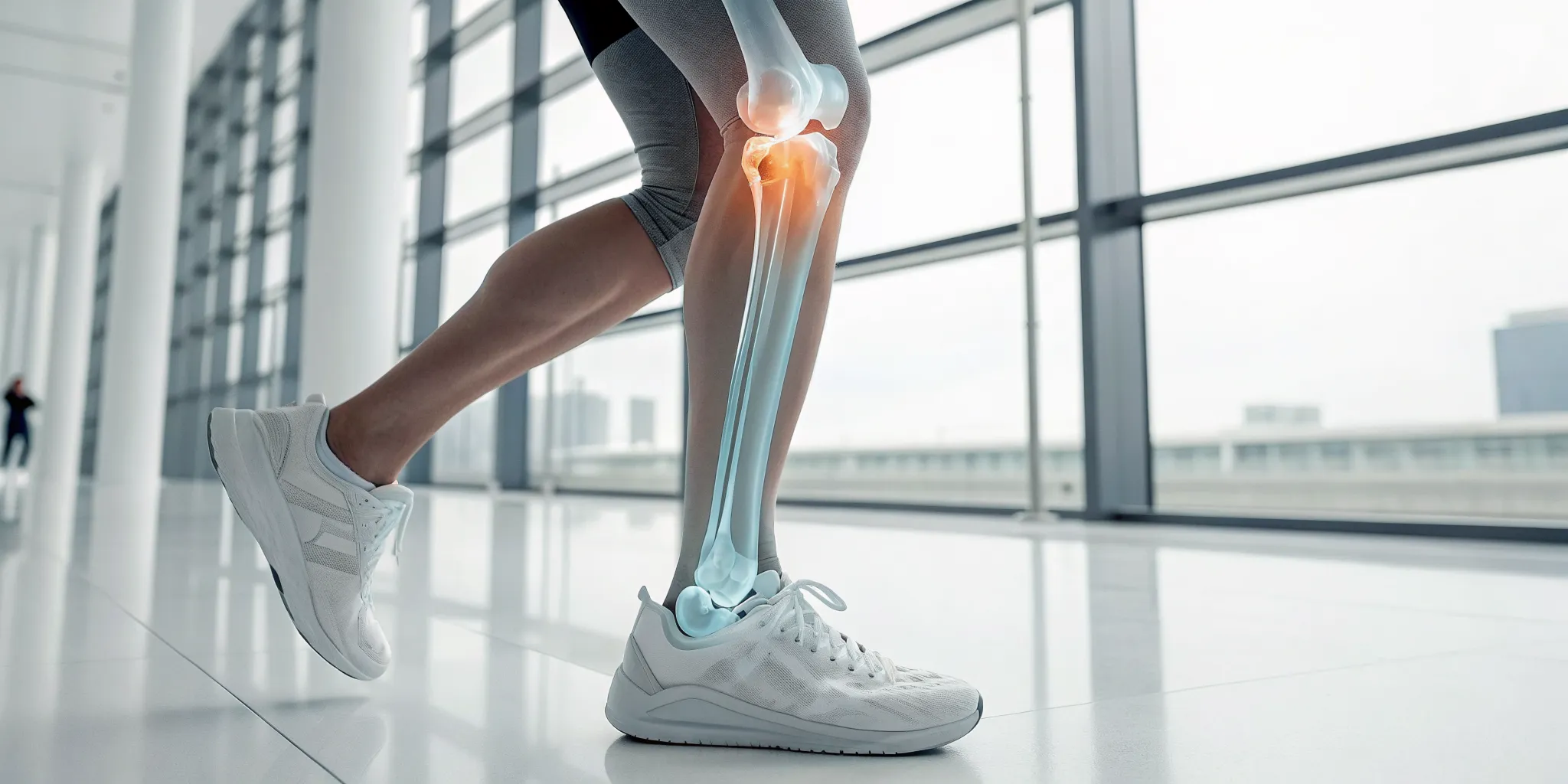
That ache in your back is rarely just about your back. It’s often a signal that your whole system is out of balance. A bulging disc might be the immediate source of pain, but factors like chronic inflammation, poor posture, and even high stress can be major contributors. A truly effective solution looks at the whole picture. Instead of just chasing symptoms, a holistic approach creates an internal environment where your body can heal itself. By integrating a targeted bulging disc therapy treatment with supportive strategies like an anti-inflammatory diet and stress management, you can address the problem from all angles. This guide shows you how to build that comprehensive plan for lasting relief.
Key Takeaways
- Prioritize Non-Surgical Solutions First: Surgery is rarely the initial answer for a bulging disc. A personalized plan combining physical therapy, chiropractic care, and other conservative treatments is highly effective for reducing pain and addressing the underlying issue without invasive procedures.
- Embrace Strategic Movement Over Bed Rest: While rest seems logical, gentle and targeted activity is crucial for healing. Guided exercises strengthen the core muscles that support your spine, improve blood flow, and help prevent future pain, making it a more effective path to recovery than staying inactive.
- Make Your Daily Habits Work for You: Your recovery isn't limited to appointments; it happens every day. Small changes like improving your posture at work, maintaining a healthy weight, and choosing anti-inflammatory foods create a supportive environment for your body to heal and build long-term spinal resilience.
What Is a Bulging Disc?
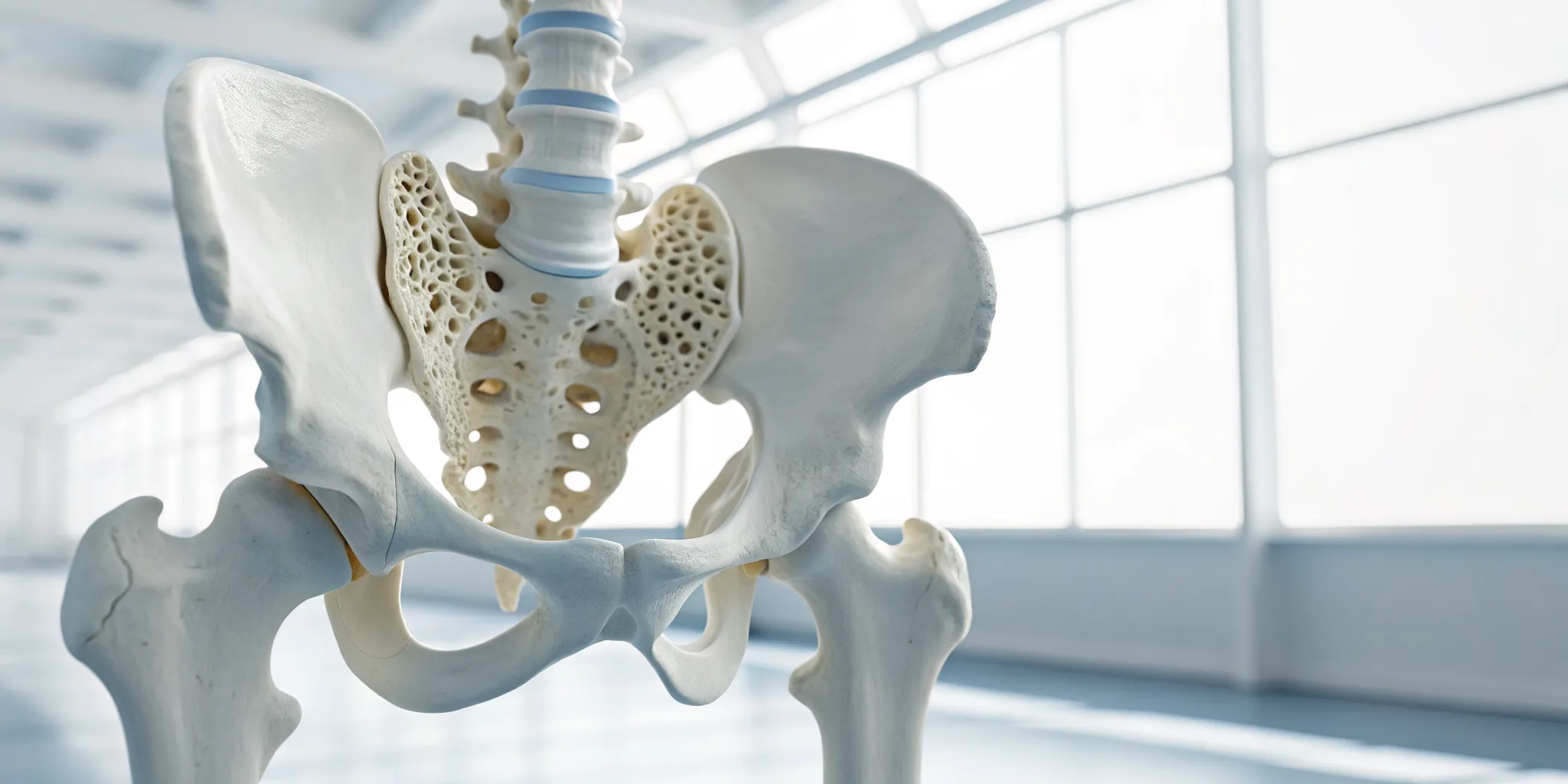
Think of your spine as a stack of bones (vertebrae) with soft, cushiony discs in between. These discs act as shock absorbers, allowing you to bend and move without your bones grinding together. Each disc has a tough outer layer and a soft, gel-like center. A bulging disc happens when one of these cushions gets compressed and bulges outward, moving out of its normal space between the vertebrae.
The good news is that the disc itself remains intact. Unlike a more severe injury, the tough outer wall doesn't tear or rupture. Many people have bulging discs without even knowing it. However, if the bulge presses on a nearby nerve, it can cause significant pain, numbness, or weakness. Understanding the root cause of this pressure is the first step toward finding relief. At Ascend Functional Health, we focus on identifying what’s causing your discomfort so we can create a personalized plan to help your body heal. Our approach to physical medicine is designed to address these kinds of structural issues without invasive procedures, focusing instead on restoring your body's natural function and strength.
Defining the Condition: Slipped, Ruptured, or Bulging?
You’ve probably heard the terms "slipped disc," "ruptured disc," and "bulging disc" used interchangeably, but they describe different things. A bulging disc is the least severe of the three. Think of it like a tire with a weak spot that bulges out but doesn't pop. The disc’s tough outer wall is stretched and pushed outward, but it remains intact. In contrast, a herniated disc, also called a slipped or ruptured disc, occurs when that outer wall actually tears, allowing the soft, gel-like center to leak out. While a herniated disc often sounds more alarming, both conditions can cause pain if they press on spinal nerves. The key is to get an accurate diagnosis to determine the right course of action.
Common Locations for Disc Issues
Bulging discs don't happen just anywhere along the spine; they have favorite spots. Most often, they occur in the lower back (the lumbar spine) or the neck (the cervical spine). This makes sense when you think about it—these are the areas of your spine that handle the most movement and stress, from lifting heavy objects to sitting at a desk all day. It’s much less common for a disc issue to develop in the mid-back (thoracic spine). If you're dealing with persistent lower back pain or a stiff, aching neck that just won't quit, a bulging disc could be the culprit. Understanding the specific conditions we treat can help you connect your symptoms to their underlying cause.
How Common Are Bulging Discs?
If you’ve been diagnosed with a bulging or herniated disc, you are far from alone. More than three million people in the U.S. face this issue every year. The most important thing to know is that this diagnosis is not a life sentence of pain or a one-way ticket to the operating room. In fact, research shows that nine out of ten people with a herniated disc get better without surgery. This highlights the power of conservative, non-invasive treatments like chiropractic care and targeted physical therapy. With the right strategy, your body has an incredible capacity to heal. We see stories of recovery all the time from people who committed to a plan and avoided surgery altogether.
Why Do Discs Bulge?
So, what causes a disc to bulge in the first place? It’s rarely just one thing. Often, it’s a combination of factors that build up over time. The natural aging process is a major contributor; as we get older, our spinal discs tend to dry out and become less flexible, making them more prone to bulging. A sudden injury from a fall or accident can also force a disc out of place.
Beyond that, your daily habits play a big role. Repetitive movements, especially those involving lifting or twisting, can put consistent strain on your spine. Even something as simple as poor posture while sitting at a desk all day can contribute. Other factors include carrying excess weight, which adds pressure to your spine, and sometimes, it just comes down to genetics.
Bulging vs. Herniated Discs: What's the Difference?
You’ve probably heard the terms "bulging disc" and "herniated disc" used interchangeably, but they describe two different conditions. A bulging disc is when the disc pushes outward but the tough outer layer remains intact. Imagine squishing a jelly donut without breaking it—the sides bulge out, but the jelly stays inside. This is a more common and generally less severe condition.
A herniated disc, on the other hand, is when a tear or crack forms in that tough outer layer, allowing the soft, gel-like center to leak out. This leaked material can directly press on and irritate spinal nerves, often causing more intense and acute symptoms. While both conditions can cause pain, understanding the difference helps your healthcare provider determine the most effective treatment plan for you.
What Does a Bulging Disc Feel Like?
A bulging disc can be sneaky. Sometimes it causes no symptoms at all, but when it presses on a nearby nerve, the discomfort can be hard to ignore. The first step toward feeling better is learning to recognize what your body is telling you. Understanding these signs helps you know when it's time to seek professional care and get on the right path to healing.
Physical Symptoms to Watch For
A bulging disc happens when one of the soft, cushion-like discs between your vertebrae pushes out of its normal space. This can happen in your neck or your lower back, and the symptoms often depend on the location. If the disc is in your neck, you might feel neck pain and stiffness, or pain that travels down your arms and into your fingers. For a bulging disc in the lower back, you might experience low back pain, sciatica (a sharp pain that runs down your leg), or discomfort in your legs and feet. These symptoms are often addressed through physical medicine to restore function and reduce pain.
Symptoms of a Bulging Disc in the Neck
When a disc bulges in your neck, the symptoms can be quite distinct. You'll likely feel localized pain and stiffness right in your neck, which can make turning your head uncomfortable. But the discomfort often doesn't stop there. Because the bulging disc can press on nerves that travel out from your spinal cord, you might experience pain that radiates from your neck, through your shoulder, and down your arm. This can feel like a sharp, shooting pain, or sometimes a dull ache. It's also common to have numbness, tingling, or even weakness in your arm or hand, which can affect your grip strength. Some people even experience frequent headaches that originate from the neck tension. These are all signals that a nerve is being irritated, and it's your body's way of telling you that something needs attention.
Red Flags: When to See a Doctor Right Away
It’s always a good idea to talk to a healthcare provider if you’re concerned about new or persistent back pain. While some discomfort might resolve on its own, certain symptoms are red flags that shouldn't be ignored. You should seek medical attention if the pain is severe enough to interfere with your daily activities or if your symptoms don't improve after four to six weeks. It's especially important to get help if your symptoms are getting worse. Pay close attention to any tingling, numbness, or weakness in your arms, hands, legs, or feet. If you ever experience a loss of bladder or bowel control, treat it as a medical emergency and seek help right away. These are all conditions we treat with personalized care plans.
Difficulty Standing or Walking
When a bulging disc in your lower back presses on the nerves that travel down to your legs, even simple movements can become difficult. You might find that standing for more than a few minutes causes intense pain, or that walking feels unsteady. This isn't just about discomfort; nerve compression can lead to weakness, numbness, or a tingling sensation in your legs and feet, making you feel like your leg could give out. This kind of symptom is a clear signal that the issue is significantly interfering with your body's function and impacting your daily life. It’s a major red flag that tells you it's time to get a professional evaluation to understand the root cause and find a path back to moving with confidence.
What Causes a Bulging Disc?
A bulging disc rarely appears out of nowhere. It’s usually the result of gradual wear and tear or a combination of factors that place stress on your spine over time. Understanding these underlying causes is key to not only finding relief but also preventing future issues. Instead of just treating the pain, we focus on identifying the root cause of your discomfort. By looking at the whole picture—from your daily habits to your body's mechanics—we can build a plan that addresses the source of the problem for more sustainable healing.
Common Risk Factors
Several factors can increase your likelihood of developing a bulging disc. Some are within your control, while others are not. Recognizing these risk factors can help you make informed decisions about your lifestyle and be more proactive about your spinal health. It’s about understanding how different aspects of your life contribute to the overall condition of your spine and what you can do to support it better.
Age and Gender
The natural aging process is a major contributor to disc issues. As we get older, our spinal discs tend to dry out, lose their elasticity, and become less flexible, making them more prone to bulging. Think of them like car tires that wear down over time. While this is a normal part of aging that can affect anyone, men are more likely to experience disc problems than women. This doesn't mean it's inevitable, but it does highlight the importance of maintaining spinal health as the years go by.
Lifestyle and Occupational Hazards
Your daily activities have a significant impact on your spine. Repetitive movements, especially those involving lifting or twisting, can put consistent strain on your back. This is common in physically demanding jobs but can also affect athletes or anyone with a very active lifestyle. On the other end of the spectrum, a sedentary life isn't much better. Even something as simple as poor posture while sitting at a desk all day can contribute to disc compression. At Ascend Functional Health, our physical medicine services focus on correcting these imbalances through targeted care.
Genetic Factors
Sometimes, it just comes down to genetics. You might inherit a predisposition to weaker cartilage in your spinal discs, making you more susceptible to bulging discs than someone else, even with similar lifestyles. While you can't change your genes, knowing that you might be at a higher risk can empower you to be extra diligent about other factors you can control, like maintaining a healthy weight, practicing good posture, and strengthening your core muscles to provide your spine with better support.
Diagnosing a Bulging Disc
If you suspect you have a bulging disc, getting an accurate diagnosis is the first and most important step. Self-diagnosing can lead to improper care and may worsen the problem. A thorough evaluation by a healthcare professional will help pinpoint the exact cause of your pain and rule out other potential issues. This process allows us to create a personalized treatment plan tailored to your specific needs, ensuring you get the most effective care possible. At Ascend, we start by listening to your story to understand the full context of your symptoms before moving on to a physical assessment.
The Initial Examination
Your first appointment will likely begin with a detailed conversation about your symptoms, medical history, and daily activities. From there, a physical exam helps identify the source of the pain. According to the Mayo Clinic, doctors check your back for tenderness and may ask you to move in certain ways to see what motions trigger your discomfort. This hands-on approach provides valuable clues about which disc might be affected and whether any nerves are involved, guiding the next steps in the diagnostic process.
Physical and Neurological Tests
To get a clearer picture of how the bulging disc is affecting your body, your doctor will perform a few simple tests. A neurological exam is standard procedure and involves checking your reflexes, muscle strength, and walking ability. Your provider will also test your ability to feel light touches or pinpricks in different areas. These tests are designed to assess whether the bulging disc is pressing on a nerve and interfering with the signals being sent between your brain and other parts of your body.
The Straight Leg Raise Test
One of the most common tests for a bulging or herniated disc in the lower back is the straight leg raise test. As noted by the Cleveland Clinic, this simple maneuver involves you lying on your back while your doctor gently lifts your affected leg. If this movement causes pain to shoot down your leg, it’s a strong indicator that a disc is irritating your sciatic nerve. It’s a quick, non-invasive way to confirm nerve root compression and is often one of the first physical tests performed.
Advanced Diagnostic Imaging
While a physical exam provides a lot of information, sometimes your doctor needs to see exactly what’s happening inside your spine. Advanced imaging tests can confirm the location and severity of a bulging disc and rule out other conditions that might be causing your symptoms. These tests create detailed pictures of your bones, discs, and nerves, offering a clear roadmap for your treatment plan and ensuring your care is as precise as possible.
MRI and CT Scans
An MRI (Magnetic Resonance Imaging) scan is often the gold standard for diagnosing disc issues. It uses radio waves and a strong magnet to create detailed images of your soft tissues, including your spinal discs and nerves. This allows your doctor to see the exact location of the bulge and determine if it's affecting any nearby nerves. A CT (Computed Tomography) scan may also be used, which takes a series of X-rays from different angles to create cross-sectional images of your spine, providing a clear view of your vertebrae.
Myelograms and X-Rays
Although X-rays don't show soft tissues like discs, they are still very useful. An X-ray can help rule out other potential causes of your back pain, such as a fracture, infection, or tumor. A myelogram is a more specialized test where a special dye is injected into the spinal fluid before a CT scan. This dye makes your spinal cord and nerves show up more clearly on the scan, highlighting any areas where a bulging disc might be causing compression.
Assessing Nerve Damage
If your doctor suspects that a bulging disc has caused nerve damage, they may recommend tests to measure how well your nerves are functioning. These tests can feel a bit intimidating, but they provide crucial information about the health of your nervous system. They help determine the extent of any nerve compression and can guide decisions about the best course of treatment. The goal is to understand if the electrical signals from your brain are reaching your muscles correctly.
Tests like nerve conduction studies and electromyography (EMG) measure how well electrical signals travel along your nerve pathways. An EMG assesses the health of your muscles and the nerve cells that control them. Together, these tests can pinpoint the exact location of nerve damage and determine its severity. This information is vital for creating a targeted and effective recovery plan that addresses the full scope of your condition.
Non-Surgical Treatments for a Bulging Disc
If you’ve been diagnosed with a bulging disc, your first thought might be about surgery. But the good news is that most people find significant relief through non-surgical treatments. The goal is to reduce pain and inflammation, take pressure off the affected nerve, and strengthen your body to prevent future issues. This approach focuses on helping your body heal itself with targeted support.
At Ascend Functional Health, we prioritize conservative, effective strategies to get you back to feeling your best. Our holistic health solutions are designed to address the root cause of your pain, not just mask the symptoms. Let’s walk through some of the most common and effective non-surgical options available.
How Physical Therapy and Exercise Can Help
Physical therapy is a cornerstone of bulging disc treatment for a reason—it works. A skilled therapist will guide you through specific exercises designed to strengthen the muscles that support your spine, improve your flexibility, and correct your posture. This isn't about just any workout; it's a personalized plan to stabilize your core and reduce pressure on your spinal discs. Most people start to feel a noticeable difference within four to six weeks of consistent sessions. Our Physical Medicine programs focus on restoring movement and function to help you heal effectively.
Managing Pain with Medication
When you're in pain, it's hard to focus on anything else. Over-the-counter nonsteroidal anti-inflammatory drugs (NSAIDs) like ibuprofen can be very helpful in the short term. They work by reducing both pain and the inflammation that’s likely irritating the nerves around your bulging disc. While these medications can provide the relief you need to participate in physical therapy, they don't fix the underlying problem. Think of them as a tool to help you get through the toughest days while you work on a more permanent solution with your healthcare team.
Prescription Options for Severe Pain
If over-the-counter medications aren't providing enough relief, your doctor might suggest stronger options to manage severe pain. This could include prescription-strength pain relievers or muscle relaxers to help calm intense spasms that often accompany a bulging disc. For pain that stems directly from nerve irritation, medications like gabapentin are often used to specifically target and reduce those signals. In some cases, a more direct approach is needed. Your doctor may recommend corticosteroid injections, which deliver powerful anti-inflammatory medication right to the area around the affected nerve. These treatments are designed to break the cycle of severe pain, giving you the breathing room needed to fully engage in physical therapy and other corrective exercises that address the root of the problem.
Can Injections or Chiropractic Care Help?
For more persistent pain, your doctor might suggest an epidural steroid injection. This procedure delivers powerful anti-inflammatory medication directly to the area around the affected nerve, providing targeted relief from swelling and irritation. Another highly effective option is chiropractic care. Gentle, precise spinal adjustments can help restore proper motion to the spinal joints, which can alleviate pressure on the disc and surrounding nerves. This is especially helpful for low back pain that has lingered for a month or more, offering a path to relief without invasive procedures.
When to Consider Chiropractic Care
If your back pain has stuck around for more than a month and isn't responding to rest or basic care, it might be time to consider chiropractic care. The focus is on gentle, precise spinal adjustments that restore proper motion to your joints. This can take a significant amount of pressure off the bulging disc and the irritated nerves around it, offering a path to relief without invasive procedures. It’s a non-invasive way to address the structural side of the problem, which is a key part of our physical medicine approach. By improving your spine's alignment, you're not just finding temporary relief—you're helping your body heal for the long term.
Can Physical Therapy Heal a Bulging Disc?
If you’re dealing with the persistent pain of a bulging disc, you’re probably wondering what your options are. The good news is that physical therapy is often one of the most effective non-surgical treatments available. It’s a proactive approach that doesn’t just mask the pain; it addresses the underlying mechanical issues to provide lasting relief and prevent future flare-ups. The goal is to reduce pressure on the affected disc, improve your mobility, and strengthen the muscles that support your spine.
A skilled physical therapist acts as your guide, creating a customized plan that fits your specific condition and lifestyle. This isn't about pushing through pain with intense workouts. Instead, it’s a carefully designed program of gentle exercises and targeted therapies. By focusing on restoring proper movement and building strength, physical medicine helps your body heal itself. It empowers you with the tools and knowledge to manage your symptoms, get back to the activities you love, and feel more in control of your health.
Why a Strong Core Is Your Best Defense
Think of your core muscles—the ones in your abdomen, back, and pelvis—as a natural corset that supports your spine. When these muscles are weak, your spinal discs have to bear more of the load, which can contribute to issues like bulging discs. A key part of physical therapy is strengthening this support system. Your therapist will guide you through specific, controlled exercises designed to build core stability without straining your back. This isn't about doing endless crunches; it's about activating the deep, stabilizing muscles that are crucial for a healthy spine. A stronger core means less pressure on your discs and a solid foundation for all your movements.
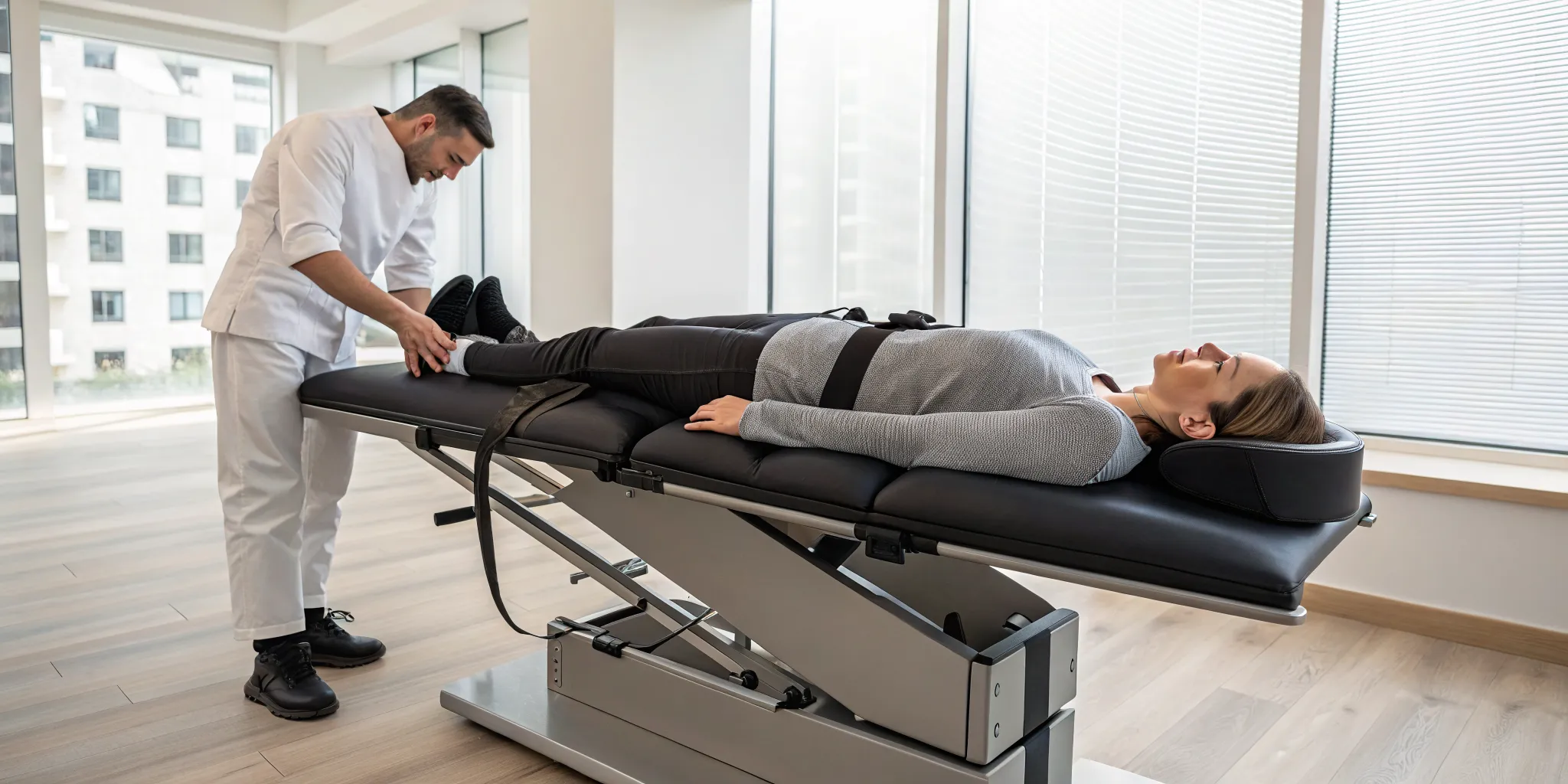
The Role of Manual Therapy and Traction
Physical therapy is more than just exercise. It often includes hands-on techniques that can provide significant pain relief and improve mobility. Your therapist might use manual therapy to gently mobilize your spine and release tight muscles that are contributing to your pain. Another common technique is spinal traction. This involves gently stretching the spine to create space between the vertebrae, which can help relieve pressure on the bulging disc and any compressed nerves. These hands-on approaches can lessen pain and improve daily function, making it easier for you to participate in your strengthening exercises and get back to your routine.
What to Expect From Your Recovery
Patience and consistency are your best friends during recovery. While every person’s healing journey is unique, most people with mild to moderate bulging discs start to feel significant improvement within six to eight weeks of consistent physical therapy. The goal is steady progress, not an overnight cure. You’ll learn to listen to your body, understanding which movements help and which to avoid. Your therapist will be there to adjust your program as you get stronger, helping you build resilience and confidence. Remember, the work you put in now is an investment in your long-term spinal health, helping you stay active and pain-free for years to come.
Lifestyle Changes for a Faster Recovery
While professional treatments are the foundation of your recovery, the small choices you make every day have a massive impact on your healing process. Think of these lifestyle adjustments as powerful tools you can use to support your body, reduce pain, and prevent future issues. It’s about taking an active role in your own recovery journey, which can be incredibly empowering when you're dealing with persistent pain. You have more control over your healing than you might think, and it starts with your daily habits.
You don't need to make drastic overhauls overnight. Instead, focus on incorporating small, sustainable changes into your routine. By paying attention to how you move, work, and rest, you can create an environment where your body can heal more effectively. These daily habits work in tandem with your physical medicine plan, helping to speed up recovery and build long-term resilience against future back problems. Simple shifts in your posture, a commitment to gentle movement, and prioritizing rest can significantly reduce the strain on your spine. It’s about creating a supportive environment for your back, both inside and out, and giving your body the best possible chance to get back to feeling great and staying that way.
Moving Your Body and Managing Your Weight
Carrying extra weight can place significant pressure on your spinal discs, making it harder for a bulging disc to heal. Finding a healthy weight for your body is one of the most effective ways to take the strain off your back. If you're unsure where to start, our functional medicine approach can help you create a personalized plan. Gentle, consistent exercise is also key. Activities like walking, swimming, or cycling are fantastic because they improve blood flow to the spine, strengthen your core and back muscles, and increase flexibility without jarring your body. The goal is to stay active in a way that feels good and supports your spine.
How to Fix Your Posture and Desk Setup
How you sit, stand, and walk all day long directly affects your spinal health. Poor posture puts unnecessary strain on your back and can aggravate a bulging disc. Pay attention to sitting up straight, keeping your shoulders back, and avoiding slouching. If you work at a desk, creating an ergonomic setup is crucial. Make sure your chair supports your lower back, your screen is at eye level, and your feet are flat on the floor. It’s also important to get up, stretch, and walk around every 30-60 minutes. These small breaks prevent your muscles from getting stiff and give your spinal discs a chance to decompress.
The Link Between Sleep, Stress, and Healing
Your body does its most important repair work while you sleep, making quality rest non-negotiable for healing a bulging disc. Aim for seven to eight hours of consistent sleep each night. You can improve your sleep quality by creating a relaxing bedtime routine and making sure your bedroom is dark, quiet, and cool. Just as important is managing your stress levels. Stress causes your muscles to tense up, which can increase pain and slow down the healing process. Simple mindfulness and relaxation techniques, practiced for just a few minutes each day, can make a world of difference in how you feel both mentally and physically.
More Therapies for Bulging Disc Pain Relief
While physical therapy and chiropractic care are cornerstones of bulging disc treatment, a truly holistic plan often includes other therapies that support your body’s healing process. These complementary approaches can help manage pain, reduce inflammation, and improve your overall well-being. Think of them as powerful allies in your recovery, working alongside your primary treatments to help you feel better faster. Integrating these methods can create a more comprehensive and personalized path to relief.
Could Acupuncture or Massage Provide Relief?
If you're dealing with persistent pain, both acupuncture and massage therapy can offer significant relief. Acupuncture, a key component of traditional Chinese medicine, uses fine needles to stimulate specific points on the body, which can help ease chronic back and neck pain from a bulging disc. Similarly, a targeted massage therapy session can do wonders for tight, tense muscles surrounding your spine. By easing muscle spasms and improving blood flow to the injured area, massage not only reduces pain but also creates a better environment for healing.
Specific Benefits of Acupuncture and Massage
These therapies go beyond simple relaxation; they create real physiological changes that support healing. Acupuncture works by stimulating specific points that can trigger the release of endorphins, your body's natural pain-relieving chemicals. It also helps to reduce inflammation around the irritated nerve root, which is often a primary source of bulging disc pain. Massage therapy complements this by directly addressing the tight, spasming muscles that often guard the injured area. By releasing this tension and increasing blood flow, massage helps deliver more oxygen and nutrients to the tissues that need it most, creating an optimal environment for your body to repair itself. These hands-on approaches are a key part of a comprehensive physical medicine plan, helping to restore balance and function.
When to Use Heat vs. Cold Therapy
Knowing when to use heat versus cold can make a big difference in your day-to-day comfort. In the initial stages of an injury or after an activity that causes a flare-up, applying a cold pack is your best bet. The cold helps constrict blood vessels, which can reduce swelling and numb the sharp pain. After a few days, or when the initial inflammation has subsided, you can switch to gentle heat. A warm compress or heating pad helps relax tight muscles and increase circulation, bringing more oxygen and nutrients to the area to promote healing and provide soothing symptom relief.
Eating to Reduce Inflammation
What you eat has a direct impact on your body's inflammation levels, which is a key factor in bulging disc pain. Adopting an anti-inflammatory diet can be a powerful tool for managing your symptoms from the inside out. Focus on incorporating foods rich in omega-3 fatty acids, like salmon and walnuts, which are known for their inflammation-fighting properties. Spices like turmeric and ginger are also excellent additions. By fueling your body with nutrient-dense foods, you can help heal a bulging disc naturally and support your long-term spinal health.
How Long Does Recovery Take?
One of the first questions on everyone’s mind is, "How long until I feel better?" It's completely understandable to want a clear finish line. While there's no single answer that fits everyone, the good news is that most people find significant relief with non-surgical treatments. Recovery is a process, and your body needs time to heal. The key is to focus on consistent progress rather than a specific date on the calendar.
Your healing journey will depend on several factors, including the severity of your disc bulge, your overall health, and how consistently you follow your treatment plan. Think of it less like a sprint and more like a steady walk toward feeling like yourself again. With a personalized approach that combines therapies like physical medicine and lifestyle adjustments, you can create the best possible environment for your body to repair itself. We'll break down what a typical timeline looks like and the signs that show you're on the right track.
What to Expect from Your Treatment Timeline
While every person's body heals at its own pace, we can look at some general timelines to set realistic expectations. For many people, mild to moderate cases of a bulging disc can heal within six to eight weeks with a dedicated physical therapy plan. This doesn't mean you'll be pain-free overnight, but you should notice a gradual reduction in symptoms and an increase in your ability to move comfortably. If your condition is more severe, especially if it involves nerve compression, recovery may take a bit longer. The focus is always on steady, forward progress and celebrating small wins along the way, like being able to walk a little farther or sit without pain for longer.
What Affects Your Healing Time?
Your recovery timeline is unique to you and is influenced by a few key things. The severity of the disc bulge is a major factor, as is your overall health and age. But one of the most important elements you can control is your commitment to your treatment plan. You can typically expect to see the benefits of physical therapy within four to six weeks of consistent effort, though complete healing can take several months. Your body's ability to heal is also impacted by lifestyle choices. Things like maintaining a healthy weight, staying hydrated, avoiding smoking, and managing stress all play a supportive role in helping you get back on your feet faster.
What Happens if a Bulging Disc Goes Untreated?
It’s tempting to hope that back pain will just resolve on its own, but ignoring a bulging disc can be a risky strategy. While some minor discomfort might fade, an untreated disc bulge can get progressively worse, especially if you continue the activities that caused the strain in the first place. Over time, this can lead to more persistent pain, numbness, or even a loss of feeling in your arms or legs. Pay close attention to any worsening symptoms, like tingling or weakness, as these are clear signs that the nerve is becoming more irritated. Getting a proper diagnosis and starting a conservative treatment plan is the best way to address the problem before it becomes more serious, helping you avoid the need for more invasive procedures down the road.
Signs Your Bulging Disc Therapy Is Working
It’s encouraging to know that your efforts are paying off. Progress isn't always linear, but you can look for specific signs that you're healing. One of the first things you might notice is that your pain becomes less intense or less frequent. Another great sign is pain centralization—when pain that has traveled down your leg or arm starts to retreat back toward your spine. You’ll also find yourself able to do more with less discomfort, whether that’s standing at the counter to cook dinner or taking a longer walk. Research shows that nearly 90% of people improve within six weeks using conservative treatments, which is a powerful reminder that your body is capable of healing.
When Is Surgery Necessary?
The thought of surgery can be intimidating, so let’s clear the air: it is rarely the first step in treating a bulging disc. The vast majority of people find lasting relief through non-surgical treatments that focus on reducing pain, calming inflammation, and strengthening the body to prevent future problems. At Ascend Functional Health, our entire approach is built on giving your body the support it needs to heal itself through conservative methods like physical medicine and chiropractic care. Surgery is typically only considered when these effective, less invasive strategies have been explored but haven't provided the necessary relief, and your quality of life is still significantly impacted.
Who Is a Candidate for Surgery?
So, when does the conversation shift toward a surgical solution? A surgeon might recommend an operation if you're experiencing severe, persistent pain that conservative treatments can't manage, making it difficult to perform daily activities. The other major factor is the presence of neurological issues. This includes progressive weakness, numbness, or tingling in your arms or legs that doesn't improve. In rare cases, there are absolute surgical indications, such as cauda equina syndrome, a serious condition involving loss of bladder or bowel control that requires immediate medical attention. These situations are the exception, not the rule, but they are important to be aware of.
Common Surgical Procedures
If you and your medical team decide that surgery is the best path forward, it’s helpful to know what the options are. The type of procedure recommended will depend on the specifics of your condition, including the location of the bulging disc and the severity of your symptoms. The goal of any surgical intervention is to take pressure off the compressed nerve root to relieve pain and restore function. Let's look at two of the most common procedures performed for disc-related issues.
Microdiskectomy
A microdiscectomy is a minimally invasive procedure that has become a gold standard for relieving nerve pressure. During this surgery, the surgeon removes only the small portion of the disc that is bulging out and pressing on the nerve. Because it’s less invasive, it often results in a quicker recovery time. This procedure has a very high success rate, with studies showing that it effectively relieves pain for most patients, allowing them to return to their normal activities with significantly less discomfort.
Diskectomy and Spinal Fusion
In cases where the disc is severely damaged or the spine is unstable, a more extensive procedure may be necessary. A discectomy involves removing the entire damaged disc. Because removing the disc can create instability between the vertebrae, the surgeon will often perform a spinal fusion at the same time. This involves joining the two vertebrae together with bone grafts and hardware to create a single, solid bone. This approach is designed to alleviate pain and restore function, particularly for patients who haven't found relief with other treatments.
Common Myths About Bulging Discs, Busted
When you're dealing with back pain, it's easy to fall down a rabbit hole of online information. Unfortunately, a lot of what you'll find about bulging discs is outdated or just plain wrong. These myths can create unnecessary fear and might even steer you away from the treatments that could actually help. Let's clear the air and debunk a couple of the most common misconceptions so you can move forward with confidence and a clear plan for your recovery. Understanding the truth is the first step toward effective healing.
Myth: Surgery Is Your Only Option
Hearing the words "bulging disc" can immediately make you think of operating rooms and long recovery times. But the idea that surgery is your only option is one of the biggest myths out there. The truth is, surgery is rarely the first line of defense. Many people find significant, lasting relief through conservative, non-surgical treatments. Our approach to Physical Medicine focuses on things like targeted exercises, chiropractic care, and simple lifestyle adjustments that can be incredibly effective at managing your symptoms and helping your body heal. Our goal is always to explore these powerful, less invasive options first to get you back to feeling your best.
Why Conservative Treatment Is Usually Successful
Conservative treatments are so effective because they address the root of the problem instead of just masking the pain. The goal is to create an environment where your body can heal itself. By reducing inflammation, taking pressure off the affected nerve, and strengthening the muscles that support your spine, you’re not just finding temporary relief—you’re building long-term resilience. This holistic approach is why nearly 90% of people see improvement within six weeks. Our approach to physical medicine is built on this principle: we create a personalized plan that supports your body’s natural healing process, helping you regain strength and function without invasive procedures.
Myth: You Should Stop Moving Completely
When you're in pain, your first instinct might be to curl up on the couch and stay there. While a little rest is okay, the belief that you should completely stop moving is a myth that can actually slow down your recovery. In fact, prolonged bed rest isn't recommended for a bulging disc. Gentle, strategic movement is key to healing. Engaging in specific stretches and exercises helps reduce pain, improve flexibility, and strengthen the core muscles that support your spine. It might seem counterintuitive, but staying active under the guidance of a professional is one of the best things you can do to promote healing and prevent future issues.
Prevention Is Key: Protecting Your Spine
While it's great to know how to treat a bulging disc, an even better strategy is to prevent one from happening in the first place. Protecting your spine isn't about being fragile or avoiding activity; it's about building a strong, resilient foundation that can handle the demands of daily life. By adopting a few key habits, you can significantly reduce your risk of injury and keep your back feeling great for the long haul. Think of it as investing in your future self. These proactive steps empower you to take control of your spinal health, ensuring you can stay active and enjoy the things you love without being held back by pain.
Mastering Proper Lifting Techniques
We’ve all heard the advice to "lift with your legs, not your back," but what does that actually look like? It’s simpler than you think. Before you pick something up, get close to the object and plant your feet firmly. Instead of bending at the waist, bend your knees and hips to squat down, keeping your back straight and your core muscles engaged. Grip the object, and then use the power of your leg muscles to stand up, keeping the item close to your body. This technique transfers the strain from your vulnerable spinal discs to your strong leg and glute muscles. It’s a small change in movement that makes a huge difference, whether you’re lifting a heavy box or just a bag of groceries.
The Role of Stretching and Exercise
Consistent, mindful movement is one of the best things you can do for your spine. Physical therapy is a cornerstone of bulging disc treatment because it works, and the same principles apply to prevention. A targeted exercise routine helps strengthen the core muscles that act as a natural brace for your spine, improves flexibility to allow for a greater range of motion, and helps you maintain good posture. When your supporting muscles are strong and your spine is flexible, your discs are better protected from daily wear and tear. Our Physical Medicine programs are designed to build this exact kind of functional strength, creating a resilient body that's less susceptible to injury.
Lifestyle Choices That Impact Spinal Health
The small choices you make every day add up to have a massive impact on your long-term spinal health. Carrying extra weight, for example, places constant pressure on your spinal discs, increasing the risk of injury. Finding a healthy weight for your body is one of the most effective ways to take that strain off your back. Beyond weight, staying hydrated is crucial, as your discs need water to stay plump and effective as shock absorbers. An anti-inflammatory diet can also help reduce systemic inflammation that might contribute to disc problems. These daily habits support your body from the inside out, creating an environment that promotes strength and healing.
How to Create Your Personal Treatment Plan
Finding relief from a bulging disc isn’t about a single magic bullet; it’s about creating a smart, comprehensive plan that’s tailored specifically to you. Your body, symptoms, and lifestyle are unique, which means your recovery path should be, too. A successful treatment plan often involves a combination of therapies that work together to reduce pain, address inflammation, and strengthen your body to prevent future issues. This integrated approach looks at the whole picture, moving beyond just managing symptoms to address the root cause of your discomfort.
Think of it as building a custom roadmap to recovery. A generic map might get you into the right city, but a personalized one guides you directly to your destination, accounting for your starting point, your preferred route, and any roadblocks along the way. Your treatment plan should do the same, considering factors like your activity level, the demands of your job, and your overall health goals. By working with a team that listens and understands your specific needs, you can build a strategy that helps you heal effectively and get back to feeling your best, with a clear path forward.
Who Should Be on Your Healthcare Team?
The first step in your recovery is getting an accurate diagnosis from a professional. A bulging disc should be evaluated by a qualified specialist who can pinpoint the exact issue and recommend the right course of action. Your healthcare team might include a chiropractor, a physical therapist, and a functional medicine practitioner who can collaborate on your care. This team approach ensures all aspects of your health are considered, from spinal alignment to underlying inflammation. At Ascend, our Physical Medicine services bring together experts who can create a cohesive and personalized plan designed just for you.
Combining Therapies for Better Results
For most people, non-surgical options are highly effective. In fact, physical therapy is often a first-line treatment that helps people avoid surgery and return to the activities they love. The most successful recovery plans combine several strategies. Your plan might include chiropractic adjustments to restore proper motion, targeted exercises to strengthen your core, and anti-inflammatory nutritional guidance to support healing from the inside out. This multi-faceted approach, which is central to Functional Medicine, ensures you’re not just masking the pain but building a stronger, more resilient body for the long term.
Related Articles
- How to Heal a Bulging Disc Naturally
- Treating a Herniated Disc with Physical Therapy
- Physical Therapy for Herniated Disc: What Really Works?
- Herniated disk: Diagnosis and treatment
Frequently Asked Questions
How can I tell if my pain is from a bulging disc or just a regular backache? A typical muscle strain usually feels like a localized ache or soreness that gets better with a few days of rest. Pain from a bulging disc often has a different character because it can involve a nerve. You might feel sharp, shooting pain that travels from your back down into your leg (sciatica) or from your neck into your arm. Numbness, tingling, or weakness in your limbs are also key signs that something more than a simple muscle issue is going on. The only way to know for sure is to get a professional evaluation.
Can a bulging disc heal completely on its own? While the pain from a bulging disc can sometimes fade on its own, the underlying structural problem usually doesn't resolve without some help. If the poor posture or muscle weakness that caused the bulge isn't addressed, the issue is likely to return or even get worse over time. Proactive treatment helps correct these root causes, strengthening your spine and reducing the risk of future flare-ups so you can find lasting relief.
Is it safe to exercise if I have a bulging disc? Yes, and in fact, the right kind of movement is essential for your recovery. The key is to focus on gentle, controlled exercises that strengthen your core and support your spine without putting stress on the disc. High-impact activities or movements that involve heavy twisting should be avoided, especially early on. Working with a physical therapist is the best way to learn which exercises are safe and beneficial for your specific condition.
What's the main difference between chiropractic care and physical therapy for this condition? Think of them as two skilled specialists working on the same team. A chiropractor primarily focuses on the health of your spinal joints, using precise adjustments to restore proper motion and take pressure off the disc and nerves. A physical therapist focuses more on the surrounding muscles and your overall movement patterns, guiding you through exercises to build strength, stability, and flexibility. Both are incredibly valuable, and using them together often leads to the best results.
Do I have to give up my favorite activities forever? The goal of any good treatment plan is to get you back to doing the things you love, not to create a long list of restrictions. While you may need to temporarily modify or take a break from certain high-impact activities during the initial healing phase, the work you do in physical therapy and chiropractic care is designed to build a stronger, more resilient body. This helps you return to your hobbies with confidence and a better understanding of how to move safely.