Let's get one thing straight: spinal decompression shouldn't hurt. If you're asking, "why does it hurt when I decompress my spine?", you are absolutely right to be concerned. Pain during this therapy isn't something to push through; it's your body sending a clear signal that we need to investigate. This discomfort could mean the force needs adjusting, your positioning isn't quite right, or there's another issue to address first. Feeling that decompressing your spine hurts is valuable information that helps us create a plan that works with your body, not against it.
Key Takeaways
- Distinguish Between Normal Soreness and Pain: Feeling mild muscle soreness after a session is a normal sign of your body adapting, but sharp, stabbing, or radiating pain is not. True pain is a signal to stop the treatment immediately and inform your practitioner.
- You Are in Control of Your Treatment: Your feedback is essential for a safe and effective session. Communicate any discomfort to your provider right away and use the patient safety switch if you feel anything beyond a gentle stretch.
- Effective Treatment Starts with a Full Evaluation: A comprehensive initial assessment is crucial to determine if spinal decompression is right for you. If it's not a good fit, this evaluation helps identify the true root cause of your pain and points toward other effective therapies.
How Spinal Decompression Therapy Works
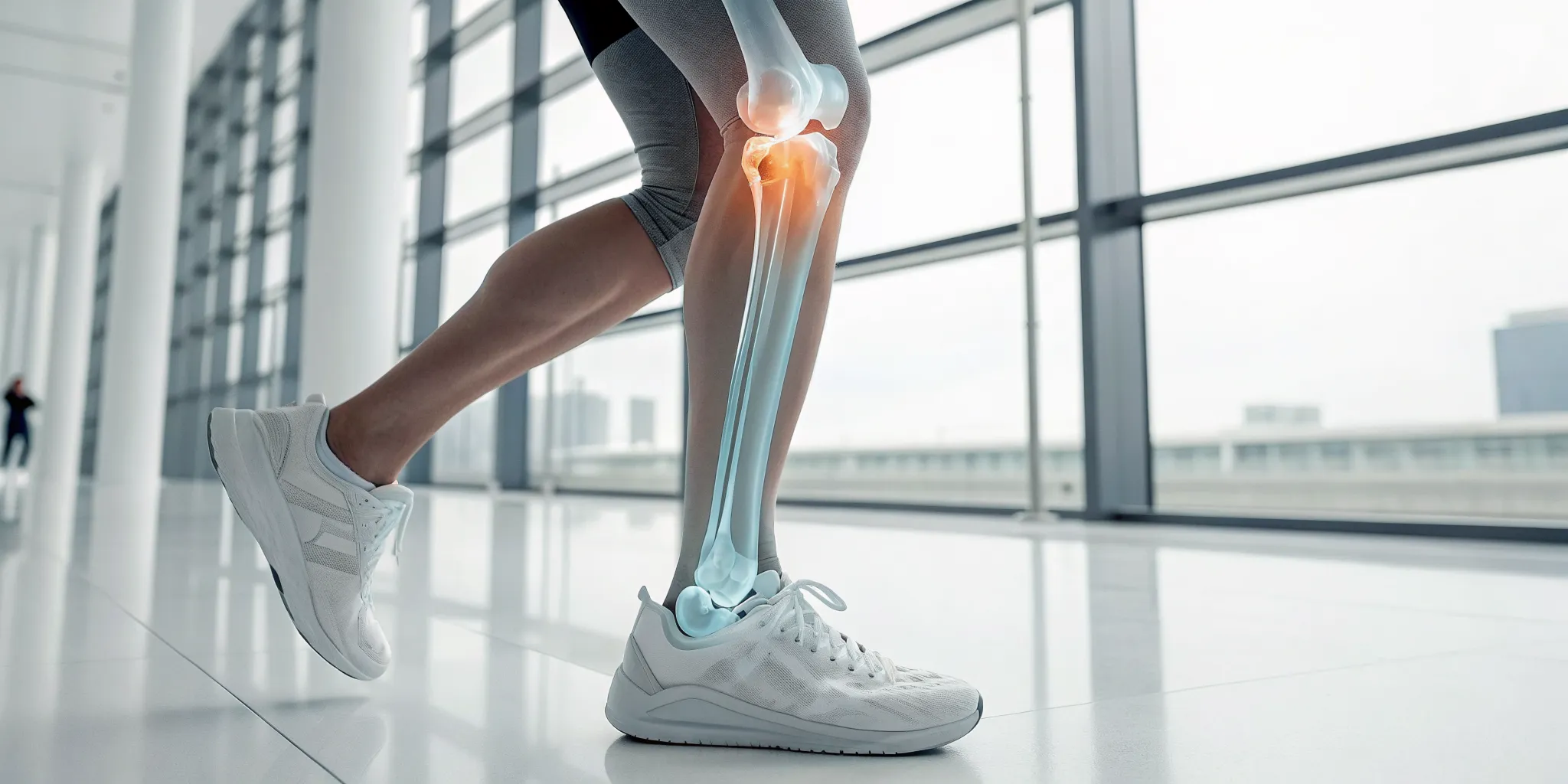
If you're dealing with persistent back, neck, or leg pain, you’ve likely heard about spinal decompression. At its core, this therapy is designed to gently stretch the spine, creating space and relieving pressure on your spinal discs and nerves. Think of it as a way to give your spine a much-needed breather from the constant compressive forces of gravity and daily life. The main goal is to address the root cause of pain from conditions like bulging, herniated, or degenerating discs, rather than just masking the symptoms.
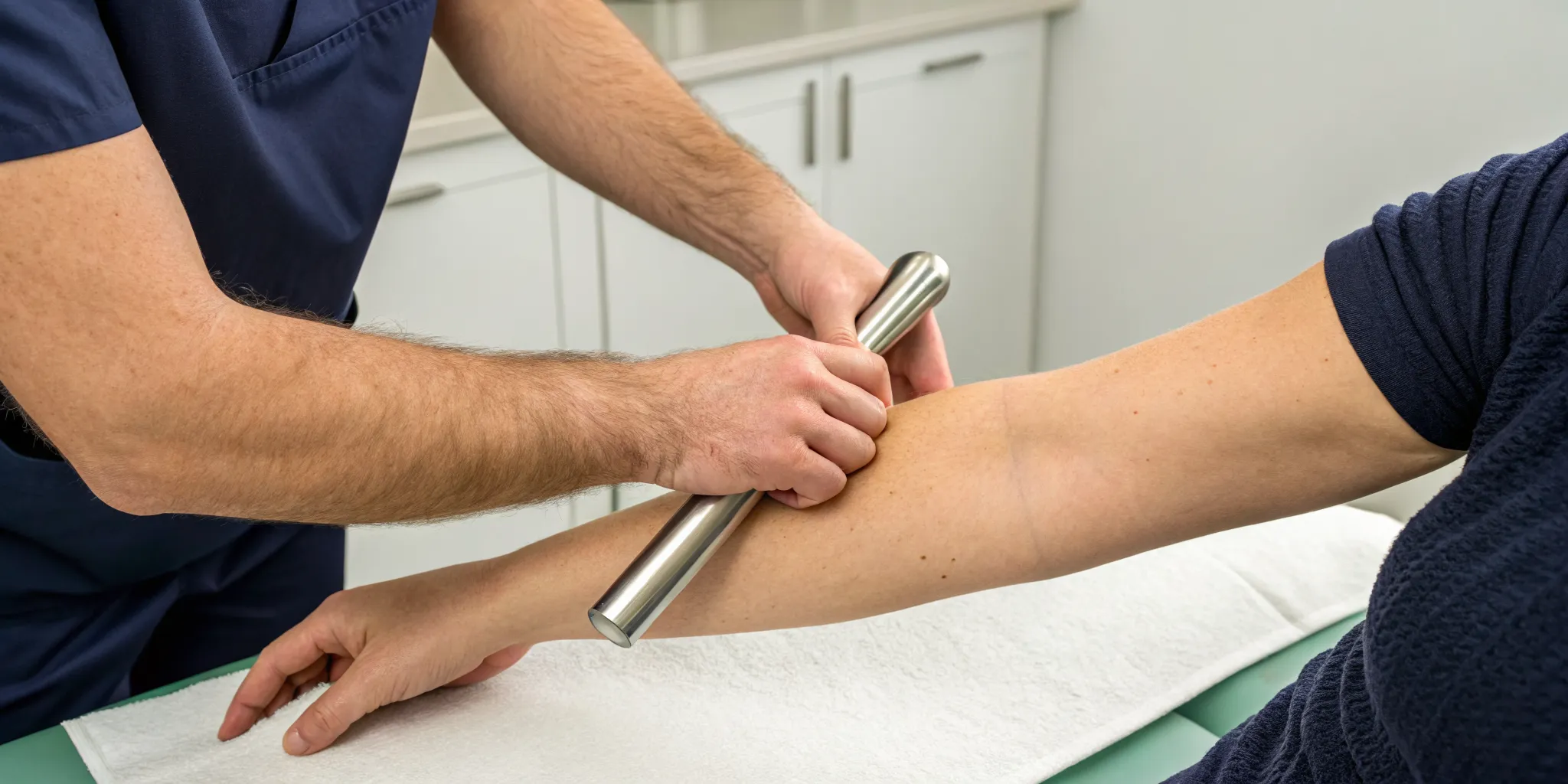
So, how does it work? The gentle stretching creates negative pressure within the discs—a bit like a vacuum effect. This is important for two reasons. First, it can help retract or pull bulging or slipped disc material back into its proper place, taking pressure off pinched nerves. Second, and just as crucial, it allows a fresh flow of oxygen, water, and nutrient-rich fluids to enter the discs. These are the building blocks your discs need to heal and rehydrate. It’s one of the key therapies we use in Physical Medicine because it supports the body's natural ability to repair itself without invasive procedures.
What Happens During a Session?
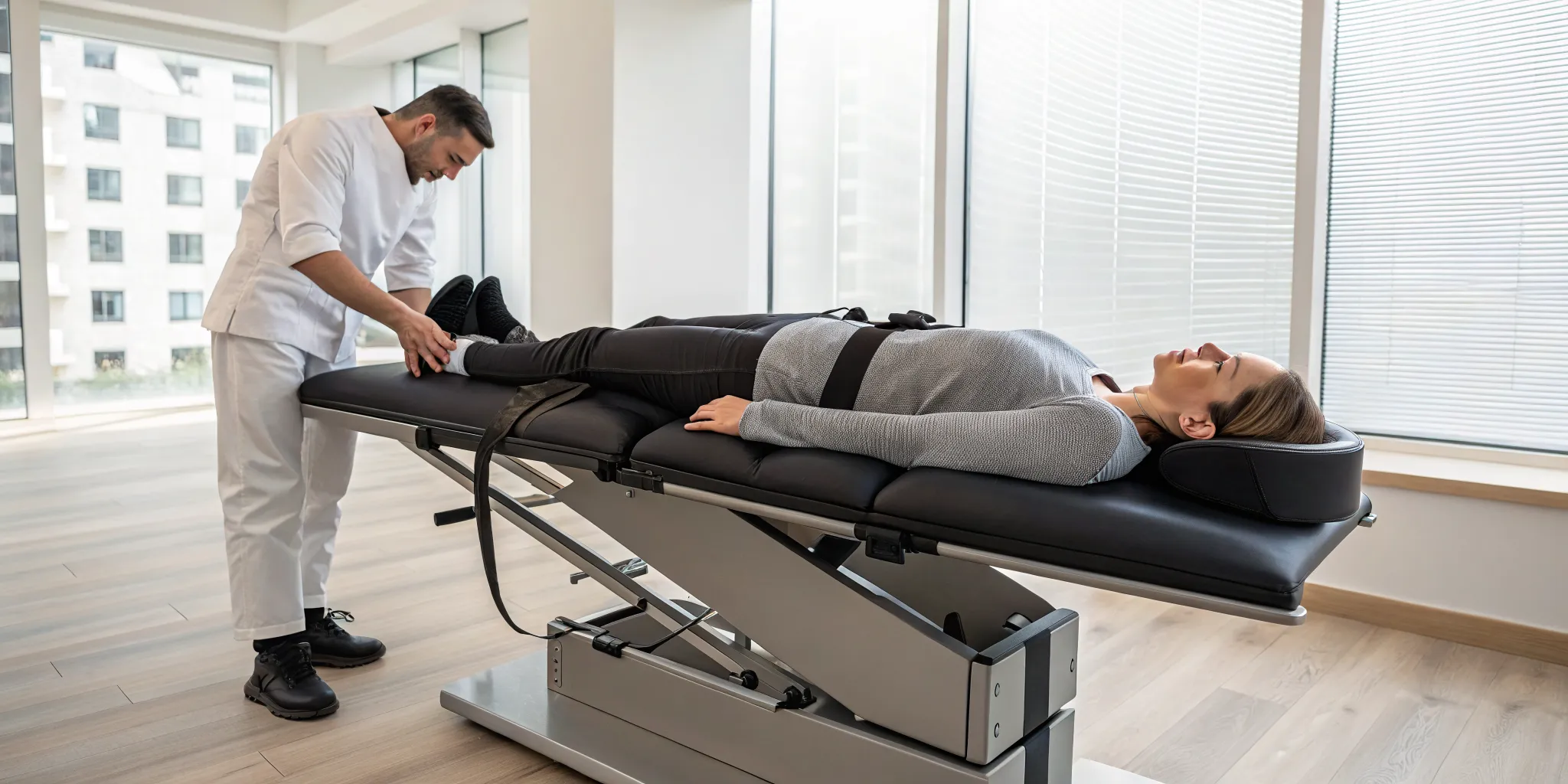
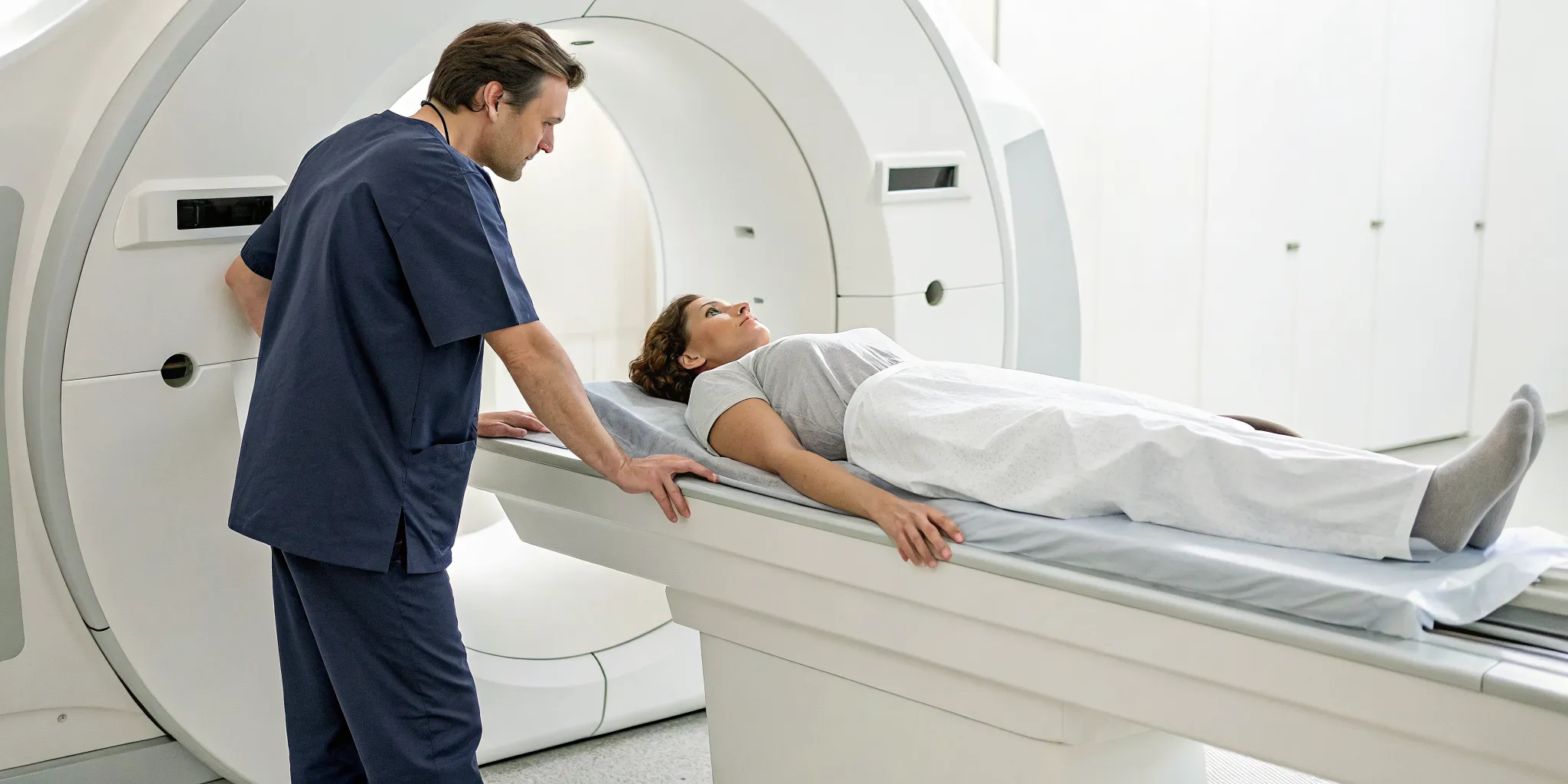
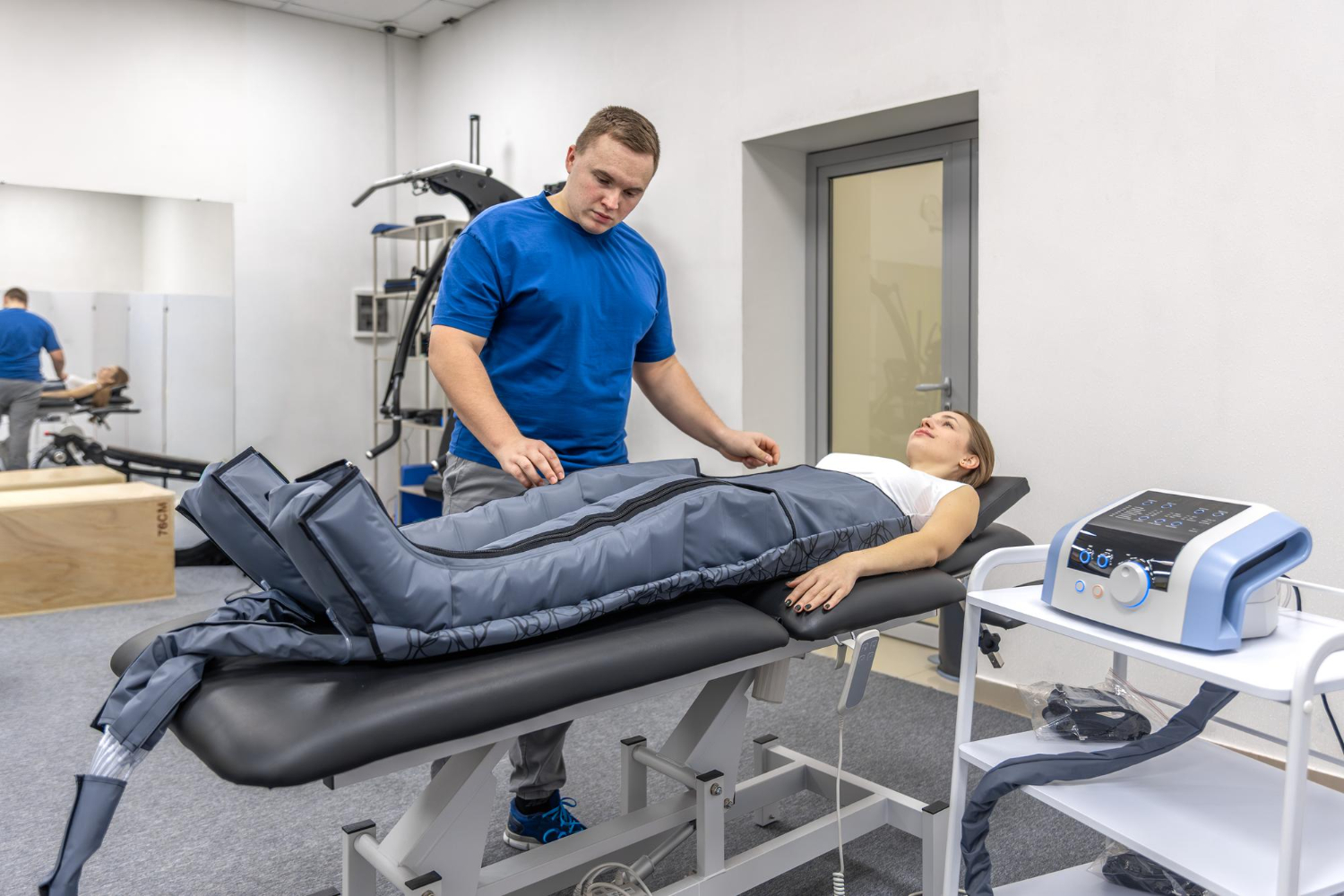
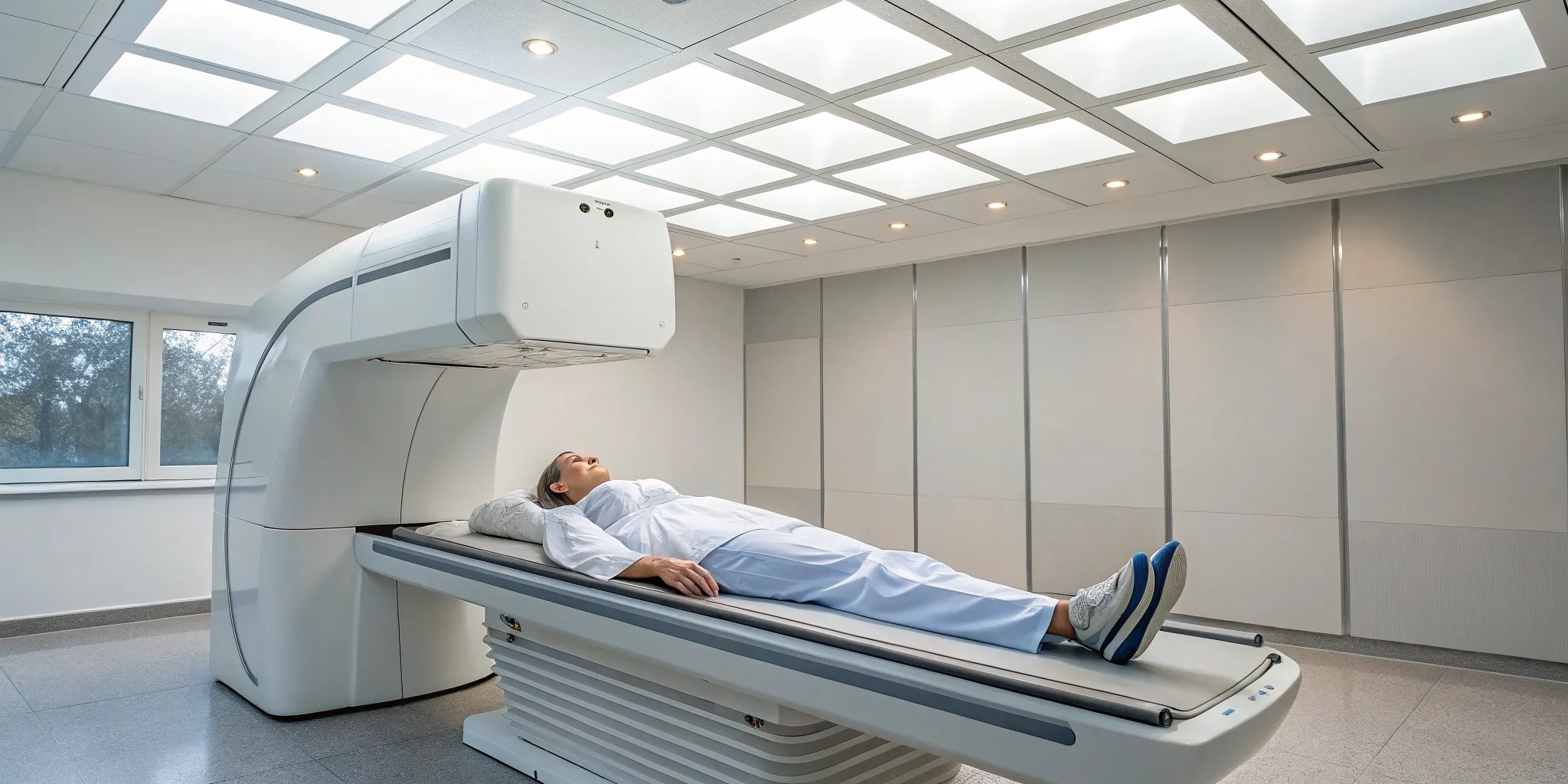
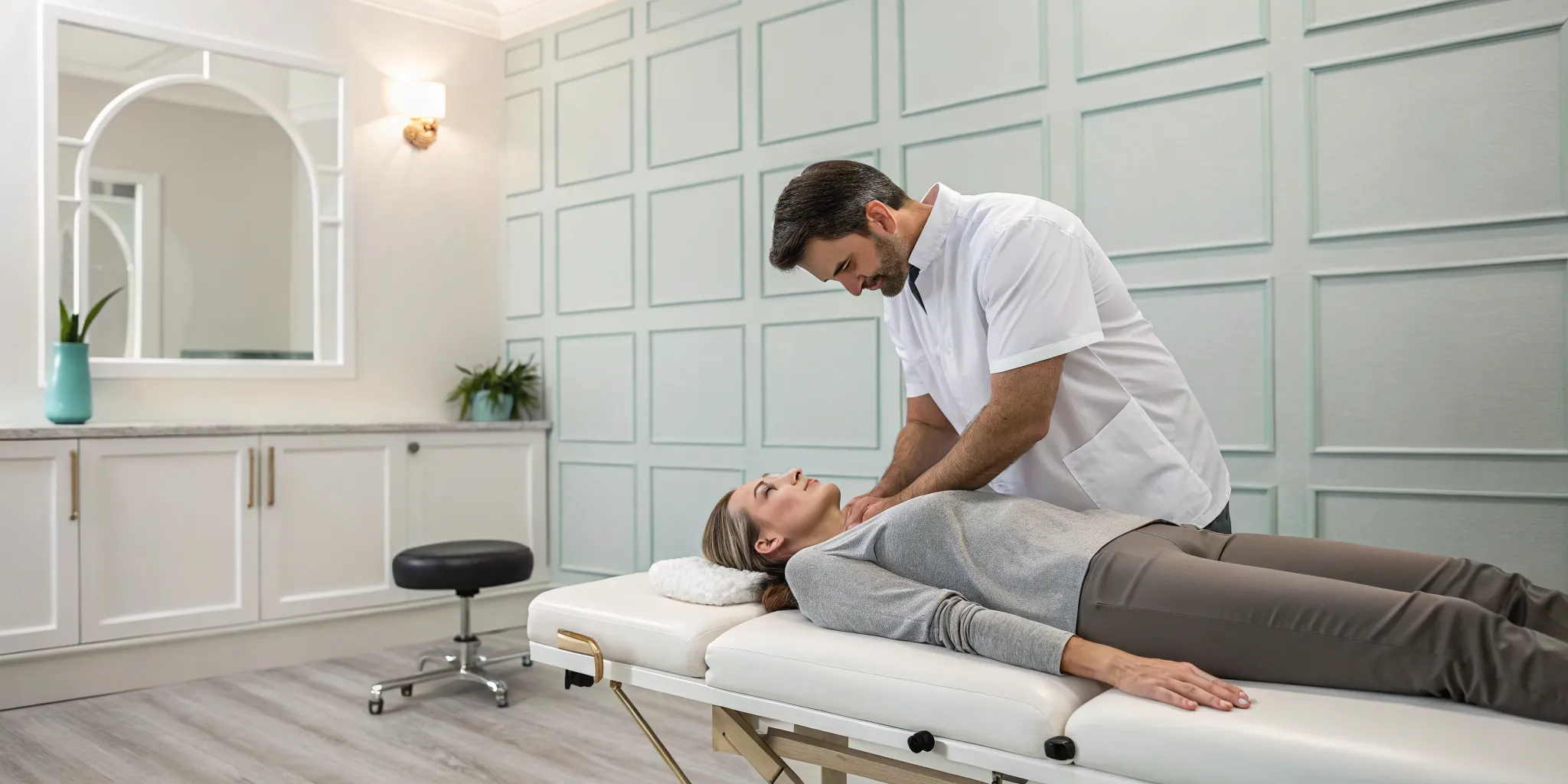
Walking into a treatment session can feel intimidating if you don’t know what to expect, but the process is quite straightforward and comfortable. You’ll lie fully clothed on a specialized, computer-controlled table. We’ll place a harness around your lower back, which connects to the table. The system then applies a gentle, precise stretching force, followed by a period of relaxation. This cycle repeats throughout the session. You shouldn't feel sharp or stabbing pain. Instead, most people describe the sensation as a mild stretch or a gentle pulling in their back. Many even find the rhythmic motion to be quite relaxing. The entire process is controlled and monitored to ensure it’s both effective and comfortable for you.
Is All Spinal Decompression the Same?
When people talk about spinal decompression, they could be referring to a couple of different things, so it’s helpful to know the distinction. The two main categories are surgical and non-surgical. Surgical decompression, like a laminectomy or discectomy, is an invasive procedure performed by a surgeon to physically remove whatever is pressing on a nerve. Non-surgical spinal decompression is the therapy we’re discussing here. It’s a conservative, non-invasive approach that is often the first line of defense for many spinal conditions we treat. This therapy can be performed using specialized traction tables, like the ones we use, or through manual techniques applied by a trained practitioner. The goal is always the same: to relieve pressure and promote natural healing.
What Should Spinal Decompression Feel Like?
One of the first questions people ask about spinal decompression is, "Will it hurt?" It's a valid concern, especially when you're already dealing with back pain. The short answer is no—the treatment itself should not be painful. The goal is to create a gentle, therapeutic stretch in your spine, not cause more discomfort.
You’ll be comfortably secured to a specialized table that moves to decompress the targeted area. While the treatment is gentle, your body is undergoing a significant change. It's normal to feel new sensations, but sharp pain is never part of the plan. Understanding the difference between normal therapeutic feelings and actual pain is key to a successful and safe treatment experience.
A Relaxing and Gentle Process
The entire process is designed to be comfortable and soothing. You’ll lie on a specialized table, fully clothed, while a harness is secured around your waist. The table is computer-controlled, which allows for incredibly precise and gentle movements. It slowly creates a stretch in your spine, holds it for a period, and then releases. This cycle repeats throughout the session. The sensation is often described as a mild, relieving pull in the lower back or neck. Many people find the rhythmic motion so calming that they can completely relax or even doze off during the treatment. This approach is a cornerstone of our Physical Medicine services because it works with your body to create an ideal environment for healing, rather than forcing a change.
How to Tell Normal Soreness from a Real Problem
It’s important to know what to feel for during your session. A gentle stretching or pulling sensation along your spine is completely normal. However, if spinal decompression hurts your lower back with a sharp or sudden pain, that’s a red flag. This isn't typical and could signal an issue, like incorrect pressure for your body or an undiagnosed condition that needs attention. While mild soreness afterward is common, sharp pain during the treatment means something is wrong. Always tell your practitioner immediately if you feel anything beyond a gentle stretch.
The Difference Between Discomfort and Pain
So, what kind of discomfort is considered normal? During the treatment, you should only feel that gentle stretching. Afterward, it’s common to experience some mild soreness or muscle stiffness, much like you would after a new workout. Your muscles and ligaments are adapting to the new space between your vertebrae, and it can take them time to adjust. This post-session soreness is usually temporary and a sign that your body is responding to the therapy. It should feel like muscle fatigue, not a sharp, specific pain.
Is "No Pain, No Gain" True for Decompression?
A persistent myth is that spinal decompression has to be painful to be effective. In reality, the opposite is true. The process is designed to be a gentle, non-painful therapy. Your comfort is the top priority, and the computerized system allows for precise, controlled adjustments to ensure the pull is just right for you. Our approach to physical medicine is always centered on your body's needs. You are always in control and can stop the session at any moment. True healing doesn't require gritting your teeth through pain.
Feeling Sore After Spinal Decompression? Here’s Why
Feeling some new sensations after spinal decompression can be confusing. You went in for relief, so experiencing any discomfort might feel like a step backward. But in many cases, what you’re feeling is a normal part of your body’s healing process. The key is to understand the difference between productive soreness and pain that signals a problem. When your spine is gently stretched and decompressed, it creates more space for your discs and nerves. This is a significant change, and your body needs time to adjust to this new, healthier alignment. Think of it as your muscles and ligaments learning a new way to hold themselves. This adaptation process can come with some temporary aches, but it's often a sign that positive changes are happening deep within your spine. It's similar to the feeling you get after a deep tissue massage or a challenging yoga class—your body has been worked in a new way, and it's responding. Understanding why this happens can help you feel more confident in your treatment and your body's ability to heal. Let’s look at a few common reasons why you might feel sore after a session and what that means for your recovery.
Your Body's Natural Healing Response
Think of spinal decompression as a specialized workout for your spine and the muscles supporting it. During a session, the gentle stretching lengthens your spine, which can relieve pressure on your discs and nerves. This process asks your muscles, ligaments, and tendons to adjust to new positions and movements. Just like you might feel sore after trying a new exercise, your back muscles can feel tired or achy as they adapt. This type of soreness is usually mild and temporary. It’s a sign that your body is responding to the therapy and beginning the process of realignment and healing, which is a core goal of physical medicine.
Muscle Spasms and Adjustments
For a long time, the muscles surrounding your spine may have been overcompensating for an underlying issue, like a compressed disc. They’ve been tight and guarded, trying to protect the sensitive area. When spinal decompression begins to create space and relieve that pressure, your muscles can get confused. This sudden change can cause them to tighten or spasm as they adjust to a new, healthier alignment. This response is often temporary and part of the body’s process of adapting to the treatment. It’s a sign that real structural changes are happening, and our approach to physical medicine is designed to guide your body through this adjustment period safely.
Nerve Sensitivity and Irritation
If you have a nerve that is already significantly inflamed or compressed, the changes in pressure during a decompression session can sometimes cause temporary irritation. The negative pressure created by the therapy is designed to be gentle, but an already sensitive nerve can react to even minor shifts in its environment. This can lead to a temporary increase in discomfort or nerve-related sensations. It’s a key reason why a thorough initial evaluation is so important. By understanding the specific conditions we treat and the state of your nerves beforehand, we can tailor the therapy to minimize irritation and support healing, rather than causing a flare-up.
Underlying Spinal Instability
Spinal decompression works best when the spine has a stable foundation. If there's an underlying instability in your spine—meaning the vertebrae move more than they should—the stretching force of decompression can sometimes be counterproductive. When the joints are separated, your body’s protective reflex can kick in, causing the surrounding muscles to tighten up forcefully in a process called muscle guarding. This is your body’s attempt to protect what it perceives as an unstable area. Pain in this scenario is a clear signal that decompression may not be the right approach, highlighting why our philosophy is to first identify and address the root cause of your pain.
Could a Pre-Existing Condition Be the Cause?
While mild soreness can be normal, sharp or intense pain is not. Spinal decompression is highly effective for issues like herniated discs and sciatica, but it isn’t the right fit for every back problem. Certain underlying conditions, such as significant spinal instability, might be aggravated by the traction forces used in decompression. This is why a comprehensive initial evaluation is so important. A thorough assessment helps your practitioner determine if spinal decompression is a safe and effective option for you or if another therapy would be more appropriate. Never hesitate to communicate exactly what you’re feeling, as sharp pain could indicate an underlying issue that needs a different approach.
Healing Isn't One-Size-Fits-All
It’s easy to compare your progress to what you think it should be, but healing is never a one-size-fits-all process. Recovery takes time, and everyone’s body responds differently. Factors like your age, the specific condition being treated, your overall health, and even your stress levels can influence how you feel after each session. The goal is steady, gradual improvement, not an overnight fix. Our approach with functional medicine recognizes that your back pain is connected to your whole-body health. Being patient with yourself and focusing on consistent progress is the most effective way to achieve lasting relief.
Is Your Pain a Red Flag?
While mild soreness is a sign that your body is adapting, certain types of pain are not part of the healing process. It’s important to listen to your body and understand the difference between normal discomfort and a red flag. True pain during or after spinal decompression is rare, but knowing what to watch for helps you stay safe and ensures your treatment is effective. Think of these signals as your body’s way of saying, “Hey, let’s pause and check in.” Communicating these feelings to your practitioner immediately is key to a safe and successful recovery.
Pay Attention to Sharp, Sudden Pain
Let’s be clear: you should not feel sharp, stabbing, or sudden pain during or after your session. While you might feel a deep stretch or a dull ache as your muscles and ligaments adjust, sharp pain is a warning sign. This type of sensation is different from the gentle pulling of the decompression table or the mild soreness that can follow. It’s more acute and localized. If you experience a sudden jolt of pain, it’s your body’s signal that something isn’t right. Don’t try to push through it. This is your cue to speak up instantly.
When to Stop Treatment Immediately
If you feel any sharp or acute pain, you need to stop the treatment right away. Every spinal decompression machine is equipped with a safety switch that you control. If you feel anything that crosses the line from discomfort to pain, use it. There’s no reason to endure pain during this therapy. After a session, you should also be on the lookout. If you experience sharp or tender pain once you’re home, contact your practitioner immediately. Your feedback is crucial for adjusting the treatment to fit your body’s specific needs and ensuring your care plan is on the right track.
Watch for Numbness, Tingling, or Radiating Pain
Pay close attention to any new nerve-related sensations. Symptoms like numbness, tingling, weakness, or a “pins and needles” feeling in your legs, feet, arms, or hands are red flags. This also includes pain that radiates down your limbs, like sciatica. Since spinal decompression is designed to relieve nerve pressure, creating new nerve-related symptoms is counterproductive and indicates a problem. Severe pain—anything you’d rate a 7 or higher out of 10—that lasts more than a day or two is also not normal. These are signs that require immediate attention from your healthcare provider, as they can point to underlying conditions we treat that need a different approach.
What to Do If You Feel Pain After Treatment
Feeling unexpected pain during or after a treatment can be unsettling, but knowing what to do puts you back in control. Your feedback is one of the most important parts of your healing process. Whether you’re on the treatment table or recovering at home, there are clear, simple steps you can take to manage discomfort and ensure your treatment plan stays on track. Think of it as a partnership: your practitioner guides the therapy, and you provide the real-time information they need to make it work for you. Open communication is the key to making sure your spinal decompression therapy is both safe and effective.
Speak Up: What to Do Mid-Treatment
If you feel sharp, stabbing, or radiating pain at any point during your session, you need to speak up immediately. This isn't the time to be tough or quiet. Your practitioner needs to know exactly what you’re feeling, as this may signal that the treatment needs to be adjusted or stopped. Pain is your body’s way of communicating, and listening to it is crucial. Simply telling your provider, "I'm feeling a sharp pain in my lower back on the right side," gives them the information they need to make an immediate change. Remember, the goal is gentle, therapeutic stretching, not painful pulling.
How to Manage Soreness at Home
It’s fairly common to feel some mild soreness or stiffness after your first few spinal decompression sessions, similar to how you might feel after a new workout. Your body is adapting to the changes. To manage this, you can apply an ice pack to the sore area for 15-20 minutes at a time during the first 24 hours to help reduce inflammation. After a day or two, you can switch to a heating pad to help relax tight muscles. Staying hydrated and doing gentle stretches approved by your doctor can also help ease discomfort. This kind of self-care is a vital part of our Physical Medicine approach, supporting your body’s recovery between sessions.
Track Your Soreness Levels
Keeping a simple log of how you feel after each session can be incredibly helpful. Think of it like a journal for your body. Note the intensity of any soreness on a scale of 1 to 10, where it’s located, and what it feels like—is it a dull ache or a sharp twinge? This information isn’t just for you; it’s valuable feedback for your practitioner. Sharing these details helps us fine-tune your treatment plan, ensuring the pressure and angles are perfectly suited to your body’s needs. This simple practice empowers you to take an active role in your recovery and helps us ensure your progress is steady and comfortable.
Gentle Movement and Position Changes
While it might be tempting to stay perfectly still when you’re sore, gentle movement is often your best friend. Light walking can help increase blood flow and prevent stiffness from setting in. Pay attention to your body and avoid any activities that cause sharp pain. Small adjustments to your daily habits can also make a big difference. Try placing a small pillow behind your lower back when sitting or sleeping with a pillow between your knees to maintain spinal alignment. These simple changes support the work being done in your sessions and can help minimize discomfort as your body adjusts.
Using Ice and Heat Therapy
One of the most effective ways to manage post-treatment soreness is with temperature therapy. For the first 24 hours after a session, applying an ice pack to the sore area for 15-20 minutes can help reduce any inflammation. The cold helps constrict blood vessels, which can calm down irritation. After a day or two, you can switch to a heating pad for 15-20 minutes at a time. The warmth helps increase circulation and relax tight, achy muscles. Alternating between ice and heat is a simple yet powerful way to support your body’s recovery process at home.
Breathing to Calm the Nervous System
When you feel sore or uncomfortable, your body can tense up, which sometimes makes the feeling worse. This is where your breath comes in. Simple, deep breathing exercises can help calm your nervous system and release muscle tension. Try taking slow, deep belly breaths, inhaling through your nose for four counts and exhaling through your mouth for six. This practice can shift your body out of a stressed state and into a healing one. It’s a powerful tool that helps you manage discomfort and supports the holistic goals of our functional medicine approach by connecting your mind and body.
Talk to Your Practitioner: What to Say
If the pain you feel after a session is more than just mild soreness, you should contact your practitioner right away. Don’t wait until your next appointment. When you call, be as specific as possible. Instead of just saying, “My back hurts,” describe the sensation. Is it a dull ache or a sharp, shooting pain? Where is it located? Does it travel into your legs or arms? This detailed information helps your provider understand what’s happening. Clear communication ensures they can give you the right advice, whether that’s adjusting your home care routine or modifying your overall treatment plan.
You're in Control: Using the Safety Switch
During every spinal decompression session, you will be given a patient safety switch. This small device is your direct line of control over the treatment. If you feel any uncomfortable or sharp pain, you can press the button to stop the machine immediately. Don't hesitate to use it. Using the safety switch isn’t an overreaction; it’s a built-in feature designed to keep you safe and comfortable. It also provides your practitioner with important feedback. Feeling empowered to stop the treatment if needed is a critical part of a safe and patient-centered therapy experience, which is central to how we treat all health concerns.
When to Call Your Doctor About Post-Treatment Pain
While mild soreness can be a normal part of your body’s adjustment to spinal decompression, it’s crucial to know the difference between typical discomfort and pain that signals a problem. Your healing journey is a partnership between you and your practitioner, and open communication is key. Never hesitate to speak up if something feels wrong. Trusting your instincts and knowing what to watch for ensures your treatment remains safe and effective. If you experience anything beyond a dull, achy sensation, it’s time to pay close attention and likely reach out to your doctor. Your provider is there to guide you, but you are the number one expert on what’s happening in your own body.
Red Flag Symptoms You Can't Ignore
Certain symptoms are considered "red flags" because they can indicate a serious issue that requires immediate medical attention. Think of these as non-negotiable signs to call your doctor right away. Don't wait to see if they go away on their own.
Pay close attention to any of the following:
- Severe or worsening pain
- New nerve problems, like shooting pains, weakness, or numbness in your legs or arms
- Intense muscle spasms you can't control
- Pain that spreads to new areas
- Fever or chills, which could signal an infection
- Loss of bladder or bowel control
These symptoms are not a normal response to spinal decompression. They could point to a variety of underlying health concerns that need to be addressed promptly.
If the Pain Doesn't Go Away
The mild, dull soreness that can sometimes follow a session should start to fade within a day or two. If you’re dealing with pain that sticks around or gets worse, it’s a clear sign to contact your provider. Specifically, if you experience severe pain (a 7 or higher on a 10-point scale) that lasts for more than 48 hours, it’s not a normal reaction. You should also call your doctor immediately if you feel any sharp, acute, or tender pain after your therapy. This is different from general muscle soreness and needs to be evaluated. Your treatment plan is dynamic, and this kind of feedback helps your practitioner make the right adjustments to your physical medicine protocol.
Could It Be a More Serious Problem?
Sometimes, post-treatment pain can be your body’s way of telling you there’s a more significant underlying issue that needs a closer look. For example, sharp pain during or after a session could indicate a problem like a herniated disc that is being aggravated by the treatment. This is why it’s so important to stop immediately if you feel any sharp sensations and let your practitioner know. Pushing through this type of pain is never a good idea. At Ascend, our functional medicine approach is all about identifying and addressing the root cause of your symptoms, and unexpected pain provides valuable information for that process.
Should You Stop Treatment If It Hurts?
Feeling pain during a treatment that’s supposed to bring relief can be confusing and alarming. The short answer is yes, you should absolutely speak up if you feel pain. Spinal decompression is designed to be a gentle, restorative therapy, not an endurance test. Pain is your body’s way of communicating that something isn’t right, and it’s a signal that needs to be addressed immediately.
However, stopping treatment altogether isn’t always the only solution. Often, a simple adjustment is all that’s needed to turn a painful experience into a comfortable one. The key is open communication with your practitioner. They are your partner in this process, but they can’t know what you’re feeling unless you tell them. Think of it less as a red light to stop and more as a yellow light to pause, assess, and work together to find the right path forward for your body. Your comfort and safety are the top priorities, and any good treatment plan has the flexibility to adapt to your unique needs.
Making the Call: Pause or Stop Treatment?
Let’s be clear: spinal decompression should feel like a gentle stretch, not a source of sharp or intense pain. If you experience discomfort that goes beyond a mild pulling sensation, it’s time to speak up. Pain during a session is not normal and can indicate that the pressure is incorrect, your body is positioned improperly, or that the treatment is aggravating an undiagnosed condition. Every decompression table is equipped with a safety switch for this very reason—it allows you to stop the treatment instantly if you feel you need to. Don’t hesitate to use it. Listening to your body and communicating immediately is the best way to ensure your therapy is both safe and effective.
How Your Provider Can Adjust Your Treatment
Your feedback is the most valuable tool your practitioner has to customize your treatment. When you share what you’re feeling, they can make real-time adjustments to improve your comfort. This might involve lowering the amount of force being used, changing the angle of the pull to better target the problem area, or simply adding pillows to support your body in a more comfortable position. Our goal at Ascend is to provide effective Physical Medicine that works with your body, not against it. A successful session is a collaborative effort, and your input helps guide the process to ensure you get the most relief possible without unnecessary discomfort.
Creating a New Plan Together
What if adjustments don’t resolve the pain? This doesn’t mean your situation is hopeless. It simply means that spinal decompression might not be the right fit for you at this moment. Sometimes, a spine needs more stability before it can benefit from traction. If that’s the case, we can pivot. This is where a holistic approach truly shines. We can explore other therapies that might be more suitable for your body’s current needs. By working together, we can create a new plan that addresses the root cause of your pain and puts you on a more effective path to healing. Our wide range of services ensures we can find the right solution for you.
Why At-Home Decompression Attempts Can Be Risky
When you’re dealing with back pain, the idea of finding relief right in your own home can be incredibly tempting. You might see videos of people hanging from bars or using inversion tables, and it’s easy to think, “Maybe that could work for me.” While the intention is good, attempting spinal decompression on your own can be risky. Unlike professional therapy, which uses precise, computer-controlled technology to create a gentle and targeted stretch, at-home methods are often uncontrolled and can put unpredictable stress on your spine. Without a proper evaluation to understand the root cause of your pain, you could inadvertently make the problem worse. True healing comes from a targeted approach, not a one-size-fits-all attempt that can easily do more harm than good.
The Dangers of Hanging Incorrectly
Hanging from a pull-up bar is a common at-home method people try for decompression, but it often leads to more problems. Many people report feeling sharp lower back pain when they hang, especially when they try to relax their muscles or get down. This happens because simply hanging creates a harsh, uncontrolled pull on your entire spine. Your body isn't designed for that kind of abrupt force, and your muscles may instinctively spasm to protect themselves, leading to more pain and even potential injury. Unlike the gentle, cyclical pull of professional decompression, hanging doesn't isolate the problem area or apply a therapeutic force. It’s an imprecise action that can easily strain muscles and ligaments, leaving you in more discomfort than when you started.
Inversion Tables: A Word of Caution
Inversion tables are another popular tool, but they come with their own set of risks. Going completely upside down can place a significant amount of pressure on your spine, joints, and even your blood vessels. While a slight angle might offer a gentle stretch, it’s very difficult to control the exact amount of force being applied. If the treatment is too strong, it can trigger muscle tension, nerve sensitivity, or inflammation. Remember, professional spinal decompression should be a relaxing experience, not a painful one. If you feel any sharp or strong pain while using an inversion table, it’s a clear signal to stop. This is why our Physical Medicine approach always begins with a thorough evaluation to ensure any therapy is perfectly suited to your body’s specific needs.
How to Prepare for Your First Session
Walking into your first spinal decompression session can feel a little nerve-wracking, especially if you’re worried about pain. But a little preparation can make all the difference, turning uncertainty into confidence. The key to a successful experience is open communication and a clear understanding of the process. A great practitioner will guide you every step of the way, but knowing what to expect and how to contribute to your own care empowers you to get the best possible results. Think of it as a partnership—you and your provider are a team working toward your healing.
Your role in this partnership starts before you even get on the treatment table. It involves understanding the initial assessment, knowing what sensations are normal, and being ready to share your complete health story. Taking these steps ensures your treatment plan is safe, effective, and perfectly tailored to you.
Why Your First Step Is a Full Evaluation
Before any treatment begins, your practitioner should conduct a thorough assessment. This initial evaluation is more than just paperwork; it’s the foundation of your entire treatment plan. During this time, we’ll discuss your symptoms, health goals, and the specifics of your condition. This is our opportunity to determine if spinal decompression is the right fit for you and to map out a personalized approach.
A proper assessment also includes a detailed conversation about the therapy itself. Your provider should explain the benefits and any potential risks, ensuring you can make an informed decision about your care. This is your time to ask questions—no matter how small they seem. Understanding the process helps build trust and ensures we’re aligned on the goals of your physical medicine plan.
What to Realistically Expect
Let’s clear the air: spinal decompression therapy should not be painful. During the session, you should feel a gentle, intermittent pulling or stretching sensation in your spine. It’s often described as quite relaxing. However, it’s common to experience some mild muscle soreness after your first few sessions, similar to how you might feel after trying a new workout. This is a normal response as your body adjusts to the treatment.
What you shouldn’t feel is sharp, stabbing, or radiating pain. Those sensations are red flags that something isn’t right. Knowing the difference between normal therapeutic soreness and actual pain is crucial. By setting realistic expectations, you can relax into the treatment and communicate effectively with your provider if you feel anything unusual.
Don't Hold Back: Share Your Full History
Being open and honest about your complete medical history is one of the most important things you can do to ensure a safe session. Your practitioner needs to know everything, from old sports injuries and past surgeries to any underlying health conditions you may have. Even things that seem unrelated can impact how your body responds to treatment.
This information allows us to create a treatment plan that is not only effective but also safe for your specific situation. Certain conditions may require us to adjust the protocol or suggest an alternative therapy altogether. Our goal is always to understand the full picture of your health, which is a core principle of functional medicine. The more we know, the better we can help you heal without causing further issues.
What Safe Spinal Decompression Looks Like
Your experience with spinal decompression should feel safe, controlled, and tailored specifically to you. At Ascend Functional Health, we don’t believe in a one-size-fits-all approach. Instead, we build our care around a foundation of trust and a deep understanding of your unique health needs. Our process is designed to put you at ease from the very beginning, ensuring that every step we take is a collaborative one. We prioritize your comfort and safety above all else, which is why our method is built on three key pillars: a comprehensive evaluation, a personalized treatment plan, and an integrated, whole-body approach to your well-being. This isn't just about treating a symptom; it's about understanding the complete picture of your health to create lasting relief and support your body's innate ability to heal. We know that the idea of any spinal treatment can be intimidating, especially if you're already in pain. That's why we take the time to walk you through every detail, making sure you feel confident and in control. Our goal is to create a therapeutic environment where your body can relax and respond to treatment, not tense up in anticipation of discomfort. By focusing on clear communication and a gentle technique, we ensure your journey toward a pain-free back is as smooth and effective as possible.
A Thorough Evaluation Comes First
Before we even consider starting therapy, we begin with a conversation. Your first step is a thorough evaluation where we sit down with you to discuss your symptoms, your health history, and your goals. We want to understand what you’re feeling and what you hope to achieve. This is your opportunity to ask every question you have, and it’s our responsibility to explain all the potential benefits and risks so you can make a fully informed decision. We look at the full scope of conditions we treat to ensure we have a complete picture of your health. This initial meeting sets the stage for a treatment plan that is truly designed for you.
Your Treatment Plan, Tailored to You
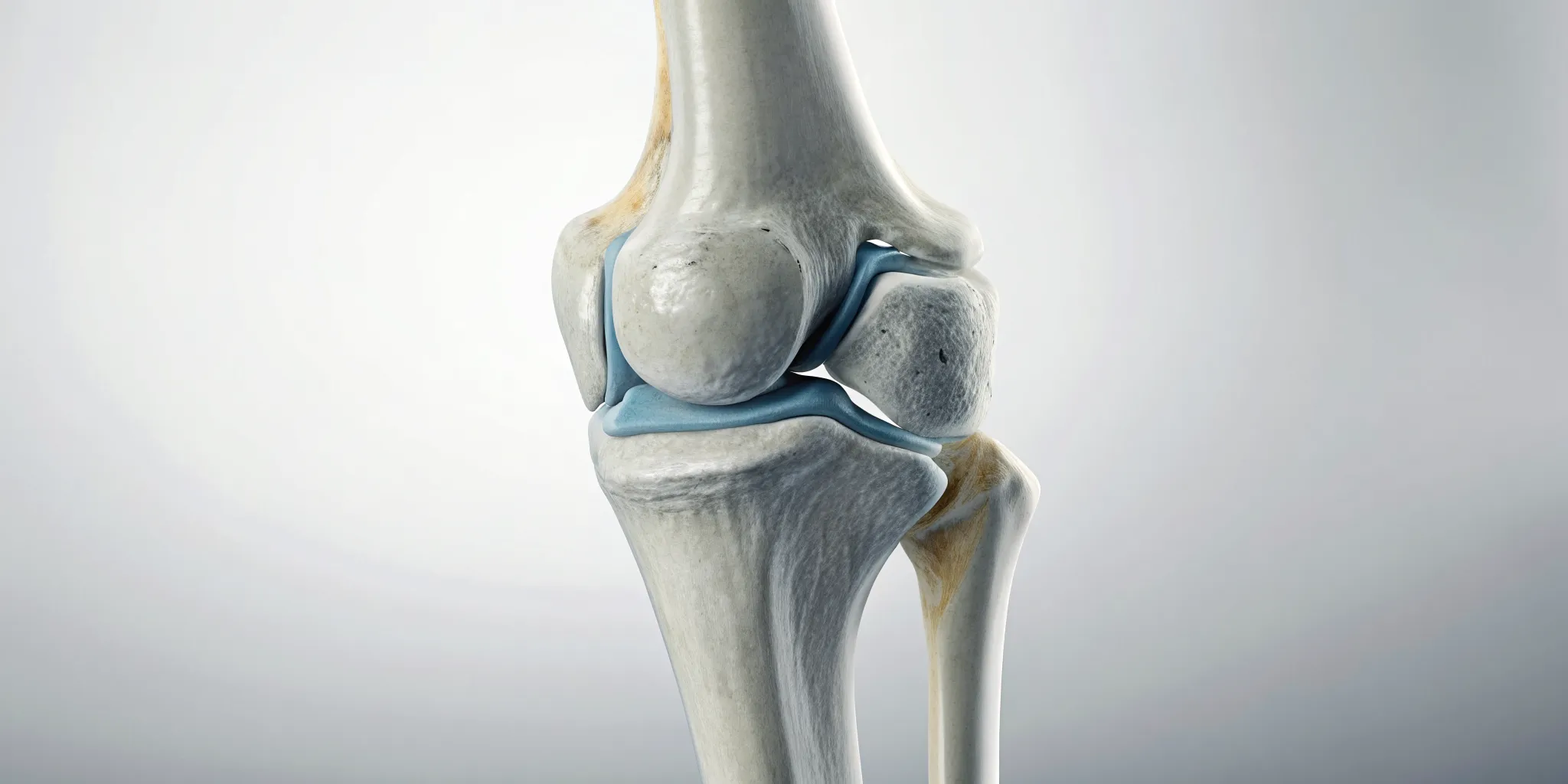
Because your body and your pain are unique, your treatment plan will be, too. Spinal decompression therapy works by creating more space between the vertebrae in your spine, which can relieve the pressure on nerves that cause back pain. We customize the force and angle of the spinal stretch to target your specific problem areas, ensuring the treatment is both gentle and effective. Throughout each session, we monitor your comfort closely. If you ever feel sharp or acute pain, we need you to tell us right away. Think of it as a partnership—your feedback is a critical part of tailoring the therapy for the best possible results within our Physical Medicine services.
The Importance of Correct Technique and Settings
The effectiveness of spinal decompression hinges on precision. It’s not a one-size-fits-all therapy; the settings must be perfectly calibrated to your body. If you feel sharp or sudden pain, it’s a clear red flag that something is off. This isn't something to push through. Pain often signals that the pressure is incorrect for your specific condition or that your body isn't positioned properly on the table. Our approach to Physical Medicine is built on the principle that therapy should support your body's healing process, not cause more stress. Correct technique ensures the gentle, restorative stretch is targeted exactly where you need it, creating the ideal environment for your discs to heal.
This is why your feedback is so important. We rely on you to tell us what you’re feeling so we can make real-time adjustments to the settings. A slight change in the angle of pull or the amount of force can make all the difference between a comfortable, effective session and one that causes discomfort. You are always in control and will have a safety switch to stop the treatment instantly if you feel you need to. A successful session is a team effort, where our expertise and your input come together to create a safe and healing experience.
Looking at the Big Picture of Your Health
Spinal decompression is an incredibly effective, FDA-approved therapy, but we see it as one important piece of a much larger puzzle. We use this versatile treatment to help with a range of issues, including bulging, herniated, or degenerating discs. However, true healing comes from addressing the root cause of your pain. That’s why we integrate your treatment with a whole-body perspective. We may explore how inflammation, nutrition, or other lifestyle factors are contributing to your spinal health. By combining targeted therapy with the insights of Functional Medicine, we can create a more comprehensive and sustainable path toward recovery.
What If Spinal Decompression Isn't for You?
Spinal decompression can be an incredibly effective therapy, but it’s not the right fit for every person or every condition. If you’re finding the treatment painful or it’s simply not delivering the results you hoped for, please don’t feel discouraged. Your healing journey is unique, and sometimes it takes a different approach to find what works for your body. At Ascend, we believe in a whole-body approach, which means we have many other ways to help you get to the root of your pain and find lasting relief. Let’s look at a few other paths we can explore together.
Exploring Other Physical Medicine Options
Spinal decompression is just one tool in a much larger toolbox. Our Physical Medicine services are designed to address the full spectrum of issues that cause discomfort, including upper, middle, and lower back pain, weakness, and limited movement. This comprehensive approach combines treatments like chiropractic adjustments, targeted physical therapy, and other hands-on techniques to restore proper function and alignment. If decompressing the spine isn't providing relief, we can shift our focus to strengthening supporting muscles, improving joint mobility, or correcting postural imbalances that might be contributing to the problem. It’s all about finding the right combination of therapies to support your body’s specific needs.
Getting to the Root of the Problem
Sometimes, persistent pain is a signal that there’s a deeper issue at play. If you continue to experience pain, it's always best to talk to a doctor who can look beyond the immediate symptoms. Back pain isn't always just a mechanical problem; it can be fueled by underlying factors like chronic inflammation, food sensitivities, or even gut health imbalances. Our Functional Medicine approach uses in-depth testing to uncover these root causes. By understanding what’s happening inside your body on a cellular level, we can create a personalized plan with targeted nutrition and lifestyle changes to reduce inflammation and support your body’s natural healing processes from the inside out.
Could Regenerative Medicine Help?
While mild soreness after a new therapy can be normal, sharp pain often means something is wrong. If spinal decompression is causing this kind of discomfort, it could be a sign that the tissues in your back need more intensive support to heal. This is where Regenerative Medicine can be a game-changer. This cutting-edge field uses your body's own healing agents to repair and rebuild damaged tissues like spinal discs, ligaments, and cartilage. For chronic pain that hasn't responded to other treatments, regenerative therapies can offer a powerful way to address the source of the injury directly, helping your body heal itself on a fundamental level for long-term relief.
Frequently Asked Questions
What's the difference between normal soreness and a real problem? Think of normal soreness like the feeling you get after a good stretch or a new workout—it's a dull, generalized ache in your muscles as they adjust. A real problem feels different. It's typically a sharp, stabbing, or shooting pain. You should also watch for any new numbness, tingling, or weakness in your arms or legs. While mild muscle fatigue is a sign your body is adapting, sharp pain is a signal to stop and talk to your practitioner right away.
How many sessions will I need before I feel better? This is a great question, but the answer is different for everyone. Your healing timeline depends on several factors, including the specific condition being treated, how long you've had it, and your overall health. Some people feel relief after just a few sessions, while others with more chronic issues may need a more extended course of treatment. The goal is steady progress, and your practitioner will work with you to map out a plan and adjust it based on your response.
What can I do between sessions to support my healing? Your time at home is a huge part of your recovery. Staying well-hydrated is one of the best things you can do, as it helps your spinal discs rehydrate and heal. Your practitioner will likely give you specific gentle stretches or light exercises to do. It's also important to be mindful of your posture and avoid activities that strain your back, like heavy lifting. Following these simple guidelines can make a big difference in your results.
Are there people who absolutely should not get spinal decompression? Yes, while it's a safe therapy for many, it isn't the right choice for everyone. Generally, it's not recommended for individuals with certain conditions like severe osteoporosis, spinal fractures, or significant spinal instability. It's also typically avoided during pregnancy. This is exactly why we conduct a thorough evaluation before starting any treatment. Being completely open about your medical history ensures we can choose the safest and most effective path for you.
I'm nervous about the treatment. What does it actually feel like? It's completely normal to feel a little anxious, but most people are pleasantly surprised by how comfortable the treatment is. You shouldn't feel any pain. Instead, you'll feel a gentle, rhythmic stretching in your spine as the table slowly and precisely applies and releases traction. Many people find the sensation deeply relaxing and even fall asleep during their sessions. You are always in control and have a safety switch to stop the machine at any moment if you feel uncomfortable.
Related Articles
- Spinal Decompression Hurts Lower Back: Normal or Not?
- Revitalize Your Spine with Spinal Decompression Therapy in Tampa, FL
- Is Lumbar Decompression Chiropractic for You?