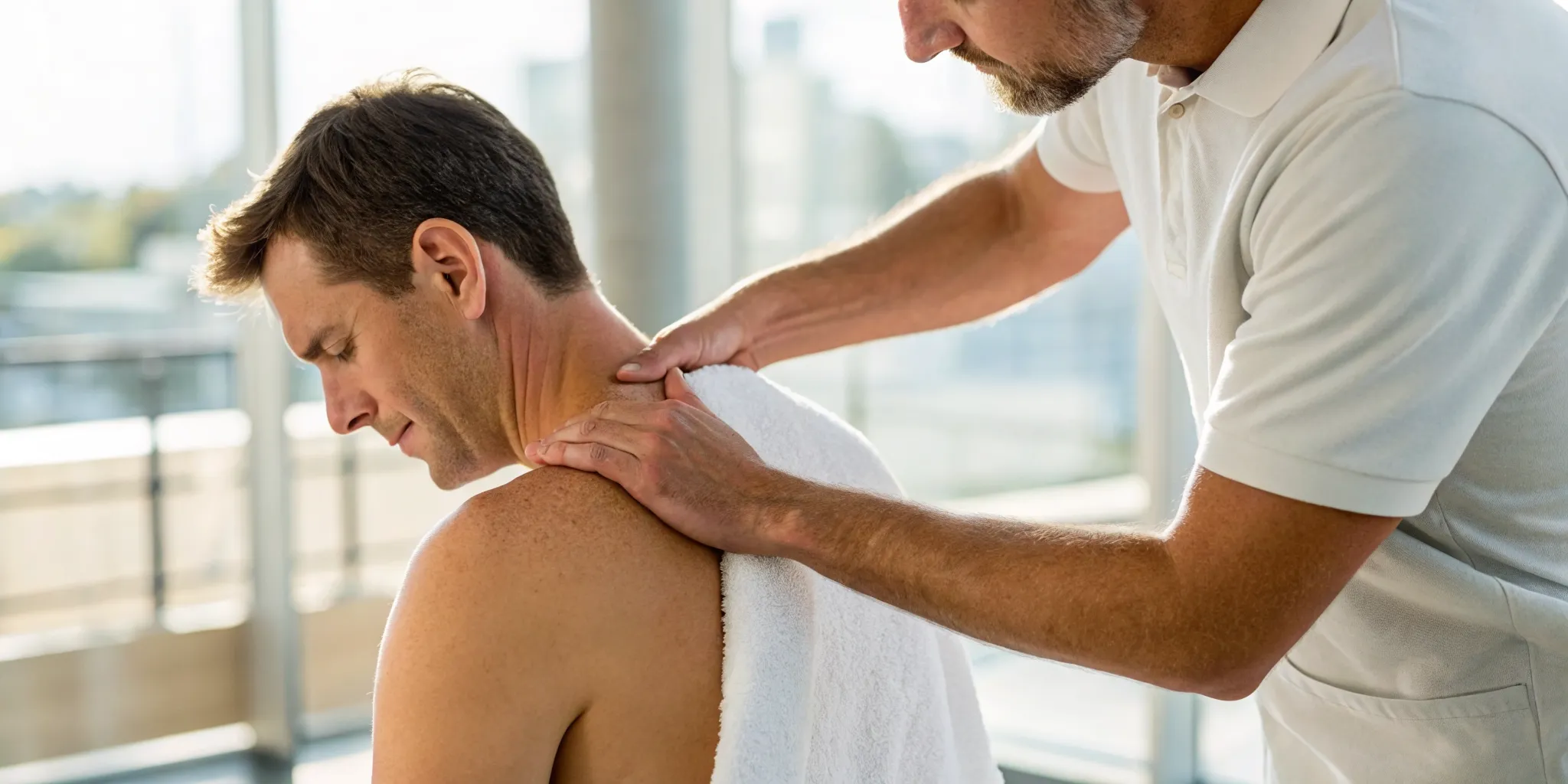
Your spine carries the load of your entire day, from sitting at a desk to lifting groceries to playing with your kids. Over time, all that work can lead to wear and tear, sometimes resulting in a painful disc bulge. True healing requires more than just treating the spot that hurts; it demands a holistic view of how your body moves and functions. A comprehensive disc bulge therapy plan looks at your whole lifestyle, from your posture and core strength to your diet and daily habits. By addressing these foundational elements, you not only alleviate current pain but also build a stronger, more resilient back for the future.
Key Takeaways
- Recognize the Telltale Signs: A disc bulge often causes more than just back pain; look for radiating pain down your leg (sciatica), numbness, tingling, or muscle weakness. Identifying these specific symptoms is the first step toward getting an accurate diagnosis and effective care.
- Prioritize Non-Surgical Solutions: The majority of disc bulges heal without surgery. A combination of physical therapy, chiropractic care, and spinal decompression is a powerful, effective approach to relieve pressure on the nerve and support your body’s natural healing process.
- Adopt Proactive Habits for Prevention: Your daily choices are your best defense against future back problems. Focus on strengthening your core, maintaining a healthy weight, and practicing good posture and lifting mechanics to build a resilient spine for the long term.
What Is a Disc Bulge and How Does It Happen?
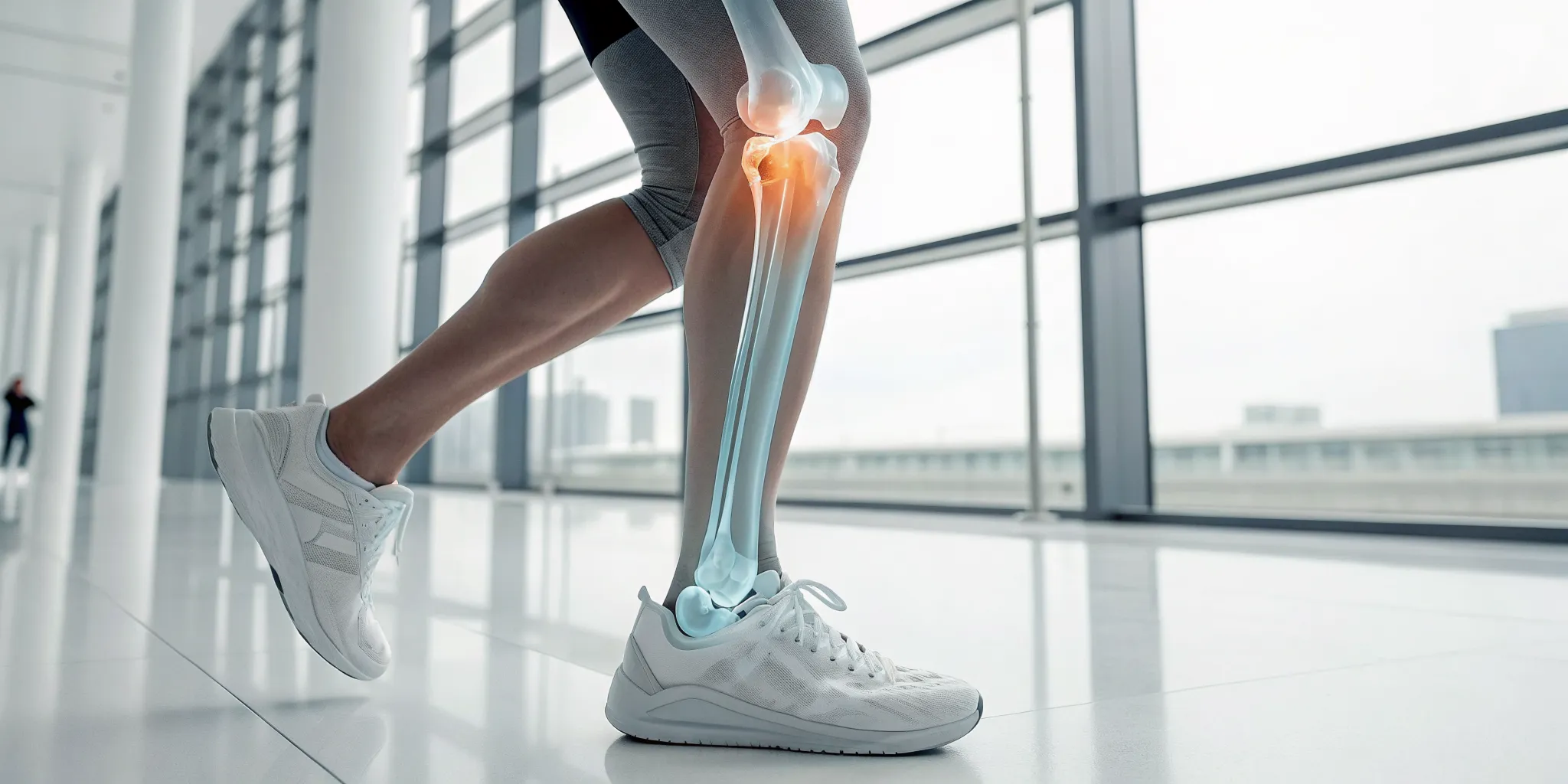
If you’re dealing with persistent back pain, you’ve probably heard the term “disc bulge.” It sounds serious, but it’s a common condition that often responds well to non-surgical care. A disc bulge happens when the soft, gel-like center of one of your spinal discs pushes against its tough outer layer, causing it to swell or protrude outward. Think of it like a jelly donut that’s been squeezed a little too hard, making the filling press against the dough.
This protrusion can be problematic because it might press on nearby spinal nerves. When a nerve gets compressed, it can trigger a range of uncomfortable symptoms. You might feel sharp pain in your lower back, or a radiating pain known as sciatica that travels down your leg. Some people also experience numbness, tingling, or even muscle weakness in the affected areas. Understanding what’s happening in your spine is the first step toward finding the right path to healing, and our approach to physical medicine focuses on addressing these root causes directly.
A Quick Look at Your Spinal Discs
Your spine is made up of a stack of bones called vertebrae, and in between each one is a spinal disc. These discs are your body’s natural shock absorbers. They have a tough, fibrous outer ring and a soft, jelly-like center. This structure allows them to be both strong and flexible, protecting your spine as you bend, twist, and move through your day. A disc bulge occurs when a tear or weak spot develops in that tough outer ring, allowing the inner "jelly" to push out. This is what creates the bulge that can irritate surrounding nerves and cause pain.
What Causes a Disc Bulge?
Disc bulges can happen for a few different reasons, and it’s often a combination of factors. The most common cause is simply the natural aging process. Over time, our spinal discs lose some of their water content and become less flexible, making the outer layer more prone to tiny tears. An acute injury, like a fall or lifting something too heavy with improper form, can also cause a disc to bulge suddenly. Repetitive movements, especially those involving frequent bending or twisting, can put cumulative stress on your discs, leading to gradual wear and tear. Identifying the source of the problem is key to creating a lasting solution for the conditions we treat.
Are You at Risk?
While anyone can develop a disc bulge, certain factors can increase your likelihood. Age is a big one, with people between 30 and 50 being most commonly affected. Other risk factors include:
- A sedentary lifestyle: Sitting for long periods puts more pressure on your spinal discs.
- Being overweight: Excess body weight adds stress to the discs in your lower back.
- Smoking: Nicotine can restrict blood flow to the discs, hindering their ability to repair themselves.
- Genetics: A family history of disc problems can make you more susceptible.
- Occupation: Jobs that require repetitive lifting, bending, or driving can take a toll on your spine.
Knowing your risk factors can help you make proactive changes. Our team is here to help you build a personalized plan to support your spinal health, and you can learn more about our approach.
How to Know If You Have a Disc Bulge
Figuring out the source of your pain is the first step toward finding relief. A disc bulge, sometimes called a slipped or herniated disc, happens when the soft, cushion-like discs between your vertebrae get pushed out of place. This can put pressure on your spinal cord and surrounding nerves, leading to a range of uncomfortable symptoms. While the idea of a spinal issue can sound scary, understanding the specific signs can help you determine your next steps and seek the right care. Recognizing these symptoms early on is key to preventing further complications and starting on the path to recovery.
Key Symptoms to Look For
So, what does a disc bulge actually feel like? The experience can vary, but there are some common signs. You might feel a persistent ache or stiffness in your lower back. For many, the most telling symptom is a sharp, shooting pain that travels down one leg, a condition known as sciatica. This happens when the bulging disc presses on the sciatic nerve. Along with pain, you might notice tingling, numbness, or even weakness in your leg or foot. These sensations occur because the nerve signals are being interrupted. If these symptoms sound familiar, it’s a good indication that one of your spinal discs may be the culprit.
Red Flags: When to See a Doctor
While some back pain can be managed at home, certain symptoms are red flags that you shouldn't ignore. It's time to see a doctor if the pain is severe enough to interfere with your daily activities, like working or sleeping. If your symptoms haven't improved after four to six weeks, or if they're getting worse, it's important to get a professional evaluation. You should also seek immediate medical attention if you experience significant weakness in your limbs or lose control of your bladder or bowels, as this could signal a serious issue. Don't wait it out; getting a proper diagnosis is crucial for effective physical medicine treatment.
How a Disc Bulge Is Diagnosed
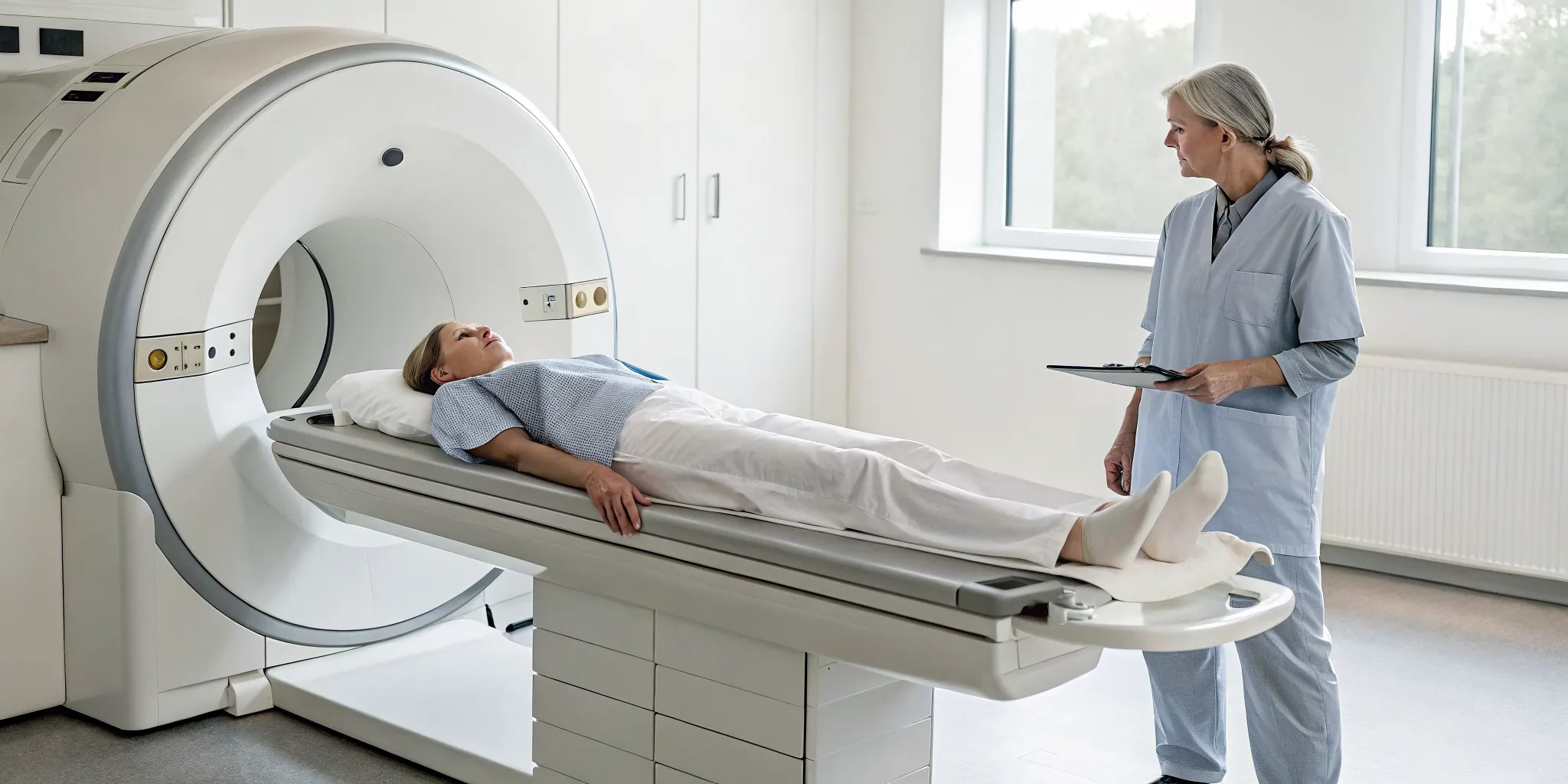
When you see a specialist, they will start by discussing your medical history and symptoms. For many people, this conversation combined with a physical exam is enough to make a diagnosis. During the exam, your doctor will check your reflexes, muscle strength, and your ability to feel different sensations. They might perform a "straight leg raise test," where they gently lift your leg while you lie on your back. Pain during this test is a strong indicator of a herniated disc. In some cases, your doctor may order imaging tests like an MRI or X-ray to get a clearer picture of your spine and confirm the diagnosis.
What Are the Best Non-Surgical Treatments?
If you’re dealing with a disc bulge, your first thought might be surgery. But the good news is that most cases can be resolved with conservative, non-surgical treatments. The goal is to reduce pain and inflammation while giving your body the support it needs to heal. Finding the right combination of therapies can help you get back to your life without going under the knife. It’s all about taking a proactive approach to your recovery, starting with gentle, effective methods that address the root of the problem.
Many people find lasting relief by exploring these options first, which can range from targeted exercises and chiropractic care to simple at-home remedies. This approach not only manages your symptoms but also helps correct the underlying issues that led to the disc bulge in the first place, setting you up for better long-term spinal health. The key is patience and consistency. Healing takes time, and working with a healthcare provider who understands your unique situation is crucial. They can help you create a personalized treatment plan that combines several strategies for the best results. Below, we’ll explore some of the most effective non-surgical treatments available, so you can feel empowered to make the best choice for your body and your lifestyle.
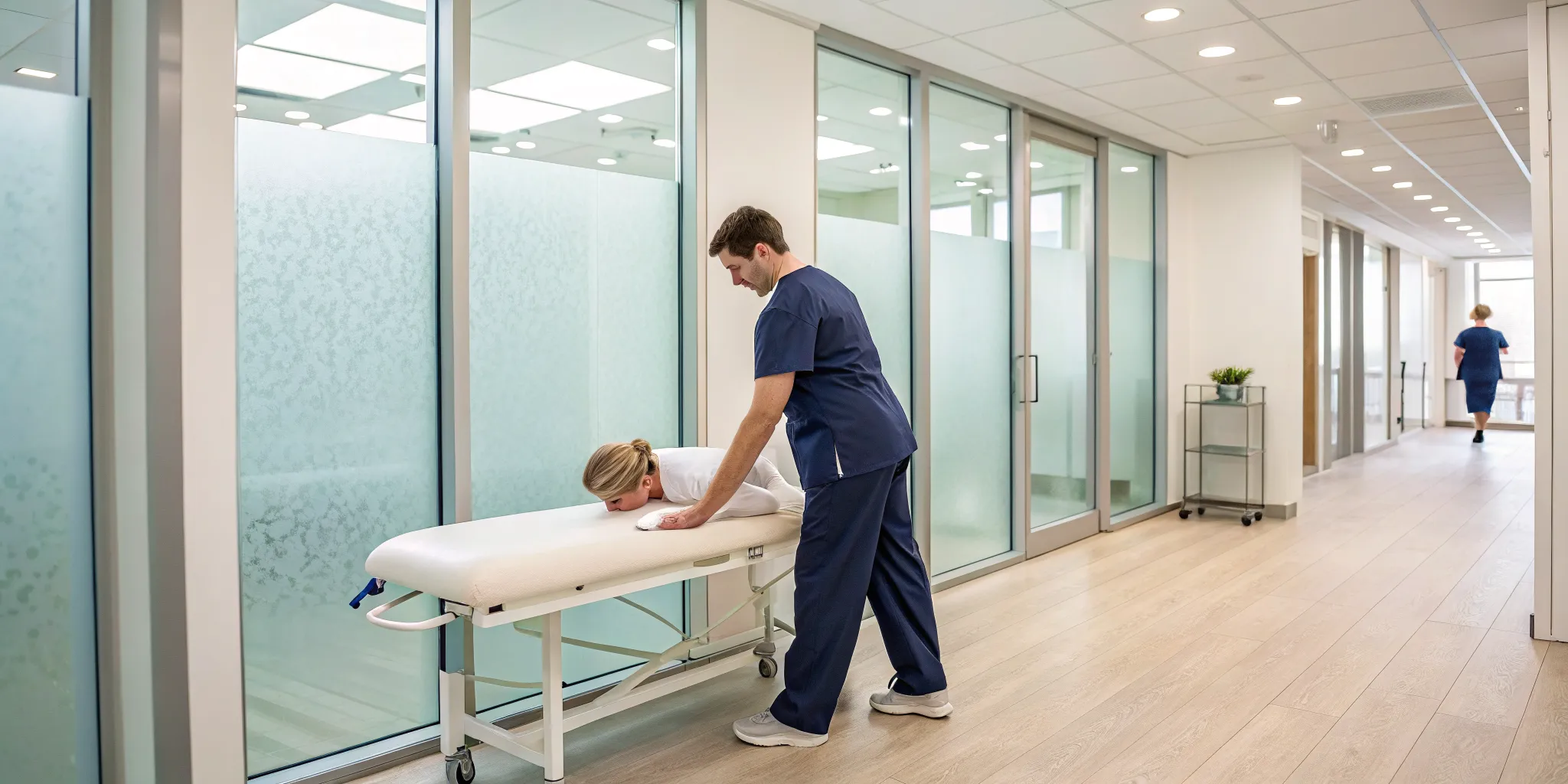
Physical Therapy and Specific Exercises
One of the most effective ways to manage a disc bulge is through physical therapy. A therapist can guide you through specific exercises designed to take pressure off your spinal nerves and lessen pain. The focus is often on strengthening your core muscles, which act as a natural corset for your spine, providing stability and support. Improving your flexibility is also key, as it helps restore normal movement and prevents future injuries. At Ascend, our physical medicine programs create a personalized plan to help you build strength and find lasting relief.
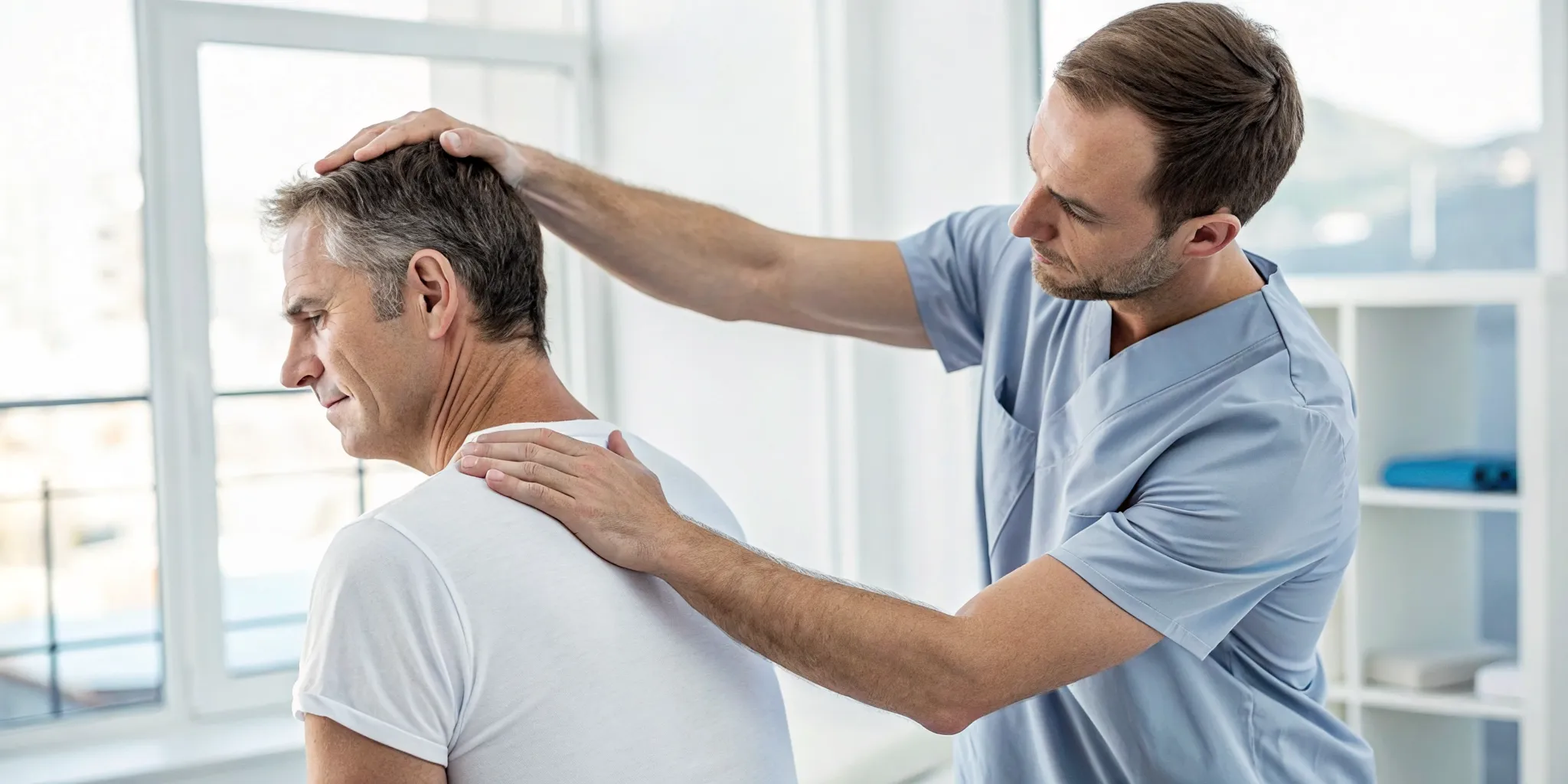
Chiropractic Care and Spinal Decompression
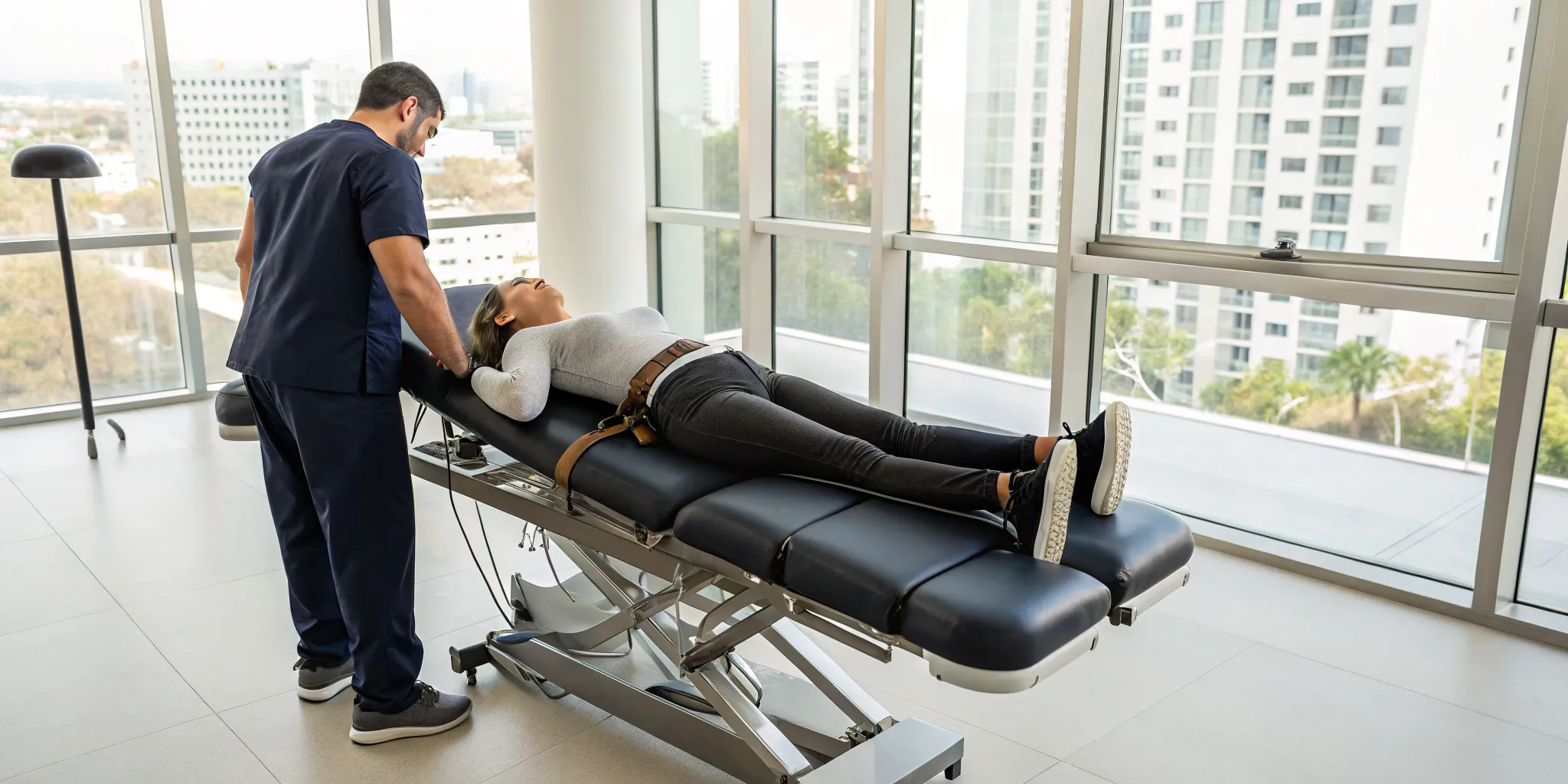
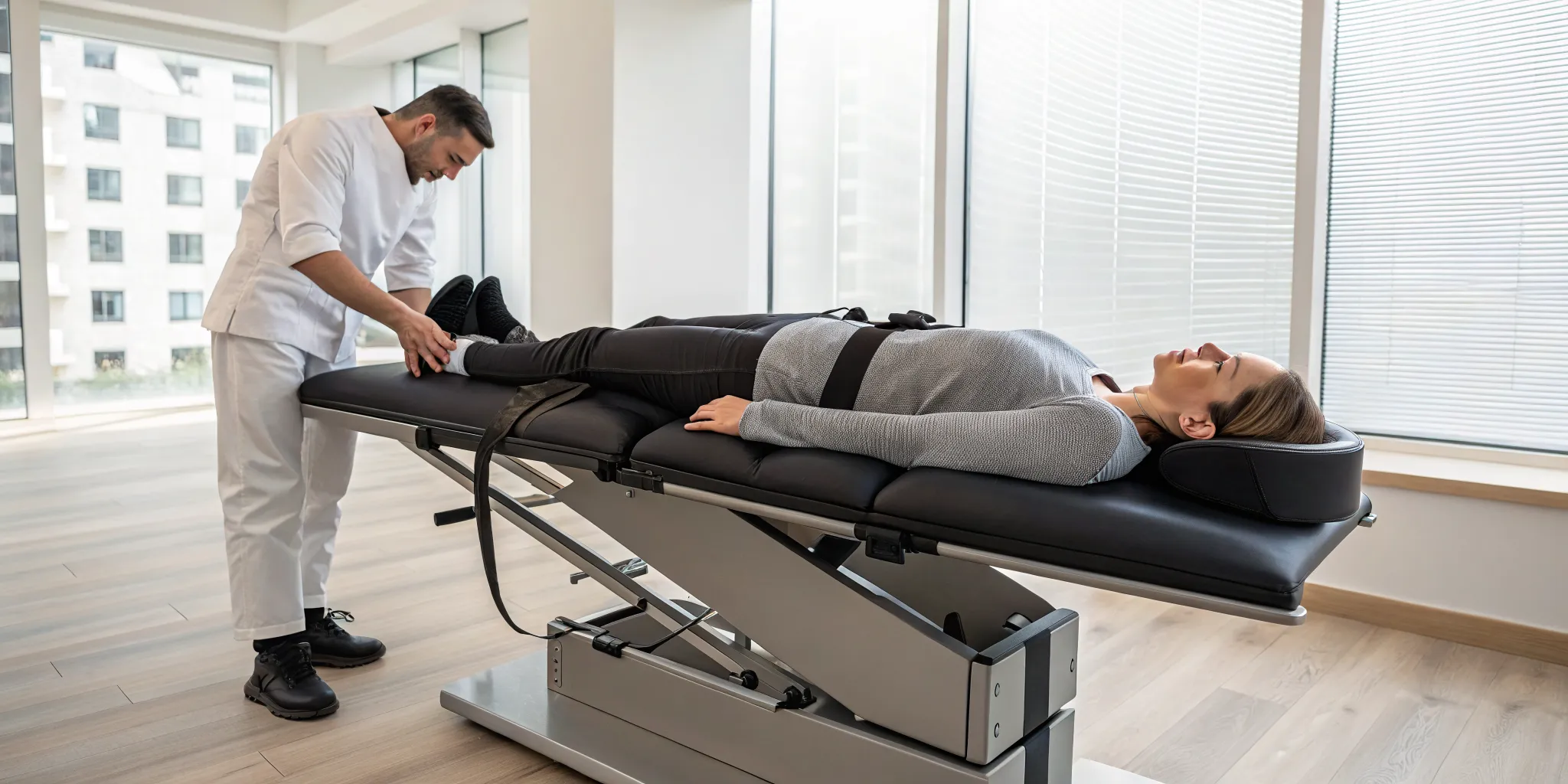
Chiropractic care is another excellent non-surgical option for disc-related pain. Gentle spinal adjustments can help realign your vertebrae, which may reduce pressure on the bulging disc and surrounding nerves. This can be particularly helpful for lower back pain that has lingered for a month or more. Another powerful technique is non-surgical spinal decompression, which uses a specialized table to gently stretch the spine. This creates negative pressure within the disc, helping it retract and allowing for better flow of healing nutrients.
Epidural Steroid Injections
When pain is severe and doesn't respond to other treatments, your doctor might suggest an epidural steroid injection. This procedure involves injecting a steroid medication near the irritated spinal nerves to reduce swelling and inflammation. Doctors typically use an X-ray to guide the needle to the precise location, ensuring the medication gets right to the source of the pain. While these injections can provide significant short-term relief, they are often used as a tool to make other therapies, like physical therapy, more manageable, rather than a standalone long-term solution.
Medication for Pain Management
Medication can be a useful tool for managing the acute pain and inflammation from a disc bulge, allowing you to participate more comfortably in your recovery therapies. Over-the-counter pain relievers like ibuprofen or acetaminophen are often the first line of defense. If those aren't enough, a doctor might prescribe stronger anti-inflammatory drugs or muscle relaxants to calm spasms. The goal is to use medication to control symptoms while you work on addressing the underlying cause of the disc bulge through more corrective treatments.
Applying Heat and Cold Therapy
Don’t underestimate the power of simple heat and cold therapy. When the injury is new and inflammation is high, applying cold packs for about 15 minutes at a time can help reduce swelling and numb the sharp pain. After a few days, or for more chronic, dull aches, switching to gentle heat can work wonders. A heating pad or warm bath helps relax tight muscles and increases blood flow to the area, which promotes healing. Alternating between the two can provide a well-rounded approach to managing your discomfort at home.
Which Lifestyle Changes Can Help You Heal?
While targeted treatments are essential for healing a disc bulge, the small choices you make every day have a massive impact on your recovery. Think of these lifestyle adjustments as the foundation that supports your professional care. By changing a few key habits, you can reduce inflammation, take pressure off your spine, and build a stronger, more resilient back for the long haul. It’s about creating an environment where your body can truly heal.
Eating an Anti-Inflammatory Diet
What you eat can either fuel inflammation or fight it. For disc-related pain, which is often tied to inflammation, your diet is a powerful tool. Start by incorporating foods known for their anti-inflammatory properties. This includes fatty fish like salmon, which is rich in omega-3s, as well as walnuts and spices like turmeric. On the flip side, try to limit processed foods, sugar, and refined carbohydrates that can make inflammation worse. Staying well-hydrated is also crucial, as water helps keep your spinal discs plump and healthy. Our functional medicine approach often starts with nutrition because it’s fundamental to reducing systemic inflammation and supporting your body’s healing process.
Correcting Your Posture and Strengthening Your Core
Think of your core muscles as a natural corset that supports and stabilizes your spine. When these muscles are weak, your spinal discs and joints take on extra strain, which can contribute to a bulge. Simple exercises like planks, bridges, and pelvic tilts can make a huge difference in building core strength. Good posture is just as important. Whether you’re sitting at a desk or standing in line, try to keep your spine in a neutral position. Avoid slouching and be mindful of your alignment throughout the day. This is a key part of the physical medicine we practice, as it corrects the underlying mechanics that lead to pain.
Managing Your Weight to Support Your Spine
Carrying extra weight places significant, constant pressure on the discs in your lower back. Even losing a small amount of weight can provide substantial relief and reduce the risk of further injury. By maintaining a healthy weight, you lighten the load your spine has to carry every single day. This isn’t about a crash diet; it’s about making sustainable changes that support your overall well-being and protect your back. Combining an anti-inflammatory diet with gentle, low-impact movement like walking or swimming can help you manage your weight effectively while aiding your recovery. This holistic view is central to treating the many conditions we see.
Modifying Your Daily Movements
How you move matters. Everyday actions like lifting groceries, getting out of a car, or even sitting for long periods can aggravate a disc bulge if done incorrectly. It’s essential to become more mindful of your body mechanics. When lifting anything, bend at your knees and hips, not your waist, and keep the object close to your body. Avoid sudden twisting motions, which can be particularly harmful to your discs. If you have a desk job, make a point to get up, stretch, and walk around every 30 minutes to prevent your back from getting stiff and sore. These small adjustments protect your spine from unnecessary stress.
What Exercises Can Help Your Recovery?
When you're dealing with a disc bulge, the thought of exercise might seem daunting, but gentle, targeted movement is one of the most effective ways to find relief and support your body's healing process. The right exercises can strengthen the muscles that support your spine, improve flexibility, and reduce pressure on the affected disc. It’s all about working smarter, not harder.
Before you start any new exercise routine, it's crucial to get a proper diagnosis and personalized recommendations. The exercises below are commonly suggested for disc bulge recovery, but your body is unique. Working with a professional who understands spinal health ensures you’re doing what’s best for your specific condition. At Ascend, our physical medicine approach focuses on creating a customized plan that helps you heal safely and effectively. Think of these exercises as a starting point for a conversation with your healthcare provider.
Pelvic Tilts and Bridges
Pelvic tilts and bridges are foundational exercises for rebuilding strength in your core and lower back. When these muscles are strong, they act like a natural brace for your spine, taking pressure off your discs. A pelvic tilt is a subtle but powerful movement where you lie on your back with your knees bent and gently flatten your lower back against the floor. This small motion activates deep core muscles. Bridges take it a step further by having you lift your hips off the floor, which strengthens your glutes and hamstrings. These muscles are key players in supporting your lumbar spine and promoting better alignment.
Cat-Cow and Child's Pose
If your back feels tight and stiff, Cat-Cow and Child's Pose can feel incredibly soothing. These gentle stretches, borrowed from yoga, are designed to improve spinal flexibility and release tension. During the Cat-Cow stretch, you move your spine through gentle flexion and extension, which helps mobilize the vertebrae and hydrate the discs. Child's Pose offers a gentle stretch for your entire back, hips, and shoulders. It’s a restorative posture that can help calm your nervous system and ease the muscle guarding that often accompanies back pain. These movements encourage blood flow to the area, which is essential for healing.
Knee-to-Chest Stretches
The knee-to-chest stretch is a simple way to get targeted relief for lower back pain. By lying on your back and gently pulling one or both knees toward your chest, you create a mild stretch in the lumbar spine. This action can help decompress the area, creating more space for the nerves and reducing the pinching sensation that a disc bulge can cause. It’s a go-to move for many people experiencing discomfort because it’s easy to control the intensity of the stretch. Remember to move slowly and avoid any sharp or shooting pain. Listening to your body is key.
Core Stabilization Exercises
A strong, stable core is your best defense against future back problems. Core stabilization exercises, like planks and bird-dogs, train the muscles of your abdomen and back to work together to protect your spine. Unlike crunches, which can sometimes put stress on the discs, these exercises focus on maintaining a neutral spine while challenging your stability. A plank, for example, teaches your entire core to fire up and hold your body in a straight line. Consistently practicing these movements helps build endurance in the muscles that support your lumbar region, reducing the daily strain on your spine.
When Is Surgery the Right Choice?
Deciding on surgery is a significant step, and it’s rarely the first option for a disc bulge. The goal of holistic care is always to help your body heal with the least invasive methods possible. At Ascend, we focus on comprehensive physical medicine to address the root cause of your pain, using techniques like chiropractic adjustments and spinal decompression to give your body the support it needs to recover. Most people find significant relief through these conservative treatments.
However, there are times when surgery becomes a necessary conversation. This usually happens after you’ve diligently tried non-surgical options without seeing the improvement you need. It’s not about failure; it’s about finding the right path for your specific situation. The decision to proceed with surgery is a collaborative one made between you and your healthcare team, based on your symptoms, diagnostic imaging, and how your condition impacts your daily life. Think of it as another tool in the toolbox, reserved for specific circumstances where it offers the best chance for long-term relief and function.
How Long to Try Conservative Treatments
Patience is key when healing a disc bulge. Most people start to feel better within a few days or weeks of consistent, conservative care. It’s important to give these treatments a fair shot. A general rule of thumb is to try non-surgical approaches for about six weeks. If you’ve been consistent with your physical therapy, chiropractic care, and lifestyle changes but your pain isn’t improving or is getting worse, it’s time to have a follow-up conversation with your doctor. This timeframe allows your body a chance to respond to treatment and gives your healthcare provider a clear picture of your progress before considering more invasive options.
Warning Signs That Point to Surgery
While most disc bulges heal without surgery, certain symptoms are red flags that may require more immediate or invasive intervention. Surgery is typically considered if conservative treatments haven't helped, especially if you experience severe or worsening symptoms. Pay close attention to progressive muscle weakness, like difficulty lifting your foot or a weakened grip. Numbness or tingling that spreads or becomes intense is another warning sign. The most critical indicators are loss of bladder or bowel control or numbness in your inner thighs and the back of your legs (saddle anesthesia). If you experience these, seek medical attention right away, as they can signal a serious condition.
A Look at Your Surgical Options
If you and your doctor decide surgery is the best course of action, it’s helpful to know what to expect. The most common procedure for a herniated disc is a microdiscectomy. During this minimally invasive surgery, a surgeon makes a small incision to remove the portion of the disc that is pressing on your nerve root. The goal is to relieve pressure and, in turn, alleviate your pain and other symptoms. This is generally reserved for cases where nerve compression is causing significant weakness, numbness, or pain that hasn't responded to other treatments. Remember, this step is only taken after a thorough evaluation and a trial of non-surgical care.
How to Prevent Future Disc Issues
After you’ve put in the work to heal a disc bulge, the last thing you want is a repeat performance. The good news is that you have a lot of control over your long-term spinal health. Preventing future issues isn’t about making drastic, unsustainable changes. Instead, it’s about layering small, consistent habits into your daily life that support and protect your spine. Think of it as building a foundation of resilience, one day at a time.
By focusing on how you move, how you work, and how you care for your body overall, you can significantly reduce your risk of re-injury. These proactive steps help maintain the integrity of your spinal discs and keep your back strong and flexible for years to come. Creating a sustainable prevention plan is one of the most empowering things you can do for your health. Working with a professional can help you build a personalized strategy, incorporating services like Physical Medicine to keep your body aligned and functioning at its best. The goal is to move from a reactive state of treating pain to a proactive state of maintaining wellness.
Daily Habits for a Healthier Spine
Your daily movements have a huge impact on your spine. One of the most effective habits you can build is strengthening your core. Your abdominal and back muscles act like a natural corset, stabilizing your spine and taking pressure off your discs. Simple exercises like planks and bridges can make a world of difference. Another critical habit is learning proper lifting techniques. Always bend at your knees and hips, not your waist. Keep your back straight, engage your core, and lift with your powerful leg muscles. Avoid twisting while lifting, as this motion puts your discs at significant risk. These small adjustments protect your back from unnecessary strain during everyday activities.
Improving Your Workplace Ergonomics
If you work at a desk, your office setup could be contributing to spinal stress. Poor posture from slouching over a computer for hours on end compresses your lumbar discs. To counter this, adjust your workspace to support a neutral spine. Your chair should allow your feet to rest flat on the floor with your knees at a 90-degree angle. Your monitor should be at eye level to prevent you from hunching forward. Consider incorporating a standing desk to vary your position throughout the day. Most importantly, take frequent breaks. Set a timer to get up, stretch, and walk around for a few minutes every hour. This simple habit can prevent stiffness and alleviate the cumulative strain of sitting.
Long-Term Strategies for Spinal Health
Two of the most important long-term strategies for a healthy spine are maintaining a healthy weight and engaging in regular exercise. Excess body weight places constant, additional pressure on your spinal discs, accelerating wear and tear. By managing your weight, you directly reduce this load. Our Functional Medicine approach can help you identify the root causes of weight gain and create a sustainable plan. Regular, low-impact exercise like swimming, walking, or cycling strengthens the muscles that support your spine and improves flexibility. It also increases blood flow to your discs, delivering the nutrients they need to stay healthy. Consistency is more important than intensity, so find an activity you enjoy and make it a regular part of your routine.
Related Articles
- Bulging Disc Therapy Treatment: A Complete Guide
- Spinal Stenosis of Lumbar Region: Symptoms & Treatment
Frequently Asked Questions
What’s the difference between a disc bulge and a herniated disc? People often use these terms interchangeably, and for good reason: the symptoms and treatments are very similar. The main technical difference is how far the disc material has moved. A disc bulge is when the disc swells and protrudes outward, but its tough outer layer remains intact. A herniated disc is when that outer layer actually tears, allowing some of the soft inner gel to leak out. Both can press on nerves and cause pain, so the focus is less on the label and more on finding a treatment plan that relieves that pressure.
How long does it usually take to recover from a disc bulge without surgery? Recovery time really varies from person to person. Many people start to feel significant relief within four to six weeks of starting a consistent, non-surgical treatment plan. However, complete healing can take several months. Your personal timeline will depend on the severity of the bulge, your overall health, and how dedicated you are to your physical therapy and lifestyle adjustments. The key is patience and consistency, not rushing the process.
Is it safe to exercise if I have a disc bulge? Yes, but it’s all about choosing the right kind of movement. Gentle, controlled exercise is one of the best things you can do to aid your recovery. It strengthens the muscles that support your spine and promotes healing blood flow. You should avoid high-impact activities like running or any movement that causes sharp, shooting pain. It's always best to work with a professional, like a physical therapist or chiropractor, who can give you a set of exercises tailored specifically to your condition.
Can a disc bulge just heal on its own? While the acute pain from a disc bulge might subside over time, the underlying mechanical issue that caused it usually won't fix itself. Your body might reduce the inflammation, but without addressing things like core weakness, poor posture, or improper movement patterns, the problem is very likely to come back. Seeking professional care helps you not only manage the immediate pain but also correct the root cause to prevent it from happening again.
I sit at a desk all day. What's the single most important change I can make? If you can only change one thing, focus on incorporating frequent movement into your day. Even with the most ergonomic chair, sitting for hours on end puts constant pressure on your lower back. Set a timer to get up and walk around for a couple of minutes at least once every hour. A quick stretch or a short walk to the kitchen can break the cycle of static posture and give your spinal discs a much-needed break from the compressive load.