A diagnosis of low bone density can feel like a definitive label, but from a functional medicine perspective, it’s simply a clue. It’s your body’s way of telling us that something deeper is out of balance. A bone density screening provides the "what," but our focus is on discovering the "why." Is it a hidden nutrient deficiency, a hormonal imbalance, or an issue with gut health that’s preventing proper absorption? This article will not only explain the mechanics of the screening but will also explore the root causes of bone loss. We’ll show you how to look beyond the diagnosis to create a personalized plan that restores your body’s ability to build and maintain strong bones.
Key Takeaways
- Know your numbers with a simple scan: A bone density test is a quick, painless way to check your bone strength. It's generally recommended for women 65 and older, but certain risk factors, like family history or specific health conditions, mean you might benefit from earlier screening.
- Understand your T-score to take action: Your results will give you a T-score, which shows if your bone density is normal, low (osteopenia), or in the osteoporosis range. Use this information not as a label, but as a guide to work with your provider on a plan to prevent future fractures.
- Build stronger bones through diet, exercise, and root-cause analysis: You can directly support your bone health with calcium-rich foods, vitamin D, and weight-bearing exercises. A functional medicine approach takes this further by investigating underlying issues like hormone imbalances or gut health to create a truly personalized and effective plan.
What Is a Bone Density Screening?
Think of a bone density screening as a way to check in on the strength of your skeleton. Officially known as a DEXA or DXA scan, this simple test uses a special low-dose X-ray to measure the amount of calcium and other essential minerals packed into your bones. The more minerals your bones have, the denser and stronger they are, making them much less likely to break. This scan gives us a clear picture of your bone mass, helping to determine your risk for fractures and conditions like osteoporosis. It's a crucial piece of information for anyone looking to maintain their mobility and quality of life as they age.
It’s a proactive step toward understanding your body on a deeper level. Instead of waiting for a problem like a fracture to occur, a bone density screening allows you to get ahead of potential issues. The results can tell you if you have low bone density (osteopenia) or osteoporosis, a condition that causes bones to become weak and brittle. Knowing where you stand is the first step in creating a plan to protect your bones for years to come. Our team uses these insights to develop personalized health solutions that address your body’s specific needs, focusing on long-term wellness rather than just reacting to symptoms.
How Do DEXA Scans Work?
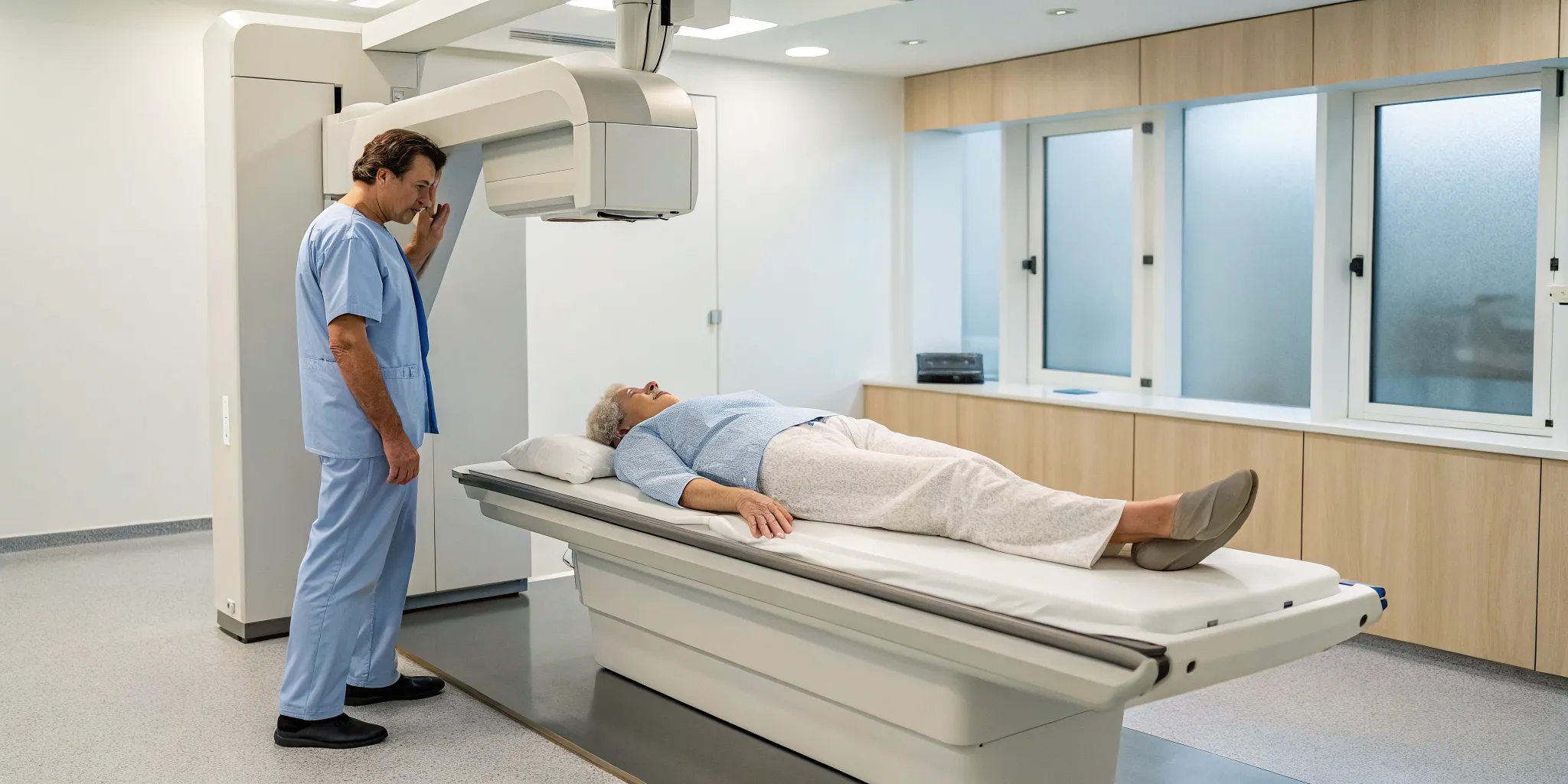
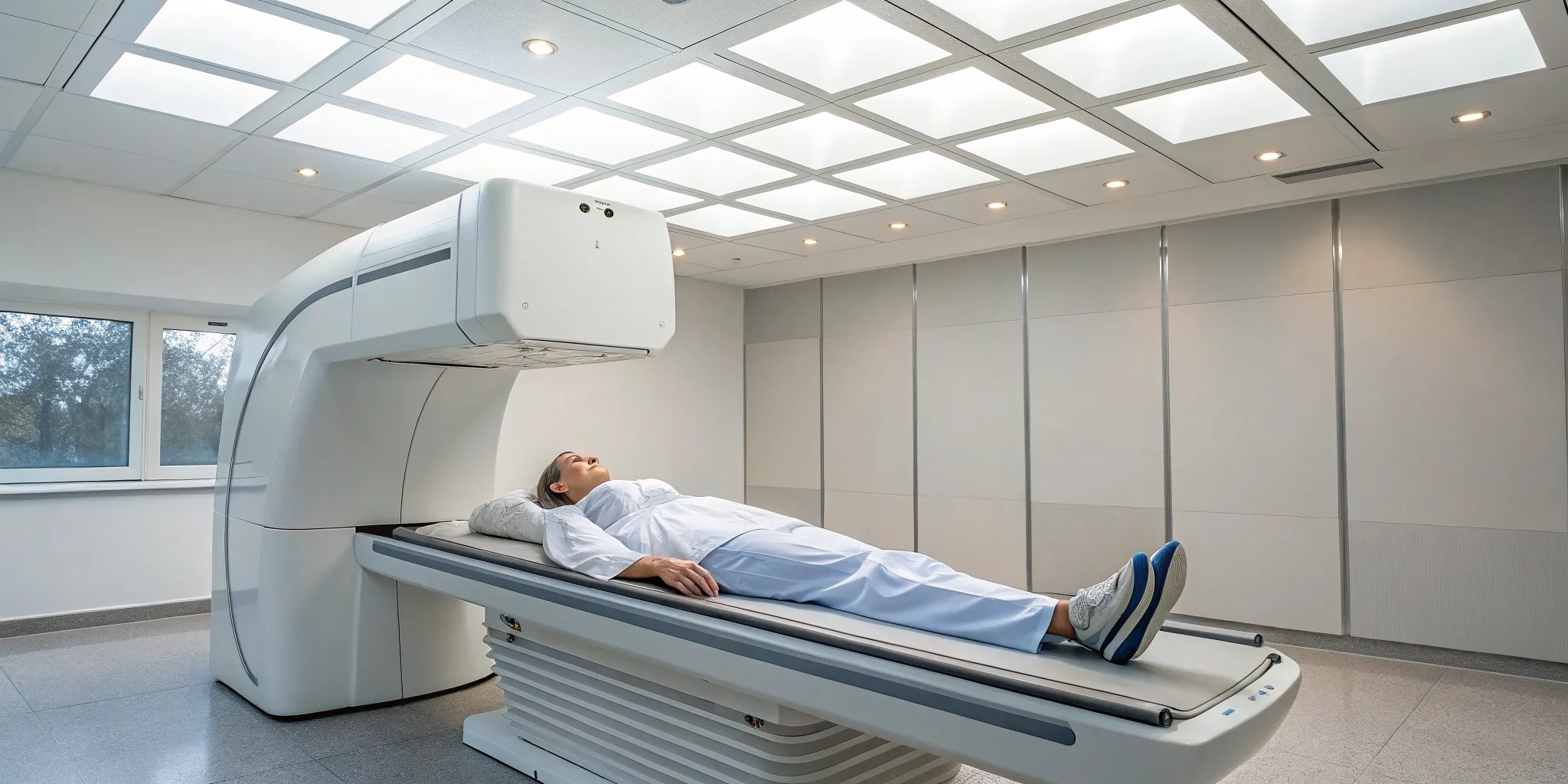
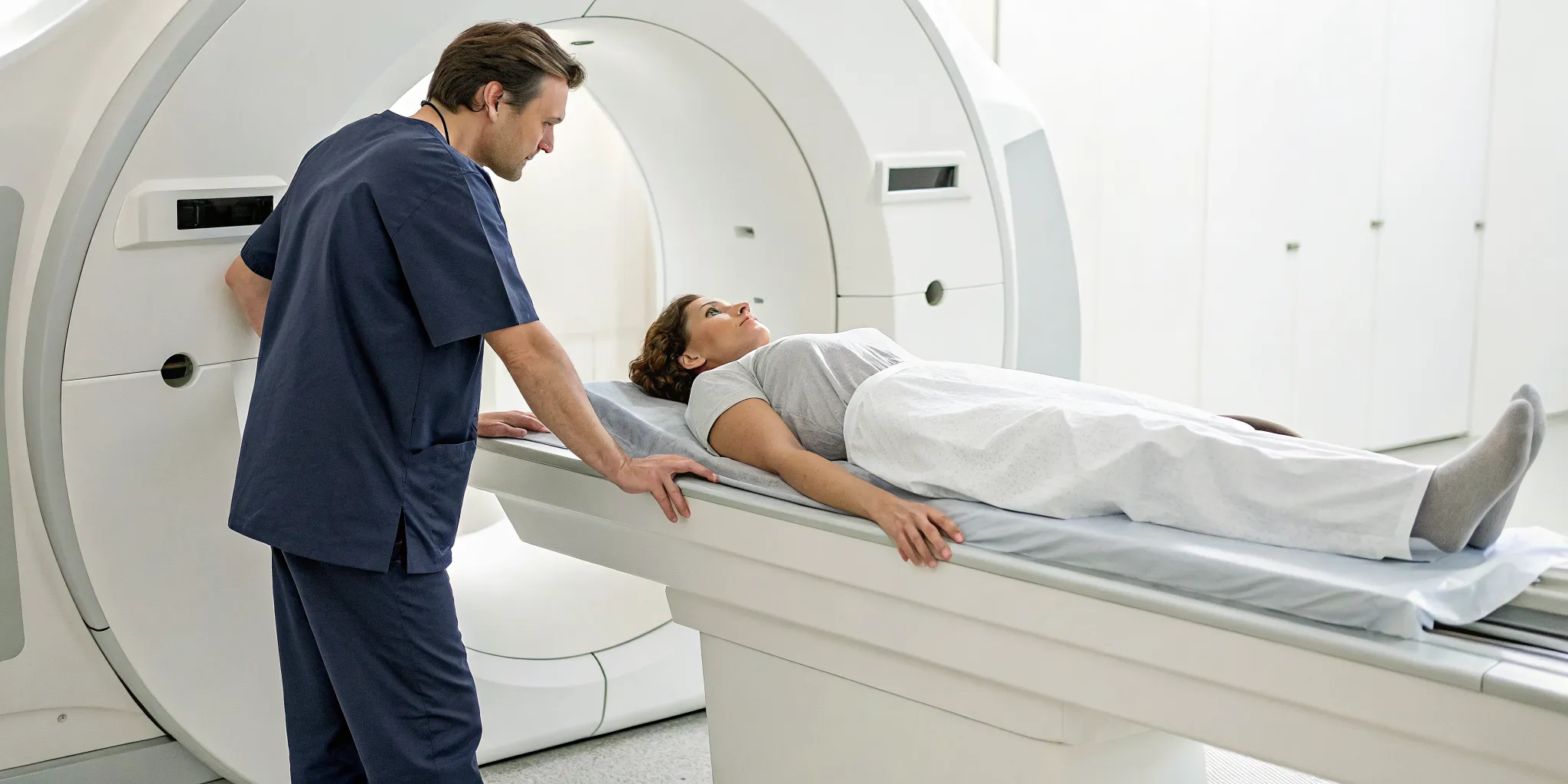
The most common and accurate method for checking bone health is a central DEXA scan, which focuses on your lower spine and hip. The process is straightforward and completely painless. You’ll lie comfortably on your back on a padded table, fully clothed. An imaging arm will slowly pass over your body while another scanner passes underneath. All you have to do is stay still, and you may be asked to hold your breath for a few seconds to ensure a clear image. The entire test is quick, usually taking only about 10 to 20 minutes to complete. It’s a non-invasive way to get a precise snapshot of your bone strength.
Why Your Bone Health Is So Important
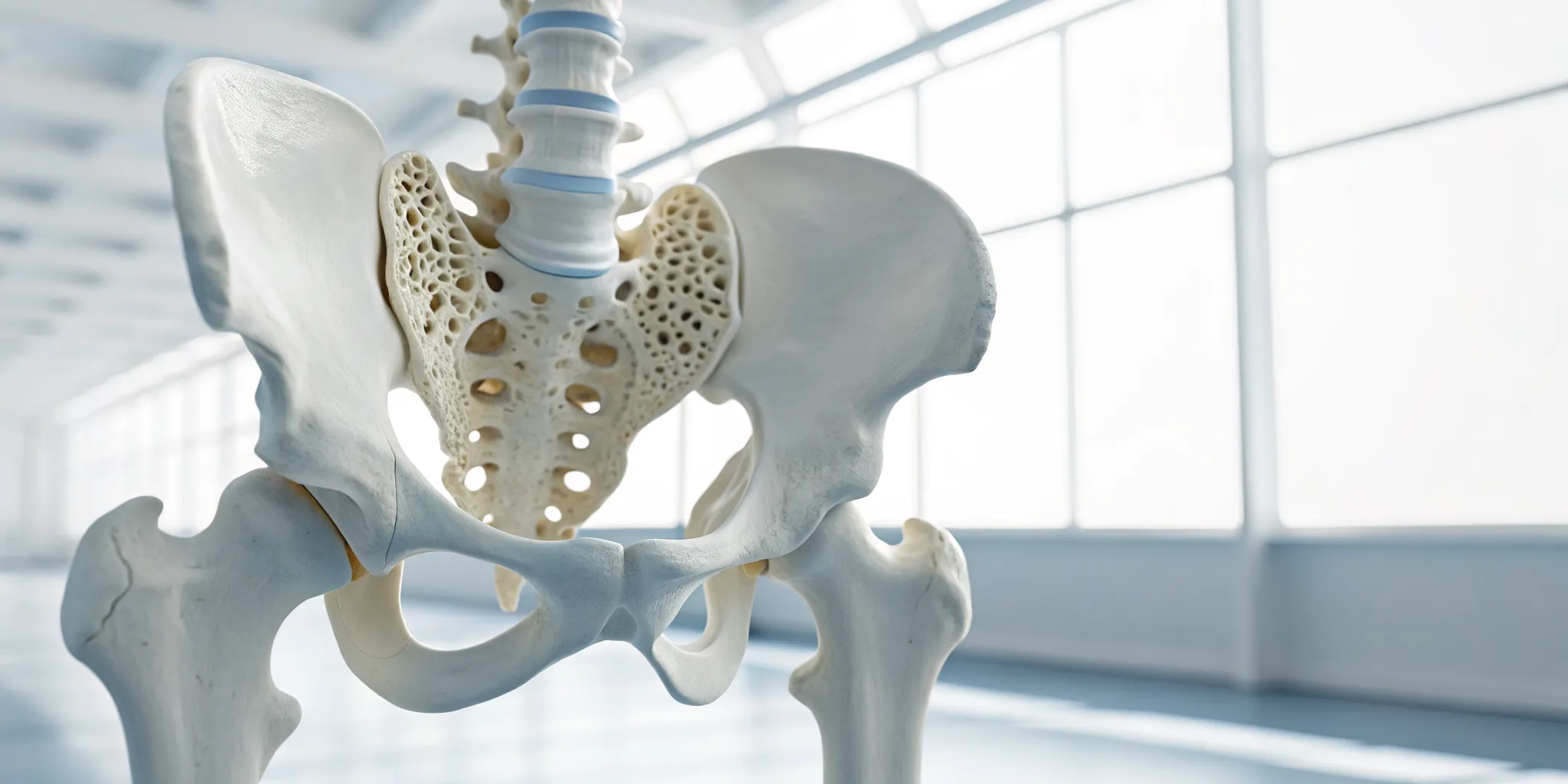
Strong bones are the foundation of a healthy, active life. As we age, our bone density naturally decreases, which can lead to osteoporosis. This disease causes bones to become so thin and brittle that a minor fall or even a strong cough could cause a fracture. It most often affects older adults, particularly women over 65, and the most common fracture sites are the hip, spine, and wrist. A bone density test is the best way to diagnose osteoporosis before a break happens. It helps you understand your personal fracture risk so you can take meaningful steps to protect your bones and maintain your independence.
Who Needs a Bone Density Screening?
A bone density screening isn't something everyone needs, but for certain people, it's an incredibly important tool for understanding long-term health. Think of it as a proactive check-in on your skeletal framework. As we get older, our bones can naturally lose density, making them more fragile and susceptible to fractures. The goal of a screening is to catch this process early, long before a break happens.
Deciding whether you need a scan comes down to a few key factors, including your age, gender, and personal health history. While there are general guidelines, your unique circumstances are what matter most. Understanding these recommendations is the first step in having an informed conversation with your healthcare provider about whether a bone density test is the right next step for you. It’s all about getting ahead of potential issues and creating a plan to keep your bones strong for years to come.
Guidelines by Age and Gender
The most common question people have is, "When should I get my first bone density scan?" General guidelines provide a great starting point. For most women, the recommendation is to get a baseline bone density scan at age 65 or older. This is because the hormonal shifts of menopause can accelerate bone loss, making this age a critical checkpoint.
For men, the guidelines are a bit different. Routine screening isn't typically recommended for all men. However, if you are a man over 65 and have concerns about your bone strength, or if you have other risk factors, it's a good idea to talk with your doctor about whether a scan is appropriate for you.
Key Risk Factors for Earlier Testing
Age isn't the only piece of the puzzle. Many people benefit from getting screened earlier than 65 due to specific risk factors that can affect bone health. Postmenopausal women younger than 65 should consider a scan if they have factors that increase their chances of developing osteoporosis.
These can include having a low body weight, losing more than half an inch in height in one year, or breaking a bone after age 50. Your family and medical history also play a huge role. A parent who had osteoporosis or a hip fracture is a significant indicator, as are certain medical conditions and medications. Changes in your hormones, which we can explore through Longevity Medicine, are also a critical factor to consider.
What Are the Main Risk Factors for Osteoporosis?
Understanding your risk for osteoporosis is the first step toward protecting your bone health. Some factors are within your control, like diet and exercise, while others, such as your family history and age, are not. The key is to know where you stand so you can be proactive. By identifying your personal risk factors, you can work with your healthcare provider to create a plan that keeps your bones strong and resilient for years to come. This isn't about feeling overwhelmed; it's about gathering information to make empowered decisions for your long-term well-being.
How Lifestyle and Diet Play a Role
The daily choices you make have a significant impact on your bone density. A diet lacking in calcium and vitamin D is one of the biggest contributors to weakened bones, as these nutrients are the primary building blocks for bone tissue. Similarly, a sedentary lifestyle can be detrimental. Your bones respond to stress by becoming stronger, which is why weight-bearing exercises are so crucial. Habits like smoking or drinking too much alcohol can also interfere with your body's ability to absorb calcium and build new bone. Even having a low body weight can increase your risk, as it often correlates with smaller, less dense bones.
Medical Conditions and Medications
Sometimes, bone loss is a side effect of another health challenge or medication. Certain medical conditions, including rheumatoid arthritis, hyperthyroidism, and some gastrointestinal diseases, can accelerate bone weakening. It’s a reminder of how interconnected our body systems are. Additionally, the long-term use of specific medications, such as corticosteroids, can contribute to a decline in bone density. This is why our approach to functional medicine involves looking at your complete health picture. By understanding all the contributing factors, we can better address the root cause of bone loss instead of just managing the symptoms.
Hormones and Family History
Two of the most significant risk factors for osteoporosis are things you can’t change: your hormones and your genes. Hormonal shifts, particularly the drop in estrogen women experience after menopause, can lead to rapid bone loss. Estrogen plays a protective role in bone maintenance, so when levels decline, bones can become more vulnerable. Your family history is another important piece of the puzzle. If one of your parents had osteoporosis or experienced a hip fracture, your own risk is higher. While you can't alter your genetic makeup, knowing your family history gives you a powerful reason to focus on the lifestyle factors you can control.
What to Expect During Your Bone Density Test
If your doctor has recommended a bone density test, you might be wondering what the experience is actually like. The good news is that it’s one of the easiest and most painless diagnostic tests you can have. It’s a quick, non-invasive way to get a clear picture of your bone health, and knowing what to expect can make the process feel even more straightforward. Many people picture a loud, enclosed machine like an MRI, but a bone density scan is a much more open and quiet experience.
From a few simple prep steps to the scan itself, the entire process is designed to be simple and comfortable. We'll walk you through exactly what happens before, during, and after your appointment so you can feel confident and prepared. At Ascend Functional Health, we believe that understanding your health journey is key to achieving your wellness goals. Our comprehensive approach focuses on getting to the root cause of health issues, and a bone density test is a valuable tool in that process. It gives us the data we need to create a personalized plan for you, whether that involves nutritional guidance, lifestyle adjustments, or other targeted therapies.
How to Prepare for Your Test
Getting ready for your bone density test is simple. Your doctor will likely ask you to stop taking any calcium supplements for 24 to 48 hours before your appointment. On the day of the test, choose comfortable clothing without any metal parts like zippers, buttons, or buckles. It’s also best to leave any metal jewelry at home. Think of it like getting ready for a yoga class: simple, comfy, and metal-free. If you have any questions about your specific medications or how to prepare, don't hesitate to contact our office. We're here to make sure you feel completely at ease before you even walk through the door.
A Step-by-Step Look at the Process
The most common type of bone density test is called a central DEXA scan, which is considered the gold standard for accuracy. During the scan, you’ll lie comfortably on your back on a padded table, fully clothed. A mechanical arm will slowly pass over your body while another scanner moves underneath you. The whole thing is completely open, so you won't feel enclosed or claustrophobic. You’ll just need to stay still for a few minutes and may be asked to hold your breath for a few seconds at a time. The test itself usually takes only 10 to 30 minutes, and then you’ll be on your way.
Is It Safe? A Note on Radiation
It's natural to have questions about safety, especially when X-rays are involved. Bone density scans use a very low dose of radiation, even less than what you’d get on a cross-country flight, making them safe for most people. However, the scan is not recommended if you are pregnant or think you might be, as any amount of radiation can pose a risk to a developing baby. It's incredibly important to let your provider know if there's any chance you could be pregnant before your test. Your safety is always our top priority, and we'll take every precaution to ensure your well-being.
How to Read Your Bone Density Results
Getting your bone density results can feel a little intimidating, especially when you're faced with terms like "T-score" and "Z-score." But don't worry, these numbers are just tools to help you and your doctor understand your bone health. They provide a clear snapshot of where you stand and what your next steps should be. Let's break down what these scores mean so you can feel confident and informed about your results.
What Are T-Scores and Z-Scores?
Your report will feature two key numbers: a T-score and a Z-score. The T-score is the most common measurement for postmenopausal women and men over 50. It works by comparing your bone density to the optimal bone density of a healthy 30-year-old. Here’s how to interpret it:
- -1.0 or higher: Your bone density is considered normal.
- Between -1.0 and -2.4: This indicates low bone density, also known as osteopenia.
- -2.5 or lower: This score suggests you likely have osteoporosis.
The Z-score is used for premenopausal women, men under 50, and children. Instead of comparing you to a young adult, it compares your bone density to what’s normal for someone of your same age, sex, and body size. A bone density scan provides this detailed picture for your doctor.
What Your Score Means for Your Health
A score in the osteopenia or osteoporosis range isn't a reason to panic, but it is a clear signal to take action. Your first step should always be to discuss the results with your healthcare provider. They can help you create a personalized plan to protect your bones and prevent fractures. This plan will likely include lifestyle adjustments, such as incorporating weight-bearing exercises like walking or strength training into your routine.
You'll also want to focus on getting enough calcium and vitamin D through your diet or supplements. At Ascend, our functional medicine approach helps identify the root causes of bone loss to create a targeted plan for you. Depending on your results and risk factors, your doctor may also recommend follow-up scans every few years to monitor your progress.
What to Do If You Have Low Bone Density
Getting a diagnosis of low bone density can feel a little unsettling, but it's really the first step toward taking control of your bone health. Think of it as a roadmap. Now you know the terrain and can choose the best path forward to build stronger, more resilient bones. The great news is that there are many effective strategies, from medical treatments to simple lifestyle adjustments, that can help protect your bones for years to come. It’s all about creating a proactive plan that works for you and your body.
Exploring Your Treatment Options
Your first step is to chat with your healthcare provider to create a personalized plan. Depending on your specific situation, they might suggest a few different approaches to stop further bone loss. This often includes a combination of regular, weight-bearing exercise like walking or strength training, and focusing on nutrition to ensure you’re getting enough calcium and vitamin D. In some cases, your doctor may also discuss medications designed to strengthen your bones and lower your fracture risk. At Ascend, our functional medicine approach helps us create a protocol tailored specifically to your body’s needs.
Lifestyle Changes to Build Stronger Bones
Beyond medical treatments, small changes to your daily routine can make a huge difference in your bone health. Focus on incorporating calcium-rich foods into your diet, like yogurt, cheese, and leafy greens such as spinach and collards. It's also important to get enough vitamin D, which helps your body absorb that calcium. You can find it in fatty fish, fortified foods, and good old-fashioned sunshine. And don't forget to move your body! Aiming for regular physical activity not only strengthens your muscles but also helps maintain your bone strength and improves your balance.
How Often Should You Get Screened?
After your first bone density test, you’ll naturally wonder when you need to get another one. The answer isn’t the same for everyone. Your follow-up schedule depends entirely on your initial results, your personal risk factors, and your overall health picture. The goal is to monitor your bone health effectively without unnecessary testing. Working with a healthcare provider who understands your unique situation is the best way to determine a timeline that makes sense for you. At Ascend Functional Health, our comprehensive approach helps create a personalized plan tailored to your body’s needs, ensuring we track your progress and make adjustments only when necessary. This prevents over-testing while keeping a close eye on what matters most: your long-term bone strength and well-being.
Guidelines for Follow-Up Testing
When it comes to bone density screening, the frequency of follow-up tests is based on your individual risk level. According to MedlinePlus, how often you need another bone density scan depends on your results and risk profile. For those with a low risk of fractures, a follow-up test might not be needed for 10 to 15 years. If you fall into a moderate-risk category, re-testing every three to five years is often recommended. For individuals at high risk, more frequent monitoring, typically every two years, is suggested to track changes and adjust treatment plans as needed. This tiered approach ensures you get the right level of care at the right time.
A Look at Insurance and Costs
Understanding the financial side of bone density screenings is a practical step for many patients. The good news is that most insurance plans recognize this test as a vital preventive screening, especially for at-risk individuals. As noted by MyHealthfinder, many insurance plans, including Medicare, cover bone density screenings for women who meet the criteria. However, coverage details can vary, so it’s always a good idea to call your insurance company directly to confirm your specific benefits and find out about any potential out-of-pocket costs. This simple step can help you plan ahead and avoid any surprises, allowing you to focus on your health.
How to Strengthen Your Bones Naturally
Whether your bone density results were exactly what you hoped for or a bit of a surprise, the next steps are all about proactive care. The great news is that you have so much power to support your bone health through simple, daily habits. Think of it less as a strict regimen and more as a way of life that nourishes your body from the inside out. The two most powerful tools you have are what you eat and how you move. By focusing on specific nutrients and incorporating the right kinds of exercise, you can help slow bone loss and build a stronger foundation for the years to come.
The Best Foods for Bone Health
Building strong bones starts on your plate. Calcium is the star player, acting as the primary building block for your bone structure. You can find it in dairy products like milk, yogurt, and cheese, but also in plant-based sources like leafy greens (think collard greens and spinach) and fortified foods. But calcium can’t do its job alone; it needs vitamin D to help your body absorb it effectively. Your body naturally produces vitamin D from sun exposure, but you can also get it from fatty fish like salmon and tuna. Our approach to functional medicine helps you understand how your diet directly impacts your body’s systems, including your skeletal health.
Exercises to Improve Bone Density
Movement is essential for telling your bones to stay strong. When you engage in specific types of exercise, you put gentle stress on your bones, which signals your body to build more bone tissue. A well-rounded routine includes a mix of activities. Weight-bearing exercises, where your body works against gravity, are fantastic. This includes things like walking, jogging, or even dancing. Muscle-strengthening exercises, like lifting weights, also help support your skeleton. Finally, don’t forget balance exercises like tai chi, which can improve stability and reduce fall risk. Our physical medicine services can help you find a safe and effective movement plan tailored to your body’s needs.
How Functional Medicine Improves Bone Health
Receiving a diagnosis of low bone density can feel like a final verdict, with medication often presented as the only path forward. But what if we looked at it differently? Instead of just treating the symptom (bone loss), what if we asked why it’s happening in the first place? This is the core principle of functional medicine. It’s a partnership approach that goes beyond the diagnosis to understand the unique story of your body and health.
We see bone health as a reflection of your body's overall wellness. Weakening bones are often a sign that something else is out of balance, whether it’s a hidden nutrient deficiency, a hormone imbalance, or chronic inflammation. Our goal is to connect those dots. By addressing the root causes, we can create a personalized and sustainable plan to not only halt bone loss but also help your body rebuild stronger, healthier bones for the long run. It’s about restoring your body’s innate ability to heal and thrive, giving you the tools and support you need to feel strong and resilient.
Finding the Root Cause of Bone Loss
Think of us as health detectives. Instead of just noting that your bones are losing density, we investigate the underlying reasons. Bone loss is rarely caused by a single issue; it’s usually a combination of factors unique to you. Our functional medicine approach involves a deep look into potential contributors that conventional medicine might overlook. We explore everything from chronic inflammation and poor gut health, which can hinder nutrient absorption, to imbalances in key hormones like estrogen, testosterone, and thyroid hormones. We also assess for deficiencies in crucial bone-building nutrients like vitamin D, vitamin K2, magnesium, and calcium, creating a complete picture of your health.
Our Comprehensive Approach to Treatment
Once we identify the root causes, we build a personalized roadmap to better bone health. This isn't a one-size-fits-all protocol. Your plan is tailored specifically to what your body needs to restore balance and function. It typically includes targeted nutritional guidance to ensure you’re eating foods that support bone formation, along with specific, high-quality supplements to correct any deficiencies. We also incorporate personalized exercise recommendations and stress management techniques, as both play a vital role in how your body builds and maintains bone. By addressing all these interconnected pieces, we help you create a strong foundation for lasting bone health.
Related Articles
- Functional Movement Screening: A Complete Guide
- Functional Medicine Doctor: A Patient's Guide
- What is Functional Medicine? A Simple Guide
Frequently Asked Questions
Is a bone density scan uncomfortable or claustrophobic? Not at all. It’s one of the easiest medical tests you can have. You simply lie down on a comfortable, padded table, fully clothed, while a scanner arm passes over you. The machine is completely open, so you won't feel enclosed like you might in an MRI. The entire process is quiet, painless, and usually finished in about 15 minutes.
What's the real difference between osteopenia and osteoporosis? Think of osteopenia as a yellow light for your bone health. It means your bone density is lower than the ideal, but not low enough to be classified as osteoporosis. It’s a warning sign that gives you a valuable opportunity to be proactive. Osteoporosis is the red light; it’s a more serious condition where bones have become significantly weak and are at a much higher risk of fracturing.
Can I actually rebuild bone, or just prevent more loss? Your body is constantly in a state of remodeling bone tissue, so improving bone density is absolutely possible. While the primary goal is to halt further loss, a targeted plan can help your body build stronger bones. This involves more than just taking calcium; it requires a comprehensive approach that includes the right nutrition, specific exercises, and addressing any underlying health issues that might be contributing to the loss in the first place.
I'm not over 65. Why should I think about my bone health now? Your bone density peaks around age 30. Think of it like a savings account: the more bone mass you build in your younger years, the more you have to draw from as you get older. The habits you form now, from your diet to your exercise routine, directly impact how strong your skeleton will be later in life. Being proactive is the best way to set yourself up for long-term strength and mobility.
How is a functional medicine approach to bone health different from what my regular doctor might suggest? A conventional approach often focuses on diagnosing and managing bone loss, typically with medication, after it has already occurred. Functional medicine works a bit differently by asking why the bone loss is happening. We investigate the root causes, which could be anything from a hidden hormone imbalance or poor gut health preventing nutrient absorption to chronic inflammation. By identifying and addressing these underlying factors, we create a personalized plan to help your body restore its own ability to build and maintain strong bones.