Figuring out the financial details of your healthcare doesn't have to be overwhelming. When you're considering a specialized treatment like spinal decompression, being proactive is your greatest asset. Instead of just wondering, "is spinal decompression covered by insurance?", you can take clear, simple steps to get a definitive answer. This guide is designed to be your action plan. We'll provide the exact questions to ask your benefits administrator, explain the paperwork you'll need to gather, and show you how to work with our team to manage any preauthorization requirements. Our goal is to demystify the process and put you in the driver's seat of your health journey, giving you the confidence to move forward with your care.
Key Takeaways
- Know why approval can be complex: Spinal decompression is sometimes labeled "investigational" by third-party payers, not because it's unsafe, but because they require specific types of long-term data. Understanding this helps you and your doctor build a stronger case for your care.
- Be proactive with your financial planning: The best way to clarify your potential costs is to contact your plan administrator directly. Ask specific questions about non-surgical spinal decompression and work with your healthcare team to manage any required preauthorization paperwork.
- Consider all your payment options: If direct payment from your plan isn't an option, you can still move forward. Look into using pre-tax funds from an HSA or FSA, and ask your clinic about flexible payment plans that allow you to invest in your health without financial strain.
What Is Spinal Decompression?
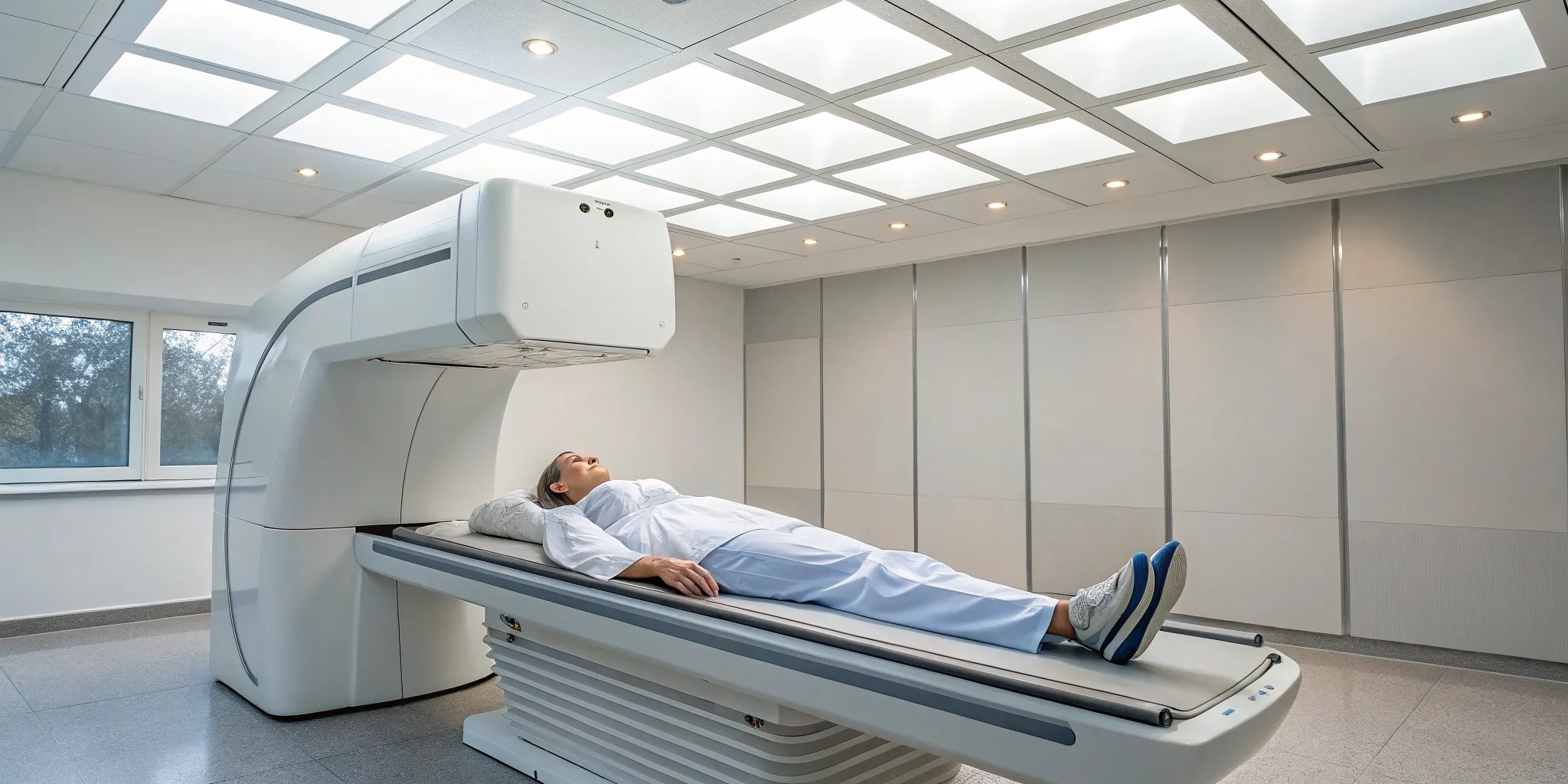
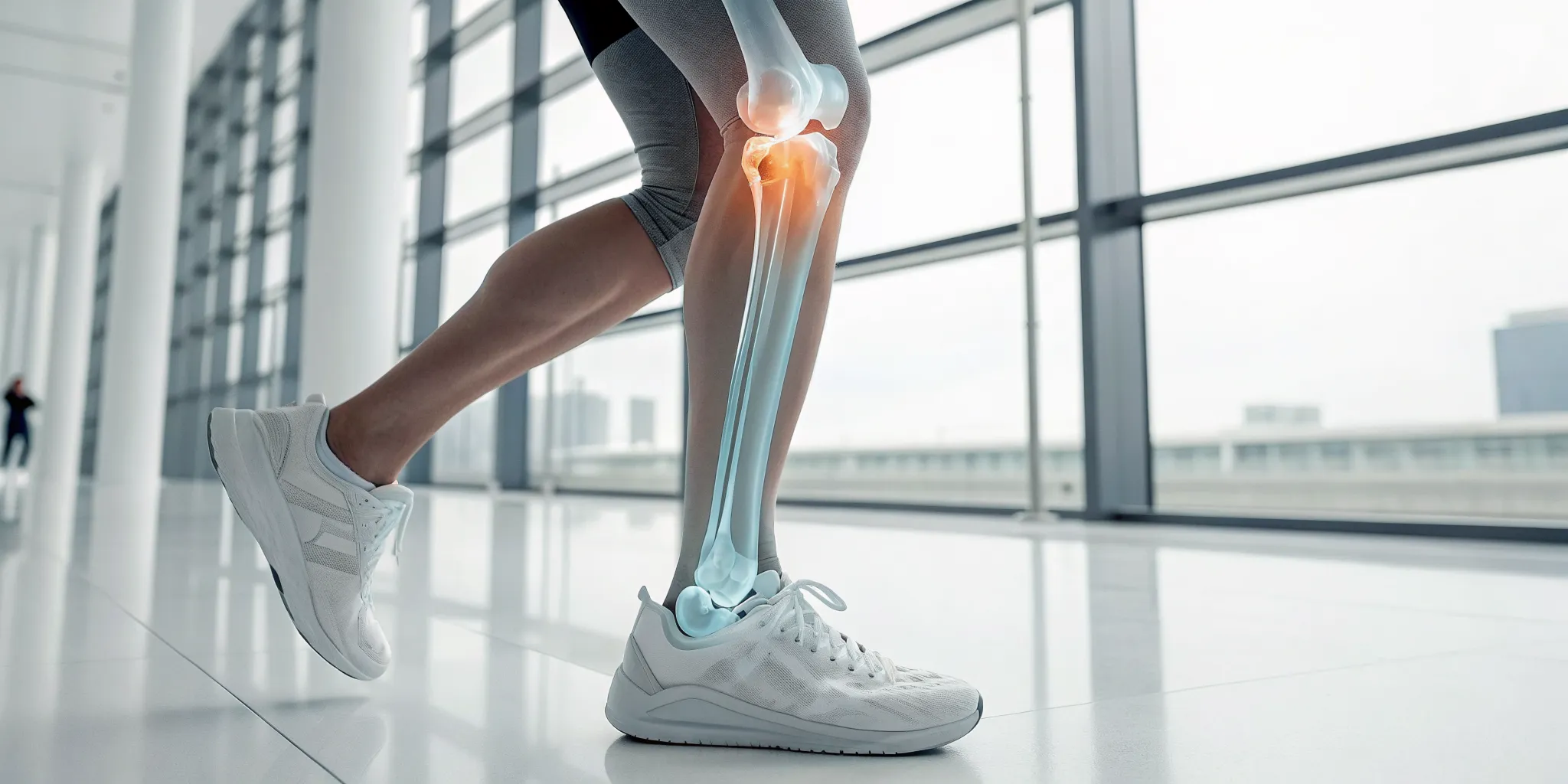
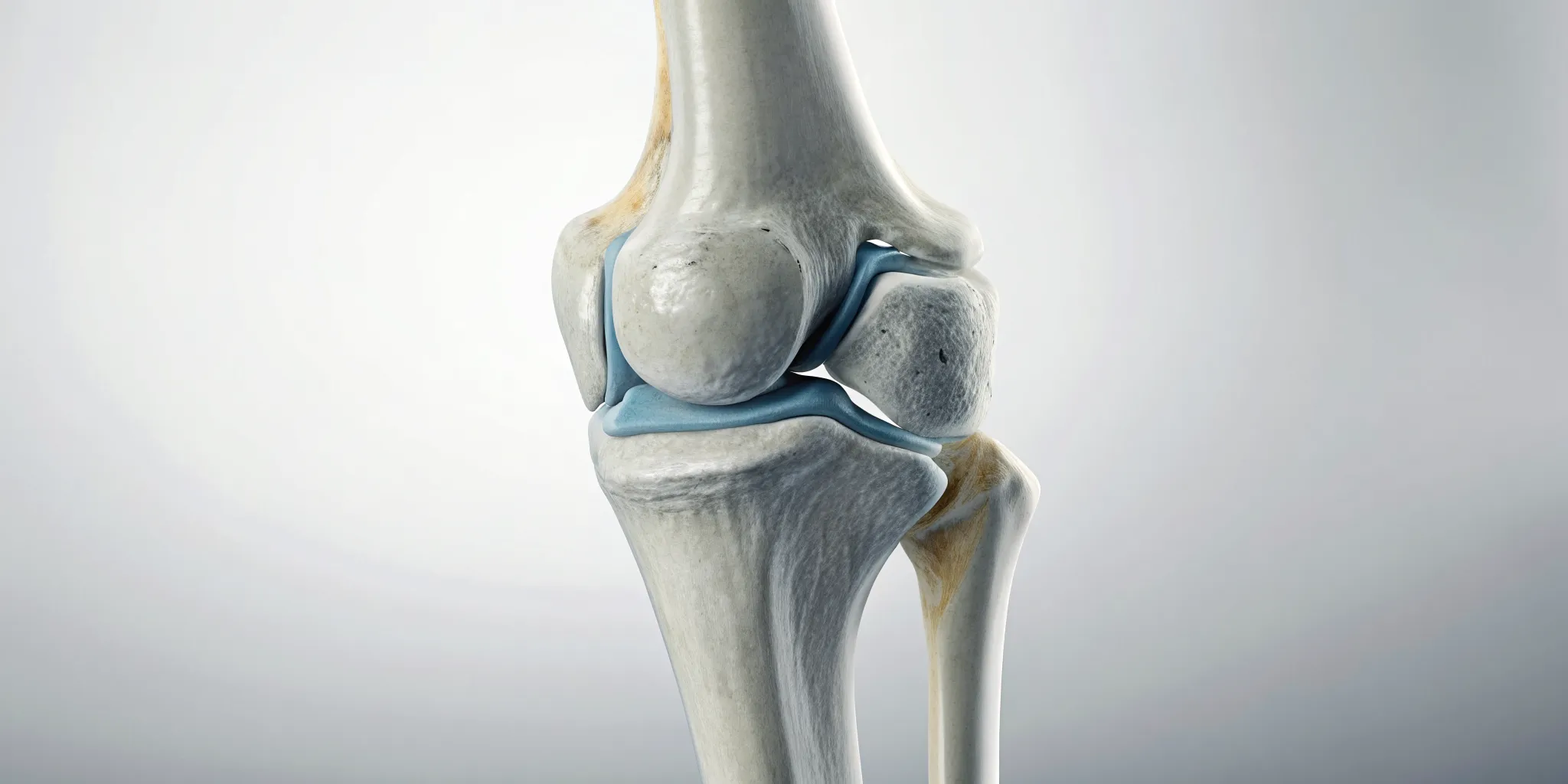
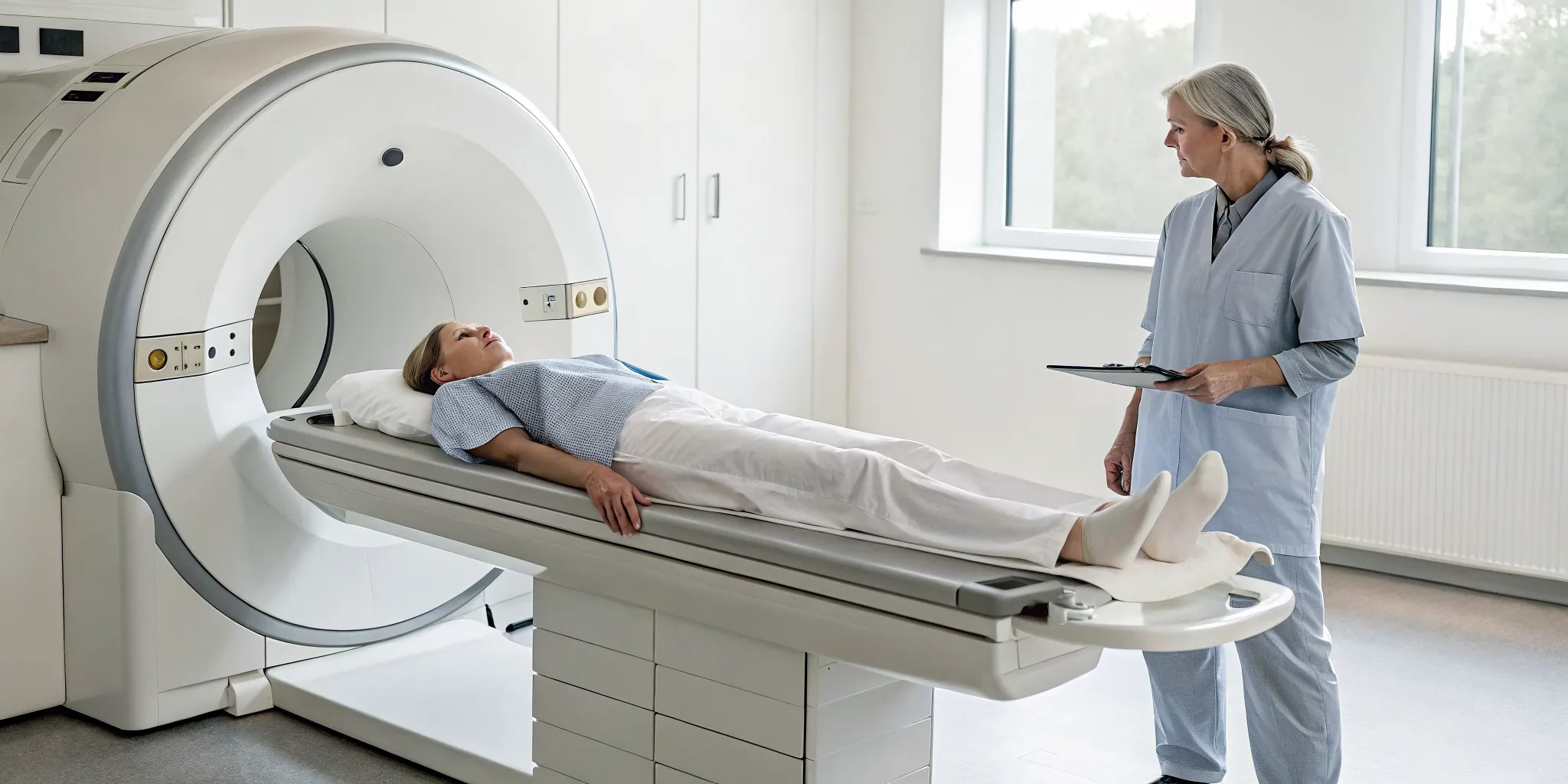
If you're dealing with persistent back or neck discomfort, you’ve likely looked into a lot of different options. Spinal decompression is a gentle, non-invasive therapy designed to relieve pressure on your spine. Think of it as a sophisticated and targeted way to create space in your spinal column, giving your body a chance to heal.
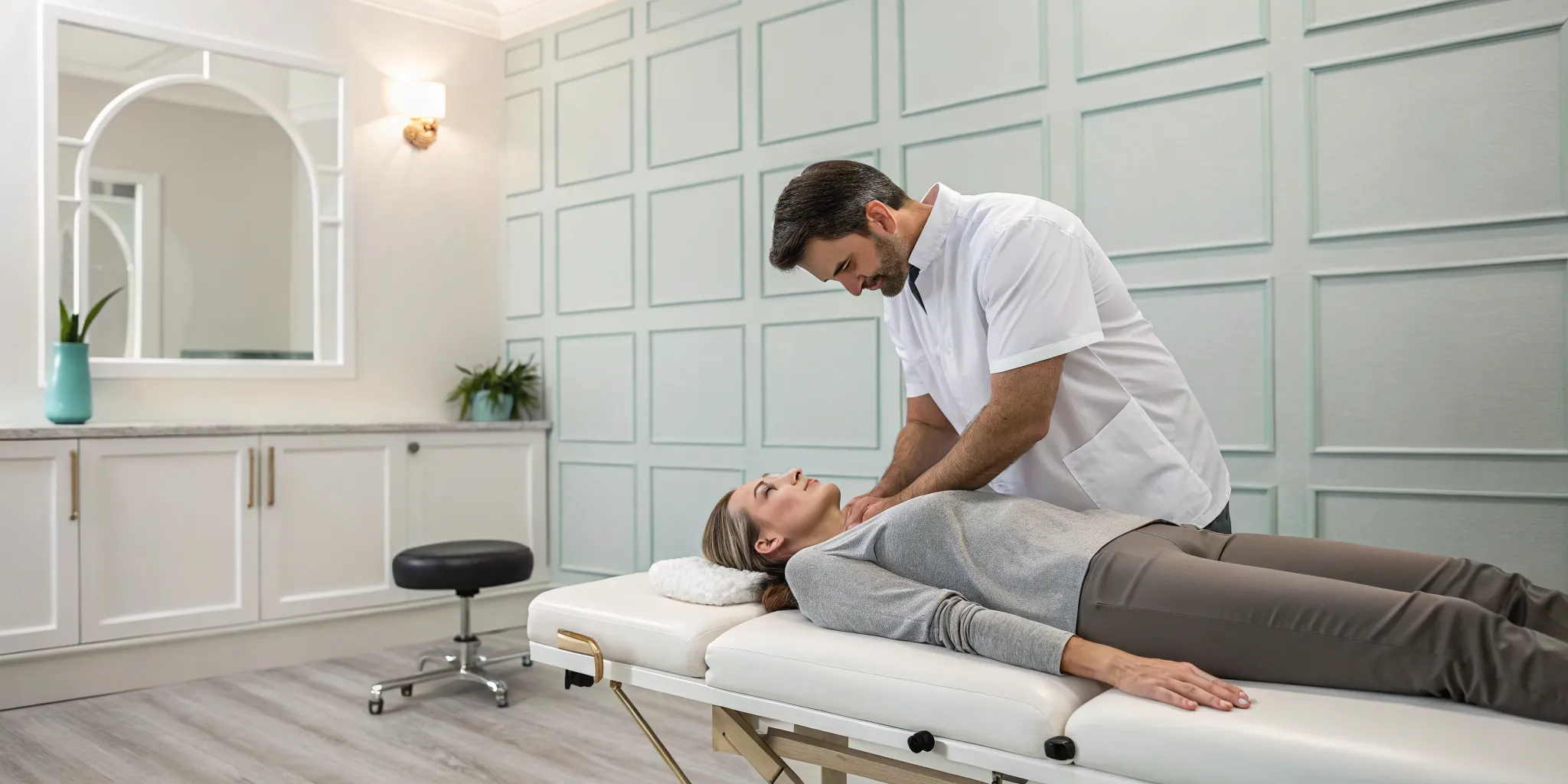
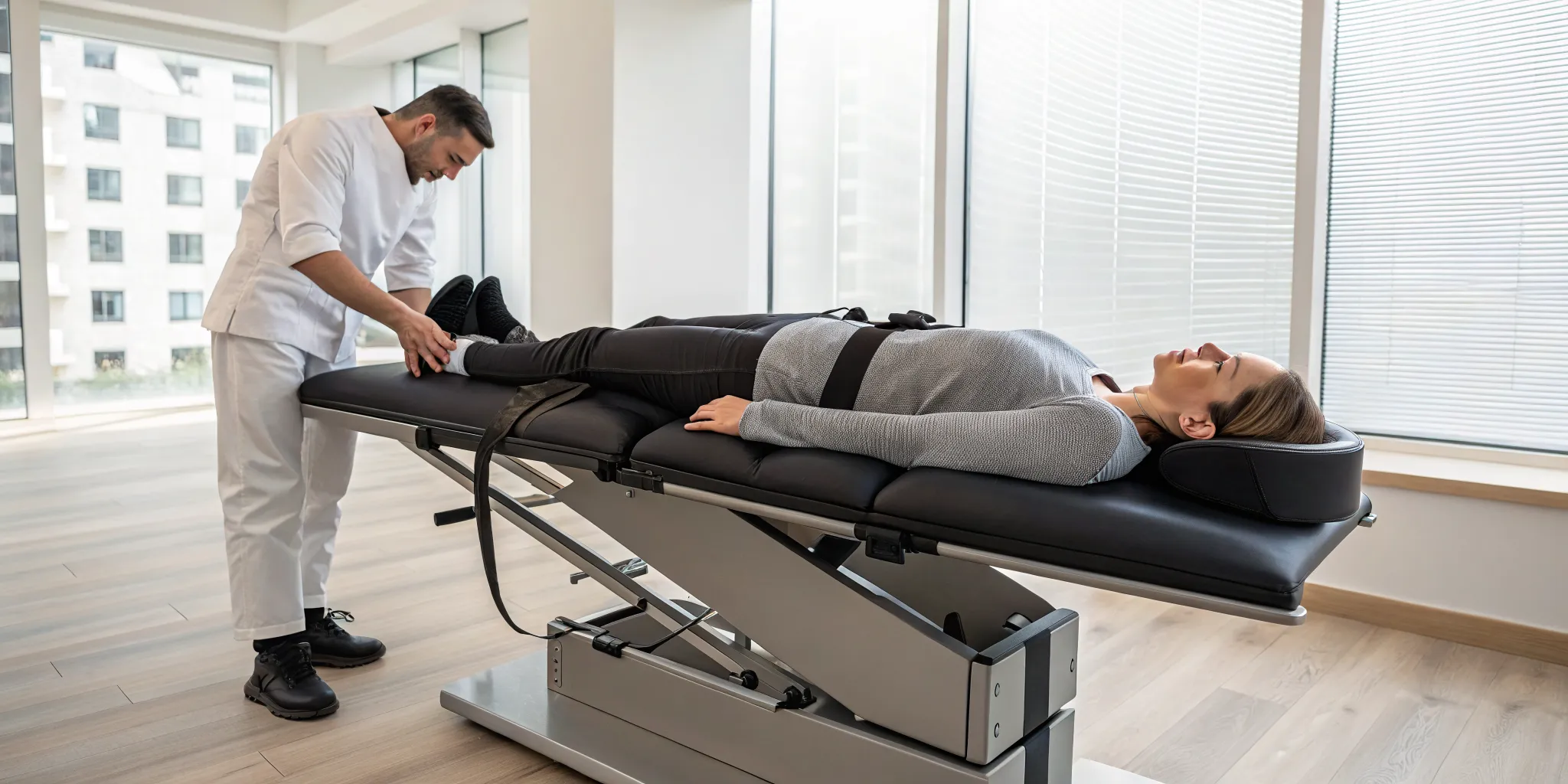
During a session, you’ll rest comfortably on a specialized table. This table is motorized and computer-controlled to apply a very precise and gentle stretching force to your spine. This isn't a jarring or aggressive movement; instead, it’s a slow, controlled elongation that methodically separates the vertebrae. The goal is to reduce the pressure on your spinal discs, which act as cushions between the bones. When these discs are compressed, they can bulge or put pressure on nerves, leading to discomfort. By creating negative pressure within the disc, this therapy helps your body’s natural healing processes get to work. It's a cornerstone of a holistic physical medicine approach that focuses on addressing the underlying cause of your symptoms.
How Does It Work?
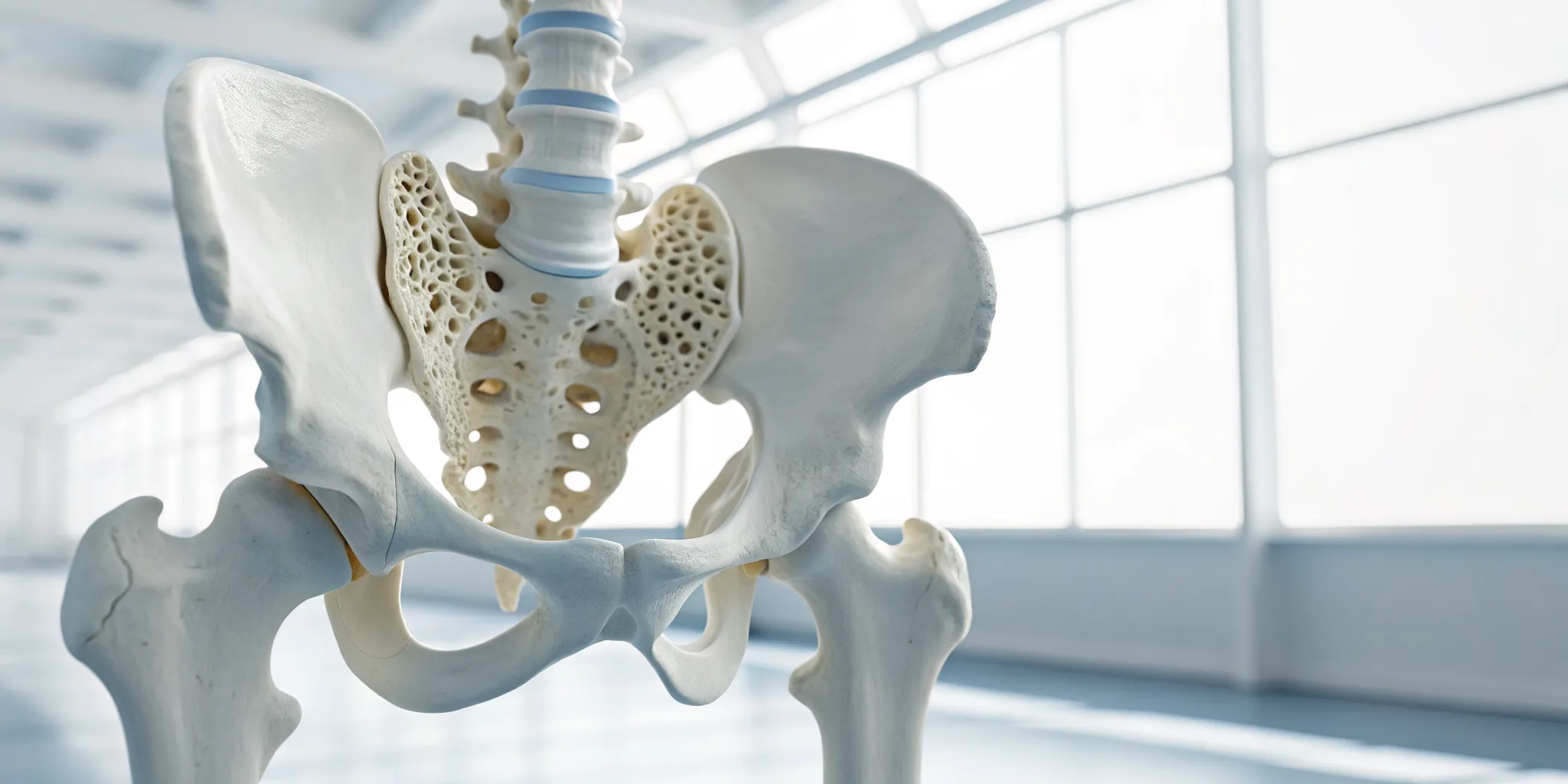
The science behind spinal decompression is straightforward. The gentle, computerized stretching of the spine creates a vacuum-like effect inside the discs. This negative pressure does two very important things. First, it can help retract bulging or herniated disc material, taking pressure off pinched nerves. This is often the key to relieving the sharp, radiating discomfort associated with conditions like sciatica.
Second, and just as crucial, this process encourages the movement of water, oxygen, and nutrient-rich fluids into the discs. Healthy discs need these elements to thrive, but when they are compressed, their supply can be cut off. By restoring this flow, spinal decompression helps rehydrate the discs and provides the building blocks they need to heal, making it an effective part of a plan for many of the conditions we treat.
Conditions It Can Help
Spinal decompression is particularly helpful for people experiencing specific types of spinal issues. It’s often a go-to therapy for those with bulging or herniated discs who are looking for a non-invasive path toward relief. If you’re dealing with the radiating leg discomfort, numbness, or tingling characteristic of sciatica, this therapy can be incredibly effective by targeting the nerve compression at its source.
It’s also used for individuals with spinal stenosis, where the spinal canal has narrowed, and for those with worn spinal joints. For many, it represents a powerful way to manage chronic discomfort and improve mobility without resorting to more aggressive measures. To find out if you’re a good candidate for this therapy, the best first step is a thorough consultation. You can reach out to our team to schedule an appointment.
Does Insurance Cover Spinal Decompression?
Navigating the financial side of your health journey can feel like a job in itself. When it comes to specialized treatments like spinal decompression, one of the most common questions we hear is about payment and reimbursement. The answer isn't always straightforward, but understanding the process can help you make informed decisions for your health and budget. While every situation is unique, let's walk through the common factors that influence whether your health plan will contribute to the cost of this therapy.
Why Coverage Can Be Complicated
Getting reimbursement for spinal decompression can be complex because many third-party payers classify it as "investigational." This can happen even though the technology is FDA-cleared and has helped many people find relief from chronic back and neck pain. From a payer's perspective, they often want to see a larger volume of specific types of research before they will consistently reimburse for a service. This creates a frustrating gap where a treatment is known to be effective, but getting a health plan to help with the cost is not guaranteed. At Ascend, we focus on creating a comprehensive physical medicine plan to give you the best possible outcome, both for your health and your finances.
The "Experimental" Label Explained
So, what does it mean when a treatment is labeled "experimental"? Essentially, it’s a classification used by benefits providers that can make reimbursement challenging. The decision to apply this label often comes down to the specific rules of your benefits company and the details of your personal health plan. It doesn't mean the treatment is unsafe or doesn't work. It simply means it hasn't been accepted into their standard list of reimbursable procedures. Think of it this way: your provider has determined this is the right path for you, but we may need to provide extra information to help your benefits company understand that choice.
How Your Diagnosis Affects Coverage
Your specific diagnosis plays a huge role in this process. For a health plan to consider contributing to the cost, your provider must clearly demonstrate that spinal decompression is "medically necessary" for your condition. This involves building a strong case that documents your symptoms and shows why this particular therapy is essential for your recovery. Reimbursement is more likely for well-documented conditions we treat, such as herniated discs, sciatica, or degenerative disc disease. Furthermore, presenting spinal decompression as part of a holistic treatment strategy, one that includes other therapies like corrective exercises, can often strengthen your case for approval.
What Determines Your Coverage?
Figuring out if your health plan will help with the cost of spinal decompression isn't always straightforward. The answer isn't a simple yes or no. Instead, it depends on a unique combination of factors, including your personal health background, the specifics of your benefits package, and even the providers available in your community. Understanding these key elements is the first step in clarifying your potential financial responsibility and making an informed decision about your care. By looking at each piece of the puzzle, you can get a much clearer picture of what to expect.
Your Health History and Condition
For a health plan to contribute to your treatment, they typically need to see that it is “medically necessary.” This means your healthcare provider must create detailed documentation that clearly shows why spinal decompression is an essential therapy for your specific health problem. A thorough diagnosis, along with a history of other treatments you may have tried without success, builds a strong case. For instance, if you are dealing with persistent back pain from a herniated disc, your provider will explain why decompression is a targeted and necessary approach for your particular health concern. This paperwork helps show that the care is a crucial part of your recovery.
Your Specific Plan and Network
Every health benefits plan has its own unique rules and guidelines. Your level of contribution depends entirely on the fine print of your specific agreement. Some plans may classify spinal decompression as an “investigational” or “experimental” therapy, even though it has a strong track record and is cleared by the FDA. This classification can directly affect how much of the cost your plan is willing to shoulder. The type of plan you have also plays a significant role. Plans that offer more flexibility in choosing specialists often provide better options for this kind of care. Our team can help you understand the right questions to ask your benefits administrator, so please contact us for guidance.
Your Location and Local Providers
Where you live and which providers are included in your plan's network can also influence your out-of-pocket costs. The benefits available for specialized chiropractic services can vary quite a bit from one region to another. Generally, choosing a provider that is considered "in-network" by your plan will lead to lower personal expenses compared to seeing an "out-of-network" provider. At Ascend, we have experience with a wide range of health plans and can help you understand how your benefits apply to our physical medicine services. We are committed to making the financial side of your care as transparent as possible so you can focus on healing.
How to Check Your Coverage
Figuring out what your health plan will pay for can feel like a puzzle, but you don't have to solve it alone. Taking a few direct steps can give you a clear picture of your benefits and help you plan for the cost of care. The best approach is to be proactive and gather all the information you need before you begin treatment. This way, you can focus on what truly matters: your health and recovery.
Our team at Ascend Functional Health is also here to help you understand the financial aspects of your care. We believe in transparency and want you to feel confident and informed every step of the way. Think of us as your partners in health, ready to assist you with the administrative details so you can concentrate on healing.
Steps for Verifying Your Benefits
The most straightforward way to understand your benefits is to contact your benefits administrator directly. When you call the number on your card, you can get the most accurate and specific information for your plan. Be sure to ask them specifically if "non-surgical spinal decompression" is a covered service. Sometimes, the terminology matters. Using the exact name of the therapy can prevent confusion and get you a clearer answer. While our team is always here to help, a direct call gives you firsthand information about your personal plan details. If you have questions about this process, feel free to contact our office for guidance.
Questions to Ask Your Health Plan Provider
When you speak with your benefits administrator, having a list of questions ready can make the conversation much more productive. You’re not just asking if the therapy is a paid-for service; you’re trying to understand the full scope of your benefits.
Consider asking these questions:
- Is non-surgical spinal decompression therapy a covered benefit under my plan?
- Do you handle payments for mechanical traction differently than manual traction?
- Are chiropractic visits that include decompression therapy eligible for payment?
- Do I need a referral or pre-approval before starting treatment?
- Can I use my Health Savings Account (HSA) or Flexible Spending Account (FSA) for any out-of-pocket costs?
These questions will help you get a complete picture and avoid any surprises down the road.
Getting Help with Preauthorization
Some health plans require preauthorization (or prior approval) before they will agree to pay for certain treatments. This means your healthcare provider needs to get approval from your plan administrator before you begin your spinal decompression sessions. Securing preauthorization is a critical step to confirm that the service will be a paid-for benefit, helping you avoid unexpected bills later. Our team has experience with this process and can help manage the necessary paperwork to demonstrate why physical medicine like spinal decompression is the right choice for your condition. We'll work with you to ensure all the requirements are met so you can start your treatment with peace of mind.
What Paperwork Do You Need for Approval?
When you're working to get spinal decompression therapy approved, documentation is everything. Think of it as building a clear, compelling story about your health journey and why this specific therapy is the right next step for you. Having your paperwork in order can make the process much smoother. It helps demonstrate that the treatment isn't just a preference but a necessary part of your path toward healing. Your provider’s office will guide you, but knowing what’s needed can help you feel more prepared and in control.
Proving Medical Necessity
Your benefits provider will want to see that spinal decompression is "medically necessary" for your situation. This simply means you need to show how the therapy directly addresses your health condition and is essential for your recovery. Your provider will document how your symptoms affect your daily life and detail other treatments you’ve tried that haven’t provided lasting relief. This helps create a strong case that decompression is a logical and needed intervention for your specific health issues. The goal is to paint a clear picture of why this treatment is a crucial part of your care plan.
Gathering Your Medical Records
A solid paper trail is your best friend. The foundation of your request is a clear diagnosis, which is why your provider will gather all relevant medical records. This includes any imaging reports you have, like MRIs or X-rays, that visually confirm your condition. It’s also helpful to include notes from previous doctors and a summary of treatments you’ve already undergone. This collection of documents provides objective evidence that supports your need for advanced physical medicine approaches like spinal decompression. It shows that you and your care team have been thorough in exploring your options.
Outlining Your Treatment Plan
Working with a knowledgeable provider who understands how to handle the approval process is key. A detailed treatment plan is a critical piece of the puzzle. This document, prepared by your doctor, will outline the specifics of your spinal decompression therapy, including the recommended number of sessions, the frequency of your visits, and the clear goals you’re working toward. It shows your benefits provider that there is a strategic, well-thought-out approach to your care. When you have an experienced team on your side, you can feel confident that your case is being presented clearly and professionally.
What Are Your Payment Options Without Coverage?
When your health plan doesn't extend to a specific therapy, it’s easy to feel discouraged. But please don’t let that be a barrier to getting the care you need. Thinking about the financial side of your health journey is a valid concern, and many paths can make your treatment plan manageable. The most important thing is finding a solution that brings you long-term relief. Let's walk through a few common options for handling payments when you're not using a benefits plan.
Exploring Payment Plans
Many forward-thinking clinics understand that paying for a full treatment plan upfront isn't always practical. That’s why flexible payment plans are often available. These plans allow you to break down the total investment into smaller, more manageable monthly payments. This approach can ease the financial pressure, letting you focus on what truly matters: your healing and recovery. We believe financial concerns shouldn't stand in the way of your well-being. If you have questions about structuring a payment plan that works for your budget, we encourage you to contact our office to discuss the possibilities. We're here to help find a solution that fits your needs.
Using Your HSA or FSA
If you have a Health Savings Account (HSA) or a Flexible Spending Account (FSA), you may be able to use those funds for spinal decompression. These accounts are designed to help you set aside pre-tax money specifically for qualified medical expenses, which can make your healthcare dollars stretch further. Using these accounts is a smart way to invest in your health. Since every account has its own guidelines, it’s a good idea to confirm that this type of physical medicine is an approved expense. Taking a few minutes to check your account details can provide a clear and simple way to pay for your care.
Understanding Self-Pay Options
Paying directly for your care, often called "self-pay," is a straightforward option. Knowing the potential investment ahead of time helps you plan accordingly. A single spinal decompression session typically ranges from $50 to $250. A complete treatment plan is tailored to your specific needs and usually involves a series of sessions, with the total investment generally falling between $1,290 and $3,900. While this may seem significant, it's helpful to view it as an investment in your long-term health and freedom from chronic discomfort. A personalized consultation will determine the exact number of sessions you’ll need to address the conditions we treat and achieve lasting results.
Why Is It Sometimes Labeled "Experimental"?
If you’ve started looking into your benefits for spinal decompression, you might have run into a frustrating word: “experimental.” It can be confusing to see a treatment that has helped so many people get this label. This classification is often the biggest hurdle patients face when seeking approval for their care.
Understanding why this happens can help you and your doctor build a stronger case for your treatment plan. The label doesn't mean the treatment is new or unproven. Instead, it points to a gap between how medical providers and benefit providers evaluate a procedure. Let’s break down the three main reasons why spinal decompression is sometimes flagged this way.
FDA Status vs. Insurance Standards
One of the most common points of confusion is the difference between FDA approval and what a health plan considers standard practice. Spinal decompression therapy is performed using equipment that is approved by the U.S. Food and Drug Administration (FDA). This means it has been cleared as safe and effective for its intended use, which is a major milestone for any medical device.
However, health plan providers follow their own set of standards. They often require a large volume of specific types of long-term research before they will consider a treatment a "standard" part of care. So, even with FDA approval and a history of successful patient outcomes, some plans may still classify the treatment as "investigational" until more large-scale studies are published.
The Need for More Long-Term Data
Benefit providers typically want to see proof that a treatment is “medically necessary” for your specific condition. To make this determination, they rely on extensive clinical data, often from studies that follow thousands of patients over many years. While there is plenty of evidence showing that spinal decompression is effective for conditions like herniated discs and sciatica, some providers feel there isn't enough of this specific type of long-term data yet.
This is a key reason for the "experimental" label. They may view the treatment as still being tested from a data perspective, even though it has been used successfully in clinics for years. At Ascend Functional Health, we focus on creating a personalized treatment plan that clearly outlines why physical medicine approaches like decompression are the right choice for your health goals.
How Insurers View the Cost
Finally, it’s important to acknowledge that financial considerations can influence how a treatment is categorized. Some healthcare professionals believe the "experimental" label is sometimes used for financial reasons rather than being a true reflection of the treatment's effectiveness. Because spinal decompression can be a more involved therapy than simple adjustments or other conventional options, it can represent a higher initial expense.
Providers may be slower to adopt payment approval for treatments that change their financial models, even if those treatments can lead to better long-term outcomes and potentially lower costs down the road by helping patients avoid more invasive procedures. Understanding this perspective can help you see the full picture when discussing your care options.
Making the Best Financial Choice for Your Health
When you're dealing with chronic pain, the last thing you want to worry about is navigating the financial side of treatment. It’s completely understandable to feel concerned about the cost of care. But thinking about this cost as an investment in your long-term well-being can shift your perspective. Getting back to a life without pain, being able to play with your kids, or simply sitting comfortably at your desk has a value that’s hard to quantify.
The reality is that many health benefit plans are slow to adopt newer, effective therapies, and they may not automatically pay for treatments like spinal decompression. This can be frustrating, but it doesn’t mean relief is out of reach. It just means we need to get a little creative and proactive. Thinking through your options ahead of time can help you create a clear path forward, allowing you to focus on what truly matters: your healing journey. Let’s walk through some practical ways to approach the financial side of your care so you can make the best decision for your health and your wallet.
Weighing the Cost Against Long-Term Relief
It’s helpful to frame the expense of spinal decompression against the potential costs of not addressing the root issue. Many people explore this therapy as a way to find lasting relief from bulging or herniated discs, sciatica, and other debilitating back problems, often to avoid more invasive procedures. When you consider the expense, recovery time, and potential complications of major surgery, the cost of a non-surgical approach often looks very different.
While many third-party payers still consider this therapy "investigational," there's a reason patients continue to seek it out and pay for it directly: it works. Investing in your health now can prevent years of chronic pain and the ongoing expenses of managing symptoms. It’s about choosing a solution that addresses the underlying cause of your discomfort, helping you heal and improve your quality of life for years to come.
Creating a Payment Strategy
The good news is that even if your health plan doesn't directly pay for spinal decompression, you have options. Many people use tax-advantaged accounts to cover their care. If you have a Health Savings Account (HSA) or Flexible Spending Account (FSA) through your employer, these funds can typically be used for spinal decompression therapy. This allows you to pay for your treatment with pre-tax dollars, which can result in significant savings.
Additionally, many clinics understand that patients are often paying for this care themselves and offer flexible payment plans to make it more manageable. These plans allow you to spread the cost of your treatment over several months. The best first step is to have an open conversation with our team. We can help you understand all the available options and find a strategy that fits your budget. You can contact our office anytime to discuss your specific situation.
Considering Other Treatment Paths
Spinal decompression is a powerful therapy, but it rarely works in isolation. At Ascend Functional Health, we see it as one component of a comprehensive healing plan designed just for you. Your care might also include corrective chiropractic adjustments, specific exercises, or other therapies aimed at restoring function and stability. This holistic approach is key to achieving lasting results because it addresses your body as an integrated system.
When spinal decompression is part of a broader physical medicine plan, it supports a more complete recovery. By combining treatments, we can tackle your pain from multiple angles, addressing muscle imbalances, joint dysfunction, and nerve pressure all at once. This not only improves your outcome but also demonstrates a well-rounded approach to your healing, which can be beneficial when outlining your care plan.
Related Articles
- Is Lumbar Decompression Chiropractic for You?
- Spinal Decompression Hurts Lower Back: Normal or Not?
- Revitalize Your Spine with Spinal Decompression Therapy in Tampa, FL
- Spinal Decompression Therapy in Tampa, FL - Alessi Functional Health
Frequently Asked Questions
What does a spinal decompression session actually feel like? Many people are surprised by how relaxing the process is. You’ll lie on a comfortable, padded table while a specialized system applies a very gentle and controlled stretching force to your spine. It’s not a sudden or jarring movement at all. Instead, you’ll feel a slow, rhythmic elongation in your back or neck as the pressure is gradually relieved. Most patients find the sessions to be comfortable and pain-free.
How is this different from an inversion table or regular stretching? While stretching and inversion tables can offer some temporary relief, spinal decompression is a much more precise and targeted therapy. The computerized system is designed to apply a specific amount of force to gently separate the vertebrae, creating negative pressure within the disc itself. This is what helps retract bulging material and encourages healing fluids to enter the disc. It’s a sophisticated clinical approach that goes beyond a general stretch.
How many sessions will I need to feel better? The number of sessions needed is unique to each person and depends on your specific condition, its severity, and your overall health. A complete treatment plan is designed to create lasting change, not just temporary relief. After a thorough initial consultation, your provider will create a personalized plan that outlines the recommended frequency and number of visits needed to help you reach your health goals.
Why is the approval process for this therapy so complicated? The process can be complex because many benefits providers have strict criteria for what they will help pay for. They often classify spinal decompression as "investigational," not because it's unsafe, but because they require a very large volume of specific long-term studies before adding it to their list of standard procedures. This means your provider must build a strong case with detailed paperwork, including your health history and imaging reports, to show why the therapy is medically necessary for you.
What are my next steps if my benefits provider won't help with the cost? If your plan doesn't offer assistance, you still have several great options for making care manageable. Many people use their Health Savings Account (HSA) or Flexible Spending Account (FSA) to pay for treatment with pre-tax dollars. Another common path is to arrange a flexible payment plan with the clinic, which allows you to spread the investment over time. The best first step is to have an open conversation with our team about your situation so we can help you find a financial strategy that works for you.