The conversation around stem cell arthritis therapy is full of hope. But what’s the other side of the story? For every success you hear about, there are critical questions about safety, effectiveness, and cost that need answers. Because these treatments are still experimental, insurance almost never covers them. This leaves you to foot a bill that can run into thousands of dollars—with no guarantee of results. Before you invest your money and hope, it’s essential to weigh the unproven promises against the very real risks and scientific uncertainties.
Key Takeaways
- Recognize That It's Still Experimental: Stem cell therapy for arthritis lacks the large-scale studies, long-term safety data, and standardized protocols to be considered a proven treatment. The science has not yet caught up to the marketing hype.
- Weigh the Significant Risks and Costs: Since these treatments are not FDA-approved for arthritis, you face potential health risks from unregulated clinics and are responsible for the full, often expensive, cost with no guarantee of a successful outcome.
- Prioritize Proven, Holistic Strategies First: A smarter approach is to start with evidence-based care that addresses the root cause of your pain. A combination of physical medicine, functional medicine, and safer regenerative options like PRP offers a reliable path to relief without the uncertainty.
Understanding Osteoarthritis: A Widespread Challenge
If you're dealing with the daily grind of joint pain, it can feel incredibly isolating. But the reality is, you're in very large company. Osteoarthritis isn't just a minor ache of getting older; it's a significant health challenge that affects millions of people and fundamentally changes how they live their lives. Understanding why this condition is so common and so persistent is the first step toward finding real, sustainable relief. It’s not just about masking the pain—it’s about getting to the root of what’s happening inside your joints and creating a strategy that supports your body's ability to heal.
The Scope of the Problem: Arthritis by the Numbers
The numbers surrounding osteoarthritis (OA) really paint a picture of how widespread this is. Globally, OA affects a staggering 250 million people. Here in the U.S., projections show that 67 million Americans will be living with some form of arthritis by 2030. It’s particularly common as we age, with studies showing that about 10% of men and 13% of women over 60 are dealing with OA in their knees alone. This highlights the growing need for effective treatment strategies that go beyond temporary fixes and address the underlying issues causing the pain and degeneration. If your joints are aching, you are far from alone in this journey.
Why Arthritis Is So Difficult to Treat
One of the biggest frustrations with arthritis is that it feels like a one-way street. Biologically, the smooth, slippery tissue that cushions your joints, called articular cartilage, has very poor blood supply and can't repair itself effectively once damaged. This is why most conventional treatments only manage symptoms with pain relievers, rather than addressing the core problem. Inside an arthritic joint, the environment is hostile—acidic, low in oxygen, and flooded with inflammatory chemicals. When your body tries to patch things up, it creates a weaker scar tissue, not the strong, flexible cartilage you need. This is why a holistic approach is so critical for managing joint pain and supporting real healing.
Can Stem Cell Therapy Really Help Arthritis?
If you’re dealing with arthritis pain, you’ve likely heard the buzz around stem cell therapy. It’s often presented as a revolutionary treatment that could potentially repair joint damage, not just mask the symptoms. The core idea is compelling: using the body’s own master cells to heal from within. While traditional arthritis treatments—like steroid injections, pain medication, or even eventual joint replacement surgery—focus on managing pain and inflammation, stem cell therapy aims to address the root of the problem by regenerating damaged tissue.
The hope is that by introducing these powerful cells into an arthritic joint, they can transform into new cartilage cells, reduce inflammation, and fundamentally change the joint's environment for the better. This potential to go beyond symptom management is what makes the therapy so appealing. It suggests a future where you could not only feel better but actually have a healthier, more functional joint. It’s a shift from simply coping with the condition to actively trying to reverse the damage. But before getting caught up in the excitement, it’s important to understand what stem cells are and the theory behind how they are supposed to work for joint pain.
What Kinds of Stem Cells Are Used in Treatment?
Not all stem cells are created equal, and where they come from matters. You may have heard of Embryonic Stem Cells (ESCs), which can become any cell in the body but are surrounded by ethical debates. There are also Induced Pluripotent Stem Cells (iPSCs), which are adult cells reprogrammed in a lab to act like embryonic ones, though they carry some safety concerns. For arthritis, however, the focus is almost always on adult stem cells—specifically Mesenchymal Stem Cells (MSCs). These are the most studied for osteoarthritis because they have the unique ability to develop into bone, cartilage, and fat cells. MSCs are typically sourced from a patient’s own bone marrow, fat tissue, or from donated umbilical cord tissue.
Mesenchymal Stem Cells (MSCs)
Mesenchymal Stem Cells, or MSCs, are the specific type of adult stem cells getting all the attention for osteoarthritis. Think of them as your body's internal repair crew. They are particularly promising because they have the ability to transform into new cartilage cells, which is exactly what’s needed in a worn-down joint. But their job doesn't stop there. Research shows that MSCs also release powerful anti-inflammatory signals that can calm the chronic inflammation driving arthritis pain. They essentially act as conductors for healing, sending out chemical messages that protect existing cells and encourage the surrounding tissue to begin the repair process. This multi-faceted approach—rebuilding, reducing inflammation, and directing healing—is why MSCs are at the center of the conversation for regenerative arthritis treatment.
Donor Cells vs. Your Own Cells
When considering MSC therapy, a big question is where the cells come from: your own body (autologous) or a donor (allogeneic). Using your own cells, typically taken from your fat tissue or bone marrow, seems like the most natural choice and eliminates any risk of rejection. However, there’s a potential downside. The effectiveness of your stem cells can decline with age and the progression of chronic disease. If your osteoarthritis is advanced, your own MSCs might not be as robust or effective as they once were. This is where donor cells, usually sourced from umbilical cord tissue of healthy, screened newborns, come into play. These cells are young and vibrant, and some research suggests they may have a stronger healing capacity. The choice isn't simple, and it highlights the need for a personalized approach to determine what makes the most sense for your specific health situation.
How Is It Supposed to Work?
So, what’s the theory behind injecting these cells into a painful knee or hip? The main idea is that stem cells have two unique abilities: they can self-renew, and they can differentiate, or transform, into specialized cells. The hope is that MSCs can regenerate damaged cartilage and reduce the inflammation that drives arthritis pain. While current treatments for osteoarthritis mostly help you manage symptoms, they don’t repair the underlying damage. Researchers are exploring stem cell therapy as a way to actually rebuild the joint. Beyond creating new cartilage, some studies suggest MSCs also release proteins that calm inflammation and signal your body’s own repair mechanisms to get to work.
The Reality Check: Why Stem Cell Therapy Isn't a Guaranteed Fix
When you're dealing with chronic arthritis pain, the promise of a treatment that could regenerate your joints sounds incredible. Stem cell therapy is often marketed as that revolutionary fix, but it’s important to step back from the hype and look at what the science actually says. While the concept is exciting, the reality is that stem cell therapy for arthritis is still highly experimental and comes with significant uncertainties.
The biggest issues are a lack of solid proof that it works, a shortage of long-term safety data, and a complete absence of standardized treatment protocols. This means that what you get at one clinic can be vastly different from another, with no guarantee of quality or effectiveness. Before you invest your time, hope, and money into this treatment, you need to understand the real-world limitations and why it’s far from a sure thing. It's crucial to weigh the potential downsides against the marketing claims.
Does It Actually Work? The Problem with the Proof
The most straightforward question is also the hardest to answer: does stem cell therapy for arthritis actually work? Right now, there is simply not enough strong proof to say that it does. While some small studies and patient testimonials report pain relief, this isn't the same as rigorous scientific evidence. The improvements could be due to a placebo effect or the body's natural anti-inflammatory response to an injection.
Many medical experts argue that these treatments are not only unproven but also expensive and potentially dangerous. Without clear evidence showing that the benefits outweigh the risks, you’re essentially paying for an experiment with your own body and health on the line.
Findings from Major Clinical Research
When you look past the marketing and into the actual clinical research, the case for stem cell therapy weakens considerably. The science, as one medical expert puts it, has not yet caught up to the hype. For instance, a significant study directly compared stem cell injections to standard steroid shots for arthritis. After a full year, the results showed that stem cells did not reduce pain or improve joint function any better than the conventional steroid treatment. This is a critical finding, especially when you consider the cost. The Arthritis Foundation also warns that because these treatments are not FDA-approved for arthritis, you are responsible for the full, often expensive, cost and face potential health risks from unregulated clinics—all with no guarantee of a successful outcome.
What Happens Years Later? The Lack of Long-Term Data
Even if a treatment provides short-term relief, you need to know if it will last and if it's safe down the road. This is another area where stem cell therapy for arthritis falls short. Most of the existing research involves small groups of people over short periods. These types of studies make it difficult to draw firm conclusions about long-term effectiveness or potential side effects that might appear years later.
Because the field is so new, we just don't have the data to know what happens five or ten years after the procedure. This lack of long-term research means that fundamental questions about the treatment's durability and safety remain unanswered, leaving patients to take a significant leap of faith.
No Two Clinics Are the Same (And That's a Problem)
If you were to get a knee replacement, the surgical procedure would be highly standardized no matter which hospital you went to. The same cannot be said for stem cell therapy. There is no universally accepted method for how to prepare, dose, or inject the cells. One clinic might use stem cells from your fat tissue, while another uses bone marrow, and the techniques for processing them can vary wildly.
This lack of standardization creates a "wild west" environment where quality and safety are not guaranteed. Because many clinics operate without strict oversight, you have no way of knowing if you're receiving a high-quality, safe treatment or something that offers little benefit and potential risk. This inconsistency is one of the biggest disadvantages of stem cell therapy today.
What Major Medical Organizations Say
It’s one thing to hear claims from individual clinics, but it’s another to see what large, respected medical organizations have to say. When you’re trying to make a smart decision about your health, looking to these established groups for guidance is a critical step. Their positions are based on a comprehensive review of the available scientific evidence, not just a handful of patient testimonials or slick marketing materials. Both the experts who perform joint surgeries and the patient advocacy groups dedicated to arthritis have weighed in on stem cell therapy. Their consensus sends a clear and consistent message of caution that you should definitely hear before making any decisions about your care.
The Stance of Orthopedic Surgeons
When it comes to joint health, orthopedic surgeons are the experts. Major groups like the American Academy of Orthopaedic Surgeons (AAOS) do not recommend stem cell injections as a routine treatment for arthritis. Their reasoning is straightforward: the scientific evidence just isn't strong enough to support it. They emphasize that while research is ongoing, the current data doesn't prove that these treatments are effective or safe for widespread use. The FDA backs this up, having issued warnings to clinics promoting unapproved stem cell "cures" and has not approved any stem cell products specifically for arthritis.
The Arthritis Foundation's Position
The Arthritis Foundation, a leading voice for patients, also advises caution. While they are hopeful about the potential of regenerative medicine, they stress that stem cell therapies for arthritis are still considered experimental. They have developed specific guidance for patients, urging them to be wary of clinics making bold claims that aren't backed by solid research. Their main message is for you to become your own best advocate by educating yourself on the facts, asking tough questions, and understanding that these treatments have not yet passed the rigorous testing required for FDA approval. They encourage a healthy dose of skepticism to protect both your health and your wallet.
What Are the Real Risks and Side Effects?
Beyond the questions of effectiveness, it’s crucial to talk about safety. Any medical procedure comes with potential risks, and stem cell therapy is no exception. Because many of these treatments are still experimental and often performed in unregulated settings, the risks can be even greater. Understanding the potential side effects is a non-negotiable step in making an informed decision about your health.
The concerns aren't just theoretical. They involve real-world complications that can arise from the procedure itself, the way the cells are handled, and how your body responds to them. From immediate issues like infection at the injection site to more complex, long-term problems, these are factors that every patient should seriously consider. It's easy to get caught up in the promise of a cure, but a responsible approach means looking at the full picture. Before you move forward with any treatment, you need a clear understanding of what could go wrong so you can weigh the potential benefits against the genuine risks involved. This isn't about creating fear; it's about empowering you with knowledge.
Infection and Bleeding at the Injection Site
Any time you have an injection, there's a chance of infection or bleeding. This is a basic risk of any procedure that breaks the skin. However, the risk can be much higher with stem cell injections if the clinic doesn't follow strict sterile protocols. There have been serious cases where patients were hospitalized with infections after receiving stem cell treatments. This highlights the importance of choosing a reputable medical facility that prioritizes patient safety and adheres to the highest standards of care. A clean environment and proper technique are fundamental to minimizing this immediate and potentially dangerous side effect.
Will Your Body Reject the Cells?
Your immune system is designed to protect you from foreign invaders. If the stem cells used in your treatment come from a donor (allogeneic cells), your body might see them as a threat and launch an attack. This is known as immune rejection, and it can cause inflammation and lead to the treatment failing. While this specific risk is largely avoided when a patient's own stem cells are used (autologous cells), it's a critical question to ask your provider. You need to know exactly where the cells are coming from and what steps are being taken to ensure your body will accept them without a negative reaction.
The Risk of Uncontrolled Cell Growth or Tumors
One of the most serious long-term concerns with stem cell therapy is the potential for the cells to grow uncontrollably. Stem cells are powerful because of their ability to multiply and transform into different types of tissue. However, if this process isn't perfectly controlled, there's a small but real risk that the cells could form the wrong kind of tissue or even develop into tumors. This is a primary reason why researchers are so cautious and why regulatory oversight is so important. The long-term behavior of these cells in the body is still not fully understood, making this a significant factor to consider before undergoing an experimental treatment.
Why Isn't the Science Clearer?
If you've looked into stem cell therapy, you've probably found a mix of amazing success stories and confusing scientific claims. It can be frustrating trying to figure out what's real. The truth is, the science behind stem cells for arthritis is still a work in progress. While the potential is exciting, the research community hasn't reached a clear consensus, and there are a few key reasons why the evidence isn't as solid as we'd like it to be. Understanding these challenges is the first step to making a truly informed decision about your health.
Why Small Studies Don't Tell the Whole Story
One of the biggest hurdles in stem cell research is the size and quality of the studies. Many of the studies you might see cited are quite small, sometimes involving only a handful of patients. When a study group is too small, it's difficult for researchers to draw strong conclusions that apply to the general population. A positive result in ten people doesn't guarantee the same outcome for thousands. This is a common issue in emerging fields of medicine, but it means we have to be cautious about accepting the findings as definitive proof. It’s a starting point for more research, not the final word on an effective treatment.
How Flawed Studies Can Mislead Patients
Beyond size, the design of a study is critical. The gold standard in medical research is the placebo-controlled trial, where one group gets the real treatment and another gets a fake one, like a saltwater injection. This helps determine if the treatment itself is causing the improvement. Unfortunately, some stem cell studies lack this rigorous design. In fact, a few studies found that stem cell injections for knee osteoarthritis were no more effective than a placebo. This doesn't mean all stem cell therapy is ineffective, but it highlights how poorly designed research can produce misleading or overly optimistic results.
Is It Real Science or Just Good Marketing?
The excitement around stem cells has often outpaced the scientific evidence. A major claim you'll hear is that stem cells can rebuild or regrow cartilage in arthritic joints. While this is the ultimate hope, the current evidence doesn't fully support it. What seems more likely is that stem cells may help reduce inflammation and provide temporary pain relief for some people. This is still a valuable outcome, but it's very different from a permanent cure that rebuilds the joint. It's important to separate the marketing promises from what the science can actually back up right now.
The Financial Reality of Stem Cell Therapy
Beyond the physical risks and scientific uncertainty, there's a significant financial side to consider with experimental stem cell treatments. Because these procedures are not yet proven to be effective for arthritis, they come with a hefty price tag and are rarely covered by insurance. This leaves you footing the entire bill for a treatment that offers no guarantees.
When you’re in pain, it’s easy to be drawn in by promises of a quick fix. But it’s so important to look at the full picture—not just the potential benefits, but the very real costs and dangers, especially when dealing with unregulated clinics. Your health and your finances are too important to risk on a gamble. At Ascend, we believe in transparent, evidence-based care that prioritizes your long-term well-being over unproven, expensive procedures. Our goal is to provide you with safe and effective health solutions that address the root cause of your pain.
Will Insurance Cover It? (Probably Not)
One of the first things you'll discover is that stem cell therapy for arthritis is almost never covered by insurance plans. Because it's considered experimental, the cost falls directly on you. We're talking about thousands of dollars for a single course of treatment, with no assurance that it will work. This financial burden is a major factor to weigh, especially when there are other proven, more affordable therapies available. You're essentially paying a premium for a procedure that researchers are still trying to understand, and that financial risk is entirely your own.
Why Unregulated Clinics Are a Major Red Flag
The lack of regulation in the stem cell industry has unfortunately opened the door for questionable clinics to make bold, unsupported claims. Because there's no standard protocol, the quality, safety, and effectiveness of treatments can vary dramatically from one place to another. Some clinics may use unsafe practices, leading to serious infections or other adverse reactions. It's crucial to choose a provider who prioritizes your safety and uses established, research-backed methods. Our approach to Regenerative Medicine is grounded in proven techniques that work with your body’s natural healing processes in a safe, controlled environment.
The Ethical Questions You Should Ask
When you're exploring a treatment that’s still in the early stages of research, it’s so important to be your own best advocate. Asking direct questions isn't just your right; it's a crucial part of making a safe and informed decision for your health. The world of regenerative medicine is exciting, but it also has gray areas. A trustworthy provider will welcome your questions and give you straightforward answers. Before you move forward with any stem cell therapy, take a moment to consider a few key ethical points. This isn't about being cynical—it's about being smart and protecting yourself from clinics that might prioritize profit over your well-being. Your health is your most valuable asset, and you deserve complete transparency from anyone you entrust with your care.
Where Do the Stem Cells Come From?
This is one of the most important questions you can ask. The source of stem cells carries significant ethical weight, particularly when they come from embryonic sources. Many people have moral or personal objections to the use of embryonic stem cells, and it's a topic that has sparked a lot of debate. Beyond the ethics, the source also matters for your safety. Treatments using adult stem cells, often taken from your own body (like from fat tissue or bone marrow), sidestep these ethical issues entirely. They also tend to have a lower risk of being rejected by your immune system. Make sure you get a clear answer on where the cells originate before you consent to any procedure.
Are You Getting the Full Story on This Experimental Treatment?
A reputable clinic will be upfront about the fact that stem cell therapy for arthritis is still considered experimental. They should be willing to have an open conversation about the potential downsides and what is still unknown. Be wary of any provider who presents the treatment as a guaranteed cure. One of the most critical distinctions to understand is whether the treatment uses your own cells or cells from a donor. Using a patient's own adult stem cells can help avoid serious risks like immune rejection or other complications. You deserve to have all the facts—the good and the bad—so you can weigh the potential benefits against the known risks.
How to Spot Misleading Marketing Claims
If it sounds too good to be true, it probably is. Because these treatments are often paid for out-of-pocket and can be very expensive, some clinics resort to aggressive or misleading marketing claims to attract patients. Watch out for websites that feature dramatic testimonials but offer little to no scientific evidence. Be skeptical of claims of "curing" arthritis or promises of a completely pain-free life. A responsible provider will set realistic expectations and focus on improvements in function and quality of life, not on miracle cures. Do your own research beyond the clinic's website and brochures to get a more balanced view.
How Regulation Protects You as a Patient
When it comes to your health, knowing who to trust is everything. The field of regenerative medicine is exciting, but it’s also new, and that means the rules are still catching up to the science. This gray area allows some clinics to operate without proper oversight, putting patients at risk. Understanding the regulatory landscape is the first step in protecting yourself from ineffective or even dangerous treatments. It’s about making sure any therapy you consider is backed by safety, transparency, and a commitment to your well-being.
What the FDA Says About Unproven Stem Cell Treatments
The U.S. Food and Drug Administration (FDA) plays a critical role in ensuring medical treatments are both safe and effective. When it comes to stem cells, the FDA has issued warnings to consumers about unproven therapies. Currently, the FDA has not approved any stem cell product for the treatment of arthritis. This means that any clinic offering it for joint pain is providing an experimental treatment. The FDA has strict rules about how stem cells are processed and administered, and clinics that sidestep these regulations aren't being held to the highest safety standards. This is a major red flag you shouldn’t ignore.
How to Identify a Questionable Clinic
Because the field is not uniformly regulated, the quality of care can vary dramatically from one clinic to the next. A questionable clinic often over-promises and under-delivers. Be wary of aggressive marketing that uses words like "cure" or guarantees results. Other red flags include a lack of transparency about the type of stem cells used, where they come from, or the specifics of the procedure. If a provider seems to downplay risks or pressures you into making a quick decision, it’s wise to walk away. A trustworthy clinic will welcome your questions and provide clear, honest information about the conditions they treat and the realistic outcomes you can expect.
The Dangers of "Stem Cell Tourism"
The temptation to travel to other countries for stem cell treatments—often called "medical tourism"—can be strong, especially when clinics promise miraculous results at a lower cost. However, this path is filled with risks. Many countries have far less stringent regulations than the United States, meaning there’s little to no oversight of a clinic’s safety protocols, cell quality, or staff credentials. Patients can be misled by slick marketing and left with no legal recourse if something goes wrong. Choosing a local, reputable provider for regenerative medicine ensures you are protected by domestic healthcare standards and can build a trusted relationship with your care team.
Who Is (and Isn't) a Candidate for Stem Cell Therapy?
It’s clear that stem cell therapy isn’t a magic bullet for every person with joint pain. Like any medical procedure, its potential for success depends heavily on the individual. The stage of your arthritis, the specific joint affected, and your overall health all play a role in determining whether you're a good candidate. Before you even consider this path, it’s essential to have a realistic understanding of who stands to benefit the most and for whom the treatment is unlikely to deliver the promised results. This isn't about gatekeeping; it's about making sure you invest your hope and resources wisely.
Best-Case Scenarios: Localized Damage
The most promising results for stem cell therapy are seen in people with very specific types of joint issues. The ideal candidate is someone who has localized cartilage damage in a single area, rather than widespread, advanced arthritis throughout the joint. Think of it as patching a small pothole instead of repaving an entire road. For individuals with damage from a specific injury, the natural aging process, or being overweight, the therapy may help lower inflammation and pain in the knee. In these situations, the goal isn't a complete reversal of arthritis but rather a targeted intervention that could potentially delay the need for more invasive procedures like a total knee replacement.
When It's Not Recommended: Severe Arthritis
On the other end of the spectrum, stem cell therapy is generally not recommended for individuals with severe, "bone-on-bone" arthritis. When the cartilage has worn away completely, the joint's environment is too damaged for these cells to make a meaningful difference. The therapy doesn't reliably rebuild large amounts of lost cartilage or stop the progression of severe arthritis. While it might offer some temporary pain relief by reducing inflammation, it can't fix the underlying structural problem. For those with advanced-stage arthritis, more definitive treatments like joint replacement surgery remain the most effective and predictable option for restoring function and providing long-term relief. It's crucial to match the treatment to the severity of the condition.
Safer, Proven Alternatives for Arthritis Relief
While the buzz around stem cell therapy is hard to ignore, it’s crucial to remember that it’s not the only path forward—and for many, it’s not the safest or most effective. The good news is that there are powerful, evidence-based strategies that can provide significant relief from arthritis pain and improve your quality of life. These approaches focus on addressing the root cause of your symptoms and supporting your body’s incredible ability to heal itself.
Instead of jumping to an expensive and unproven procedure, consider building a solid foundation with treatments that are backed by science and tailored to your unique body. A comprehensive plan often involves a combination of therapies that work together to reduce inflammation, restore function, and manage pain. This holistic strategy not only addresses your immediate discomfort but also sets you up for better long-term health, giving you a sustainable way to get back to the activities you love.
Proven First-Line Treatments to Consider
Before you explore expensive and experimental options, it’s essential to focus on the foundational strategies that are proven to make a real difference. A smarter approach is to start with evidence-based care that addresses the root cause of your pain. A combination of physical medicine, functional medicine, and safer regenerative options offers a reliable path to relief without the uncertainty that comes with unproven therapies. These first-line treatments are not just about managing symptoms; they are about creating a healthier environment for your joints and empowering your body to function at its best. By building this strong foundation, you give yourself the best possible chance for long-term success.
The Role of Weight Management and Physical Therapy
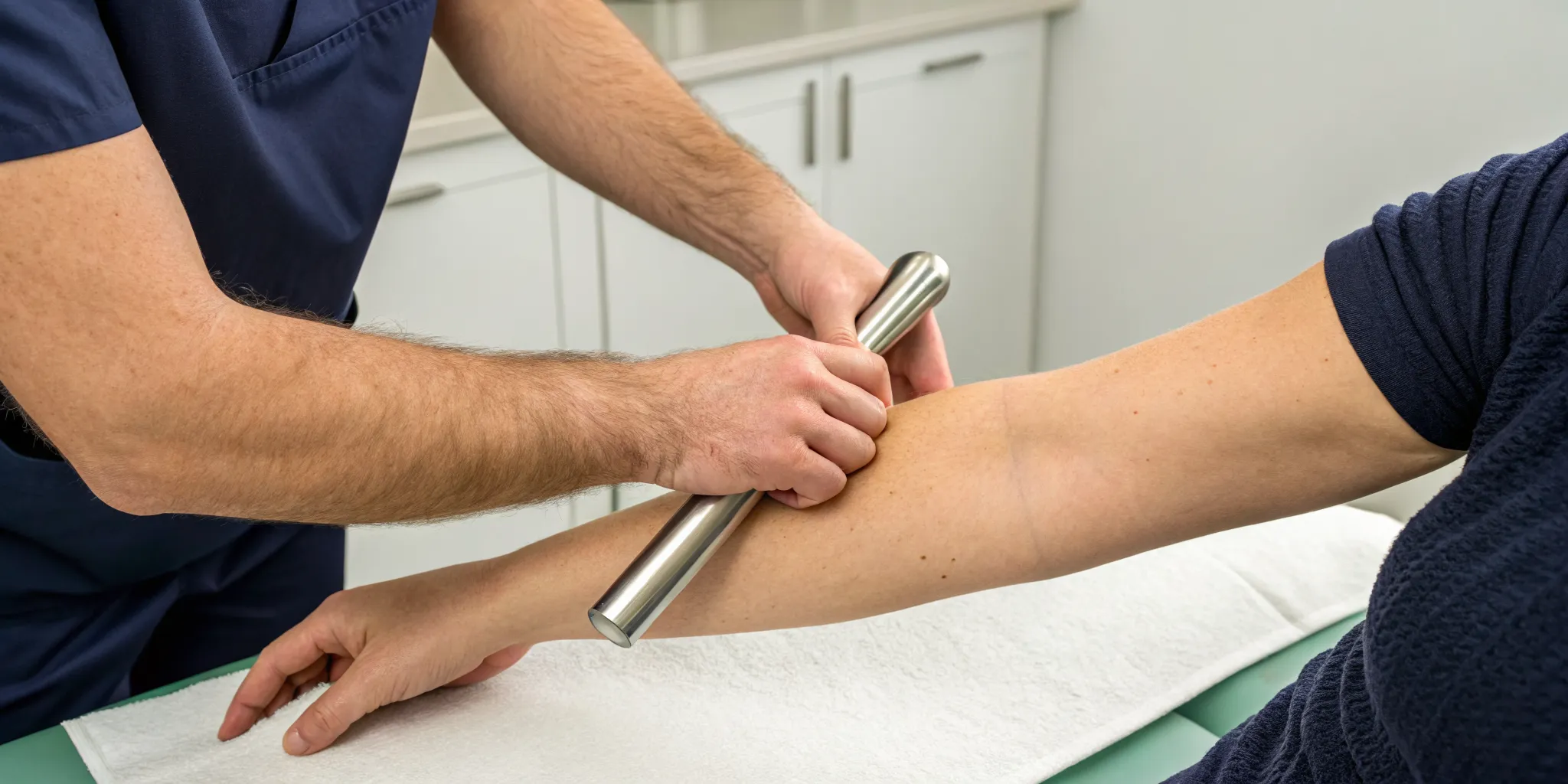
Two of the most powerful tools you have for managing arthritis are completely within your control: managing your weight and committing to physical therapy. Every extra pound you carry puts several extra pounds of pressure on your weight-bearing joints, like your knees and hips. Losing even a small amount of weight can dramatically reduce this strain, leading to less pain and improved function. Paired with weight management, physical therapy is crucial for building strength in the muscles that support your joints. A skilled therapist can design a program that improves your range of motion, enhances stability, and corrects movement patterns that may be contributing to your pain, forming the core of a solid Physical Medicine plan.
Pain Medication and Supplements
While the goal is to address the root cause of arthritis, managing pain and inflammation is a key part of the process. Over-the-counter pain relievers can provide temporary relief, allowing you to stay active and participate in physical therapy. Beyond that, a functional medicine approach can help identify supplements that target inflammation from the inside out. Nutrients like turmeric, omega-3 fatty acids, and glucosamine have been studied for their anti-inflammatory properties and ability to support joint health. Rather than paying for an experiment with your own body, you can explore these options with a provider who understands how to use targeted supplementation to support your body’s natural healing processes safely and effectively.
A Hands-On Approach: Physical and Chiropractic Medicine
Before considering experimental treatments, it’s essential to start with the fundamentals. Proven strategies like targeted exercise, weight management, and physical therapy are cornerstones of effective arthritis care. This is where a hands-on, holistic approach comes in. Our philosophy around physical medicine focuses on improving your body’s mechanics to reduce pain and restore mobility.
Through chiropractic adjustments, we can improve joint alignment and function, taking pressure off irritated nerves. Paired with personalized physical therapy, we can strengthen the muscles that support your joints, creating more stability and reducing daily strain. This integrated approach doesn’t just mask the pain; it addresses the structural issues contributing to it, helping you move more freely and with greater confidence.
Functional Medicine: Getting to the Root of Your Pain
Physical treatments are fantastic for addressing the structural side of arthritis, but what’s happening on the inside? Chronic inflammation is often a key driver of joint pain, and it can be influenced by factors like your diet, gut health, and even hidden infections. Understanding the underlying causes of your arthritis is the key to developing a truly effective and lasting treatment strategy.
This is the core of functional medicine. We look at your health from a whole-body perspective to identify and address the specific triggers that are fueling your inflammation. Through advanced testing and a deep dive into your health history, we can create a personalized plan that may include dietary changes, targeted supplements, and lifestyle adjustments to calm your system from the inside out.
Our Approach to Safe, Effective Regenerative Medicine
The idea of using your body’s own healing potential is powerful, but it’s critical to choose therapies that are both safe and proven. While many stem cell clinics make big promises, their treatments are often unproven and can carry serious risks, including infection. At Ascend, we offer regenerative medicine options that are backed by research and have a strong safety record.
Therapies like Platelet-Rich Plasma (PRP) use a concentration of your own blood platelets to stimulate healing in damaged tissues and reduce inflammation directly at the source. Prolotherapy is another option that involves injecting a natural solution to trigger the body’s repair mechanisms in weakened ligaments and tendons. These treatments work with your body’s natural processes to promote long-term healing without the uncertainties of experimental stem cell procedures.
How to Make a Smart, Informed Decision for Your Health
Taking charge of your health means being an active participant in your care. When you're exploring treatments for something as persistent as arthritis pain, it’s easy to feel overwhelmed by the options, especially with newer therapies like stem cell injections where hype can sometimes outpace the science. The best way to feel confident in your decisions is to arm yourself with the right information and ask pointed questions. Your health is your most valuable asset, and you have every right to understand the what, why, and how of any proposed treatment.
A trustworthy provider will welcome your questions and provide clear, honest answers, seeing you as a partner in your own wellness journey. Think of it as a conversation, not an interrogation. You’re gathering the facts you need to choose the path that feels right for you, your body, and your long-term well-being. This process helps you partner with your healthcare provider to find solutions that truly address the conditions you treat and support your goals for a healthier, more active life. It's about moving beyond just managing symptoms and toward genuine healing.
Your Checklist: Questions to Ask Any Provider
Before you commit to any procedure, especially one that is considered experimental, it’s essential to have a frank discussion with the provider. Don't hesitate to bring a list of questions to your consultation. Start with these to get a clear picture of what you’re signing up for:
- What is the evidence? Ask, "Can you show me the clinical studies that support using this specific therapy for my condition?" A reputable provider should be able to point to research, not just patient testimonials.
- What are the risks? A direct question like, "What are the potential short-term and long-term side effects or complications?" is crucial. They should be transparent about everything from infection to adverse reactions.
- What is the total cost? Since insurance rarely covers these treatments, ask for a complete breakdown of the price. "What does the total cost include, and are there any follow-up expenses I should expect?"
- Is this FDA-approved? Ask, "Is this treatment approved by the FDA for arthritis?" Understanding the regulatory status helps you gauge whether the therapy is established or still experimental.
Warning Signs: When to Walk Away
While you’re looking for a provider you can trust, it’s just as important to know how to spot one you can’t. Some clinics capitalize on hope and hype, so keep an eye out for these warning signs. A major red flag is any clinic that promises a "cure" or guarantees results. Medicine is complex, and ethical providers manage expectations realistically.
Be cautious of aggressive marketing and high-pressure sales tactics. Your health decisions should never feel rushed. If a clinic’s approach feels more like a sales pitch than a medical consultation, it’s wise to step back. Similarly, if a provider can't clearly explain their protocols or seems to dismiss your questions about safety and risks, consider it a sign to walk away. A focus on Functional Medicine and finding the root cause of an issue is often a better indicator of a practice committed to your long-term health.
Frequently Asked Questions
So, does this mean stem cell therapy never works for arthritis? It’s not quite that simple. Some people do report feeling temporary pain relief after the procedure. Researchers believe this is likely due to the anti-inflammatory properties of the injected cells, rather than any actual regrowth of cartilage. The main issue is that this effect is often short-lived, and it doesn't deliver on the promise of rebuilding or curing the joint. The evidence just isn't there to support it as a long-term, restorative solution.
Why is stem cell therapy so expensive if it's not covered by insurance? The high price tag comes from a few factors. The procedure requires specialized equipment and expertise to harvest and process the cells. Since the FDA has not approved it for arthritis, insurance companies consider it an experimental treatment and won't cover the cost. This leaves the entire financial burden on the patient, who is essentially paying a premium for a procedure that is still being researched and lacks guaranteed results.
My friend had a great experience with stem cell therapy. How is that possible if the science isn't there? It's great that your friend found relief, and their experience is valid. This can happen for a couple of reasons. The body has a powerful placebo response, where believing a treatment will work can create real, though often temporary, pain relief. Also, as mentioned, the cells can have a short-term anti-inflammatory effect. The challenge is that these individual stories don't replace the need for large-scale scientific studies that prove a treatment is consistently safe, effective, and better than a placebo in the long run.
Are PRP and Prolotherapy just different types of stem cell therapy? That's a great question, but no, they are different. While all three are considered regenerative medicine, they work in distinct ways. Stem cell therapy aims to introduce new "master" cells. Platelet-Rich Plasma (PRP) therapy uses a concentration of your own blood platelets to release growth factors that signal your body to heal damaged tissue. Prolotherapy involves injecting a natural solution to intentionally create a mild, localized inflammation that triggers your body's natural healing and repair processes. Both PRP and Prolotherapy have a longer history of use and a more established safety profile for certain joint and ligament issues.
What's the biggest red flag I should watch out for if I'm looking at a clinic that offers stem cell therapy? The single biggest red flag is any provider who promises a "cure" or guarantees a specific outcome. Ethical medical professionals know that there are no guarantees in medicine, especially with experimental treatments. You should also be very cautious of high-pressure sales tactics, a lack of transparency about where the cells come from, or a provider who dismisses your questions about risks and long-term data. A trustworthy clinic will give you a balanced view of both the potential and the limitations.