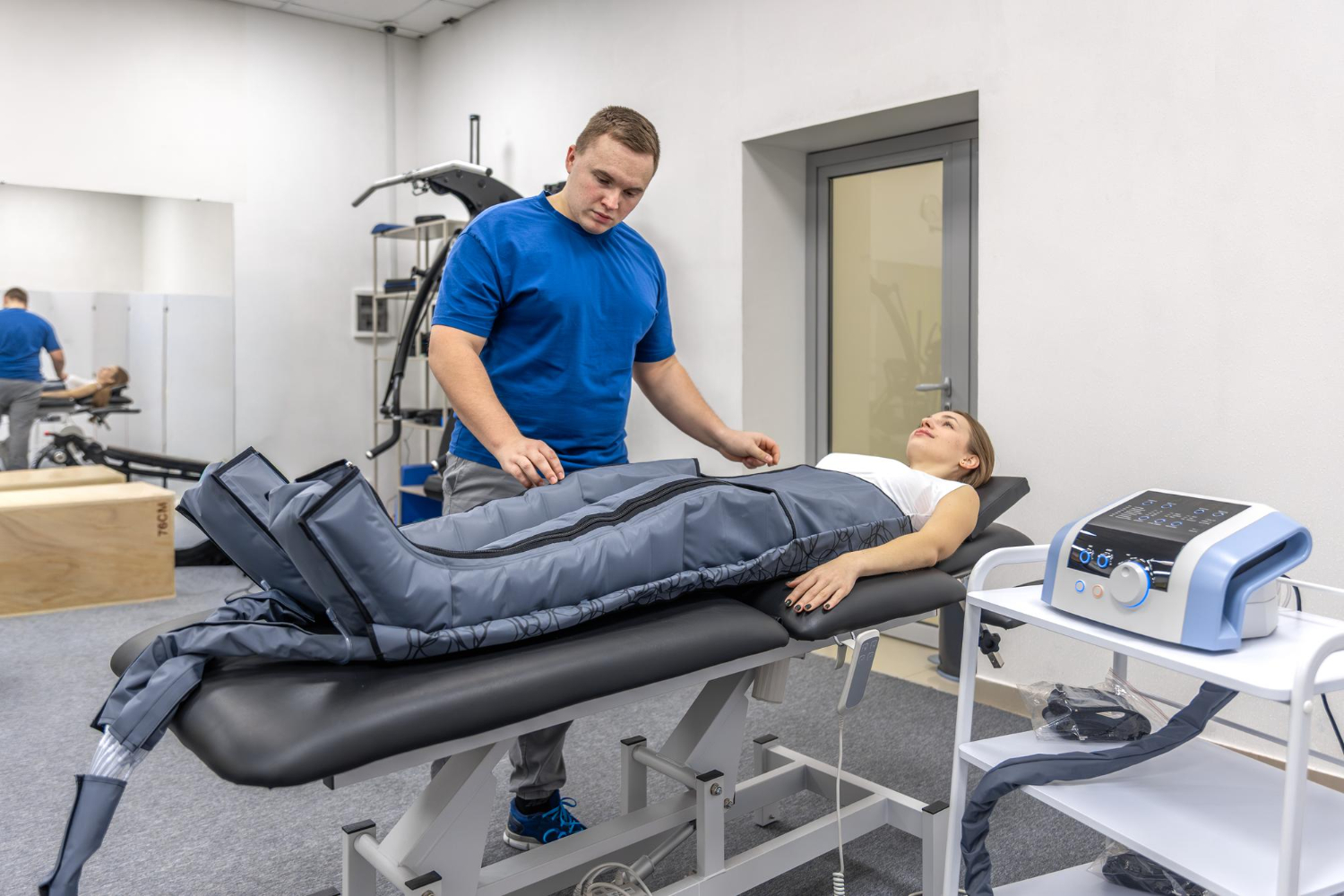
After any knee treatment, movement is medicine. It might seem counterintuitive to move a joint that’s been causing you pain, but guided physical therapy is essential for recovery. A skilled therapist can design a program to help you regain strength, flexibility, and function without putting undue stress on the healing cartilage. The goal is to strengthen the muscles that support your knee joint, which acts as a natural brace, absorbing shock and improving stability. Our Physical Medicine programs are tailored to do just that, helping restore function and improve your mobility safely and effectively.
The Best Foods for Joint Health
What you eat can either fuel inflammation or fight it. Making positive changes to your diet sends a powerful signal to your body to reduce inflammation and build stronger tissues. Focus on incorporating whole, anti-inflammatory foods into your meals. Think colorful fruits and vegetables, fatty fish rich in omega-3s (like salmon), nuts, seeds, and olive oil. At the same time, try to limit processed foods, sugary drinks, and refined carbohydrates, which can contribute to systemic inflammation and hinder your body's healing process. A functional medicine approach can help identify the right nutritional strategy for your specific needs.
Helpful Dietary Supplements
While a nutrient-rich diet is your foundation, certain supplements can provide more targeted support for cartilage health. Glucosamine and chondroitin sulfate, for example, are natural components of cartilage and may help slow down its breakdown while reducing swelling. Another plant-based extract, Avocado-Soy Unsaponifiables (ASU), has shown promise in improving joint function for those with osteoarthritis. And of course, omega-3 fatty acids are powerful anti-inflammatories that support overall joint integrity. It's important to remember that supplements aren't a one-size-fits-all solution. Building a personalized plan with a professional ensures you’re giving your body the right support for healing, which is a key part of our functional medicine approach.
Lighten the Load: The Role of Weight and Exercise
Your body weight has a direct impact on your knee joints. For every extra pound you carry, your knees feel about four extra pounds of pressure with every step. Managing your weight is one of the most effective things you can do to reduce stress on your cartilage and prevent further wear and tear. Pairing weight management with low-impact exercise is a winning combination. Activities like swimming, cycling, and walking strengthen the muscles around the knee without the jarring impact of running or jumping. This improves joint mobility and supports overall joint health for the long haul.
Simple Ways to Reduce Inflammation
Chronic inflammation is a key driver of joint pain and cartilage breakdown. Fortunately, simple daily habits can make a big difference. Beyond choosing anti-inflammatory foods and low-impact exercises, focus on getting quality sleep, managing stress, and staying hydrated. Sleep is when your body does most of its repair work, while chronic stress can keep your body in a pro-inflammatory state. By taking these small, consistent steps, you create an internal environment that calms inflammation and supports the regenerative treatments you’re receiving, helping you get back to the activities you love with less pain.
How to Choose the Right Treatment for You
Deciding on a path forward for your knee pain is a big step, and it’s one you don’t have to take alone. The best treatment is one that aligns with your specific injury, lifestyle, and long-term health goals. It’s about finding a solution that doesn’t just mask the pain but addresses the underlying cause to help you get back to living your life fully. This process starts with understanding your options, knowing what makes someone a good candidate for certain therapies, and partnering with a specialist who can guide you.
Key Questions to Ask Before Choosing a Treatment
Before you choose a treatment, it’s helpful to understand its primary goal. Many conventional approaches focus on pain relief or symptom management, which can be incredibly helpful, but they don’t always slow or reverse the underlying cartilage damage. Think about what you truly want to achieve. Are you looking for immediate relief to get through your day, or are you seeking a long-term solution that restores function and helps you avoid more invasive procedures down the road? Your age, activity level, and the extent of the cartilage wear will all influence which health solutions are most appropriate for you.
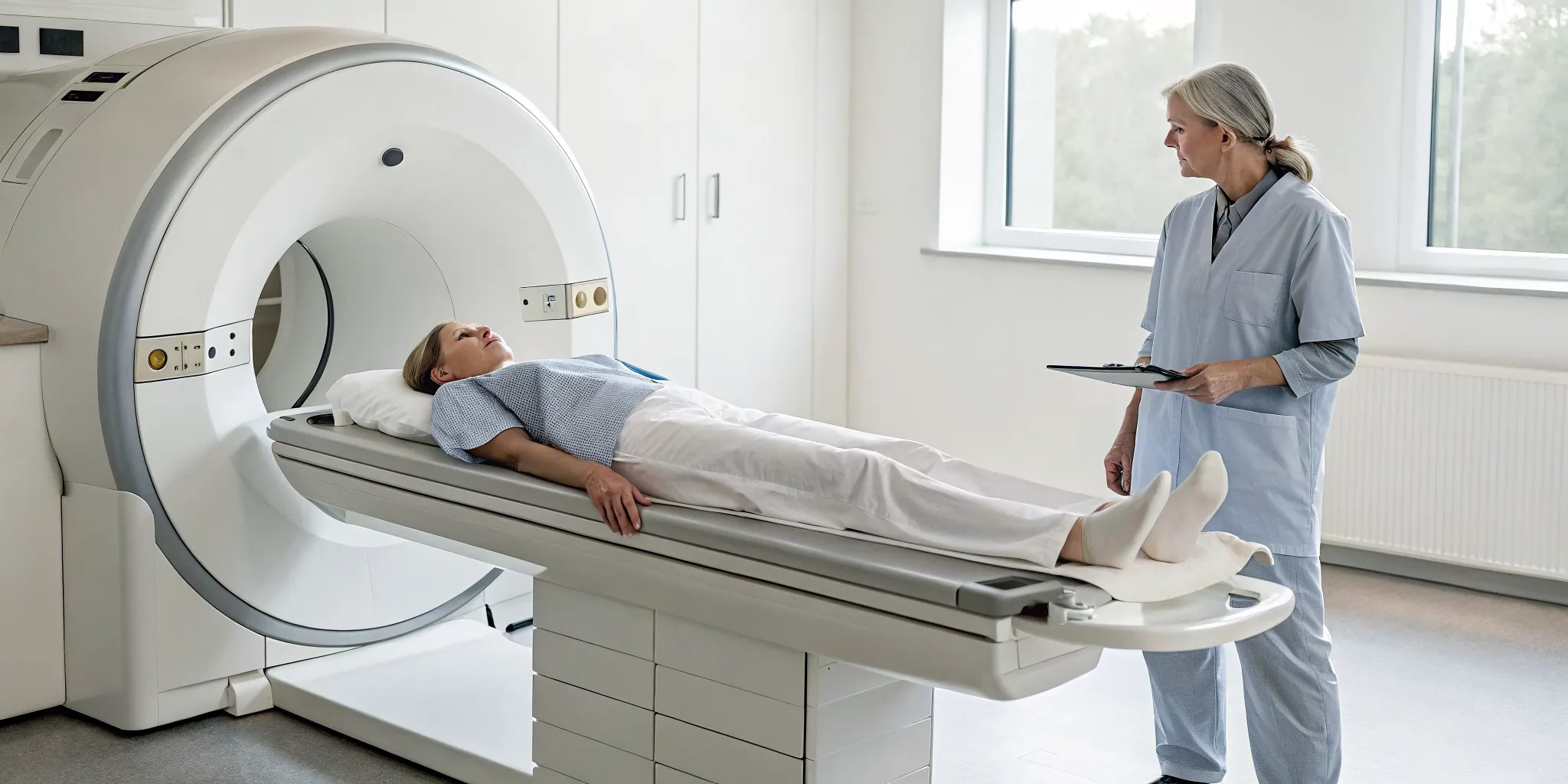
Are You a Good Candidate?
Every knee is different, which means not every treatment is a universal fit. Candidacy for regenerative procedures can be quite specific. For example, some advanced therapies are most effective for younger individuals with recent injuries and minimal arthritis. A thorough evaluation is the only way to know for sure what will work for you. This typically involves a detailed health history, a physical exam, and often imaging like an MRI to get a clear picture of your joint health. This diagnostic step is critical for creating a targeted and effective treatment plan that gives you the best possible chance at a successful outcome.
Why a Specialist is Key to Your Success
Partnering with a specialist is about more than just receiving a treatment; it’s about creating a comprehensive, personalized recovery plan. The main goal is to ease your chronic pain, help you return to the activities you love, and potentially delay or prevent the need for a full joint replacement. A specialist in regenerative medicine will explore innovative approaches that are tailored to your body’s unique needs. They will discuss all your options, set realistic expectations, and build a strategy that supports your body’s natural healing ability from every angle.
Your Cartilage Repair Journey: What to Expect
Deciding on a treatment plan is a huge step, and it’s natural to wonder what comes next. While every person’s journey is unique, the goal is always the same: to help your body heal, restore function, and get you back to living with less pain. Our approach to regenerative medicine is a partnership. We’ll guide you through each phase, from the procedure itself to the crucial recovery period that follows, ensuring you have the support you need to achieve the best possible results.
What Does Recovery Look Like?
Your recovery isn't just about resting; it's an active process. After any knee cartilage procedure, physical therapy plays a vital role in supporting healing and restoring function. A structured rehabilitation program is essential for rebuilding strength, improving mobility, and ensuring your knee joint heals correctly. Think of it as the framework that helps your body make the most of the treatment. Our physical medicine team will design a personalized plan with specific exercises and techniques to alleviate pain and get you moving safely and confidently. Your timeline will depend on your specific treatment and how your body responds, but consistent, guided movement is a non-negotiable part of a successful recovery.
What Results Can You Realistically Expect?
Healing takes time, and it’s important to set realistic expectations for your recovery. Regenerative treatments work by stimulating your body's natural repair mechanisms, which is a gradual process. You can support this process by making positive lifestyle changes. Every step you take, from engaging in low-impact aerobic exercise to daily stretching, sends a signal to your body to reduce inflammation and build stronger muscles around the joint. Our team will work with you to set achievable short-term and long-term goals, helping you celebrate small victories along the way as you work toward lasting relief and improved joint function.
Are There Any Downsides to Consider?
Before any procedure, it’s crucial to understand the full picture, including potential risks. Damage to knee cartilage can cause persistent pain, swelling, and a locking or catching sensation that limits your daily life. While regenerative treatments are designed to be minimally invasive, our team will walk you through any potential side effects or outcomes. We believe in complete transparency, ensuring you feel fully informed and comfortable with your chosen treatment plan. The goal is to address the root cause of your symptoms and significantly improve your quality of life, and that starts with an open, honest conversation.
A Warning About Common Pain Relievers
When your knee hurts, it’s natural to reach for a common pain reliever for quick relief. While these can temporarily ease discomfort, it’s important to understand their long-term effects. Research shows that some of the most common solutions can actually interfere with your body's healing process. For example, while non-steroidal anti-inflammatory drugs (NSAIDs) like ibuprofen can reduce swelling, studies suggest that extended use may actually harm cartilage repair. Similarly, steroid injections are effective at calming inflammation, but they can also damage cartilage cells and prevent healing over time. This is why our approach focuses on addressing the root cause of your symptoms rather than just masking them, creating a path toward genuine, lasting joint health.
How to Protect Your Knees for the Long Haul
Your treatment is the catalyst for healing, but long-term success depends on how you care for your knees moving forward. Simple, consistent habits can make a world of difference. Managing your weight reduces the daily stress on your knee joints, while modifying certain high-impact activities can prevent future damage. Regular physical activity is also key, as it improves balance and strengthens the muscles that support your knees, decreasing your risk of falls and injuries. These practical lifestyle changes are powerful tools for protecting your investment in your health and keeping your joints strong for years to come.
Frequently Asked Questions
My knee clicks and aches sometimes. Does this automatically mean my cartilage is damaged? Not necessarily, but you should definitely pay attention to those signals. While clicking, popping, and aching are common signs of cartilage wear, they can also be caused by other issues. The most important step is to get a proper diagnosis to understand exactly what's happening inside your joint. Ignoring these symptoms could lead to more significant problems, so it's always best to have it checked out by a professional who can identify the root cause.
What's the real difference between regenerative treatments like PRP and surgical options? Think of it as two different philosophies for repair. Regenerative medicine works from the inside out by using your body's own powerful healing agents to reduce inflammation and encourage new tissue growth. It’s a minimally invasive approach focused on creating the right environment for your body to heal itself. Surgery is more of a structural fix, where a surgeon physically repairs, replaces, or reconstructs the damaged area. The right choice depends entirely on the extent of your injury, your activity level, and your long-term goals.
Can my cartilage actually grow back, or are these treatments just for pain relief? This is the most exciting aspect of regenerative medicine. The primary goal is to go far beyond simple pain management. Treatments like PRP and stem cell therapy are specifically designed to stimulate your body's natural repair mechanisms. This process can help your body generate new, healthy tissue in the damaged area. It’s a gradual process, but the aim is true, lasting restoration of the joint, not just a temporary fix.
How long does it take to see results from a non-surgical treatment like PRP? Because these treatments work with your body's natural healing timeline, results don't happen overnight. It's a different experience than getting a quick-fix injection. Most people begin to feel a gradual reduction in pain and an improvement in function within a few weeks of the procedure. The most significant results often appear over the next several months as your body continues to repair and strengthen the tissue.
If I get treatment, can I go back to my old activities, like running? Helping you return to the activities you love is our ultimate goal. For many people, this is entirely possible. Your recovery will focus on a smart, gradual return to your favorite sports or exercises. We'll work with you to create a plan that strengthens the muscles supporting your knee and may suggest some modifications to your form or routine. This approach helps protect the joint from future injury so you can stay active for the long haul.